Emotional dysregulation: bipolar disorder, borderline personality disorder, or both?

Patients presenting with emotional dysregulation are commonly seen in general practice. In adults, this symptom may be a feature of a bipolar disorder or borderline personality disorder. Practical strategies can help distinguish between these conditions, manage comorbidity and align treatment with the evidence, supporting GPs to work effectively with patients with these disorders.
- Emotional dysregulation in adults is a frequent presentation in general practice and may indicate bipolar disorder or borderline personality disorder as key differential diagnoses.
- Bipolar disorder and borderline personality disorder share overlapping features but differ in course, triggers and treatment approach.
- Medication is the cornerstone of bipolar disorder management, whereas it may play an adjunctive role for selected patients with borderline personality disorder.
- Psychotherapy is the mainstay of treatment for borderline personality disorder and generally plays a secondary role in bipolar disorder. Good Psychiatric Management offers a pragmatic generalist framework in primary care, particularly valuable when patients are ambivalent about engaging in specialist therapies or when such services are not accessible.
- GPs are central in recognising patterns over time, monitoring physical health, assessing risk and sustaining therapeutic optimism.
- Prognosis is often better than assumed. Bipolar disorder can often be effectively managed, and borderline personality disorder features frequently improve with age.
Emotional dysregulation (also known as affective instability) is a common and challenging presentation in general practice. Patients may present with a marked reactivity of mood, with intense dysphoria, irritability or anxiety, typically lasting a few hours and rarely more than a few days, as defined in the Diagnostic and Statistical Manual of Mental Disorders – 5th Edition.1 Although acute medical illness, organic brain syndromes or substance use should be considered and excluded as possible causes, emotional dysregulation may reflect an underlying psychiatric disorder.
Children may also present with emotional dysregulation in the context of conduct or oppositional defiant disorders; however, this article focuses on adults. For the GP, a central challenge is determining whether emotional dysregulation indicates underlying bipolar disorder, borderline personality disorder or both conditions concurrently.
Misdiagnosis can carry significant consequences. A patient with bipolar disorder misdiagnosed with borderline personality disorder may miss timely initiation of a mood stabiliser, increasing relapse risk and cumulative morbidity. Conversely, a patient with borderline personality disorder incorrectly diagnosed with bipolar disorder may spend years taking medications with little benefit, while missing the opportunity for more effective evidence-based psychotherapy. Accurate diagnosis allows for the selection of an appropriate treatment paradigm. Bipolar disorder is treatable, with pharmacotherapy forming the foundation of management, whereas borderline personality disorder responds best to psychological care. Practical strategies can help guide GPs approach emotional dysregulation in general practice, to differentiate bipolar disorder from borderline personality disorder and guide treatment pathways.
Aetiology and prevalence
Bipolar disorder has a lifetime prevalence of 3.8%, and in 2020 to 2021, about 744,800 people in Australia had the condition.2 Although a less common presentation in general practice than depression or anxiety, bipolar disorder is not rare, and the consequences of a missed diagnosis can be substantial. Onset typically occurs in late adolescence or early adulthood, often with a recognisable ‘trend break’ (a distinct change from a previously stable mood pattern to the onset of mood swings); however, delays in diagnosis are common.3 These disorders have a strong genetic basis, with heritability estimates of 70 to 80%.4 Environmental factors such as sleep disruption, substance use and psychosocial stressors often precipitate episodes.5 Neurobiological studies suggest that dysregulation of circadian rhythms, reward pathways and frontolimbic networks is present in bipolar disorder.6 For GPs, important diagnostic clues may include a family history of bipolar disorder and careful identification of discrete manic, hypomanic and depressive episodes.
Borderline personality disorder is estimated to affect about 1 to 6% of the general population.7 In clinical settings, it is far more prevalent; about 6% of primary care patients and up to 20% of psychiatric outpatients meet the diagnostic criteria for borderline personality disorder.8 Borderline personality disorder typically emerges in adolescence or early adulthood. Although it is diagnosed more often in women, this is likely explained by referral and help-seeking patterns rather than true sex differences.9 The aetiology is multifactorial, involving genetic vulnerability, early adversity (particularly neglect, trauma and invalidating environments) and temperamental traits such as emotional reactivity and impulsivity.8 Neurobiological evidence points to altered frontolimbic connectivity.10 For GPs, understanding this developmental and biopsychosocial context can help frame the condition in a nonstigmatising and compassionate way.
Complex post-traumatic stress disorder (PTSD) is a related diagnosis, conceptualised as arising from prolonged and severe interpersonal trauma. Patients develop PTSD-like symptoms, as well as disturbance of self-organisation, which may include emotional dysregulation in some patients.11 It has been argued that complex PTSD may provide a less stigmatising and more accurate conceptualisation for some people diagnosed with borderline personality disorder; however, this remains an open question. Thus, the focus of this article is on borderline personality disorder.
