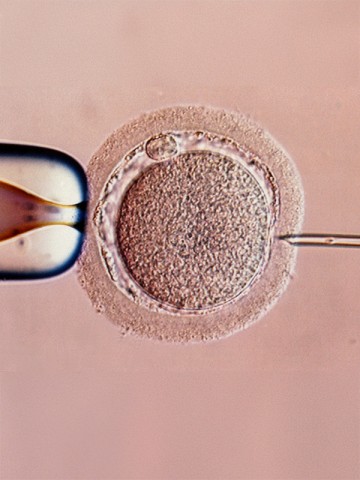
Study finds overall cancer risk not increased after medically assisted reproduction
Sasha Ellery BM BCh
Overall cancer incidence in women who undergo medically assisted reproduction appears comparable to that of the general population, a new Australian study finds, although small differences in some site-specific cancers may warrant closer clinical attention.
The study, published in JAMA Network Open, examined 417,984 women in Australia exposed to assisted reproductive technologies, intrauterine insemination with ovulation stimulation or ovulation induction using clomiphene citrate. Across these cohorts, overall invasive cancer incidence was broadly comparable to that expected for age-, jurisdiction- and calendar year-matched women.
Dr Adrian Walker, a study author and Research Fellow at the Centre for Big Data Research in Health, UNSW Sydney, Sydney, said, ‘This research is reassuring in that it indicates that cancer risk is not increased generally after fertility treatments. [It] supports previous extensive research demonstrating the safety of fertility treatment for women with infertility.’
Some variation was observed in site-specific cancers. Uterine cancer and melanoma were more common across all cohorts, whereas ovarian cancer was elevated in women exposed to assisted reproductive technology and intrauterine insemination with ovulation absolute risk was small, with rate differences for invasive cancers generally ranging from fewer than one to 6.51 extra cases per 100,000 person-years.
By contrast, cervical cancer and cancers of the trachea, bronchus and lung occurred less often than expected. The authors said this might reflect higher uptake of cervical screening and lower smoking rates among women exposed to medically assisted reproduction.
Dr Walker said that the research was aimed at comparing incidence among populations, not at determining cause and effect. The findings could be explained by an actual treatment effect or be the result of greater medical surveillance and underlying patient factors.
‘We note that women who were parous did not have an increased incidence of uterine, ovarian or melanoma cancers, suggesting against an effect of the treatment,’ he told Medicine Today.
‘Independent of plans for fertility treatment, some women have a higher risk of cancer due to factors related to their infertility, like endometriosis, polycystic ovary syndrome and obesity, and they should be supported to modify their cancer risk,’ Dr Walker explained.
‘Before and after fertility treatment, women should be up to date with the routine cancer screening programs they are eligible for.’