Rosacea: an update on classification, mechanisms and management

Advances in understanding rosacea pathophysiology have led to new targeted therapies directed at neurovascular dysregulation, microbiome dysbiosis and immune dysfunction. Management is guided by phenotype-based classification and includes both traditional and novel pharmacological agents and laser-based therapies, supported by attention to sun protection, diet and the microbiome.
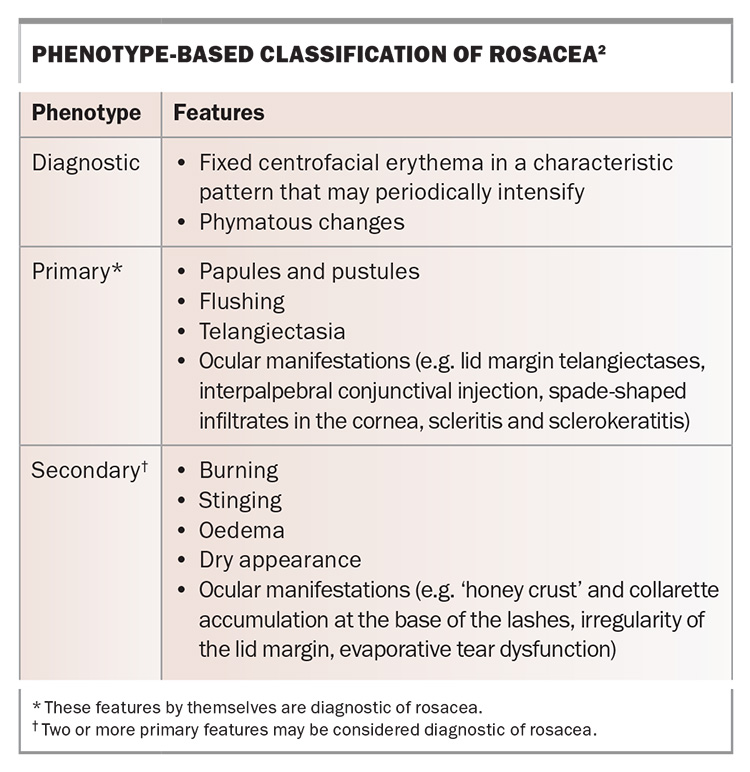
- Rosacea is a common chronic inflammatory dermatosis that is now classified by phenotype rather than subtype, recognising that multiple clinical features may coexist without predictable progression.
- Rosacea pathogenesis is multifactorial, involving immune system dysregulation, neurovascular hyperreactivity and microbial imbalance on a background of genetic susceptibility.
- Dysregulated toll-like receptor 2–cathelicidin signalling and abnormal transient receptor potential channel activation help explain the characteristic features of erythema, flushing, inflammation and phymatous change seen in rosacea.
- Management should be individualised according to phenotype and may include traditional and emerging topical and systemic pharmacological agents, as well as light-based therapies, often used in combination.