In addition to emotional dysregulation, bipolar disorder and borderline personality disorder share other features. This includes high rates of comorbid anxiety and substance use, elevated suicide risk, impulsivity and functional impairment.12-16
Clinical presentation
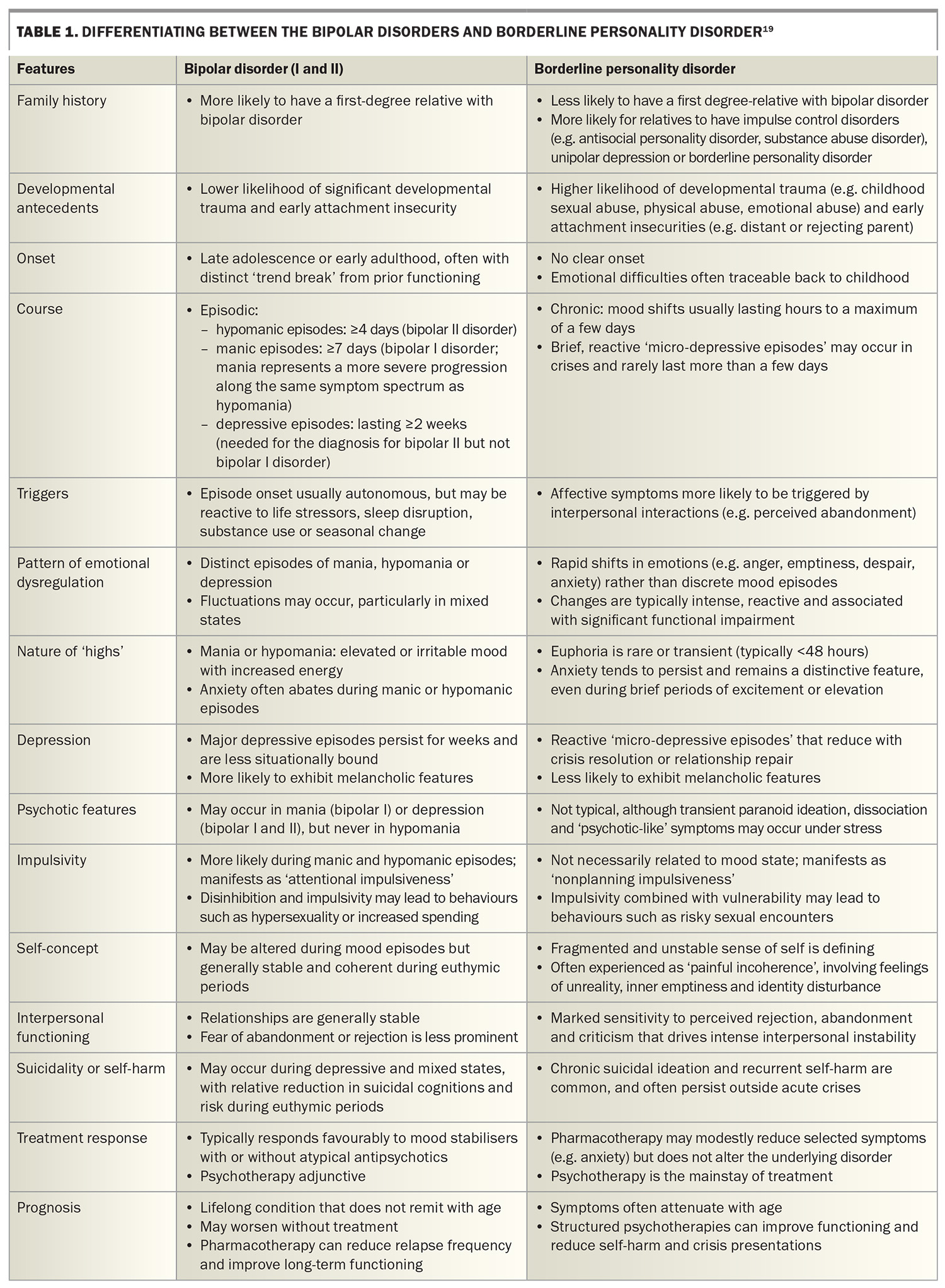
The most reliable distinctions between bipolar disorder and borderline personality disorder relate to the temporal pattern and duration of mood changes, whether symptoms occur in discrete episodes or as chronic affective reactivity and the broader clinical context. Apparent similarities in a single cross-sectional consultation often diverge when symptoms are observed longitudinally.
Bipolar I disorder is diagnosed based on the presence of at least one manic episode, defined as a distinct period of abnormally elevated, expansive or irritable mood and increased activity or energy lasting at least seven days (or of shorter duration if hospitalisation is required). Although manic episodes are typically interspersed with major depressive episodes, the latter is not necessary for the diagnosis. Manic episodes are typically severe and disruptive, and may be clinically conspicuous, with features such as disinhibition (e.g. hypersexuality, increased spending), aggression, rapid speech and psychomotor acceleration. Psychotic features (e.g. grandiose delusions, formal thought disorder) are common during mania and, when present, confirm the diagnosis of bipolar I disorder regardless of episode duration.1
Bipolar II disorder features hypomanic episodes, defined by a minimum duration of four days, involving increased energy or activity and elevated or irritable mood, but with lower severity and less impairment than mania; by definition, hypomania does not include psychotic features.1 Depressive episodes typically predominate in bipolar II disorder, and patients often present in primary care with recurrent depression.
