From sun damage to keratinocyte skin cancer – practical guidance for GPs
Australia has one of the highest rates of keratinocyte skin cancers worldwide, placing a significant clinical and economic burden on the healthcare system. GPs play a crucial role in early detection, patient education, referral and management of these cancers. This article outlines the presentation, diagnosis and management of actinic keratoses, squamous cell carcinoma and basal cell carcinoma.
- Basal cell carcinoma and cutaneous squamous cell carcinoma are the most common cancers in Australia, imposing a significant burden on both patients and the healthcare system.
- Actinic keratoses are traditionally considered pre-neoplastic lesions. Diagnosis is primarily clinical, with biopsy reserved for atypical or suspicious lesions. Treatment options include lesion-directed and field-directed therapies.
- Cutaneous squamous cell carcinoma can metastasise. Surgery is the mainstay of treatment, whereas specialised margin-controlled surgery, radiotherapy or systemic therapy is used for high-risk disease.
- Basal cell carcinoma is the most common skin cancer. It rarely metastasises but can be locally destructive, with surgical excision as the mainstay of treatment and nonsurgical options for selected low-risk lesions.
- GPs play a central role in prevention, early detection, management and timely referral of high-risk or complex cases.
Australia has one of the highest incidences of skin cancer globally, with basal cell carcinoma (BCC) and cutaneous squamous cell carcinoma (cSCC) – together referred to as keratinocyte skin cancers – accounting for the vast majority.1 Formerly known as nonmelanoma skin cancers, these conditions impose a substantial clinical and economic burden in Australia, with an estimated health expenditure of $1.3 billion in 2018 to 2019, compared with $0.4 billion for melanoma.2 Mandated reporting of keratinocyte cancers is not required in Australia, except in Tasmania, making it difficult to obtain accurate data regarding the true burden of disease.1 Nevertheless, it is estimated that 69% of Australians will undergo at least one excision for a keratinocyte cancer in their lifetime, and the incidence has risen by about 2 to 6% over the past 30 years.1
Prevention, early diagnosis and familiarity with treatment options and pathways for these cancers equip GPs to support primary prevention, facilitate early detection and prompt intervention, enhance patient care and appropriately refer complex or high-risk cases to a specialist. This article reviews the clinical features, diagnosis and management of keratinocyte skin cancers, including actinic keratoses, cSCC and BCC.
Actinic keratoses
Actinic keratoses, also referred to as solar keratoses, are lesions resulting from cumulative ultraviolet (UV) damage to epidermal keratinocytes.3,4 They signal an increased risk of developing cSCC and, although traditionally seen as pre-neoplastic, are sometimes regarded as in situ neoplasms.3,4
Presentation and diagnosis
Lesions most commonly occur on sun-exposed areas such as the face, scalp, ears and dorsal forearms.3,4 Although the annual risk of malignant transformation per lesion is estimated at 0.075 to 0.1%, some studies suggest this could reach 10% over a decade.3 Conversely, up to 70% of actinic keratoses may regress spontaneously within five years.3 There are no reliable clinical markers to predict which actinic keratoses will progress to cSCC.3
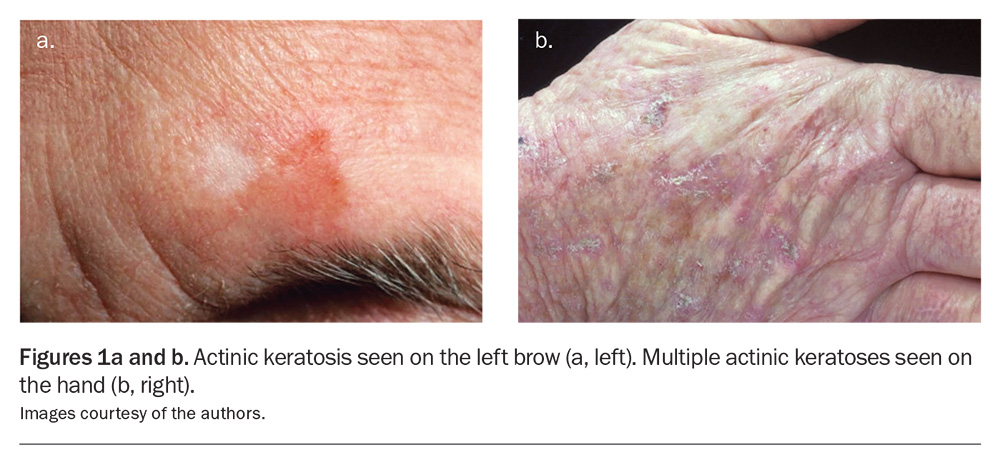
