Japanese encephalitis – here to stay

In 2022, Japanese encephalitis emerged as a major concern for the Australian healthcare system because of a rise in locally acquired cases. Health authorities, including the newly established Australian Centre for Disease Control, now formally recognise Japanese encephalitis virus as endemic in large parts of mainland Australia. Ongoing prevention relies on surveillance, mosquito control and an expanded vaccine strategy. Key priorities also include timely diagnosis and sustained public health action.
- Since its emergence on mainland Australia in 2022, the Australian Centre for Disease Control now formally recognises the Japanese encephalitis (JE) virus as endemic to large parts of mainland Australia, with ongoing environmental reservoirs.
- Genotype IV, the genotype established in Australia, was previously recognised only in Indonesia and Papua New Guinea. It is less well characterised than other genotypes and has likely adapted to local mosquito and wading bird populations.
- Although most infections are mild or asymptomatic, JE virus can cause severe neurological disease with high mortality and morbidity, and no effective antiviral is currently available. JE virus should be considered in patients with encephalitis, even without a travel history.
- In Australia, a high proportion of clinically significant cases have occurred in adults, unlike in long-endemic regions where disease is more common in younger age groups. Disease patterns are likely to continue changing with environmental shifts, vaccination and control measures.
- Because JE virus circulates in multiple reservoir and amplifying hosts and is transmitted by various mosquito vectors, control requires a One Health approach, including co-ordinated surveillance, mosquito control and public education.
- Vaccination remains central to prevention, with several population groups now targeted through state-run funded programs.
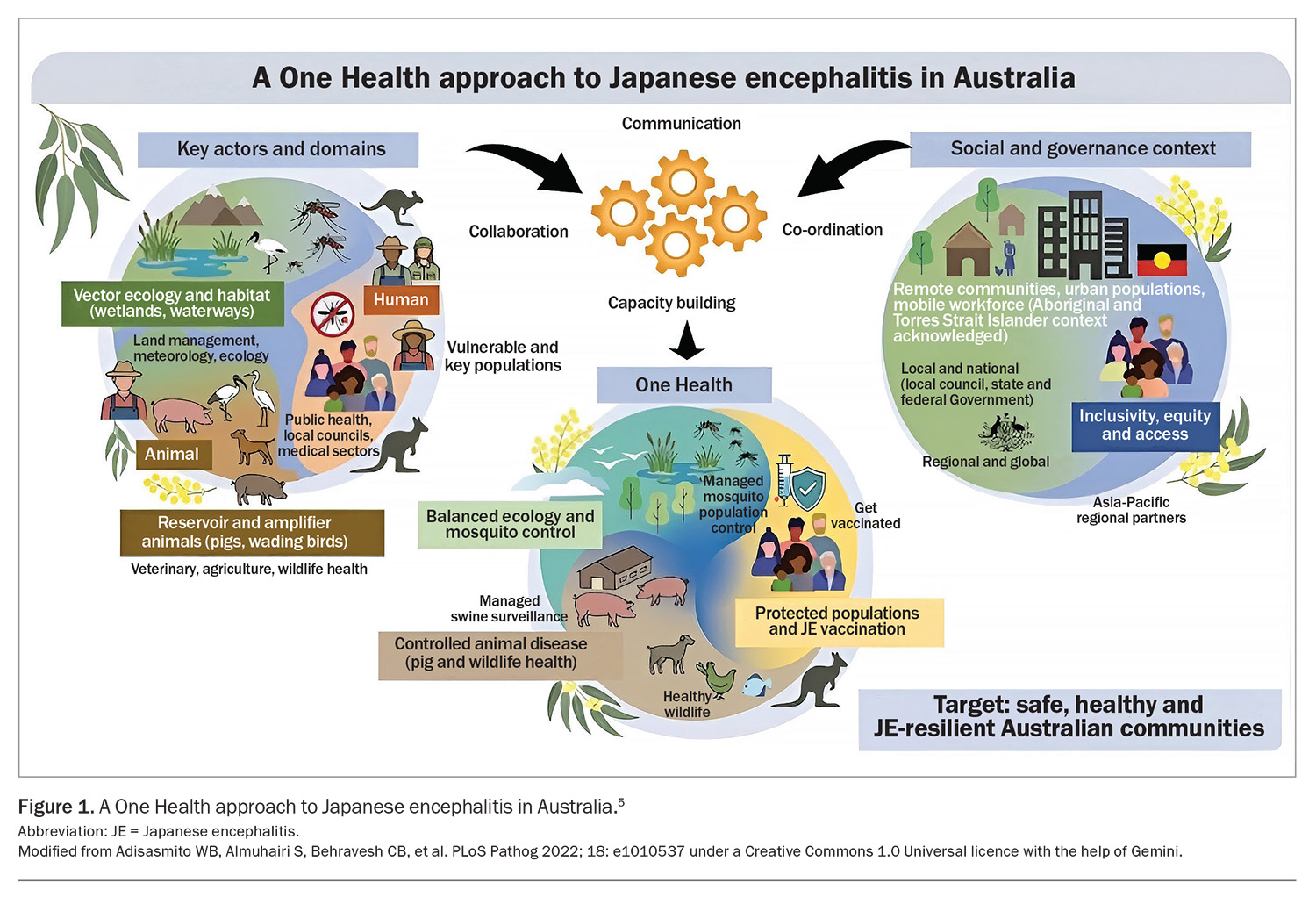
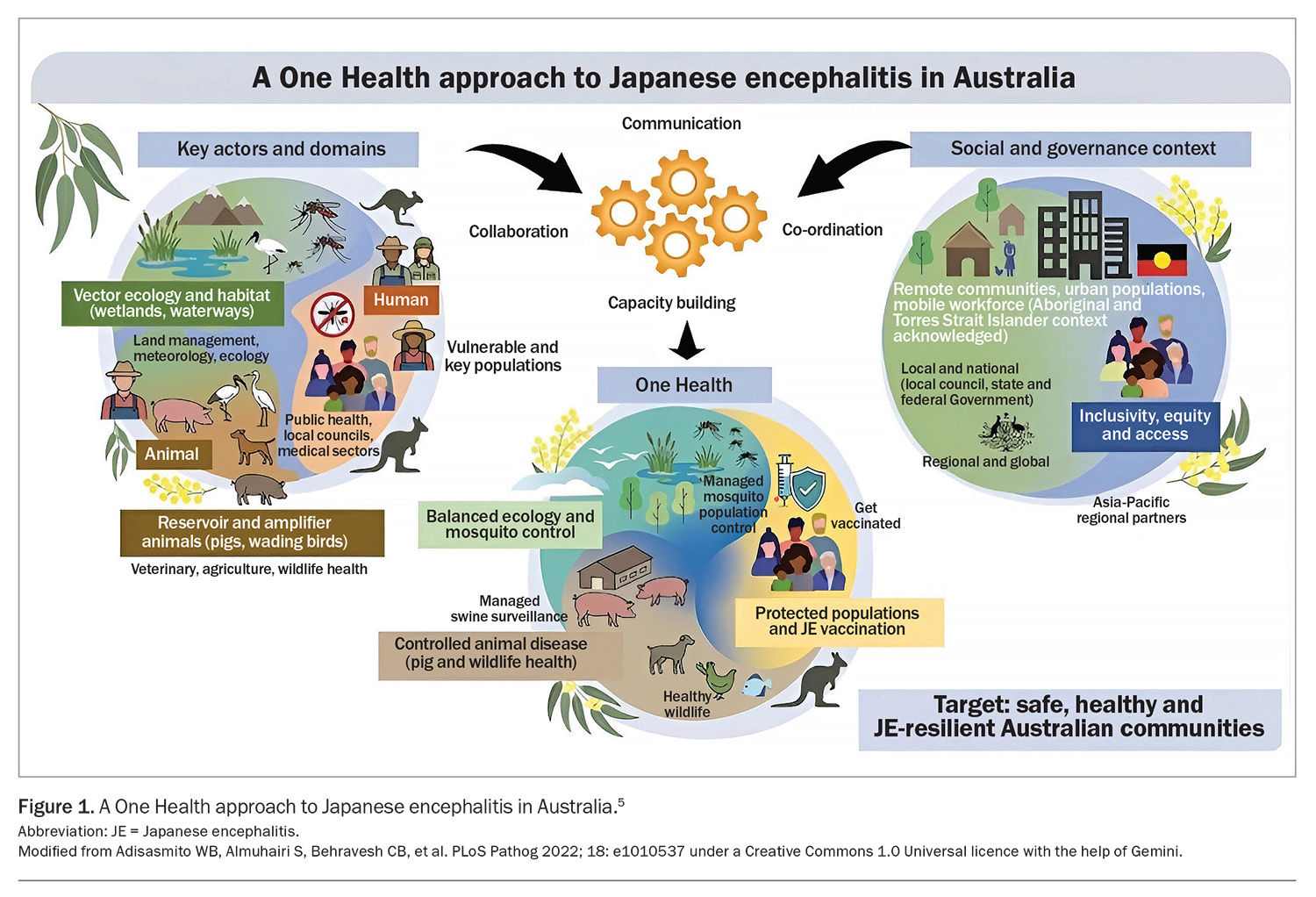
Japanese encephalitis (JE) is a potentially fatal mosquito-borne encephalitis that has transitioned from sporadic incursions to ongoing environmental circulation in mainland Australia since 2022.1 JE is caused by a single-stranded RNA flavivirus related to dengue, Zika and yellow fever viruses.2 In Australia, Culex annulirostris is a highly competent vector and is implicated in sustaining transmission.3 The nonscientific name for this species is the common banded mosquito. Beyond Australia, it is native to Indonesia, Fiji, Micronesia and the Philippines.4 Humans, horses and cattle are dead-end hosts, whereas pigs serve as amplifying hosts and waterbirds serve as reservoir hosts, helping to maintain environmental transmission cycles (Figure 1).2,5
Since the initial 2022 outbreak, described in our original article (which saw 45 human cases and six deaths), Australia has seen sporadic but consistent activity.6 Our response to the virus has evolved from an ‘emergency response’ to a ‘sustained management’ phase, meaning medical practitioners need to maintain ongoing vigilance for the possibility of JE disease in Australia, even in patients with no travel history.