Differentiating bipolar I disorder from borderline personality disorder is generally more straightforward because psychotic symptoms are common during manic states. Differentiating bipolar II disorder from borderline personality disorder is a more frequent dilemma, because the hypomanic mood states lack psychotic features and are generally less severe. It is important to screen for prior episodes of mood elevation in people presenting with depression to avoid overlooking bipolar disorder, particularly bipolar II disorder, where patients may not recognise hypomania as pathological.
Diagnosis can be challenging because hypomanic features, such as increased goal-directed activity, risk-taking behaviours and irritability or heightened emotional expression, may be misinterpreted as impulsivity and interpersonal reactivity, which are characteristic of borderline personality disorder. Similarly, depressive cognitions may be mistaken for the chronic feelings of emptiness and pervasive dysphoria typical of borderline personality disorder. In practice, differentiating bipolar II disorder from borderline personality disorder is less dependent on isolated symptom clusters and is more reliably achieved by focusing on:
- longitudinal course
- family history of mood disorders (bipolar disorder or unipolar depression)
- developmental antecedents
- characteristic patterns of interpersonal functioning.17
Borderline personality disorder is characterised by rapid, reactive mood shifts that typically last hours and are most often precipitated by interpersonal stressors. Core features include an intense fear of abandonment, chronic feelings of emptiness, unstable relationships, difficulties with boundaries and identity disturbance.1 Impulsive behaviours and recurrent deliberate self-harm, such as cutting, are frequent, as are transient stress-related paranoia and dissociative symptoms.
Patients may be only partially aware that their mood shifts can be triggered by interpersonal stressors, so affective changes can feel abrupt and difficult to explain. The Spectrum guidelines on borderline personality disorder describe this phenomenon as ‘micro-depressive episodes’: brief, reactive depressive states that emerge in the context of interpersonal crises but may appear clinically indistinguishable from depressive episodes of unipolar or bipolar disorder on cross-sectional assessment.18 These states typically remit once the crisis resolves, often lifting abruptly if the relationship is restored, and rarely persist beyond a few days. In addition to micro-depressive episodes, GPs should be aware that some patients with borderline personality disorder have comorbid major depressive episodes that may require concurrent treatment.
The key differences between the bipolar disorders and borderline personality are summarised in Table 1.19
Comorbidity of bipolar disease and borderline personality disorder
A previous systematic review suggests that about 20% of patients with bipolar disorder also meet criteria for borderline personality disorder, and vice versa.20 Diagnostic overshadowing can occur in either direction: the presence of borderline personality disorder may obscure an underlying mood disorder, whereas a diagnosis of bipolar disorder may lead the clinician to overlook enduring personality pathology that drives recurrent crises. Comorbidity can complicate assessment because patients may present with discrete manic or hypomanic episodes alongside chronic interpersonal instability and impulsivity. Recognising possible comorbidity is important and may warrant referral of the patient to a psychiatrist for diagnostic clarification.
The GP’s vantage point
Differentiating between bipolar disorder and borderline personality disorder is difficult in a single consultation. The strength of general practice lies in longitudinal care, where repeated encounters allow illness trajectories to become evident. Following a patient over time places the GP in a strong position to distinguish the episodic course of bipolar disorder from the crisis-driven reactivity of borderline personality disorder. GPs may also be aware of a relevant family history of mood disorder, as well as family dysfunction that may be pertinent in borderline personality disorder.
When diagnostic uncertainty persists, it is often preferable to adopt a descriptive formulation, such as ‘emotional dysregulation with depressive symptoms’, and arrange for the patient to undergo psychiatric assessment, rather than assigning a premature diagnosis.
Treatment of bipolar disorder
Pharmacotherapy remains the cornerstone of bipolar disorder management, with adjunctive psychosocial interventions providing additional benefit.21 The 2020 Royal Australian and New Zealand College of Psychiatrists Clinical Practice Guidelines for Mood Disorders contain detailed management recommendations.21 Key tasks for GPs include initiating and managing pharmacotherapy (with psychiatric input where indicated), supporting adherence to treatment, recognising relapse patterns, monitoring physical health and treatment-related adverse effects, co-ordinating psychiatrist input when required and providing continuity of care across episodes.
Pharmacotherapy
Pharmacotherapy is foundational in the management of the bipolar disorders. Randomised controlled trials and meta-analyses consistently demonstrate that mood stabilisers and atypical antipsychotics reduce relapse risk, shorten the duration of acute episodes and improve long-term functioning.22
The choice of pharmacotherapy often depends on the phase of illness (hypomania, mania, depression or maintenance), polarity of predominant episodes, comorbidities, prior treatment response, tolerability and patient preference. Most evidence for treatment comes from studies of bipolar I disorder, with few trials specifically focused on bipolar II disorder.