- Long-term control also depends on patient education, trigger avoidance, skin barrier support, photoprotection and attention to dietary and environmental factors.
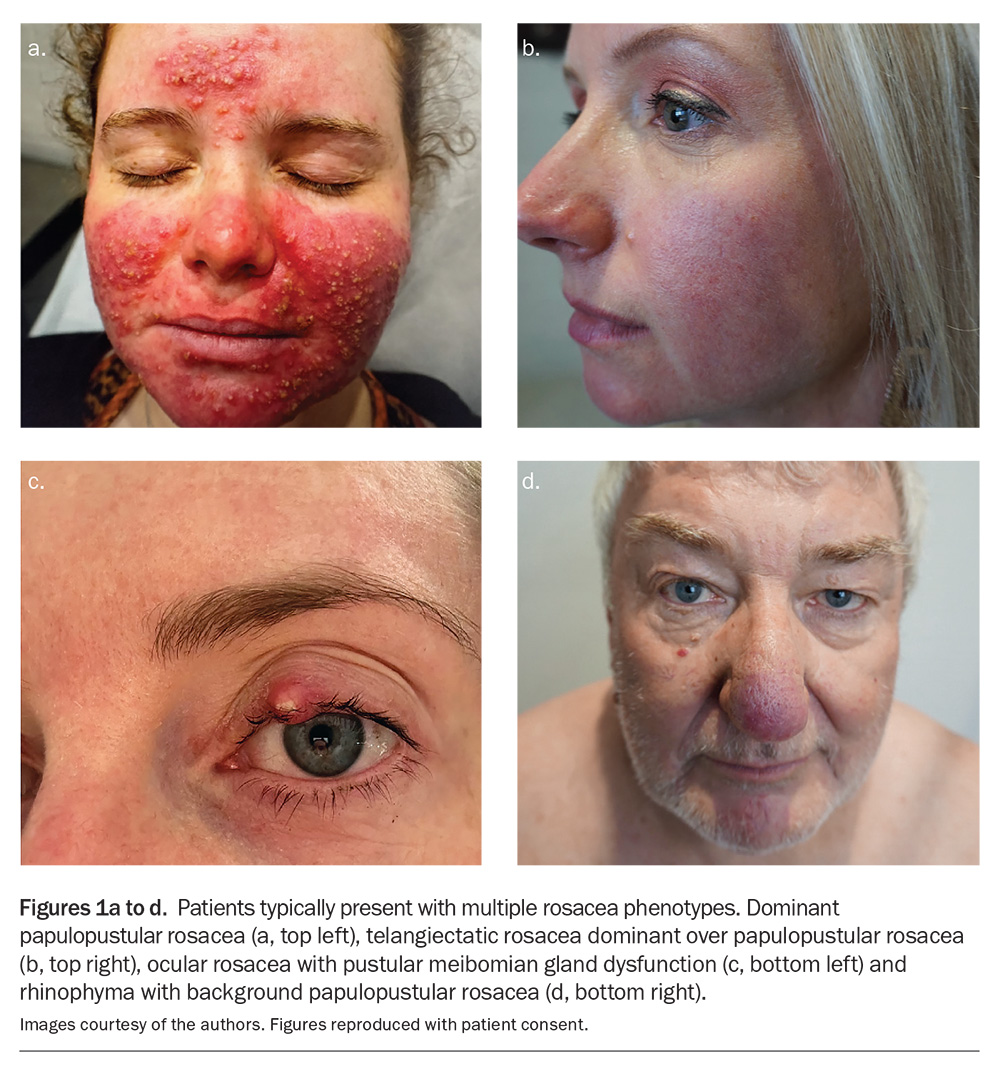
Rosacea affects an estimated 5.46% of the global adult population, with a higher prevalence among fair-skinned individuals.1 The disease is multifactorial in origin and was traditionally classified into four main subtypes: erythematotelangiectatic, papulopustular, phymatous and ocular rosacea. It is now recognised that patients may have multiple morphologies at the same time and that there is no necessary progression from one type to the next. This phenotype-based classification was published by the National Rosacea Society Expert Committee in 2017 and represents a shift from the older subtype-based system to one that focuses on specific, observable characteristics (Table).2 Such an approach allows for personalised treatment that is targeted to an individual’s specific set of symptoms. The range of rosacea phenotypes that may coexist in an individual patient is illustrated in Figures 1a to d.
Despite the common nature of the disease, many patients are unaware of their diagnosis, often until a severe flare necessitates active treatment. Treatment has traditionally been empirical, but advances in dermatological science are fostering a paradigm shift towards targeted and individualised therapy.
Pathophysiology of rosacea