Actinic keratoses exhibit a wide range of clinical appearances but classically present as rough, scaly macules, papules or plaques on an erythematous base (Figures 1a and b).3,4 Variants may be pigmented, hyperkeratotic or atrophic.3,4 Actinic keratoses are usually asymptomatic but may sting, burn or itch.4
Diagnosis is primarily clinical, with biopsy reserved for atypical lesions or when differential diagnoses, including cSCC, cannot be excluded using examination and dermoscopy.4 Key features suggesting transformation to cSCC include tenderness, bleeding, inflammation or rapid thickening.4 Histologically, actinic keratoses are confined to the lower epidermis, whereas cSCC demonstrates full-thickness keratinocyte atypia invading the dermis.3,4
Treatment
Treatment of actinic keratoses follows local and international guidelines, including recommendations from Cancer Council Australia.5 Individuals who are immunosuppressed, such as solid organ transplant recipients, should receive more aggressive treatment because of a higher risk of transformation to cSCC.4
GPs play a crucial role in initiating these therapies, referring patients to dermatologists as needed, providing counselling and managing expectations regarding the typical inflammatory response, which peaks between seven and 14 days. Pretreatment education, including visual examples of treatment reactions, improves adherence and outcomes.
Lesion-directed therapy
Isolated actinic keratoses are typically treated with cryotherapy, using one freeze–thaw cycle of five to 10 seconds.3 Expected side effects include pain, redness, swelling and, sometimes, blistering.3 Cryotherapy should be avoided when the diagnosis is uncertain, used with caution on the lower legs due to delayed healing and may cause hypopigmentation or postinflammatory hyperpigmentation in susceptible individuals due to cold-induced melanocyte damage.3,4
Topical 5-fluorouracil 4% cream (once daily), 5% cream (once or twice daily) or 0.5% with 10% salicylic acid solution (once daily), for three to four weeks, is an effective nonprocedural alternative.3,4 Curettage, shave excision and electrodesiccation are additional options for thicker lesions or when histological confirmation is needed.3,4
Field-directed therapy
For areas with multiple or indistinct lesions, field-directed therapy addresses both clinical and subclinical disease. This approach is based on the concept of field cancerisation, in which chronic UV exposure causes widespread DNA damage in the epidermis of chronically sun-exposed skin, including areas that appear clinically normal.3,4 As a result, patients often develop additional lesions in these areas over time and are at increased risk of cSCC.3,4
Field-directed therapy aims to reduce the overall risk of malignant transformation. Options include 5-fluorouracil 4% (once daily) or 5% creams, imiquimod 5% cream, diclofenac 3% in 2.5% hyaluronic acid gel and photodynamic therapy.3,4 Tirbanibulin 1% ointment has recently been approved by the TGA but is not yet commercially available. Fluorouracil is cost effective and widely used in primary care. Recent evidence suggests that combining fluorouracil with calcipotriol is effective for field treatment while minimising local skin reactions; however, this combination therapy is not commercially available in Australia and must be compounded.6 Photodynamic therapy, using methyl aminolevulinate or aminolaevulinic acid, is largely confined to dermatology clinics because of specialised equipment requirements and may be useful for actinic keratoses and superficial BCCs in cosmetically sensitive areas.3,4 A recent modification of this technique uses daylight in the visible spectrum as the activating light source.7