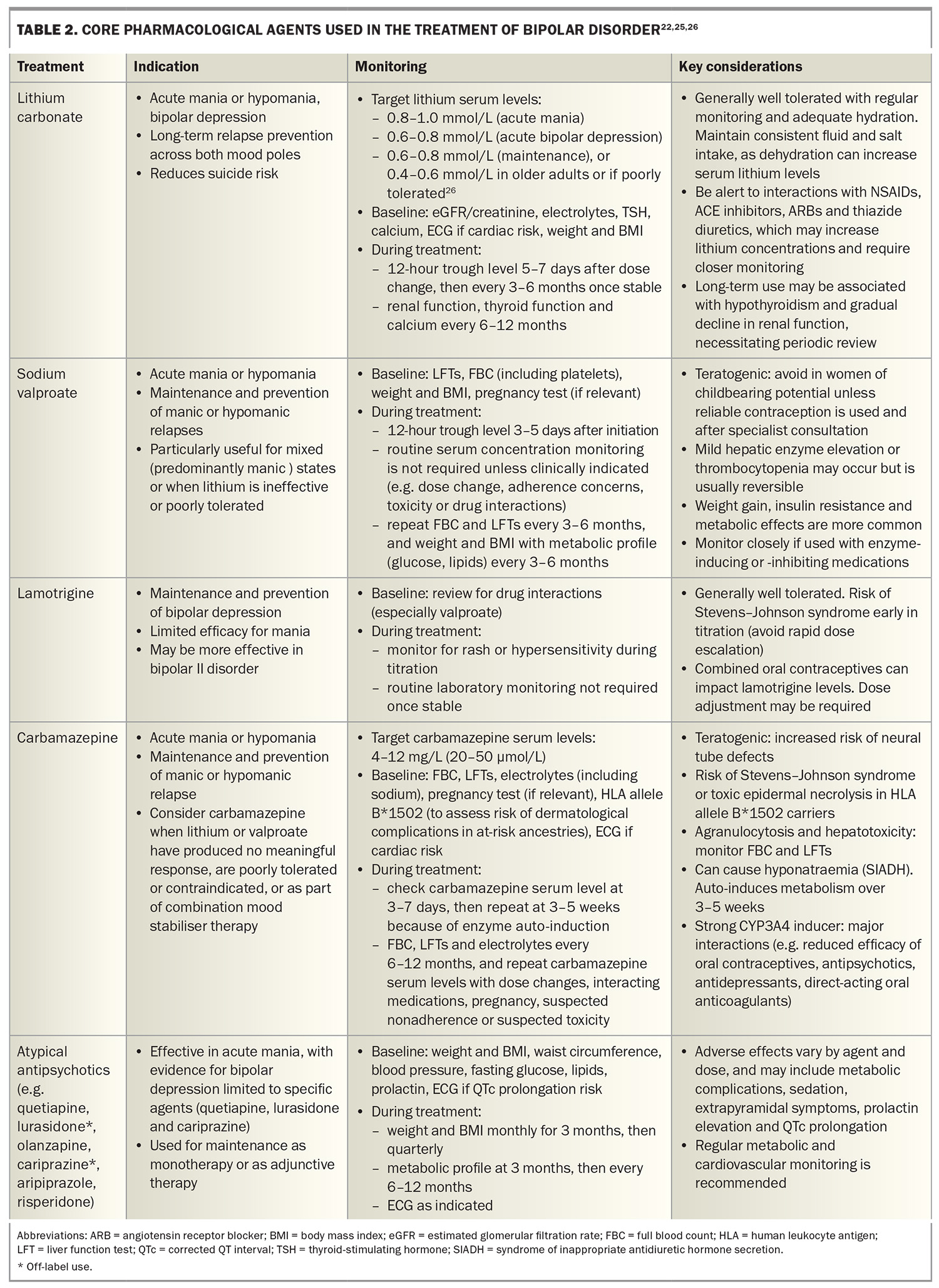
Lithium remains a gold-standard maintenance therapy for bipolar disorder, with strong evidence for preventing relapse to both mania and depression and for reducing suicide risk.23,24 Despite this, its use has declined, often because of the perceived burden of monitoring. Carbamazepine, another mood stabiliser, is also prescribed less often, whereas valproate, lamotrigine and atypical antipsychotics are increasingly prescribed (Table 2).22,25,26 Supporting adherence, providing patient education and regularly monitoring mental and physical health are crucial to ensuring safe, sustained maintenance, regardless of the agent used.
The use of antidepressants in bipolar disorder remains controversial. Systematic reviews and meta-analyses suggest possible short-term benefit in bipolar depression, particularly when combined with a mood stabiliser, but evidence for long-term efficacy is inconsistent.25,27 Some studies have revealed a reduced relapse risk with continuation, whereas others have found increased risks of switching to mania, cycle acceleration or mood destabilisation.28-30 These risks are not evenly distributed across the bipolar subtypes; patients with bipolar I disorder have a substantially higher propensity for antidepressant-induced affective switch and destabilisation, whereas those with bipolar II disorder appear to have lower switch rates and may derive modest adjunctive benefit in selected cases.31 Antidepressant monotherapy should be avoided. Decisions to initiate or continue adjunctive antidepressant treatment should be made in consultation with a psychiatrist.