Genetic predisposition is central to rosacea pathogenesis, creating a background of heightened immune and vascular reactivity. Population studies have shown an increased prevalence in people with Fitzpatrick skin type I, and twin studies have demonstrated a 46% genetic contribution.3 Genome-wide association studies have identified links to polymorphisms in genes regulating innate immunity (such as TLR2 and HLA alleles), inflammatory signalling and vascular homeostasis.4 These variants prime individuals for exaggerated immune responses, including overactivation of cathelicidin peptides and kallikrein pathways, as well as abnormal neurovascular signalling leading to flushing and vasodilation. Genetic susceptibility also influences skin barrier function and sebaceous activity, amplifying sensitivity to environmental triggers.
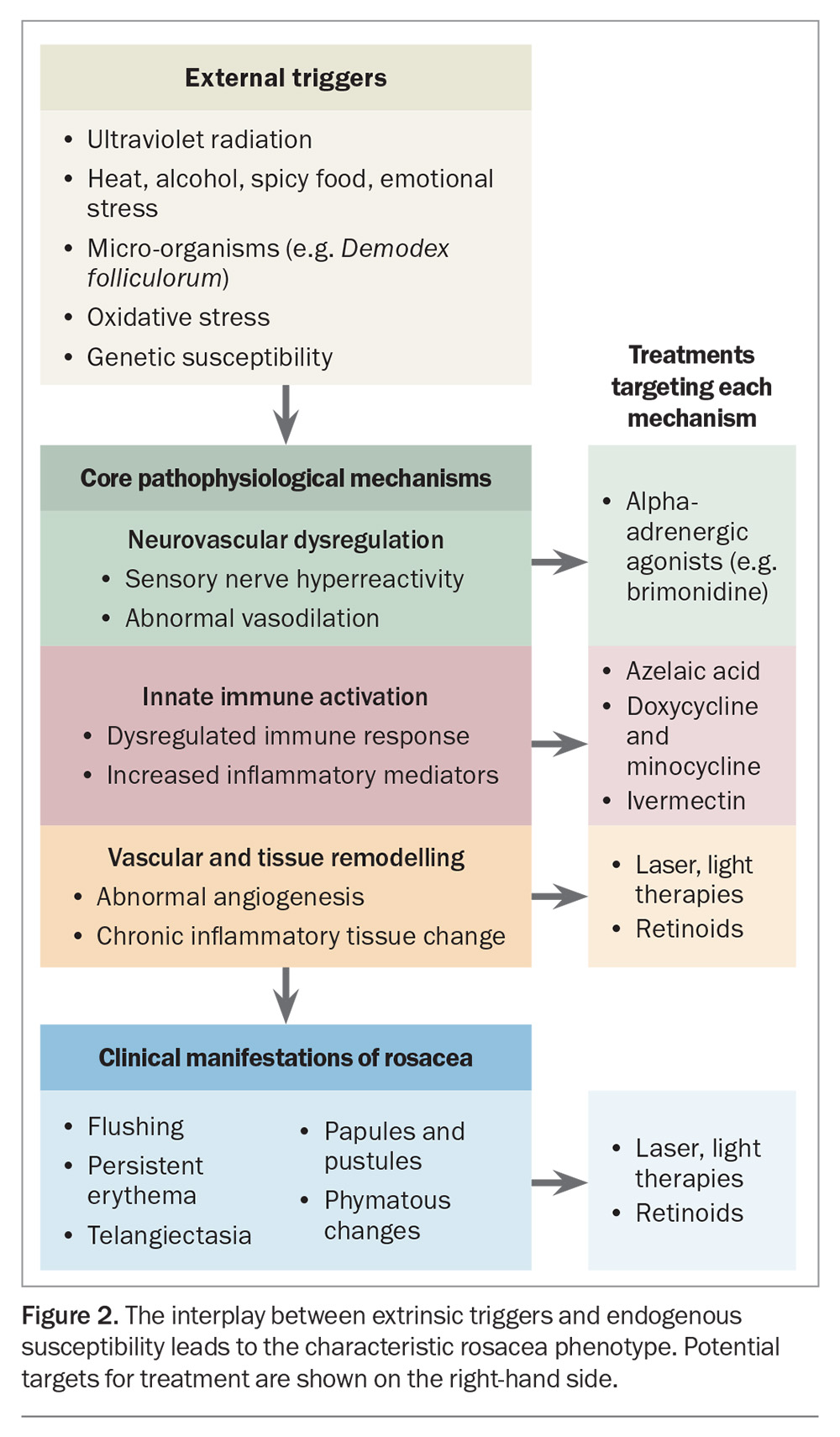
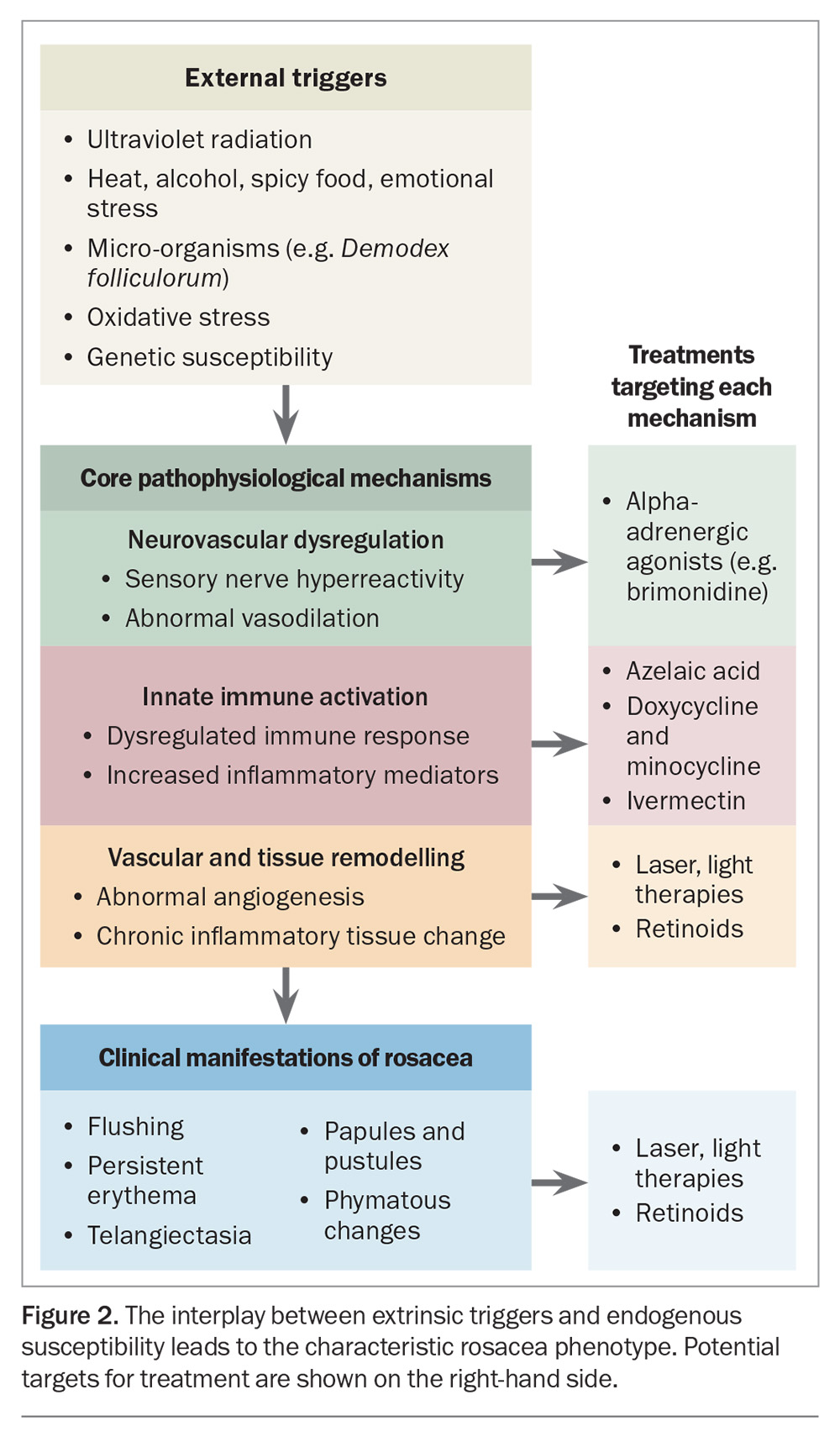
Recent research has furthered our understanding of rosacea as a disorder involving immune system dysregulation, neurovascular hyperreactivity and microbial imbalance on a background of these genetic factors. This complex interplay is illustrated in Figure 2, which shows how external triggers impact endogenous neurovascular and innate pathways to create chronic inflammatory states, vascular instability and the characteristic phenotypic features.