Virus genotypes and pathophysiology
Genotypes
Five genotypes have been identified, with genotypes I and III tending to cause summer epidemics in northern temperate areas, whereas genotypes II and IV result in endemic disease in southern tropical regions. Genotype V is dominant in South Korea.7 The genotype that has established itself in Australia is genotype IV, which was previously known to be present only in Indonesia and Papua New Guinea. This lineage was previously rare and suggests a specific adaptation to our local Culex annulirostris mosquitoes and wading bird populations.8 This has important implications for disease control in Australia, as the transmission dynamics and disease potential of genotype IV remain much less characterised than the more common genotypes.9 Current vaccines are based on genotype III and research efforts are under way to develop a vaccine based on genotype IV.10 Although broad cross-protective efficacy against other genotypes has been demonstrated with currently available vaccines, concern exists that this efficacy may be lost over time if vaccine development continues to rely on historical genotype III strains.11
Pathophysiology
After the initial mosquito bite, viraemia develops in the host. Most cases are asymptomatic, and the viraemia is usually cleared before it reaches the central nervous system. Less than 1% of people develop neurological symptoms.12 However, if the virus crosses the blood–brain barrier it can cause severe neuroinvasive disease and encephalitis, with up to 30% mortality and about 30 to 50% of survivors suffering long-term morbidity.12,13
Key epidemiological changes in Australia since 2022
JE has long been a leading cause of vaccine-preventable encephalitis in large parts of Asia and the Western Pacific, with the outer Torres Strait Islands and Tiwi Islands deemed at risk.14 Globally, the burden is estimated at around 100,000 clinical cases a year.15 Since the emergence of JE on the mainland in 2022, large parts of Australia are now recognised as seasonal risk zones, typically from November to May, although transmission can occur year-round in tropical northern Australia.16
After the initial outbreak in 2022 and early 2023, 45 confirmed and probable human cases had been reported across New South Wales, Queensland, South Australia and the Northern Territory, followed by a relative decrease in 2023 and hopes that the outbreak was a one-off event.6,17 However, this was short-lived with further locally acquired infections in late 2024. During the 2024 to 2025 summer, nine human cases were reported in Australia, including five deaths.18 Surveillance activities detected JE virus on 20 piggeries.19 This led to concern about ongoing endemicity in birds, pigs and mosquitoes. Even early after the emergence of the virus in Australia, more than 80 piggeries across multiple states were noted to have JE virus detected in pigs.1 Human serosurveys in rural towns in New South Wales as early as June to July 2022 revealed 8.7% seropositivity, suggesting significant dissemination of the virus.20
JE virus was detected in a mosquito trap in Horsham Rural City Council, Victoria, in late 2025.21 In addition, it was detected in piggery effluent collected in Strathbogie Shire, Victoria, in November 2025.22 In New South Wales, sentinel chickens in Upper Lachlan Shire returned positive results in January 2026, along with recurrent positive domestic pig serology in Queensland and New South Wales through late 2025 to early 2026.23,24 This is particularly concerning because it is estimated that about 3% of the population of Australia lives within about 4.4 km of a piggery, which is the likely flight range of Culex annulirostris.25 Ongoing surveillance through 2026 may reveal further environmental detections, such as in mosquitoes, piggery effluent, and domestic or feral pigs, confirming sustained circulation even when human case numbers are low. A fatal case was reported in northern Sydney in 2025.26
How has JE virus established itself in mainland Australia?
Multiple ecological drivers have enabled the persistence of JE virus. Australia has competent local vectors proven for genotype IV, such as Culex annulirostris, significant migratory waterbird movement along river corridors and seasonal conditions that favour mosquito proliferation.19,27 Public health analyses since 2022 have also highlighted how wetter periods and regional ecology can expand risk beyond historical northern foci into the Murray-Darling basin and surrounding regions.17,28
Although the 2022 outbreak was fuelled by a record-breaking La Niña, the years since have shown that JE virus can persist even during neutral or El Niño phases. The virus is likely ‘overwintering’ in northern Australian wetlands or in local bat and feral pig populations, ready to ‘spill over’ whenever local rainfall triggers mosquito blooms.29
Long-term climate change is likely to play an ongoing role in the persistence of JE virus in mainland Australia, along with other viruses that share the same or similar vectors such as Murray Valley encephalitis virus. Episodes of heavier than usual rainfall, expansion of the range of migratory waterbirds further south and increased mosquito breeding may all contribute to ongoing endemicity.30,31 Moreover, over time, mosquitoes may become capable of inhabiting regions with higher elevations and latitudes.
Changing disease demographics and clinical manifestations
Disease demographics
JE has typically been considered largely a childhood disease in endemic areas. Most adults develop immunity from previous, often subclinical, infection and so adult presentations with encephalitis were comparatively rare. When the virus enters new geographic locations, all age groups are susceptible to infection and so the proportion of adult cases increases. Before its arrival in Australia, this pattern was noted in other locations such as the Northern Mariana Islands.32 In Nepal, JE was first reported in 1978 and has since become well established in the low-lying Terai region. It is increasingly being recognised in areas of higher elevation such as the Kathmandu Valley. Most districts in Nepal have reported JE cases, suggesting evolving disease patterns after its relatively recent introduction into the country.33 This has important implications for disease control interventions and vaccination campaigns. During the 2022 outbreak in Australia, 55% of cases were in adults aged 60 years or older.17
Clinicians should suspect JE in compatible illness during mosquito season or after exposure in risk areas, even without overseas travel. Exposures such as working or living near a piggery and recent mosquito bites should be determined.