Psychoeducation and psychotherapies
Structured and consistent psychoeducation is an effective adjunct to pharmacotherapy in patients with bipolar disorder, with strong evidence for improving insight and adherence, as well as relapse prevention.32 It helps patients understand the illness, recognise early warning signs and implement personalised self-management strategies. GPs can reinforce these principles by monitoring for subtle changes in sleep, energy or thought patterns, and encouraging timely contact with treating clinicians. Psychoeducation also involves normalising long-term treatment, addressing medication concerns and highlighting the link between adherence and stability. GPs can promote regular routines, adequate sleep, stress management and reduced substance use. Periodic review of mood patterns and triggers can help sustain wellness between specialist appointments.
Psychotherapies such as cognitive behavioural therapy, family-focused therapy, and interpersonal and social rhythm therapy are valuable adjuncts in long-term bipolar disorder management. These approaches reduce relapse rates, improve adherence and enhance functional recovery, particularly during depressive and maintenance phases.33-35 Family-focused therapy promotes communication, problem solving and emotional regulation within families, whereas interpersonal and social rhythm therapy supports mood stability by helping patients maintain regular daily routines, sleep–wake cycles and interpersonal rhythms that influence mood regulation.
Lifestyle interventions
Lifestyle interventions are a core adjunct in long-term bipolar disorder management. A systematic review and meta-analysis found that sleep-focused interventions significantly improve depressive symptoms, whereas combined diet and physical activity interventions improve both depressive symptoms and functional outcomes.36 Multidimensional interventions targeting multiple lifestyle domains appear more effective than single-domain approaches. Given the established associations among circadian dysregulation, metabolic comorbidity and illness trajectory in bipolar disorder, systematic attention to sleep regularity, physical activity, nutrition and substance use is an evidence-informed strategy in primary care.21 Integrating structured lifestyle support alongside pharmacotherapy aligns with Royal Australian and New Zealand College of Psychiatrists guideline recommendations and addresses both mood outcomes and the substantial physical health burden associated with bipolar disorder.21
When to refer to a psychiatrist
Although many aspects of the bipolar disorders can be managed in primary care, timely referral should be considered in the following situations:
- diagnostic uncertainty – e.g. distinguishing bipolar disorder from unipolar depression, attention deficit hyperactivity disorder, borderline personality disorder or substance-induced mood disorders
- initiation or optimisation of pharmacotherapy – e.g. commencing or adjusting mood stabilisers or antipsychotic therapy
- suspected or confirmed acute relapse – emergence of manic, hypomanic, mixed or severe depressive symptoms requiring specialist assessment or adjustment of treatment
- inadequate treatment response – relapse or persistent symptoms despite adherence to first-line therapy
- complex comorbidities – e.g. substance use disorders, anxiety, trauma or significant medical illness requiring medication co-ordination
- pregnancy or reproductive planning – to manage potential medication-associated teratogenic risk, medication changes or preconception counselling.
Treatment of borderline personality disorder
Borderline personality disorder is a chronic but manageable condition. Psychotherapy is the foundation of care, with several structured approaches supported by evidence. GPs can provide continuity of care within a generalist management framework and guide patients toward appropriate treatment pathways.
Specialised psychotherapies
Several specialist therapies have an evidence base for the treatment of borderline personality disorder and are typically delivered following referral to psychologists, psychotherapists or psychiatrists trained in their use. Dialectical behaviour therapy provides the strongest evidence for reducing deliberate self-harm and suicidality.37 Mentalisation-based therapy improves emotional regulation and interpersonal functioning, whereas transference-focused psychotherapy improves identity coherence and impulse control.38,39 Schema-focused therapy is effective, including in chronic or treatment-resistant cases.40
These therapies differ in orientation and intensity; therefore, patients may need to try more than one approach before finding the right fit. Ambivalence about therapy is common. GPs can encourage engagement, particularly when patients are precontemplative, while providing continuity and support throughout the process.
Good Psychiatric Management
Where specialist therapies are unavailable, or when patient ambivalence is a barrier to engagement, Good Psychiatric Management (GPM), developed by John G. Gunderson, provides a practical, evidence-based generalist framework for managing borderline personality disorder.41 Principles of GPM, adapted for general practice, are outlined in Table 3; further details can be found in the Handbook of Good Psychiatric Management for Borderline Personality Disorder.41
GPM conceptualises borderline personality disorder as one of interpersonal hypersensitivity, providing a model for understanding recurrent crises and intense relational reactions. Core elements include psychoeducation to reduce stigma and orient patients and families, an active and pragmatic clinical stance, anticipating and planning for crises (rather than reacting to them) and maintaining continuity of care as a stabilising influence. Treatment is anchored in functional life goals (e.g. work, study, relationships or parenting) rather than aiming for symptom eradication or deep structural change. Evidence suggests outcomes with GPM are broadly comparable with more intensive therapies in many settings.42
For GPs, GPM offers a structured framework for providing continuity, containment and support within primary care. GPs should remain alert to negative countertransference (a clinician’s conscious or unconscious emotional response) that may emerge in response to patients with borderline personality disorder, particularly during crises and periods of emotional dysregulation. Common responses include frustration, irritation, helplessness, anxiety or anger, as well as emotional withdrawal, overcontrol, or urges to rescue, avoid or disengage from the patient. Failure to recognise this may increase the risk of a negative therapeutic encounter. If negative countertransference arises, it may be helpful to discuss the encounter with a colleague (e.g. in peer review or during supervision) and consider referral to a psychologist or psychiatrist.