Innate immunity
In rosacea, innate immune dysfunction is central to disease pathogenesis. Keratinocytes and immune cells in rosacea skin express abnormally high levels of toll-like receptor 2 (TLR2). Normally, TLR2 detects microbial products and initiates a controlled immune response. In rosacea, this receptor is upregulated and hyperresponsive, leading to exaggerated downstream signalling. Activation of TLR2 stimulates keratinocytes and resident immune cells to increase the production and abnormal processing of cathelicidin peptides, particularly LL-37, the single human cathelicidin.4
Unlike the antimicrobial peptides generated in normal skin, LL-37 in rosacea is cleaved into shorter, proinflammatory fragments by serine proteases such as kallikrein-5.5 These fragments have potent angiogenic, proinflammatory and fibroblast-activating properties. They promote leukocyte recruitment, cytokine release and vascular endothelial growth, leading to dilated vessels and persistent erythema.6
Sustained LL-37-driven inflammation results in repeated vascular proliferation and extracellular matrix remodelling, contributing to visible telangiectasia and skin oedema. Over time, chronic activation stimulates fibroblast and sebaceous gland hyperplasia, driving phymatous changes such as rhinophyma.7 Thus, dysregulated innate immunity through TLR2–cathelicidin signalling explains the hallmark features of rosacea: inflammation, angiogenesis and tissue hypertrophy, transforming a protective antimicrobial pathway into a chronic driver of cutaneous pathology.
Neurovascular dysregulation
A key component of rosacea pathogenesis is neurovascular dysregulation, which explains the hallmark symptoms of flushing and persistent erythema. In rosacea, sensory nerve endings in the skin express increased levels of transient receptor potential (TRP) channels, such as TRP vanilloid-1 and TRP ankyrin-1. These ion channels are abnormally sensitive to exogenous triggers including heat, spicy foods, alcohol and emotional stress.8 When activated, TRP channels cause rapid depolarisation of sensory neurons and release vasoactive neuropeptides such as substance P, calcitonin gene-related peptide and vasoactive intestinal peptide. These mediators induce arteriolar vasodilation and increase vascular permeability, resulting in visible flushing and oedema.8
Repeated episodes of neurogenic vasodilation promote chronic vascular remodelling, with the development of telangiectasia and persistent erythema.9 Thus, heightened TRP channel activity links environmental and emotional stimuli to exaggerated vascular responses, forming the neurovascular arm of rosacea pathophysiology and reinforcing the cycle of chronic skin inflammation and vascular change. Therapies such as topical brimonidine (an alpha agonist) and microbotox work to relax vascular smooth muscle and prevent the exaggerated vascular response seen phenotypically.
Microbial imbalance
Two micro-organisms, Demodex folliculorum and Helicobacter pylori, have been implicated as contributors to rosacea.
D. folliculorum is a mite that inhabits pilosebaceous units, particularly on the face. At low densities, the mites suppress TLR2 expression to evade detection, but at high densities, they upregulate TLR2 and trigger the release of inflammatory cytokines such as interleukin (IL)-8 and tumour necrosis factor-alpha.10,11 The mite’s chitin exoskeleton further stimulates innate immunity, and dying mites release Bacillus oleronius, a bacterium that produces antigenic proteins that amplify inflammation and erythema.5,12 Patients with rosacea consistently demonstrate higher D. folliculorum densities than controls.11 Treatments such as ivermectin and doxycycline reduce mite and bacterial loads while also exerting anti-inflammatory effects, although a direct causal role for D. folliculorum remains unproven. D. folliculorum is not routinely screened for in rosacea.
H. pylori, a gastric pathogen, has also been weakly linked to rosacea, but the effects of eradication on disease control are inconsistent and this bacterium is therefore not routinely screened for in rosacea.11 Screening for H. pylori should be symptom driven in cases accompanied by gastrointestinal bloating, reflux or diarrhoea.
Together, D. folliculorum and H. pylori may act as amplifiers of inflammation and vascular dysfunction, but their exact causal roles remain debated.
Pharmacological management
Current pharmacological treatments can be grouped into traditional therapies with established clinical use and newer investigational agents that reflect advances in pathophysiological understanding.
Traditional therapies
Adrenergic receptor modulators
Topical alpha-adrenergic agonists such as oxymetazoline and brimonidine induce vasoconstriction of superficial cutaneous vessels, providing temporary relief of persistent erythema for up to 12 hours. Oxymetazoline is not commercially available in Australia, although it was under TGA evaluation in 2025, with potential availability in coming years.
Brimonidine 3.3 mg/g gel has been TGA approved for the treatment of facial erythema of rosacea in adult patients since 2014. Its use has been limited by rebound erythema, a side effect typically evident in the first week of use.13 When this side effect does not occur, many patients find once-daily application of brimonidine helpful in controlling central facial erythema and flushing, and it can be an important adjunct to a rosacea treatment plan.
In contrast, systemic beta-adrenergic antagonists (beta blockers; e.g. carvedilol, propranolol) reduce flushing and erythema by inhibiting vasodilatory beta receptors. Carvedilol’s additional antioxidant properties may enhance its efficacy.14
Azelaic acid
This naturally occurring dicarboxylic acid is effective for mild forms of rosacea. Its actions include downregulation of the cathelicidin antimicrobial peptide gene and kallikrein-5, inhibition of nicotinamide adenine dinucleotide phosphate oxidase to reduce neutrophil-derived reactive oxygen species, and suppression of IL-1-beta and tumour necrosis factor-alpha.15
It is available as an over-the-counter medicine in 20% lotion formulations used twice daily, in 15% gel formulations combined with benzoic acid used once to twice daily or as commercial 10% cream products, sometimes combined with other ingredients (e.g. salicylic acid), used up to twice daily. These formulations provide multiple options for patients with mild rosacea and a dominant papulopustular phenotype.