Squamous cell carcinoma
cSCC is the second most common skin cancer in Australia, with estimated national incidence rates ranging from 279 to 593 cases per 100,000 people per year.8 However, because of the absence of mandated registry data, these figures likely underestimate the true burden of disease. Although prognosis is generally excellent with excision or other locally destructive therapies, cSCC has metastatic potential, which has a significantly deleterious effect on prognosis.8
Risk factors
The incidence of cSCC increases with age and is consistently higher in men across all age groups.9 Other risk factors include fair skin types, cumulative UV exposure, family history of skin cancer, chronic inflammation, trauma, burns or scarring.9 Individuals who are immunosuppressed – including those with chronic lymphocytic leukaemia, HIV or solid organ transplants – are at significantly increased risk of cSCC and often develop more aggressive disease.9 Infection with oncogenic strains of human papillomavirus, particularly in the periungual and anogenital regions, is also implicated.9
Presentation and diagnosis
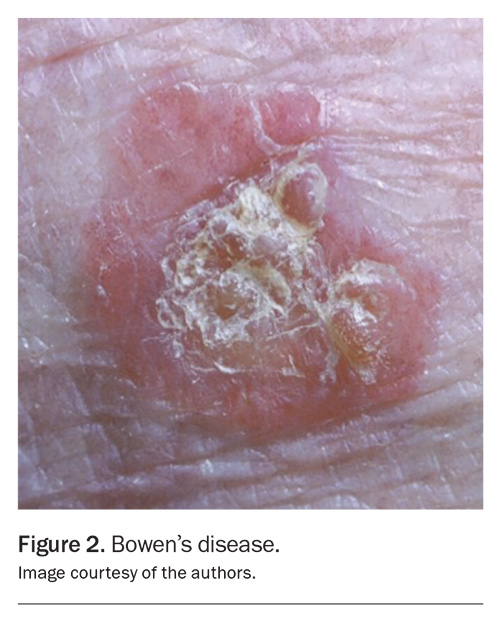
cSCC spans a broad clinical spectrum. Bowen’s disease (cSCC in situ) typically presents as a well-defined, sharply demarcated, erythematous, scaly plaque (Figure 2).10 Pigmented variants can mimic melanoma or seborrhoeic keratosis. Without treatment, 3 to 5% of Bowen’s disease progresses to invasive cSCC.10
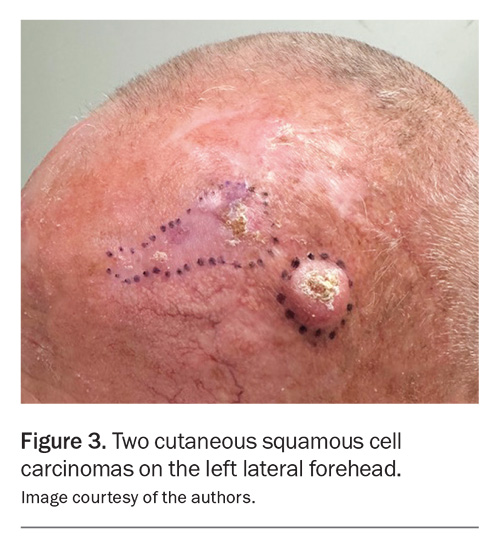
Invasive cSCC classically presents as an erythematous, often hyperkeratotic, papule or nodule that may ulcerate, bleed or be tender on palpation (Figure 3).9,11 In men, cSCC most frequently affects skin on the head and neck, whereas in women, the upper limbs are more commonly involved.11 Dermoscopy may reveal white circles, white structureless areas, glomerular vessels or hairpin vessels.11 Clinical examination should include lymph node palpation, with suspicious lymphadenopathy further evaluated using fine-needle aspiration to assess for metastatic spread.11
Diagnosis is confirmed via skin biopsy, which must be sufficiently deep to evaluate dermal invasion.11 Pathology reports should follow a structured format and include tumour subtype, degree of differentiation, depth of invasion and evidence of perineural, lymphatic or vascular invasion. These features not only confirm the diagnosis but also guide prognosis, risk stratification and management decisions.11
Treatment
Treatments can be guided by the Cancer Council Australia’s Clinical Practice Guidelines for Keratinocyte Cancer.5
Bowen’s disease
Lesion-directed treatments similar to those used for actinic keratoses may be considered for Bowen's disease, including cryotherapy, fluorouracil, diclofenac in hyaluronic acid gel, imiquimod or photodynamic therapy, depending on disease extent, lesion site and patient factors. In higher risk cases, surgical excision or radiotherapy may be more appropriate.10
Surgery
Surgery remains the mainstay of cSCC treatment. Low-risk tumours are commonly managed by complete surgical excision with histopathological control of margins.11 Lesions should be excised along relaxed skin tension lines where possible for optimal cosmetic outcomes, avoiding distortion of anatomical features. However, the priority is to achieve complete local control and preserve patient survival.11 Curettage and cautery may be considered for small, superficial cSCCs or for Bowen’s disease.
