Globus pharyngeus: more than just a lump in the throat

Globus pharyngeus is a common and often distressing sensation of a lump or tightness in the throat. Although usually benign, malignancy must be excluded. Symptoms may result from gastro-oesophageal reflux disease, anxiety or visceral hypersensitivity, with the latter two often overlapping. After appropriate diagnostic testing, a compassionate and reassuring discussion about the benign nature and generally good prognosis is important.
- Globus pharyngeus is a common and intrusive disorder for affected patients.
- Malignant causes are rare, but all patients require investigation. Laryngoscopy and, in most cases, gastroscopy are essential to exclude malignancy and other structural pathologies.
- Gastro-oesophageal reflux disease can cause globus but an objective diagnosis is key for long-term success.
- Anxiety and visceral hypersensitivity are common in patients with globus.
- Pharmacotherapy that targets visceral hypersensitivity can reduce symptoms in most patients.
Globus pharyngeus (globus) is characterised by a lump, tightening or foreign body sensation in the throat. It is a common condition with a very high lifetime prevalence of 22.5 to 45%.1 About 4% of visits to ENT surgeons are related to globus.2 Globus pharyngeus is a diagnosis of exclusion, and although benign and often self-limited, many patients report highly uncomfortable, anxiety-provoking symptoms. Suffering is often compounded by repeated negative investigations and unsuccessful treatment trials. Furthermore, because symptoms can overlap with much rarer but serious disorders such as head and neck malignancies, clinicians need to be well versed in risk assessment, investigation and management of globus.
Aetiology
Multiple and highly varied pathophysiological mechanisms can result in a globus sensation.3 Potential aetiologies are listed in Box 1. Despite extensive evaluation, no specific cause is identified in the majority of patients.
Gastro-oesophageal reflux disease (GORD) can cause globus sensation in some patients;4 however, most patients with severe, pathological GORD (e.g. long segment Barrett’s oesophagus or large hiatus hernias) do not commonly report globus. Conversely, many patients with globus lack typical GORD symptoms, such as heartburn and regurgitation. This likely explains the wide variability (20 to 70%) in the proportion of globus cases attributed to GORD.1,4
Other causes of globus include mucosal irritation, muscle tension, malignant and benign growths, visceral hypersensitivity and anxiety.3 The contribution of anxiety to globus remains debated. The original term ‘globus hystericus’ was challenged by a study showing no major gender differences and no increased prevalence of hysterical personality traits on validated tools compared with the general population.5 However, this contrasts with clinical experience, where anxiety is frequently observed. A more recent large study demonstrated that over half of patients with globus have high scores on a validated personality scale for hysteria, suggesting that anxiety is either a contributing factor or a significant consequence of globus.6 Visceral hypersensitivity, which may occur after upper respiratory tract infections, is also likely a major contributor. Throat clearing and chronic cough are commonly associated features.
Clinical presentation
Most patients with globus initially present to general practitioners, with a peak incidence between 35 and 54 years of age. The condition affects men and women equally. Patients typically describe a lump or foreign body sensation in the throat, and may report swallowing difficulties (Box 2). Overt pain is unusual and is considered a red flag. Specific questioning is essential to obtain a detailed description of symptoms, including duration and onset.
A key distinguishing feature is that globus can often be differentiated from true dysphagia by asking the following question: ‘Is the sensation in your throat more or less noticeable during meals?’ In patients with true dysphagia (e.g. oesophageal stenosis, eosinophilic oesophagitis or major oesophageal motility disorders), symptoms are typically worse during meals. In contrast, globus symptoms are usually less noticeable or absent during meals and more noticeable at rest or when swallowing saliva.