Clinical manifestations
The incubation period from JE virus infection to clinical disease is two to 14 days.34 Disease may not be apparent initially and early symptoms can be nonspecific, including lethargy, headache and nausea. In a small proportion of patients, these symptoms progress to meningoencephalitis, including photophobia, nuchal rigidity, altered consciousness, parkinsonian-like signs, seizures (particularly in children) and, rarely, acute-onset flaccid paralysis.34,35 During the 2022 outbreak, the case fatality rate was 17%, with 67% of all cases occurring in males.17 To date, it is uncertain whether genotype IV has a different disease pattern from that of other genotypes.
Diagnosis
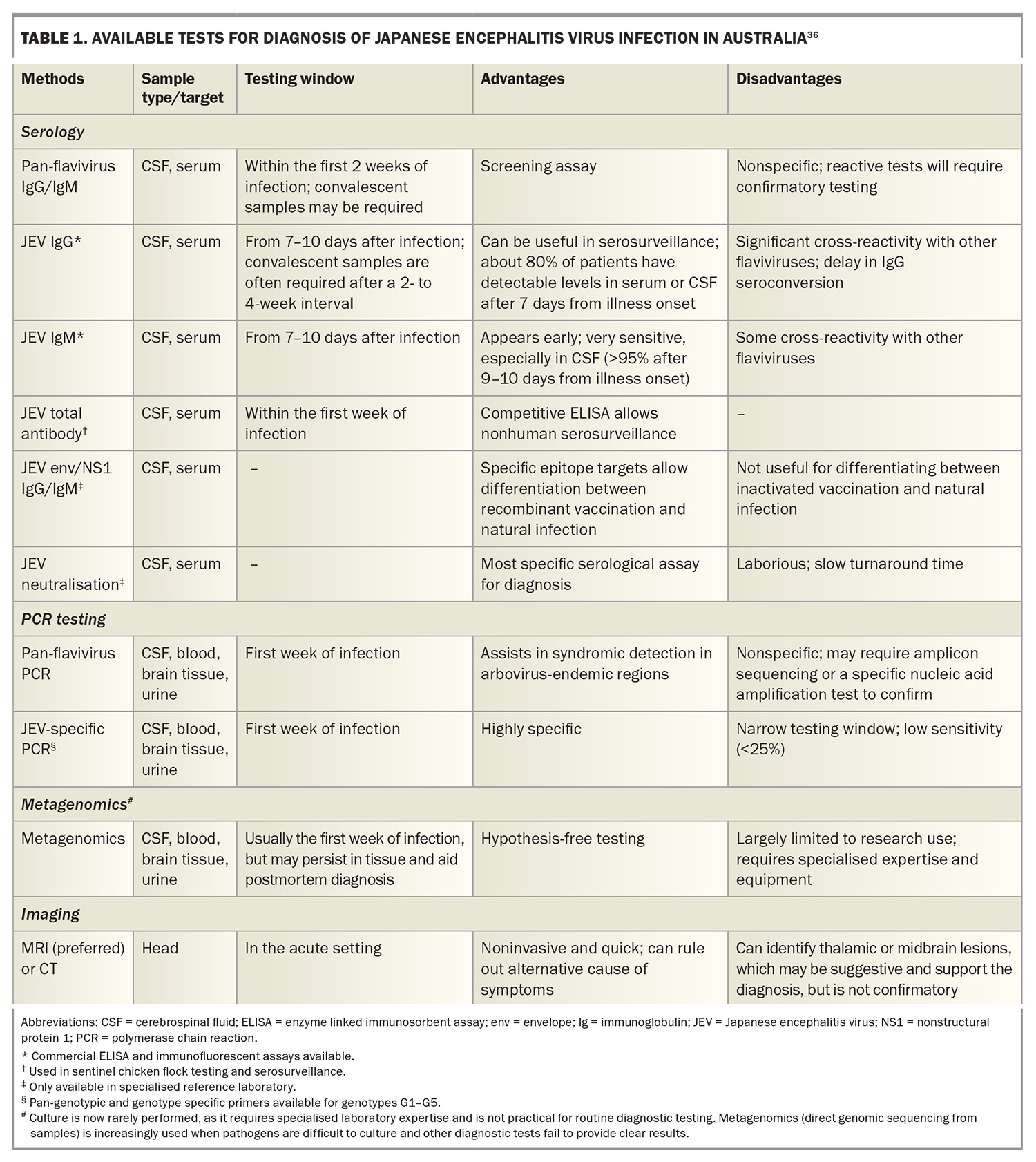
Serology remains the primary diagnostic method for JE virus infection, with cerebrospinal fluid (CSF) the preferred sample. JE virus-specific immunoglobulin M in CSF supports the diagnosis, whereas polymerase chain reaction (PCR) of CSF, serum or urine is highly specific but has limited sensitivity and is most useful early in the disease course. It is important to note that a negative PCR does not exclude the diagnosis of JE. Serology may cross-react with other flaviviruses; confirmatory or reference testing is often required at a reference laboratory.