Mohs’ micrographic surgery is a highly specialised surgical technique involving histopathological examination of frozen sections of the entire peripheral and deep margins of excised tissue, in contrast with standard specimen processing, where only 0.1 to 1% of the surgical margin is examined.12 Mohs’ micrographic surgery offers enhanced margin control and is ideal for high-risk, recurrent or cosmetically sensitive lesions. High-risk tumours – such as those with poor differentiation, perineural invasion or large size – warrant referral to a specialist or multidisciplinary team.
Radiotherapy
Radiotherapy is an option for patients with cSCC in whom surgery is not suitable for patient- or tumour-associated reasons. It is primarily used for inoperable cSCC or as an adjuvant treatment.11 Advances in fractionation techniques have improved tumour targeting while sparing normal tissue. Adjuvant radiotherapy should be considered for advanced or metastatic tumours; persistent or recurrent disease; following incomplete excision when re-excision is not feasible; or where there is significant perineural involvement.11 Referral to a specialist centre with a radiation oncologist is recommended in these cases.
Systemic therapy
For locally advanced or metastatic cSCC, systemic therapy may be required, with decisions made in a multidisciplinary setting. Cetuximab (an epidermal growth factor receptor inhibitor) and cemiplimab (a programmed cell death protein 1 immune checkpoint inhibitor) are PBS-listed systemic therapies approved for patients with metastatic or locally advanced cutaneous squamous cell carcinoma who are not candidates for curative surgery or radiotherapy, and have a WHO performance status of zero or one.
Chemoprophylaxis
In immunocompetent patients, agents such as acitretin and nicotinamide (vitamin B3) have demonstrated efficacy in reducing keratinocyte cancers. Other agents, including aspirin, are under investigation.13-15 In high-risk populations such as transplant recipients, chemoprophylaxis may help reduce tumour burden.13 A 2022 Australian study of 22 transplant recipients found that low-dose acitretin was effective in reducing keratinocyte cancer burden and well tolerated for up to five years. However, these therapies carry potential adverse effects and should be managed by experienced dermatologists.13 Nicotinamide did not reduce numbers of keratinocyte cancers or actinic keratoses in organ transplant recipients in a 2023 study.14
Basal cell carcinoma
BCC is the most common type of skin cancer, comprising about 75% of all cases.16
Risk factors
BCC shares many risk factors with cSCC, with UV radiation as the primary driver.16 Compared with cSCC, the risk of BCC is more closely associated with intermittent intense UV exposure and sunburn, particularly during childhood and adolescence, rather than cumulative lifetime exposure.16 Additional risk factors include artificial UV exposure, ionising radiation and rare inherited syndromes such as Gorlin syndrome, Bazex-Dupré-Christol syndrome and xeroderma pigmentosum.16
Presentation and diagnosis
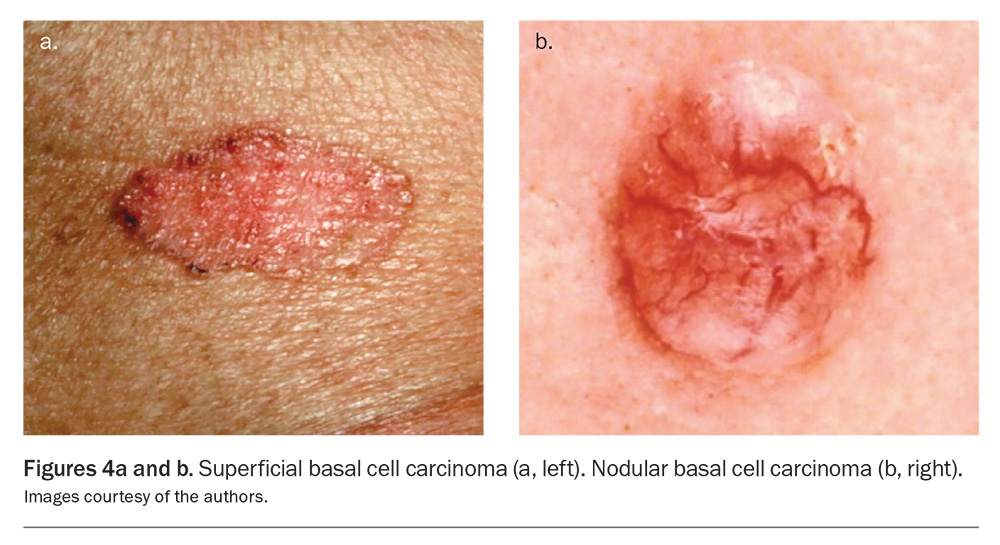
BCCs most commonly affect sun-exposed areas, with 80% occurring on the head and neck.16 Clinical presentations vary by subtype.12 Classic lesions present as pink, pearly papules with rolled borders and surface telangiectasia, whereas others may appear as erythematous scaly plaques or morphoeic, scar-like indurated areas (Figures 4a and b).12
Diagnosis is confirmed with biopsy, which also provides information on the histological subtype to guide management.12 Although metastasis is rare, untreated BCCs can be locally destructive, particularly on the head and neck, leading to significant morbidity and the need for complex surgical reconstruction.12 High-risk histological subtypes, lesion size and anatomical site all influence recurrence risk and treatment planning.12
Treatment
Similar to cSCC, management can be guided by Cancer Council Australia’s Clinical Practice Guidelines for Keratinocyte Cancer.5 The choice of therapy for BCC depends on the lesion characteristics, patient comorbidities, preferences regarding cosmetic outcome and treatment burden. Early identification and tailored intervention are key to preventing complications and reducing the healthcare burden of this increasingly prevalent cancer.