Calcineurin inhibitors
Agents such as ciclosporin, pimecrolimus and tacrolimus reduce T-cell-mediated cytokine release. Ciclosporin ophthalmic emulsions are widely used for ocular rosacea, whereas topical pimecrolimus and tacrolimus are often too irritating to provide clinical benefit.
Antiparasitic and antibiotic therapies
Ivermectin combines antiparasitic activity against D. folliculorum with anti-inflammatory actions, lowering LL-37 and cytokine expression.16 Metronidazole, although originally developed as an antibiotic, improves rosacea primarily through reactive oxygen species inhibition and T-cell modulation rather than through antimicrobial effects.17
Both ivermectin and metronidazole are available topically as once-daily field (not spot) treatments. Treatment is individualised, but often involves an active treatment phase followed by review after three months. If symptoms are controlled, treatment can then be pulsed in three-month cycles, with review every six to 12 months. Ivermectin 1% cream applied daily to dry skin has been shown to be superior to topical metronidazole 0.75% cream applied twice daily, with additional long-term maintenance benefit.18 Recent descriptions of topical ivermectin use on the upper and lower eyelid margins provide a promising treatment option in cases of ocular rosacea.19
Retinoids
Topical adapalene and systemic isotretinoin are options for refractory papulopustular and severe phymatous rosacea. Their benefits may arise from TLR2 modulation, reactive oxygen species suppression and connective tissue remodelling. Studies have shown that adapalene reduces reactive oxygen species production by neutrophils, whereas isotretinoin has been shown to reduce TLR2 expression in monocytes. Retinoids have a tendency to irritate rosacea-prone skin and benefit only a small minority of patients with a dominant pustular phenotype. Topical adapalene 0.1%, used weekly initially and increased to nightly if tolerated, requires a prescription in Australia. Oral isotretinoin (5 to 10 mg daily for a minimum of 12 months) requires a prescription from a dermatologist.
New treatment agents
Recent scientific advances have introduced novel compounds designed to intervene at key molecular checkpoints in rosacea pathogenesis.
Targeted anti-inflammatory pathways under investigation
- ACU-D1, a proteasome inhibitor, suppresses nuclear factor kappa B signalling, lowering IL-1-beta, IL-6 and IL-8, with promising lesion clearance in phase II trials.22
- DMT310, derived from Spongilla lacustris, downregulates IL-17A and IL-17F and reduces inflammatory lesions in early studies (clinical trial number: NCT05108025).
- Secukinumab, an anti-IL-17 monoclonal antibody, has shown modest reductions in lesion counts, suggesting a potential role for cytokine blockade (clinical trial number: NCT03079531).
- Phosphodiesterase-4 inhibitors (e.g. PF-07038124, roflumilast) are under investigation for their anti- inflammatory actions, extrapolated from atopic dermatitis and psoriasis (clinical trial numbers: NCT06013371 and NCT05278624).
Microbiome and novel mechanistic agents under investigation
- B244 spray, containing Nitrosomonas eutropha, reduces erythema through nitric oxide-mediated immunomodulation (clinical trial number: NCT03590366).
- CGB-400, composed of choline and geranic acid, inhibits kallikrein-5, thereby preventing cathelicidin overactivation (clinical trial number: NCT04508205).
- Omiganan, an antimicrobial peptide, has demonstrated lesion reduction via putative immunomodulation (clinical trial number: NCT02547441).
- Rifaximin, a nonabsorbed antibiotic, may improve rosacea in patients with small intestinal bacterial overgrowth (clinical trial number: NCT05150587).
Reformulated or repurposed dermatologic agents
- Encapsulated benzoyl peroxide (5%) reduces papulopustular lesions while limiting irritation, and received US Food and Drug Administration approval in 2023. It is available over the counter in Australia.
- Sarecycline, a narrow-spectrum tetracycline, reduces inflammatory lesions while minimising broad-spectrum antimicrobial effects.23 This agent is not currently approved by the TGA but is in use in other countries.
- Minocycline has emerged in multiple formulations – topical gel, topical foam and extended-release oral capsule – demonstrating superior outcomes to doxycycline in recent trials.24 These formulations are not currently available in Australia.
- Timolol, a topical beta blocker, reduces erythema, as well as vascular endothelial growth factor and matrix metalloproteinase activity. Studies are underway to investigate efficacy in rosacea (clinical trial number: NCT02774590). It is available as a compounded medication in Australia for unrelated conditions.
- Lotilaner, an antiparasitic targeting Demodex mites, is under investigation (clinical trial number: NCT05838170).
- Trametinib, a mitogen-activated protein kinase inhibitor with antiangiogenic properties, is under investigation (clinical trial number: NCT05616923).
Combination therapies
Rosacea pathogenesis involves multiple overlapping pathways; therefore, combination approaches are increasingly preferred and treatments are best individualised according to the rosacea phenotypic features unique to each patient, as illustrated in Figure 2.