Other causes of encephalitis should also be considered and tested for. Common infective causes of encephalitis include varicella zoster virus, herpes simplex virus and enteroviruses. Bacterial meningitis can cause diagnostic uncertainty, and empiric antibiotic treatment should not be delayed if this remains a possibility. Because JE can present similarly to other, longer-standing encephalitis viruses circulating in Australia, such as Murray Valley encephalitis virus and the Kunjin subtype of the West Nile virus, it is common practice to order a pan-flavivirus PCR or serology on CSF; these may be referred to as arbovirus assays. Given the changed status of JE in Australia, strong clinical suspicion needs to be maintained if no other cause is evident. Table 1 outlines the main diagnostic tests available in Australia.36
Management of a suspected case
Unfortunately, no specific antiviral therapy exists, and management is supportive, including fluids, antipyretics, seizure control and intracranial pressure management, alongside empiric treatment for alternative infectious encephalitides pending results (e.g. intravenous acyclovir). Immediate hospital referral should be made for reduced Glasgow Coma Scale score, focal neurological signs, seizures, unstable observations or if close monitoring cannot be ensured. Infectious diseases input should be sought when JE is suspected and no clear alternative diagnosis is identified.
JE remains nationally notifiable. Suspected cases should be reported promptly to public health units; do not wait for confirmatory tests if strongly suspected. Although several potential antiviral agents have been identified and research using novel drug discovery techniques is ongoing, few have demonstrated efficacy in clinical trials, so the wait for an effective therapy continues.37
Preventing the impact of JE virus
Ongoing public health and individual measures are needed to reduce the impact of the JE virus. Given the virus has shifted to endemic status in Australia, the need for a comprehensive One Health approach should be stressed, because of the multiple factors influencing the virus’s epidemiology (Figure 1).5 Broadly, this approach entails integrated mosquito management, targeted surveillance and rapid risk communication with a focus on piggeries. The Joint National Japanese Encephalitis Virus Outbreak Response Plan, published in June 2023, outlines the overarching governance arrangements between multiple organisations and the activities carried out by them. The Australian Centre for Disease Control co-ordinates the One Health response and conducts ongoing activities, including feral pig monitoring, using aerial and ground sampling to track the virus in remote populations. Mosquito trapping, using real-time PCR, provides early warning before potential human cases emerge. Further surveillance is conducted by monitoring the wastewater from commercial piggeries, which often serves as the ‘canary in the coal mine’ for local viral circulation.38,39
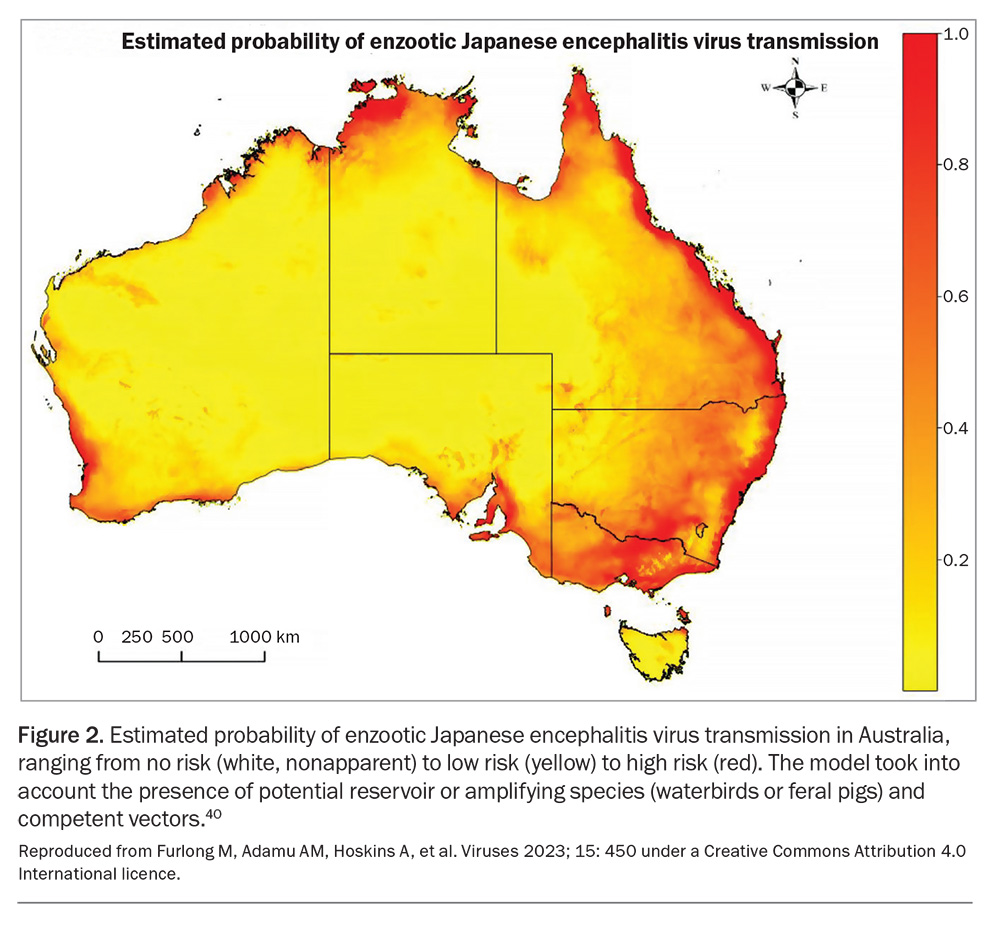