Management of suicidality and deliberate self-harm
Chronic suicidal thoughts and deliberate self-harm are common features in borderline personality disorder. Suicidality is a challenging feature of borderline personality disorder, and up to 10% of patients with this diagnosis die by suicide.43 Deliberate self-harm may serve multiple functions, including a maladaptive coping strategy for intense emotional pain or chronic emptiness, or self-punishment linked to a negative self-concept.
In general practice, a key task is to distinguish acute from chronic suicidality. Acute risk may be suggested by a change in pattern, use of more lethal methods or the presence of new stressors. Management may require co-ordination with family members, the treating psychiatrist or psychologist and review of the patient’s safety plan. Emergency department assessment and, at times, hospital admission may be necessary to contain risk; however, routine hospitalisation may be counterproductive. The aim is steady, predictable care that contains risk without making treatment contingent on crises.
Principles of managing deliberate self-harm are similar: identify triggers, validate emotional pain without over-focusing on the act itself and encourage safer coping strategies over time. Where appropriate, patients can be supported to recognise when medical care is needed. Each review offers an opportunity to reinforce healthier coping strategies and encourage engagement with psychotherapy, which remains the most effective long-term treatment.
Pharmacology as a cautious adjunct
A systematic review of pharmacological treatments for borderline personality disorder found that none of the frequently prescribed medications for borderline personality disorder – including antidepressants, atypical antipsychotics and anticonvulsant mood stabilisers – reduce the severity of borderline personality disorder or alter its underlying disease course.44
Despite this lack of evidence, psychotropic prescribing remains common. Studies show that patients with borderline personality disorder are prescribed more psychotropic medications on average than psychiatric patients without a personality disorder diagnosis.45 This practice carries risks; overdose of prescribed medications remains a common cause of deliberate self-harm and suicide attempts, with one study revealing that 25% of patients with borderline personality disorder considered suicide using prescribed medication.46 In addition, long-term psychotropic use is associated with adverse physical outcomes such as metabolic syndrome, which is estimated to affect about 40% of people with borderline personality disorder in Australia.47
Medication prescribing for borderline personality disorder should therefore be cautious and align with the following principles.
- Restrict prescribing to clearly defined situations – e.g. comorbid psychiatric conditions such as depression not responsive to psychotherapy, targeted symptom relief such as for significant agitation.
- If prescribing, use a single agent at the lowest effective dose. For as-needed prescribing, supply only small quantities for short, clearly defined, time-limited periods.
- Undertake regular medication reviews and rationalise unnecessary or ineffective agents to minimise polypharmacy.
- Maintain continuity of care independent of crises or deliberate self-harm, avoiding reactive prescribing in response to acute presentations.
- Seek psychiatric review if ongoing pharmacotherapy appears necessary.
When to refer to a psychiatrist
Referral of a patient with borderline personality disorder to a psychiatrist should be considered when:
- diagnostic uncertainty exists – e.g. difficulty distinguishing borderline personality disorder from bipolar disorder, psychotic disorders or complex PTSD
- comorbid psychiatric illness requires specialist management – e.g. psychosis, bipolar disorder, severe treatment-resistant depression or attention deficit hyperactivity disorder with significant impairment
- high or escalating risk is identified – e.g. acute suicidality, repeated high-lethality attempts, severe self-injury
- complex pharmacotherapy is being used or considered
- severe functional impairment persists despite GP-led interventions, and access to structured psychotherapy or specialist services is required
- care co-ordination is needed across multiple providers or services
- challenges to ongoing care are identified – e.g. negative countertransference.
Conclusion
Emotional dysregulation is a common but diagnostically complex presentation in general practice and, in adults, may indicate an underlying bipolar disorder or borderline personality disorder. These conditions share overlapping features, yet differ markedly in course, treatment response and prognosis. There is a risk of misdiagnosis where one condition is mistaken for the other, and diagnostic overshadowing where both conditions are present but one is missed, leaving patients either undertreated or inappropriately medicated.
For GPs, it may not be possible to make a definitive diagnosis at a single encounter; however, a clearer picture often emerges through longitudinal observation, holding diagnostic possibilities in mind and recognising when presentations suggest co-occurrence. Referral to a psychiatrist may assist in diagnostic clarification, medication advice and ongoing management.
Sustained, discrete mood episodes point toward the bipolar disorders and warrant timely initiation of mood stabilisers, particularly lithium, which has strong evidence for relapse prevention and antisuicidal properties. In contrast, the reactive, situational affective shifts of borderline personality disorder respond best to psychotherapy. GPM provides a pragmatic framework that is readily adaptable to primary care, alongside referral to specialised therapies such as dialectical behaviour therapy when available.