Other management approaches
Microbotox
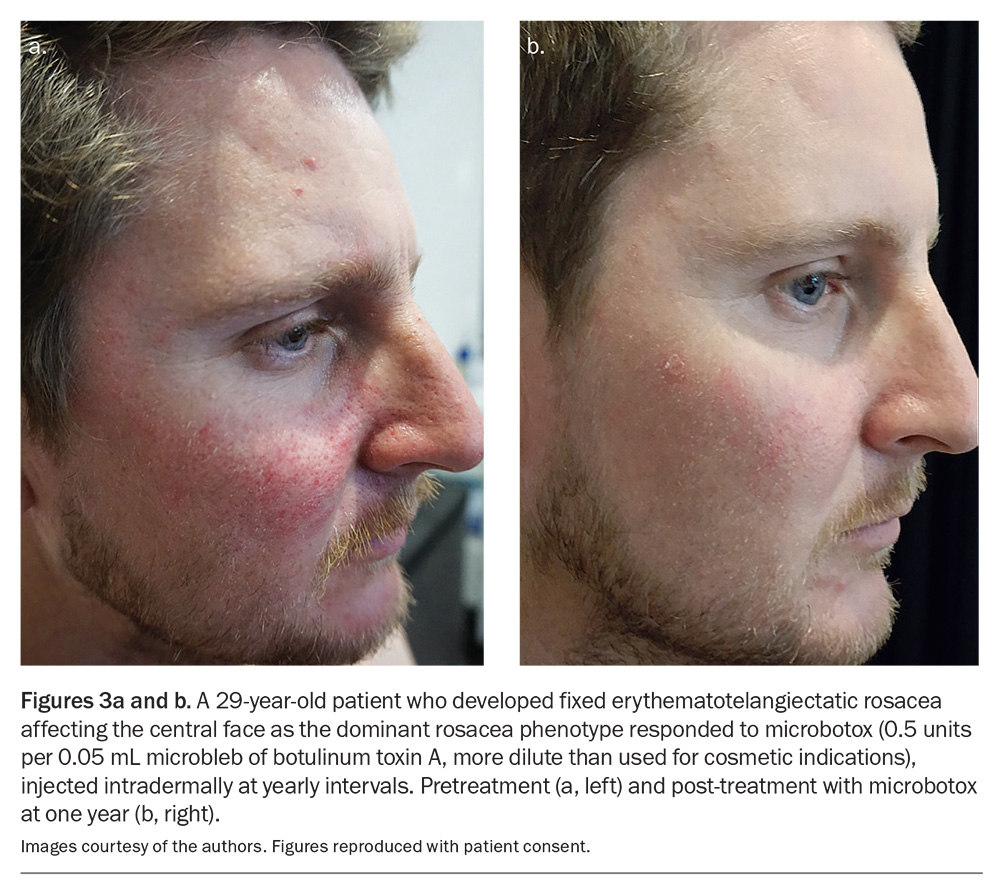
Microbotox describes the intradermal injection of botulinum toxin type A, used off label as an adjunctive treatment for central facial erythematous rosacea that is resistant to other therapies. This approach targets neurovascular and neurogenic inflammatory pathways while avoiding the muscular effects seen in cosmetic use.25 Growing clinical experience supports this modality as a yearly treatment option when other pharmacological agents have failed.
The clinical response to intradermal microbotox in a patient with dominant erythematotelangiectatic rosacea is shown in Figures 3a and b.
Laser options
Photodynamic therapy and laser modalities represent nonpharmacological options in rosacea management, targeting vascular and inflammatory components. Photodynamic therapy, typically using topical 5-aminolevulinic acid with light activation, has shown efficacy in reducing inflammatory papules and pustules. Proposed mechanisms include selective destruction of sebaceous glands, reduction of Demodex density and downregulation of inflammatory mediators.26 However, evidence is mixed; although some trials demonstrate clinical improvement, others report limited benefit and frequent side effects such as pain, erythema and post-treatment photosensitivity.27
Laser- and light-based therapies, particularly pulsed dye laser, potassium titanyl phosphate laser, neodymium-doped yttrium aluminium garnet laser and intense pulsed light, are better supported by evidence. These treatments target oxyhaemoglobin, inducing selective photothermolysis of superficial blood vessels, thereby reducing persistent erythema and telangiectasia. Multiple randomised controlled trials confirm significant, durable vascular improvement and patient satisfaction, especially with repeated sessions.28-31
Carbon dioxide laser is an ablative laser technique used in cases of moderate to severe phymatous changes with tissue hypertrophy.32,33 Pretreatment regimens, often involving long-term retinoids, and topical maintenance therapy are usually required. Layer-by-layer debulking with preservation of pilosebaceous units can be cosmetically transformative in this phenotype of rosacea.
Microbiome modulation and probiotics
Emerging evidence highlights the role of cutaneous and gut microbiota in rosacea pathogenesis. Probiotic supplementation and topical probiotics are being investigated for their potential to restore microbial homeostasis and reduce inflammation.
Clinical trials remain limited in number and size, but there is emerging evidence that combining antibiotics such as doxycycline with probiotics, including Lactobacillus and Bifidobacterium strains, can improve rosacea symptoms through tumour necrosis factor-alpha inhibition.34 Routine gut microbiome testing is not recommended in the work-up of rosacea and it is best viewed as a disease modifier rather than a treatment target in isolation.
Topical probiotics have also shown some benefit in skin barrier repair and anti-inflammatory activity, and may, in time, add to the current therapeutic armamentarium.35
Skincare
Sun protection is the cornerstone of rosacea management, as ultraviolet exposure is a common trigger for flares and persistent erythema. Patients should be advised to use a broad-spectrum sun protection factor 50+ sunscreen daily, preferably a physical or hybrid formulation containing zinc oxide, titanium dioxide or both, which are better tolerated by rosacea-prone skin.36
Skincare should be simple and barrier focused: gentle soap-free cleansers, regular moisturiser with barrier-restoring ingredients such as ceramides, and avoidance of alcohol-based products, exfoliants and fragranced cosmetics. Introducing one product at a time at weekly intervals assists in identifying irritants. Consistent photoprotection and a gentle skincare routine are vital to improving disease control and working synergistically to promote treatment efficacy.
