What’s the diagnosis?
A young woman with pustular finger nodules of acute onset
Case presentation
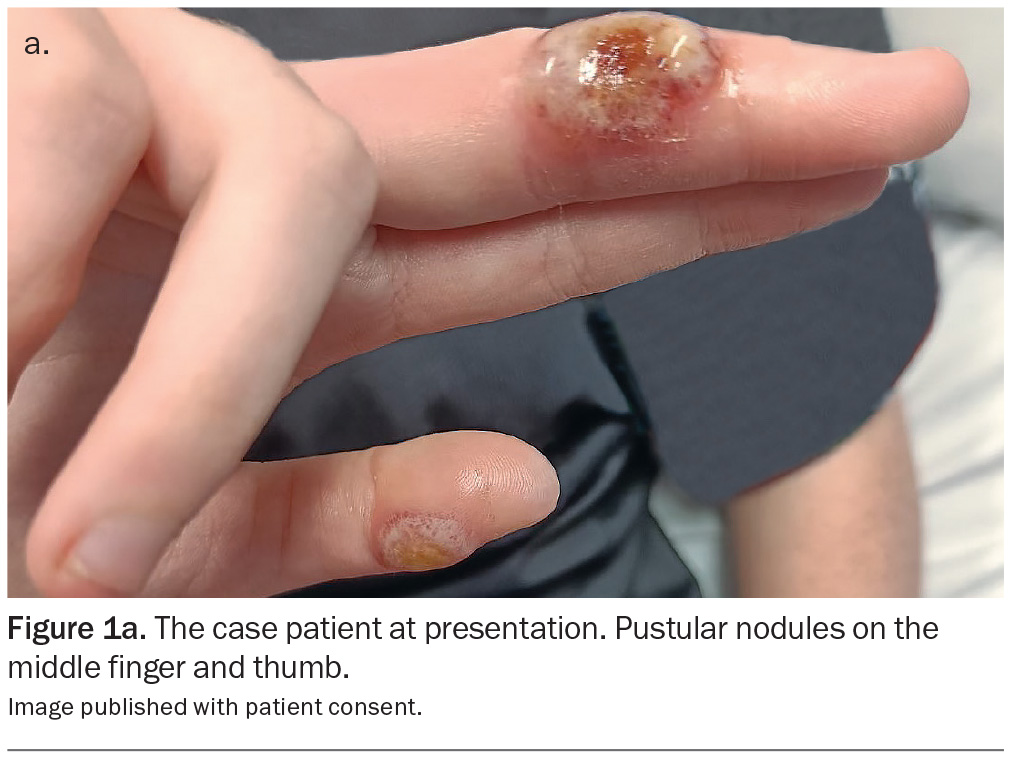
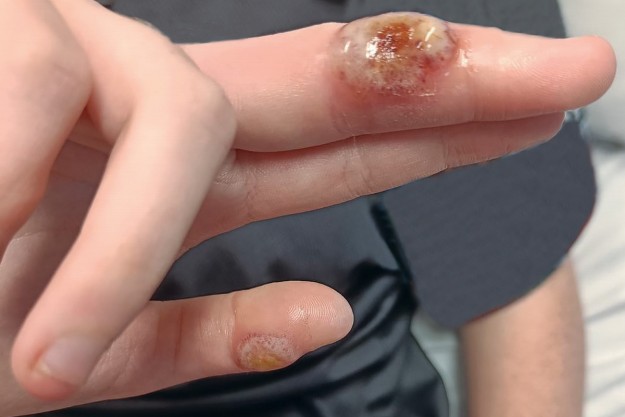
An 18-year-old woman presents with a two-week history of slowly enlarging lesions on the middle finger and thumb of her right hand (Figure 1a). The lesions are painless, and she is systemically well. She has no significant medical history and is not taking any regular medications. The lesions arose two days after a sheep bite to the affected hand.
The patient has completed a course of oral cefalexin, with no improvement. She has also tried a wart treatment (a topical paint containing salicylic acid, lactic acid and podophyllum resin), without response.