Surgery
Surgical excision remains the gold standard for most BCCs, especially high-risk subtypes (infiltrative, micronodular, basosquamous and morphoeic), which are more likely to recur and can invade deeply. High-risk lesions or those in cosmetically sensitive locations warrant referral to a dermatologist or specialist surgeon. Mohs’ micrographic surgery is particularly valuable for tumours on the central face, ears or periorbital region, or for recurrent or aggressive lesions.12
Nonsurgical treatments
For small, low-risk superficial BCCs, nonsurgical treatments may be appropriate. Options include cryotherapy, imiquimod 5% cream and off-label 5-fluorouracil 5% cream. Imiquimod 5% cream is applied five times per week for about six weeks.12 The inflammatory response varies between individuals and may be influenced by lesion biology and patient factors. Marked inflammation may necessitate pausing treatment until the side effect subsides. A biopsy is required for PBS reimbursement of imiquimod.
Photodynamic therapy
Photodynamic therapy is an effective option for superficial and thin nodular BCCs, especially in cosmetically sensitive areas. A photosensitising agent is applied, and after an incubation period of about three hours, light activation is used to destroy tumour cells. Photodynamic therapy offers excellent cosmetic outcomes, although recurrence rates may be higher than with surgery. Access may be limited to dermatology centres due to specialist equipment requirements.
Curettage
Curettage and electrodesiccation may be used for selected low-risk lesions on the trunk or limbs but require careful patient selection and close follow up. These techniques may not provide histological margin control, and recurrence rates can be higher.12
Radiotherapy
Radiotherapy is an option for adjuvant therapy or for inoperable cases, particularly for patients with contraindications to surgery; lesions in areas where cosmesis or tissue preservation is a priority, such as the lower eyelid, nose or ears; or for tumours with perineural invasion.12
Rhenium-188 brachytherapy is a newer treatment, which is TGA approved but not Medicare or PBS funded, showing promise for superficial BCC and SCC lesions less than 3 mm thick. It delivers high-dose beta radiation directly to the lesion surface in a single treatment session using a topical applicator. Early studies report favourable outcomes and good cosmesis, although long-term data are pending.17
Systemic therapy
Patients with complex locally advanced disease should be managed by a multidisciplinary team that includes surgeons, dermatologists, radiation oncologists, pathologists and medical oncologists. Systemic therapy is reserved for locally advanced or metastatic BCC. Oral Hedgehog pathway inhibitors, such as vismodegib and sonidegib, are PBS listed for patients with metastatic or locally advanced basal cell carcinoma who are unsuitable for surgery or radiotherapy. These drugs can be effective but are often poorly tolerated, with common side effects including severe muscle cramps, alopecia, fatigue and dysgeusia.12
When should a GP refer?
GPs are well positioned to educate patients on the importance of sun-safe behaviours, detect skin cancers at the earliest opportunity and provide initial management. Referral to specialist care should be considered in any of the following scenarios:
- uncertain diagnosis or discordant biopsy findings
- lesions with high-risk pathological or clinical features
- recurrent or incompletely excised tumours
- lesions in cosmetically or functionally sensitive areas
- when treatment is beyond the GP’s level of comfort or expertise.