Both bipolar disorder and borderline personality disorder are manageable conditions, and outcomes can improve significantly when their differences, overlaps and comorbidities are understood. By combining longitudinal observation, therapeutic optimism and judicious referral, GPs are well placed to manage patients presenting with emotional dysregulation through targeted, effective and hopeful care pathways. MT
COMPETING INTERESTS: None.
References
1. American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 5th ed. Arlington: American Psychiatric Association; 2013.
2. Lind PA, Siskind DJ, Hickie IB, et al. Preliminary results from the Australian Genetics of Bipolar Disorder Study: a nation-wide cohort. Aust N Z J Psychiatry 2023; 57: 1428-1442.
3. Keramatian K, Morton E, Levit A, Nunez JJ. Evidence of factors influencing delays in the diagnosis and treatment of bipolar disorder in adolescents and young adults. Protocol for a systematic scoping review. PLoS One 2023; 18: e0292923.
4. Craddock N, Sklar P. Genetics of bipolar disorder. Lancet 2013; 381: 1654-1662.
5. Geddes JR, Miklowitz DJ. Treatment of bipolar disorder. Lancet 2013; 381: 1672-1682.
6. Phillips ML, Swartz HA. A critical appraisal of neuroimaging studies of bipolar disorder: toward a new conceptualization of underlying neural circuitry and a road map for future research. Am J Psychiatry 2014; 171: 829-843.
7. Lawn S, McMahon J. Experiences of care by Australians with a diagnosis of borderline personality disorder. J Psychiatr Ment Health Nurs 2015; 22: 510-521.
8. Bozzatello P, Garbarini C, Rocca P, Bellino S. Borderline personality disorder: risk factors and early detection. Diagnostics (Basel) 2021; 11: 2142.
9. Bayes A, Parker G. Borderline personality disorder in men: a literature review and illustrative case vignettes. Psychiatry Res 2017; 257: 197-202.
10. Ruocco AC, Amirthavasagam S, Choi-Kain LW, McMain SF. Neural correlates of negative emotionality in borderline personality disorder: an activation-likelihood-estimation meta-analysis. Biol Psychiatry 2013; 73: 153-160.
11. Cloitre M. ICD-11 complex post-traumatic stress disorder: simplifying diagnosis in trauma populations. Br J Psychiatry 2020; 216: 129-131.
12. Spoorthy MS, Chakrabarti S, Grover S. Comorbidity of bipolar and anxiety disorders: an overview of trends in research. World J Psychiatry 2019; 9: 7.
13. Quenneville AF, Kalogeropoulou E, Küng AL, et al. Childhood maltreatment, anxiety disorders and outcome in borderline personality disorder. Psychiatry Res 2020; 284: 112688.
14. Trull TJ, Freeman LK, Vebares TJ, Choate AM, Helle AC, Wycoff AM. Borderline personality disorder and substance use disorders: an updated review. Borderline Personal Disord Emot Dysregul 2018; 5: 15.
15. Messer T, Lammers G, Müller-Siecheneder F, Schmidt RF, Latifi S. Substance abuse in patients with bipolar disorder: a systematic review and meta-analysis. Psychiatry Res 2017; 253: 338-350.
16. Chesney E, Goodwin GM, Fazel S. Risks of all-cause and suicide mortality in mental disorders: a meta-review. World Psychiatry 2014; 13: 153-160.
17. Bayes A, Parker G, Fletcher K. Clinical differentiation of bipolar II disorder from borderline personality disorder. Curr Opin Psychiatry 2014; 27: 14-20.
18. Rao S, Kasiviswanathan K, Pilcher C. Borderline personality disorder. A practical guide for Victorian area mental health & wellbeing services. Melbourne: Spectrum; 2024. Available online at: https://www.spectrumbpd.com.au/news/new-release-spectrums-practical-guide-for-victorian-area-mental-health-and-wellbeing-services (accessed March 2026).
19. Bayes A, Parker G, Paris J. Differential diagnosis of bipolar II disorder and borderline personality disorder. Curr Psychiatry Rep 2019; 21: 125.
20. Temes CM, Boccagno C, Gold AK, et al. Comorbidity of bipolar disorder and borderline personality disorder: phenomenology, course, and treatment considerations. Bipolar Disord 2024; 26: 548-555.
21. Malhi GS, Bell E, Bassett D, et al. The 2020 Royal Australian and New Zealand College of Psychiatrists clinical practice guidelines for mood disorders. Aust N Z J Psychiatry 2021; 55: 7-117.
22. Kishi T, Ikuta T, Matsuda Y, et al. Mood stabilizers and/or antipsychotics for bipolar disorder in the maintenance phase: a systematic review and network meta-analysis of randomized controlled trials. Mol Psychiatry 2021; 26: 4146-4157.
23. Severus E, Taylor MJ, Sauer C, et al. Lithium for prevention of mood episodes in bipolar disorders: systematic review and meta-analysis. Int J Bipolar Disord 2014; 2: 15.