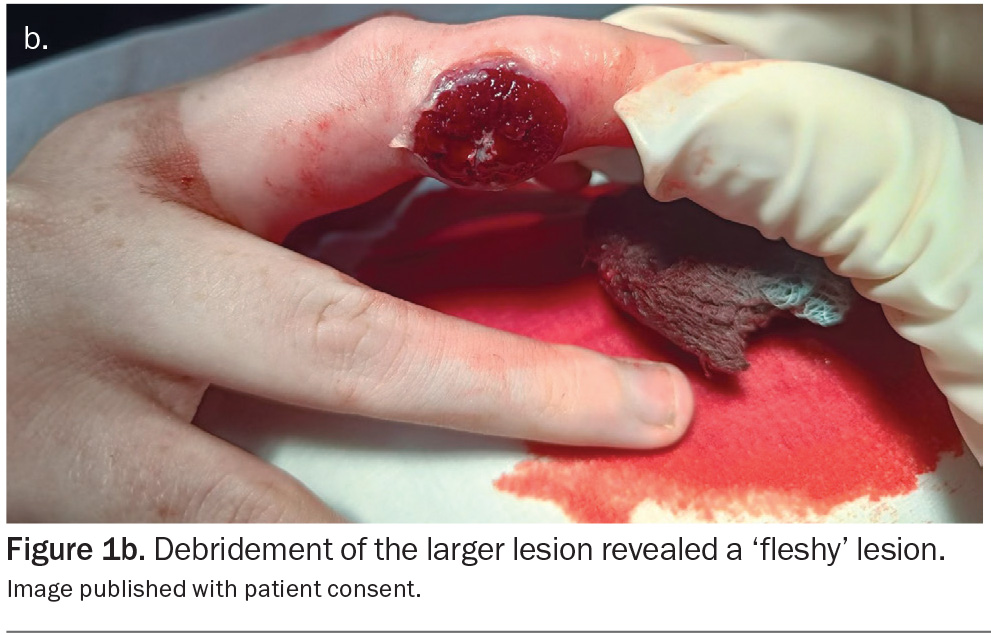
On examination, there is an erythematous, pustular nodule on the lateral middle finger and a smaller similar lesion on the thumb. After debridement, the nodule on the middle finger reveals a ‘fleshy’ lesion (Figure 1b).
Differential diagnoses
Conditions to consider among the differential diagnoses include the following.
Neutrophilic dermatosis of the dorsal hands
Neutrophilic dermatosis of the dorsal hands (NDDH), a localised variant of Sweet syndrome, usually presents as tender nodules, plaques, pustules or bullae, or a combination of these, on the back of the hands.1 The condition is typically seen in elderly patients and often associated with underlying conditions such as haematological malignancies, including myelodysplasia and leukaemia.1 The diagnosis is usually made clinically and confirmed by skin biopsy and histopathological examination, which classically shows a dense neutrophilic infiltrate without vasculitis.
This was not the correct diagnosis for the case patient, who did not match the usual demographic for NDDH and had no comorbidities. However, the pustulonodular appearance of the lesions bore some similarities to this condition.
Mycobacterium marinum infection
Mycobacterium marinum infections are rare, typically occurring in people with recreational or occupational exposure to contaminated water (such as a fish tank), and usually present as a solitary papulonodular lesion on an extremity that may evolve into a sore or abscess.2 In some cases, these atypical mycobacterium infections are associated with sporotrichoid spread (development
of further lesions along the lines of lymphatic drainage).2 The histological findings can be nonspecific, and the diagnosis is confirmed by culture of the organism.
This was not the correct diagnosis for the case patient, who had no history of relevant exposures.
Herpetic whitlow
Herpetic whitlow is a cutaneous lesion caused by herpes simplex virus (HSV) 1 or 2 that typically affects the distal fingers.3 It appears as a painful vesicle or pustule and may be associated with fever or malaise. Herpetic whitlow arises as a result of direct inoculation (exogenous or autogenous) or reactivation of latent virus.3 It is usually diagnosed clinically, with a viral swab sent for HSV polymerase chain reaction (PCR) testing for confirmation.