Dietary factors
Dietary factors long recognised as potential rosacea triggers have vasoactive amine content hypothesised to stimulate TRP receptors, thereby promoting vasodilation and skin inflammation.37 Common triggers to limit include alcohol, cinnamaldehyde- containing foods (e.g. tomatoes, chocolate, cinnamon), spicy foods, hot beverages that induce vasodilation and histamine-rich foods (e.g. wine, aged cheese, cured meats).38
Although caffeine has traditionally been described as a rosacea trigger, it has recently been shown to have an inverse association, attributed to its vasodilatory effects and low-level skin immune suppression.39 Dietary advice should be individualised, but several patterns are consistent.
Patients should be encouraged towards an anti-inflammatory diet with regular intake of omega-3 fatty acids, vegetables, whole grains and lean proteins. Advise a food-symptom diary to identify personal triggers and reinforce that the diet supports, but does not replace, medical treatment of rosacea.
When to refer to a dermatologist
It is reasonable to consider referral of a patient with rosacea to a dermatologist for the following presentations:
- disease that worsens or does not respond to treatment over a six- to 12-week trial interval
- severe disease with phymatous change at presentation
- disease that severely impacts quality of life, as this may require a combination of treatment options and aggressive early treatment
- coexisting multiple phenotypic clinical presentations, which may necessitate concurrent combination treatment.
Conclusion
Rosacea management is undergoing a transformation, fuelled by an improved understanding of its complex pathophysiology. The integration of new topical and systemic agents, technological innovations and personalised strategies holds great promise for improving patient outcomes. Continued research into the molecular mechanisms of rosacea and long-term studies of new treatments will be crucial to refining care and maximising therapeutic success.
Successful management of this condition requires an individualised treatment plan tailored to the patient’s phenotype, with education about the multiple factors contributing to the underlying pathophysiology. Social media can rapidly spread unverified or anecdotal ‘cures’ for rosacea, leading patients to try ineffective or harmful treatments. This misinformation can delay proper medical care, worsen symptoms and increase anxiety or mistrust of evidence-based dermatological advice. The chronic nature of this disease necessitates a strong commitment to treatment, maintenance of the skin barrier and attention to environmental, dietary and genetic factors. A strong doctor–patient relationship, supported by reliable resources such as DermNet and the American Acne and Rosacea Society, is vital to treatment success. MT
COMPETING INTERESTS: Dr DeAmbrosis has received payment or honoraria for consulting and speaking for UCB and L'Oréal. Dr See has received honoraria for consulting and speaking for Galderma, L’Oréal, SunPharma and Viatris; is co-chair of the All About Acne group and member of the Public Affairs Committee of the Australasian College of Dermatology.
References
1. Gether L, Overgaard L, Egeberg A. Incidence and prevalence of rosacea: a systematic review and meta-analysis. Br J Dermatol 2018; 170: 282-289.
2. Gallo RL, Granstein RD, Kang S, et al. Standard classification and pathophysiology of rosacea: the 2017 update by the National Rosacea Society Expert Committee. J Am Acad Dermatol 2018; 78: 148-155.
3. Aldrich N, Gerstenblith M, Fu P, et al. Genetic vs environmental factors that correlate with rosacea: a cohort-based survey of twins. JAMA Dermatol 2015; 151: 1213-1219.
4. Geng RSQ, Bourkas AN, Mufti A, Sibbald RG. Rosacea: pathogenesis and therapeutic correlates. J Cutan Med Surg 2024; 28: 178-189.
5. Two AM, Wu W, Gallo RL, Hata TR. Rosacea: part I. Introduction, categorization, histology, pathogenesis, and risk factors. J Am Acad Dermatol 2015; 72: 749-758.
6. Yamasaki K, Di Nardo A, Bardan A, et al. Increased serine protease activity and cathelicidin promotes skin inflammation in rosacea. Nat Med 2007; 13: 975-980.
7. Dick MK, Patel BC. Rhinophyma. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026. Available online at: https://www.ncbi.nlm.nih.gov/books/NBK544373/ (accessed March 2026).
8. Buddenkotte J, Steinhoff M. Recent advances in understanding and managing rosacea. F1000Res 2018; 7: F1000 Faculty Rev-1885.
9. Del Rosso JQ. Advances in understanding and managing rosacea: part 1: connecting the dots between pathophysiological mechanisms and common clinical features of rosacea with emphasis on vascular changes and facial erythema. J Clin Aesthet Dermatol 2012; 5: 16-25.
10. Forton FMN. The pathogenic role of Demodex mites in rosacea: a potential therapeutic target already in erythematotelangiectatic rosacea? Dermatol Ther (Heidelb) 2020; 10: 1229-1253.
11. Casas C, Paul C, Lahfa M, et al. Quantification of Demodex folliculorum by PCR in rosacea and its relationship to skin innate immune activation. Exp Dermatol 2012; 21: 906-910.
12. Lacey N, Delaney S, Kavanagh K, Powell FC. Mite-related bacterial antigens stimulate inflammatory cells in rosacea. Br J Dermatol 2007; 157: 474-481.
13. Routt E, Levitt J. Rebound erythema and burning sensation from a new topical brimonidine tartrate gel 0.33%. JAAD 2014; 70: e37-38.
14. Dandona P, Ghanim H, Brooks DP. Antioxidant activity of carvedilol in cardiovascular disease. J Hypertens 2007; 25: 731-741.
15. Coda AB, Hata T, Miller J, et al. Cathelicidin, kallikrein 5, and serine protease activity is inhibited during treatment of rosacea with azelaic acid 15% gel. J Am Acad Dermatol 2013; 69: 570-577.