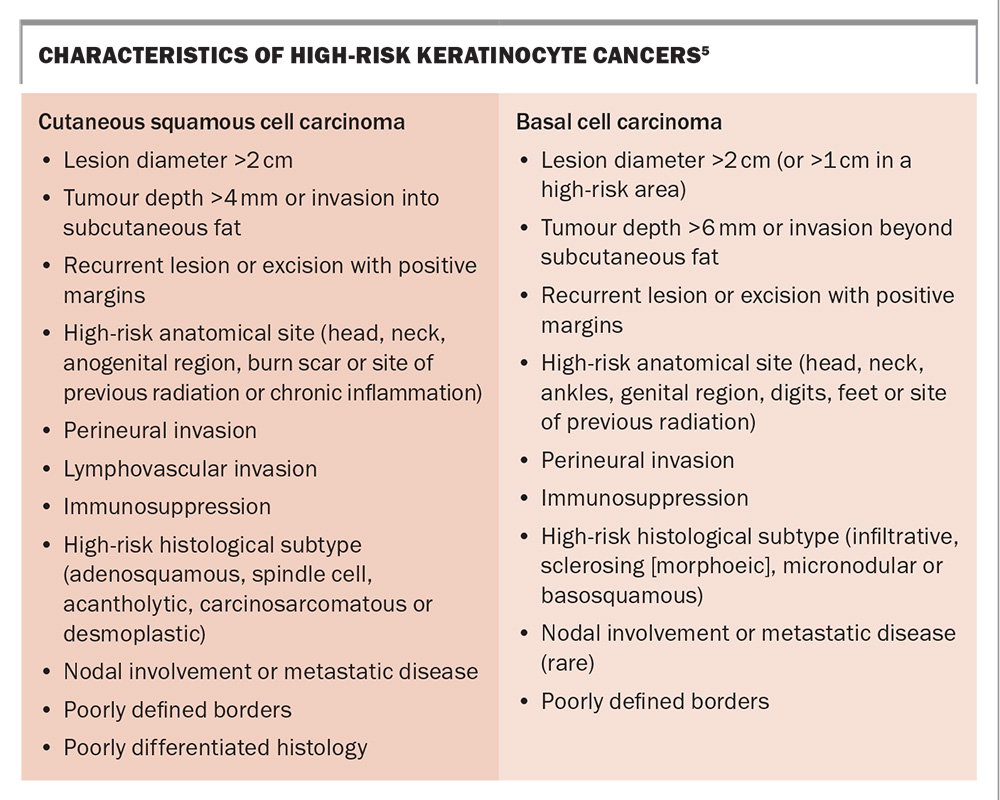
The Box contains a summary of the high-risk features of BCC and cSCC.5
Patients requiring specialised management, such as photodynamic therapy, complex surgical procedures or Mohs’ micrographic surgery, should be referred to a dermatologist. Patients with complex needs – including high-risk features, complex tumours (e.g. Merkel cell carcinoma), metastatic disease or contraindications to first-line treatment – may benefit from referral to a multidisciplinary team comprising dermatologists, surgeons, dermatopathologists, and medical and radiation oncologists. Early multidisciplinary input can improve outcomes and guide the optimal use of surgical, radiation and systemic treatment options.
Conclusion
Keratinocyte cancers remain the most common malignancies in Australia, creating a substantial burden for both patients and the healthcare system. Through early detection, patient education and appropriate management and referral, GPs can significantly reduce the morbidity, mortality and healthcare costs associated with these cancers. They are uniquely placed to lead the prevention, early detection and initial management of keratinocyte skin cancers. Multidisciplinary care is increasingly important in the management of complex and high-risk disease. MT
COMPETING INTERESTS: Associate Professor Shumack has received consulting fees from Specialist Connect Advisory services. Associate Professor Foley has received research grants from AbbVie, Amgen, Bristol-Myers Squibb, Eli Lilly and Company, Janssen, LEO Pharma, Novartis, Pfizer, Sanofi, Sun Pharma and UCB Pharma; received consulting fees from Apogee, Aslan, Eli Lilly and Company, Galderma, GenesisCare, Janssen, LEO Pharma, Mayne Pharma, MedImmune, Novartis, Oruka, Pfizer and UCB Pharma; received payment or honoraria from AbbVie, Amgen, Boehringer Ingelheim, Bristol Myers Squibb, Eli Lilly and Company, Janssen, Novartis, Sanofi, Sun Pharma and UCB Pharma; received payment for expert testimony from Pfizer; participated on an Advisory Board for AbbVie, Amgen, Aslan, Boehringer Ingelheim, Bristol Myers Squibb, Eli Lilly and Company, Galderma, GlaxoSmithKline, Janssen, LEO Pharma, Mayne Pharma, Novartis, Pfizer, Sanofi, Sun Pharma and UCB Pharma; and received drug samples for patient use from AbbVie, Amgen, Bristol-Myers Squibb, Eli Lilly and Company, Janssen, LEO Pharma, Mayne Pharma, Novartis, Sun Pharma and UCB Pharma. Dr Larney and Dr Iyengar: None.