Diagnosis and investigations
The Rome IV criteria for disorders of gut–brain interaction define globus as a persistent or intermittent, nonpainful sensation of a lump or foreign body in the throat, with no structural lesion identified on physical examination, laryngoscopy or endoscopy.7 Diagnostic criteria include:
- occurrence of symptoms between meals
- absence of dysphagia or odynophagia
- absence of a gastric inlet patch in the proximal oesophagus
- absence of evidence that GORD or eosinophilic oesophagitis is the cause
- absence of major oesophageal motor disorders.
To formally diagnose globus per these criteria, all patients would require laryngoscopy via an ENT specialist, gastroscopy and high-resolution oesophageal manometry with or without ambulatory pH testing with a gastroenterologist. However, in clinical practice the approach is often modified.
Investigations in patients with globus should be guided by the presence of red flag symptoms (Box 3), severity and duration of symptoms, pretest probability of GORD and the presence of anxiety.
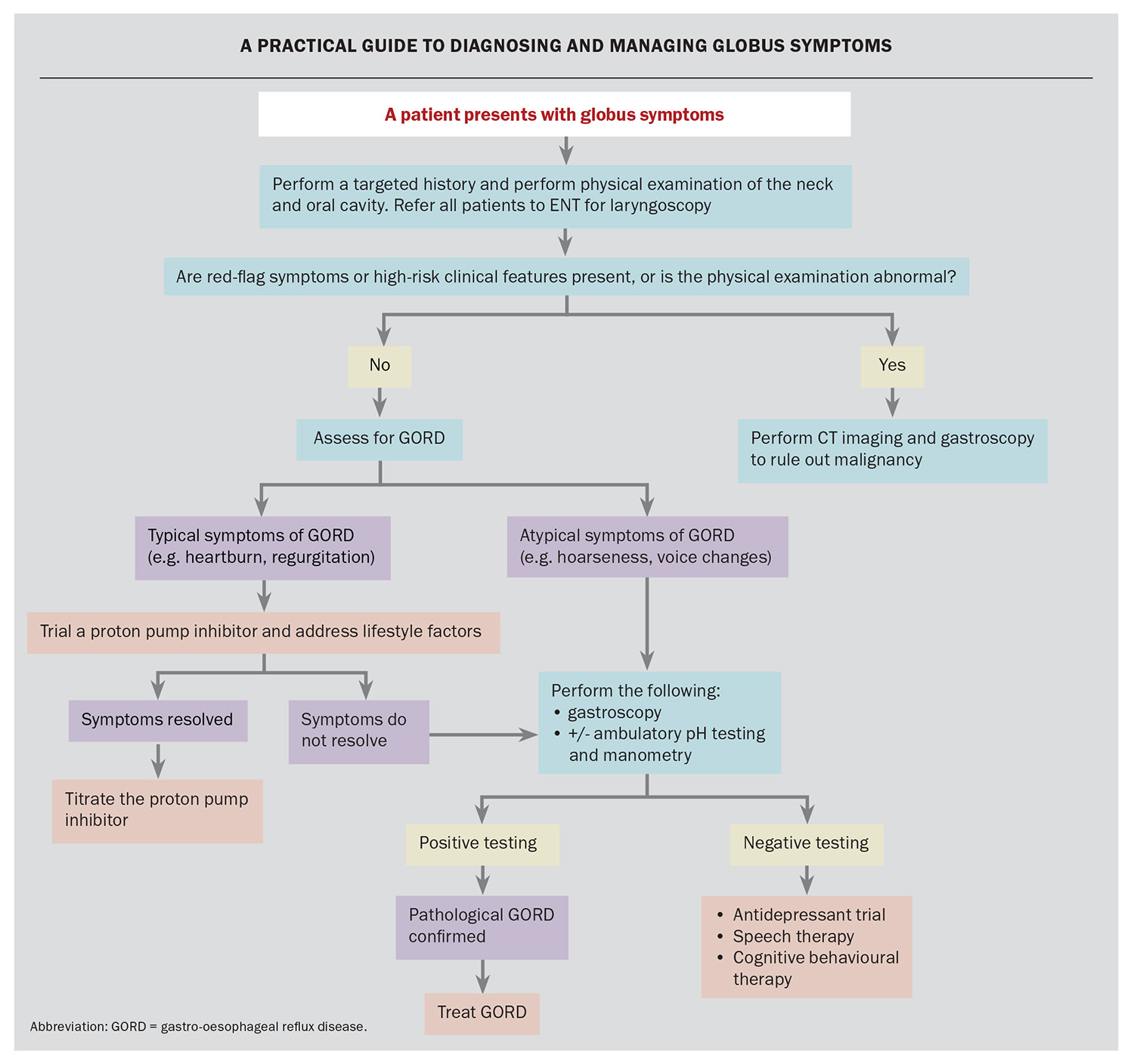
All patients with globus symptoms should undergo ENT assessment with direct visualisation of the pharyngolaryngeal structures with laryngoscopy to rule out malignancy. In patients with red flags, this should occur promptly and be combined with cross-sectional imaging with CT (Flowchart). Oesophagogastroduodenoscopy is frequently used to exclude malignant disorders of the proximal gastrointestinal tract and other disorders that can cause globus. Thyroid ultrasound may be helpful to rule out multinodular goitre and other thyroid pathology which may be contributing to globus.
In patients without typical reflux symptoms, such as heartburn and regurgitation, an empiric trial of proton pump inhibitors (PPIs) is not recommended. Instead, these patients should undergo oesophageal physiological testing (e.g. ambulatory pH impedance testing or wireless pH testing) to confirm or exclude pathological GORD.8 An objective diagnosis of GORD is based on findings such as Los Angeles grade B (or higher) oesophagitis (i.e. oesophageal ulceration greater than 5 mm in length), peptic stricture or Barrett’s oesophagus on endoscopy, as well as ruling out other gastrointestinal disorders