On an individual basis, prevention includes physical measures to reduce mosquito bites, by using topical repellents such as N,N-diethyl-meta-toluamide (DEET) or, alternatively, picaridin, especially in children, wearing protective clothing, staying in screened accommodation and reducing standing water. Medical practitioners should maintain vigilance for the possibility of JE in their patients and be aware of public health notifications and whether their patients come from an at-risk zone (Figure 2).40
Vaccination
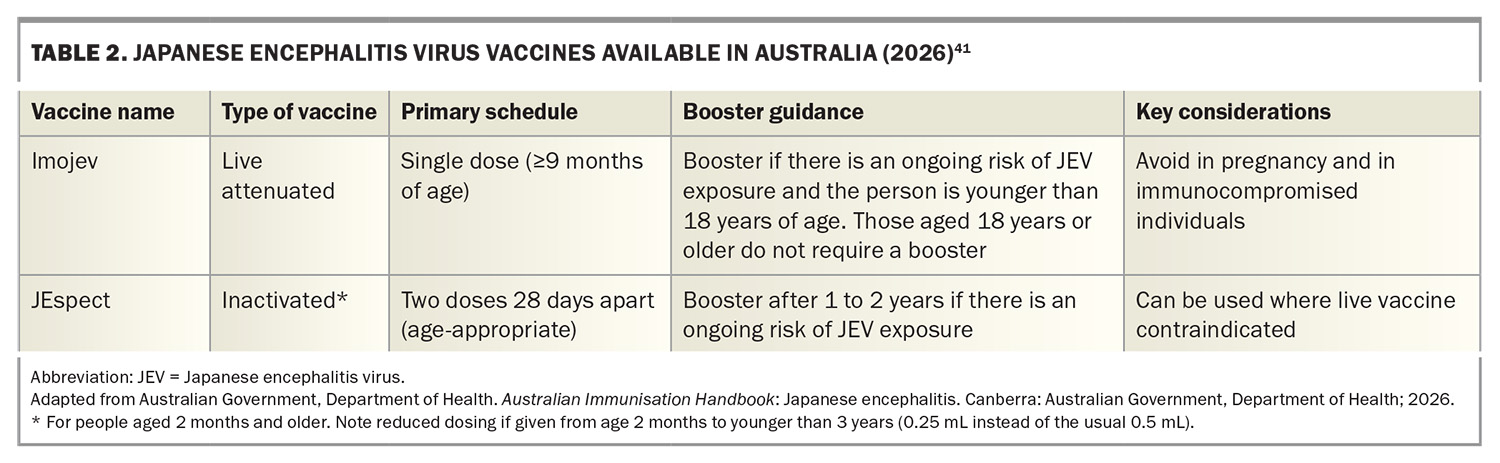
Vaccination is an important consideration, with state-funded programs providing access to both live attenuated and inactivated JE vaccines for at-risk residents and occupational groups (Table 2).41 Since 2022, when the vaccine was offered to piggery workers, the eligibility criteria have broadened significantly to reflect the endemic risk (Box).41
Funded JE vaccination is offered to several groups.
- High-risk local government areas – residents or frequent visitors to about 80 local government areas across New South Wales, Victoria, Queensland and South Australia (primarily those west of the Great Dividing Range or near major river systems).
- Vulnerable populations – e.g. people experiencing homelessness or living in dwellings with poor mosquito screening in high-risk zones.
- People at occupational risk – not just piggery workers, but also park rangers, environmental health officers and flood-recovery volunteers.
Otherwise, private purchase may be considered on a case-by-case basis.
For domestic exposure and travel, vaccination is recommended for people aged 2 months and older who live in, work in or are planning travel to a JE risk area and who may be bitten by mosquitoes during the November to May season, noting local variation. Booster doses are recommended, typically one to two years after the primary course, for those with ongoing high-level exposure. Criteria for vaccination can vary by jurisdiction; detailed information on vaccine eligibility in each state and territory is available at: https://www.cdc.gov.au/diseases/japanese-encephalitis-virus-jev-infection#support.38 Various government health agencies, for example New South Wales Health and Queensland Health, have comprehensive JE information pages, including specific local government areas identified as being at risk.
In addition to vaccination, nonpharmacological measures to reduce mosquito bites should be discussed opportunistically, such as using insect repellent, treating clothing with permethrin, avoiding dark-coloured clothing and advising that Culex mosquitoes can feed from dawn to dusk. This may also help prevent other mosquito-borne diseases.
Travellers are advised to receive the vaccine if they are visiting endemic areas outside Australia during the JE virus transmission season, especially if they intend to stay for more than one month or will be spending significant time outdoors.36 A comprehensive outline of JE virus vaccination can be found at: https://immunisationhandbook.health.gov.au/contents/vaccine-preventable-diseases/japanese-encephalitis.