24. Tondo L, Baldessarini RJ. Prevention of suicidal behavior with lithium treatment in patients with recurrent mood disorders. Int J Bipolar Disord 2024; 12: 6.
25. Liu B, Zhang Y, Fang H, Liu J, Liu T, Li L. Efficacy and safety of long-term antidepressant treatment for bipolar disorders - a meta-analysis of randomized controlled trials. J Affect Disord 2017; 223: 41-48.
26. Malhi GS, Gershon S, Outhred T. Lithiumeter: version 2.0. Bipolar Disord 2016; 18: 631-641.
27. Hu Y, Zhang H, Wang H, Wang C, Kung S, Li C. Adjunctive antidepressants for the acute treatment of bipolar depression: a systematic review and meta-analysis. Psychiatry Res 2022; 311: 114468.
28. Amsterdam JD, Lorenzo-Luaces L, Soeller I, Li SQ, Mao JJ, DeRubeis RJ. Safety and effectiveness of continuation antidepressant versus mood stabilizer monotherapy for relapse-prevention of bipolar II depression: a randomized, double-blind, parallel-group, prospective study. J Affect Disord 2015; 185: 31-37.
29. Barbuti M, Menculini G, Verdolini N, et al. A systematic review of manic/hypomanic and depressive switches in patients with bipolar disorder in naturalistic settings: the role of antidepressant and antipsychotic drugs. Eur Neuropsychopharmacol 2023; 73: 1-15.
30. El-Mallakh RS, Vöhringer PA, Ostacher MM, et al. Antidepressants worsen rapid-cycling course in bipolar depression: a STEP-BD randomized clinical trial. J Affect Disord 2015; 184: 318-321.
31. Gitlin MJ. Antidepressants in bipolar depression: an enduring controversy. Int J Bipolar Disord 2018; 6: 25.
32. Batista TA, Von Werne Baes C, Juruena MF. Efficacy of psychoeducation in bipolar patients: systematic review of randomized trials. Psychol Neurosci 2011; 4: 409-416.
33. Scott J, Paykel E, Morriss R, et al. Cognitive–behavioural therapy for severe and recurrent bipolar disorders: randomised controlled trial. Br J Psychiatry 2006; 188: 313-320.
34. Miklowitz DJ, Chung B. Family-focused therapy for bipolar disorder: reflections on 30 years of research. Fam Process 2016; 55: 483-499.
35. Lam C, Chung MH. A meta-analysis of the effect of interpersonal and social rhythm therapy on symptom and functioning improvement in patients with bipolar disorders. Appl Res Qual Life 2021; 16: 153-165.
36. Simjanoski M, Patel S, Boni R De, et al. Lifestyle interventions for bipolar disorders: a systematic review and meta-analysis. Neurosci Biobehav Rev 2023; 152: 105257.
37. Linehan MM, Korslund KE, Harned MS, et al. Dialectical behavior therapy for high suicide risk in individuals with borderline personality disorder: a randomized clinical trial and component analysis. JAMA Psychiatry 2015; 72: 475-482.
38. Volkert J, Hauschild S, Taubner S. Mentalization-based treatment for personality disorders: efficacy, effectiveness, and new developments. Curr Psychiatry Rep 2019; 21: 1-12.
39. Clarkin JF, Levy KN, Lenzenweger MF, Kernberg OF. Evaluating three treatments for borderline personality disorder: a multiwave study. Am J Psychiatry 2007; 164: 922-928.
40. Giesen-Bloo J, Van Dyck R, Spinhoven P, et al. Outpatient psychotherapy for borderline personality disorder: randomized trial of schema-focused therapy vs transference-focused psychotherapy. Arch Gen Psychiatry 2006; 63: 649-658.
41. Gunderson JG, Links PS. Handbook of good psychiatric management for borderline personality disorder. Washington, DC: American Psychiatric Association Publishing; 2014.
42. McMain SF, Links PS, Gnam WH, et al. A randomized trial of dialectical behavior therapy versus general psychiatric management for borderline personality disorder. Am J Psychiatry 2009; 166: 1365-1374.
43. Paris J, Zweig-Frank H. A 27-year follow-up of patients with borderline personality disorder. Compr Psychiatry 2001; 42: 482-487.
44. Gartlehner G, Crotty K, Kennedy S, et al. Pharmacological treatments for borderline personality disorder: a systematic review and meta-analysis. CNS Drugs 2021; 35: 1053-1067.
45. Zanarini MC, Frankenburg FR, Reich DB, Harned AL, Fitzmaurice GM. Rates of psychotropic medication use reported by borderline patients and axis II comparison subjects over 16 years of prospective follow-up. J Clin Psychopharmacol 2015; 35: 63-67.
46. Makela EH, Moeller KE, Fullen JE, Gunel E. Medication utilization patterns and methods of suicidality in borderline personality disorder. Ann Pharmacother 2006; 40: 49-52.
47. John AP, Koloth R, Dragovic M, Lim SCB. Prevalence of metabolic syndrome among Australians with severe mental illness. Med J Aust 2009; 190: 176-179.