that can cause symptoms that overlap with globus (e.g. eosinophilic oesophagitis, achalasia and, in rare cases, acid-producing proximal oesophageal inlet patches). If none of these are present, physiological testing with ambulatory pH studies is recommended.8 The diagnosis of laryngopharyngeal reflux or GORD based solely on laryngoscopic findings is unreliable and does not correlate with gold-standard testing such as ambulatory pH testing.9 Globus should not be attributed solely to anxiety without exclusion of other pathophysiological factors, which require nasendoscopy and gastroscopy at minimum.
When to refer
All patients with globus symptoms should be referred to an ENT specialist for direct visualisation of the oropharyngeal anatomy via laryngoscopy. Although the diagnostic yield is low, it is essential to exclude malignancy. Gastroenterological referral is indicated in patients with true dysphagia and recommended in many other patients. Gastroscopy is usually performed to rule out oesophageal cancer, eosinophilic oesophagitis and complicated GORD. If thyroid abnormalities are identified, endocrinological referral is warranted.
Management
Management of globus pharyngeus is relatively straightforward when a specific cause has been identified, such as an oropharyngeal malignancy, multinodular goitre or other local pathology. However, this is not the case for the majority of patients. The three most common pathophysiological mechanisms for globus in clinical practice are GORD, anxiety and visceral hypersensitivity, with frequent overlap between the latter two.
Management of GORD
If a diagnosis of GORD has been objectively confirmed by endoscopy or oesophageal physiological testing, lifestyle changes and pharmacological therapy should be initiated. Evidence-based lifestyle changes include avoidance of eating three hours prior to bedtime, bed-head elevation and weight loss.10 Pharmacological therapies include PPIs given once or twice daily. Although increasing dosing frequency from once to twice daily provides modest benefit, selecting a higher-potency PPI (e.g. esomeprazole or rabeprazole) over a lower-potency PPI (e.g. pantoprazole or lansoprazole) is a reasonable approach. A three-month therapeutic trial is appropriate before reassessment.