Conclusion
JE has shifted from episodic outbreaks to an ongoing seasonal risk in parts of mainland Australia. Prevention requires personal mosquito precautions, targeted vaccination for those at risk and sustained One Health surveillance. Clinicians should maintain a high index of suspicion, ensure appropriate diagnostic tests are undertaken and notify public health units promptly to support rapid control measures. MT
COMPETING INTERESTS: Dr Armstrong and Dr Spence: None. Professor Griffin has received speaker honoraria from Seqirus.
References
1. Australian Government, Department of Agriculture Fisheries and Forestry. Japanese encephalitis virus. Canberra: Australian Government, Department of Agriculture Fisheries and Forestry; 2025. Available online at: https://www.agriculture.gov.au/biosecurity-trade/pests-diseases-weeds/animal/japanese-encephalitis (accessed April 2026).
2. Pearce JC, Learoyd TP, Langendorf BJ, Logan JG. Japanese encephalitis: the vectors, ecology and potential for expansion. J Travel Med 2018; 25: S16-S26.
3. Van Den Hurk AF, Johansen CA, Zborowski P, et al. Mosquito host-feeding patterns and implications for Japanese encephalitis virus transmission in northern Australia and Papua New Guinea. Med Vet Entomol 2003; 17: 403-411.
4. Becker N, Petric D, Zgomba M, et al. Mosquitoes and their control. Heidelberg: Springer; 2010.
5. Adisasmito WB, Almuhairi S, Behravesh CB, et al. One Health: a new definition for a sustainable and healthy future. PLoS Pathog 2022; 18: e1010537.
6. Australian Institute of Tropical Health and Medicine. Mapping the risk of Japanese encephalitis in Australia. Townsville: Australian Institute of Tropical Health and Medicine; 2024. Available online at: https://www.aithm.jcu.edu.au/mapping-the-risk-of-japanese-encephalitis-in-australia/ (accessed April 2026).
7. Nguyen W, Gyawali N, Stewart R, et al. Characterisation of a Japanese encephalitis virus genotype 4 isolate from the 2022 Australian outbreak. Npj Viruses 2024; 2: 15.
8. Mackenzie JS, Williams DT, van den Hurk AF, Smith DW, Currie BJ. Japanese encephalitis virus: the emergence of genotype IV in Australia and its potential endemicity. Viruses 2022; 14: 2480.
9. Pyke AT, Burtonclay P, Poudel N, et al. First isolation of Japanese encephalitis virus genotype IV from mosquitoes in Australia. Vector Borne Zoonotic Dis 2024; 24: 439-442.
10. Harrison JJ, Nguyen W, Morgan MS, et al. A chimeric vaccine derived from Australian genotype IV Japanese encephalitis virus protects mice from lethal challenge. NPJ vaccines 2024; 9: 134.
11. Park JY, Lee HM. Advances and challenges in vaccination and therapeutic strategies against Japanese encephalitis virus. Pathogens 2025; 14: 1204.
12. Centers for Disease Control and Prevention (CDC). Yellow book – Japanese encephalitis. Atlanta: CDC; 2026. Available online at: https://www.cdc.gov/yellow-book/hcp/travel-associated-infections-diseases/japanese-encephalitis.html (accessed April 2026).
13. Banerjee A, Tripathi A. Recent advances in understanding Japanese encephalitis. F1000Res 2019; 8: F1000 Faculty Rev-1915.
14. Furuya-Kanamori L, Gyawali N, Mills DJ, Hugo LE, Devine GJ, Lau CL. The emergence of Japanese encephalitis in Australia and the implications for a vaccination strategy. Trop Med Infect Dis 2022; 7: 85.
15. World Health Organization (WHO). Japanese encephalitis. Geneva: WHO; 2024. Available online at: https://www.who.int/news-room/fact-sheets/detail/japanese-encephalitis (accessed April 2026).
16. Wildlife Health Australia. Japanese encephalitis virus fact sheet. Canberra: Wildlife Health Australia; 2025. Available online at: https://wildlifehealthaustralia.com.au/Portals/0/ResourceCentre/
FactSheets/PublicHealth/Japanese_encephalitis_virus.pdf (accessed April 2026).
17. Reyes Veliz A, Kane S, Glynn-Robinson A. Emergence of locally acquired Japanese encephalitis virus in Australia, January 2021-June 2022: a national case series. Commun Dis Intell (2018) 2025; 49.
18. Australian Centre for Disease Control (CDC). Be JEV-aware this summer. Canberra: Australian CDC; 2025. Available online at: https://www.cdc.gov.au/newsroom/news-and-articles/be-jev-aware-summer (accessed April 2026).
19. Commonwealth Scientific and Industrial Research Organisation (CSIRO). The science behind Japanese encephalitis virus. Canberra: CISRO; 2025. Available online at: https://www.csiro.au/en/news/All/Articles/2025/December/science-explainer-japanese-encephalitis (accessed April 2026).
20. NSW Government. Summary of NSW Japanese encephalitis virus serosurvey results. Sydney: NSW Government; 2022. Available online at: https://www.health.nsw.gov.au/environment/pests/vector/Documents/jev-serosurvey-report.pdf (accessed April 2026).