References
1. Olsen CM, Pandeya N, Green AC, et al. Keratinocyte cancer incidence in Australia: a review of population-based incidence trends and estimates of lifetime risk. Public Health Res Pract 2022; 32: 3212203.
2. Gordon LG, Leung W, Johns R, et al. Estimated healthcare costs of melanoma and keratinocyte skin cancers in Australia and Aotearoa New Zealand in 2021. Int J Environ Res Public Health 2022; 19: 3178.
3. Dodds A, Chia A, Shumack S. Actinic keratosis: rationale and management. Dermatol Ther (Heidelb) 2014; 4: 11-31.
4. Reinehr CPH, Bakos RM. Actinic keratoses: review of clinical, dermoscopic, and therapeutic aspects. An Bras Dermatol 2019; 94: 637-657.
5. Cancer Council Australia. Clinical practice guidelines for keratinocyte cancer. Sydney: Cancer Council Australia; 2019. Available online at: https://www.cancer.org.au/clinical-guidelines/skin-cancer/keratinocyte-cancer (accessed September 2025).
6. Dlott AH, Spencer SA, Di Pasqua AJ. Calcipotriol and 5-fluorouracil combination therapy for the treatment of actinic keratosis in the clinic: a review article. Clin Drug Investig 2024; 44: 733-737.
7. Rubel DM, Spelman L, Murrell DF, et al. Daylight photodynamic therapy with methyl aminolevulinate cream as a convenient, similarly effective, nearly painless alternative to conventional photodynamic therapy in actinic keratosis treatment: a randomized controlled trial. Br J Dermatol 2014; 171: 1164-1171.
8. Dettrick A, Foden N, Hogan D, et al. The hidden Australian skin cancer epidemic, high-risk cutaneous squamous cell carcinoma: a narrative review. Pathology 2024; 56: 619-632.
9. Wysong A. Squamous-cell carcinoma of the skin. N Engl J Med 2023; 388: 2262-2273.
10. Neubert T, Lehmann P. Bowen’s disease - a review of newer treatment options. Ther Clin Risk Manag 2008; 4: 1085-1095.
11. Stratigos A, Garbe C, Lebbe C, et al. Diagnosis and treatment of invasive squamous cell carcinoma of the skin: European consensus-based interdisciplinary guideline. Eur J Cancer 2015; 51: 1989-2007.
12. McDaniel B, Steele RB. Basal cell carcinoma. Treasure Island (FL): StatPearls Publishing; 2024. Available online at: https://www.ncbi.nlm.nih.gov/books/NBK482439/ (accessed September 2025).
13. Allnutt KJ, Vogrin S, Li J. A long-term cohort study of acitretin for prevention of keratinocyte carcinoma in solid organ transplant recipients. Australas J Dermatol 2022; 63: e121-e126.
14. Allen NC, Martin AJ, Snaidr VA, et al. Nicotinamide for skin-cancer chemoprevention in transplant recipients. N Engl J Med 2023; 388: 804-812.
15. Hiscutt E, Orchard S, Wolfe R, Mar V. Chemo prevention of keratinocyte cancers: could aspirin bethe solution? J Cancer Prev 2025; 30: 59-74.
16. Bartos V. Development of multiple-lesion basal cell carcinoma of the skin: a comprehensive review.Sisli Etfal Hastan Tip Bul 2019; 53: 323-328.
17. Castellucci P, Savoia F, Farina A, et al. High dose brachytherapy with non sealed 188Re (rhenium) resin in patients with non-melanoma skin cancers (NMSCs): single center preliminary results. Eur J Nucl Med Mol Imaging 2021; 48: 1511-1521.
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.