Management of visceral hypersensitivity and anxiety
If visceral hypersensitivity is suspected and GORD has been excluded, a trial of a neuromodulator is a reasonable next step. Two commonly used agents are paroxetine and amitriptyline, despite a relative paucity of high-quality data supporting their efficacy. A randomised trial of 148 patients compared paroxetine, amitriptyline and lansoprazole using the Glasgow–Edinburgh Throat Scale. After six weeks of treatment, 71.7% of patients in the paroxetine group (33/46) achieved a treatment response, compared with 46.2% (24/52) in the amitriptyline group and 14% (7/50) in the lansoprazole group.11 When using paroxetine or amitriptyline, patients need to be educated about potential side effects and a ‘start low, go slow’ approach is recommended.
Nonpharmacological interventions that target visceral hypersensitivity and anxiety have also been used with success. Cognitive behavioural therapy has shown benefit in select patients but lack of widespread expertise, limited access and cost can be barriers in clinical practice. New app- and web-based delivery mechanisms for cognitive behavioural therapy may represent a future treatment avenue for patients with globus.
Conclusion
Globus pharyngeus is a mostly benign but highly distressing condition with poorly elucidated pathophysiology. Although malignancy is rare, it needs to be excluded in all patients. Following appropriate diagnostic testing, including laryngoscopy and, in most cases, gastroscopy, a compassionate and reassuring discussion about the benign nature and overall good prognosis is important. A targeted approach to objectively diagnose GORD, exclude other oesophageal disorders and screen for anxiety is the next logical step. If objective evidence of GORD is identified, a three-month trial of a high-potency PPI is recommended. In patients without GORD, neuromodulation targeting visceral hypersensitivity is the next appropriate step. MT
COMPETING INTERESTS: None.
References
1. Tang B, Cai HD, Xie HL, Chen DY, Jiang SM, Jia L. Epidemiology of globus symptoms and associated psychological factors in China. J Dig Dis 2016; 17: 319-324.
2. Moloy PJ, Charter R. The globus symptom. Incidence, therapeutic response, and age and sex relationships. Arch Otolaryngol 1982; 108: 740-744.
3. Lee BE, Kim GH. Globus pharyngeus: a review of its etiology, diagnosis and treatment. World J Gastroenterol 2012; 18: 2462-2471.
4. Van Daele DJ. Esophageal manometry, pH testing, endoscopy, and videofluoroscopy in patients with globus sensation. Laryngoscope 2020; 130: 2120-2125.
5. Malcomson KG. Globus hystericus vel pharyngis (a recommaissance of proximal vagal modalities). J Laryngol Otol 1968; 82: 219-230.
6. Bouchoucha M, Girault-Lidvan N, Hejnar M, Mary F, Airinei G, Benamouzig R. Clinical and psychological characteristics of patients with globus. Clin Res Hepatol. Gastroenterol 2019; 43: 614-622.
7. Drossman DA. Functional gastrointestinal disorders: history, pathophysiology, clinical features and Rome IV. Gastroenterology 2016; 150: 1262-1279.e2.
8. Gyawali CP, Yadlapati R, Fass R, et al. Updates to the modern diagnosis of GERD: Lyon consensus 2.0. Gut 2024; 73: 361-371.
9. Branski RC, Bhattacharyya N, Shapiro J. The reliability of the assessment of endoscopic laryngeal findings associated with laryngopharyngeal reflux disease. Laryngoscope 2002; 112: 1019-1024.
10. Ness-Jensen E, Hveem K, El-Serag H, Lagergren J. Lifestyle intervention in gastroesophageal reflux disease. Clin Gastroenterol Hepatol 2016; 14: 175-182.e1-3.
11. Chen DY, Jia L, Gu X, Jiang SM, Xie HL, Xu J. Comparison of paroxetine and amitriptyline in the treatment of refractory globus pharyngeus. Dig Liver Dis 2016; 48: 1012-1017.
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.