21. Horsham Rural City Council (HRCC). HRCC responds to Japanese encephalitis virus detection. Horsham: HRCC; 2025. Available online at: https://www.hrcc.vic.gov.au/Our-Council/News-and-Media/Latest-News/Horsham-Rural-City-Council-Responds-to-Japanese-Encephalitis-Virus-Detection (accessed April 2026).
22. Agriculture Victoria. Japanese encephalitis current situation. Hamilton: Agriculture Victoria; 2025. Available online at: https://agriculture.vic.gov.au/biosecurity/animal-diseases/important-animal-diseases/japanese-encephalitis/japanese-encephalitis-current-situation (accessed April 2026).
23. NSW Health. Communities across southern NSW urged to protect themselves against mosquito bites. Sydney: NSW Health; 2026. Available online at: https://upperlachlan.nsw.gov.au/wp-content/uploads/2026/01/20260113-NSW-HEALTH-MEDIA-RELEASE-Communities-across-southern-NSW-urged-to-protect-themselves-against-mosquito-bites.pdf (accessed April 2026).
24. Australian Pork. JEV surveillance updates. Brisbane: Australian Pork; 2026; https://australianpork.com.au/sites/default/files/2026-02/JEV-20Surveillance-20Update-20Week-209-20-281-29.pdf (accessed April 2026).
25. Yakob L, Hu W, Frentiu FD, et al. Japanese encephalitis emergence in Australia: the potential population at risk. Clin Infect Dis 2023; 76: 335-337.
26. NSW Health. NSW records first death of person with Japanese encephalitis since 2022. Sydney: NSW Health; 2025. Available online at: https://www.health.nsw.gov.au/news/Pages/20250225_01.aspx (accessed April 2026).
27. Klein MJ, Jackson SA, Suen WW, et al. Australian Culex annulirostris mosquitoes are competent vectors for Japanese encephalitis virus genotype IV. Emerg Microbes Infect 2024; 13: 2429628.
28. van den Hurk AF, Skinner E, Ritchie SA, Mackenzie JS. The emergence of Japanese encephalitis virus in Australia in 2022: existing knowledge of mosquito vectors. Viruses 2022; 14; 1208.
29. Moore KT, Mangan MJ, Linnegar B, et al. Australian vertebrate hosts of Japanese encephalitis virus; a review of the evidence. bioRxiv [Preprint] 2024: 2024.04.23.590833.
30. Neville PJ, Evans RN, O’Brien H, Mee PT, Brohier ND, Hughes N. ‘The perfect swarm’ - flooding across northern Victoria leads to intensified mosquito breeding and subsequent re-emergence and transmission of Murray Valley encephalitis virus during the 2022-23 mosquito season. PLoS Negl Trop Dis 2025; 19: e0013407.
31. Flores Lima M, Cotton J, Faggian R. Climate change and epidemic preparedness: high-risk regions of Japanese encephalitis virus in Victoria, Australia, From 2021 to 2100. Health Security 2025; 23: 377-388.
32. Paul WS, Moore PS, Karabatsos N, et al. Outbreak of Japanese encephalitis on the island of Saipan, 1990. J Infect Dis 1993; 167: 1053-1058.
33. Bhattarai A, Pant ND, Nepal K, Adhikari S, Sharma M, Parajuli P. Anti Japanese encephalitis virus IgM positivity among patients with acute encephalitic syndrome admitted to different hospitals from all over Nepal. PLoS One 2017; 12: e0173434.
34. Halstead SB, Thomas SJ. Japanese encephalitis: new options for active immunization. Clin Infect Dis 2010; 50: 1155-1164.
35. Howard-Jones AR, Pham D, Jeoffreys N, et al. Emerging genotype IV Japanese encephalitis virus outbreak in New South Wales, Australia. Viruses 2022; 14: 1853
36. Pham D, Howard-Jones AR, Hueston L, et al. Emergence of Japanese encephalitis in Australia: a diagnostic perspective. Pathology 2022; 54: 669-677.
37. Srivastava KS, Jeswani V, Pal N, et al. Japanese encephalitis virus: an update on the potential antivirals and vaccines. Vaccines (Basel) 2023; 11: 742.
38. Australian Centre for Disease Control (CDC). Japanese encephalitis virus (JEV) infection. Canberra: Australian CDC; 2025. Available online at: https://www.cdc.gov.au/diseases/japanese-encephalitis-virus-jev-infection (accessed April 2026).
39. Australian Government. Joint national Japanese encephalitis virus outbreak plan. Canberra: Australian Government; 2023. Available online at: https://www.cdc.gov.au/sites/default/files/2025-12/joint-national-japanese-encephalitis-virus-outbreak-response-plan_0.pdf (accessed April 2026).
40. Furlong M, Adamu AM, Hoskins A, et al. Japanese encephalitis enzootic and epidemic risks across Australia. Viruses 2023; 15: 450.
41. Australian Government, Department of Health. Australian immunisation handbook: Japanese encephalitis. Canberra: Australian Government, Department of Health; 2026. Available online at: https://immunisationhandbook.health.gov.au/contents/vaccine-preventable-diseases/japanese-encephalitis (accessed April 2026).
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.