16. Mendieta Eckert M, Landa Gundin N. Treatment of rosacea with topical ivermectin cream: a series of 34 cases. Dermatol Online J 2016; 22: 13030/qt9ks1c48n.
17. Narayanan S, Hünerbein A, Getie M, Jäckel A, Neubert RH. Scavenging properties of metronidazole on free oxygen radicals in a skin lipid model system. J Pharm Pharmacol 2007; 59: 1125-1130.
18. Schaller M, Dirschka T, Kemény L, Briantais P, Jacovella J. Superior efficacy with ivermectin 1% cream compared to metronidazole 0.75% cream contributes to a better quality of life in patients with severe papulopustular rosacea: a subanalysis of the randomized, investigator-blinded ATTRACT study. Dermatol Ther (Heidelb) 2016; 6: 427-436.
19. Smith M, Wolffsohn JS, Chiang JCB. Topical ivermectin 1.0% cream in the treatment of ocular demodicosis. Cont Lens Anterior Eye 2024; 47: 102099.
20. Two AM, Wu W, Gallo RL, Hata TR. Rosacea: part II. Topical and systemic therapies in the treatment of rosacea. J Am Acad Dermatol 2015; 72: 761-770.
21. Bohne M, Struy H, Gerber A, Gollnick H. Effects of retinoids on the generation of neutrophil-derived reactive oxygen species studied by EPR spin trapping techniques. Inflamm Res 1997; 46: 423-424.
22. Jackson JM, Coulon R, Arbiser JL. Evaluation of a first-in-class proteasomeinhibitor in patients with moderate to severe rosacea. J Drugs Dermatol 2021; 20: 660-664.
23. Choe J, Barbieri JS. Emerging medical therapies in rosacea: a narrative review. Dermatol Ther (Heidelb) 2023; 13: 2933-2949.
24. Gold LS, Yamauchi P, Dirschka T, Tsianakas A, Dhawan S, Sidgiddi S. Impact of oral DFD-29, a low-dose formulation of minocycline, on quality of life in patients with rosacea: results of two phase 3 randomized controlled trials. J Clin Aesthet Dermatol 2025; 18: 66-72.
25. Calvisi L, Diaspro A, Sito G. Microbotox: a prospective evaluation of dermatological improvement in patients with mild-to-moderate acne and erythematotelangiectatic rosacea. J Cosmet Dermatol 2022; 21: 3747-3753.
26. Yang J, Liu X, Cao Y, et al. 5-Aminolevulinic acid photodynamic therapy versus minocycline for moderate-to-severe rosacea: a single-center, randomized, evaluator-blind controlled study. J Am Acad Dermatol 2023; 89: 711-718.
27. Wan MT, Lin JY. Current evidence and applications of photodynamic therapy in dermatology. Clin Cosmet Investig Dermatol 2014; 7: 145-163.
28. Husein-ElAhmed H, Steinhoff M. Light-based therapies in the management of rosacea: a systematic review with meta-analysis. Int J Dermatol 2022; 61: 216-225.
29. Salem SA, Abdel Fattah NS, Tantawy SM, El-Badawy NM, Abd El-Aziz YA. Neodymium-yttrium aluminum garnet laser versus pulsed dye laser in erythemato-telangiectatic rosacea: comparison of clinical efficacy and effect on cutaneous substance (P) expression. J Cosmet Dermatol 2013; 12: 187-194.
30. Papageorgiou P, Clayton W, Norwood S, Chopra S, Rustin M. Treatment of rosacea with intense pulsed light: significant improvement and long-lasting results. Br J Dermatol 2008; 159: 628-632.
31. Uebelhoer NS, Bogle MA, Stewart B, Arndt KA, Dover JS. A split-face comparison study of pulsed 532-nm KTP laser and 595-nm pulsed dye laser in the treatment of facial telangiectasias and diffuse telangiectatic facial erythema. Dermatol Surg 2007; 33: 441-448.
32. Olafsdottir B, Jebril W, Curman P, Bachar-Wikström E, Wikström JD. Long-term satisfaction with CO2 laser treatment for moderate to major rhinophyma: a single-centre study. Acta Derm Venereol 2025; 105: adv41335.
33. Serowka KL, Saedi N, Dover JS, Zachary CB. Fractionated ablative carbon dioxide laser for the treatment of rhinophyma. Lasers Surg Med 2014; 46: 8-12.
34. Yu J, Duan Y, Zhang M, Li Q, et al. Effect of combined probiotics and doxycycline therapy on the gut-skin axis in rosacea. mSystems 2024; 9: e0120124.
35. Habeebuddin M, Karnati RK, Shiroorkar PN, et al. Topical probiotics: more than a skin deep. Pharmaceutics 2022; 14: 557.
36. Morgado-Carrasco D, Granger C, Trullas C, Piquero-Casals J. Impact of ultraviolet radiation and exposome on rosacea: key role of photoprotection in optimizing treatment. J Cosmet Dermatol 2021; 20: 3415-3421.
37. Weiss E, Katta R. Diet and rosacea: the role of dietary change in the management of rosacea. Dermatol Pract Concept 2017; 7: 31-37.
38. Searle T, Ali FR, Carolides S, Al-Niaimi F. Rosacea and diet: what is new in 2021? J Clin Aesthet Dermatol 2021; 14: 49-54.
39. Li S, Chen ML, Drucker AM, Cho E, Geng H, Qureshi AA, Li WQ. Association of caffeine intake and caffeinated coffee consumption with risk of incident rosacea in women. JAMA Dermatol 2018; 154: 1394-1400.
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.