This was not the correct diagnosis for the case patient, whose lesions were asymptomatic and not vesicular. She had no known history of HSV infection.
Orf
This is the correct diagnosis. Orf (contagious ecthyma) is a zoonotic viral skin infection caused by a parapoxvirus that is usually contracted from sheep or goats. People are commonly inoculated with the virus via broken skin during contact with the lesions of an infected animal or contaminated fomites.
An orf lesion most commonly presents as an erythematous nodule or pustule on the upper limb, typically on the fingers, which may be painful or painless. There are six stages, each lasting approximately seven days.4 The initial lesion appears three to seven days after inoculation as an erythematous macule, which then becomes more vesicular, then targetoid, and subsequently develops into a nodule.4 The lesion then dries out, slowly resolves and finally heals, usually without scarring.
Milker’s nodule, a lesion caused by a parapoxvirus that is contracted from cows, is clinically indistinguishable from orf.5 For the case patient, this diagnosis could be excluded because she had had no exposure to cows.
Complications of orf are uncommon but may include superimposed bacterial infection, lymphadenopathy and lymphangitis. Erythema multiforme and, rarely, induction of autoimmune bullous diseases are other possible complications.6,7
Diagnosis
Orf is usually diagnosed clinically on the basis of characteristic morphology in conjunction with a history of sheep or goat exposure. If required, the diagnosis can be confirmed by laboratory investigations. Parapoxvirus PCR testing performed on a skin swab is a noninvasive investigation that delivers an accurate and rapid diagnosis; however, this may not be available at all institutions.
A punch biopsy and histopathology may aid in diagnosis, with key findings determined by stage of the lesion. In early lesions, these include parakeratosis, acanthosis, viral cytopathic changes and eosinophilic inclusions.8 In later lesions, the findings include dermal oedema, papillomatosis and capillary proliferation.8
Management
In most cases, orf is a mild, self-limiting illness that does not require specific treatment as the lesions resolve spontaneously in four to eight weeks. Regular wound care is routinely recommended to reduce the risk of secondary bacterial infection and to prevent reinfection.9 Immunosuppressed individuals are at higher risk of developing persistent or ‘giant’ lesions (large orf lesions with atypical appearance) and may attract a lower threshold for active treatment.10
There is no specific treatment for orf. If required, management options include intralesional interferon, electrocautery, topical imiquimod, cryotherapy and surgical excision.11
Outcome
For the case patient, a diagnosis of orf was suspected on the basis of the clinical features and history of contact with sheep. A swab sent for parapoxvirus PCR testing returned a positive result that confirmed the diagnosis. She was discharged with simple dressings on the lesions and advised to monitor for any signs of superimposed infection. At a follow-up visit one week after her initial presentation, both lesions were significantly reduced in size with signs of healing evident.
Key point
Orf is an infrequent diagnosis that can go unrecognised. Correct diagnosis is important to avoid unnecessary investigations and overtreatment. MT
COMPETING INTERESTS: None.
References
1. Micallef D, Bonnici M, Pisani D, Boffa MJ. Neutrophilic dermatosis of the dorsal hands: a review of 123 cases. J Am Acad Dermatol 2023; 88: 1338-1344.
2. Gluckman SJ. Mycobacterium marinum. Clin Dermatol 1995; 13: 273-276.
3. Feder HM Jr, Long SS. Herpetic whitlow. Epidemiology, clinical characteristics, diagnosis, and treatment. Am J Dis Child 1983; 137: 861-863.
4. Huerter CJ, Alvarez L, Stinson R. Orf: case report and literature review. Cleve Clin J Med 1991; 58: 531-534.
5. Handler NS, Handler MZ, Rubins A, et al. Milker’s nodule: an occupational infection and threat to the immunocompromised. J Eur Acad Dermatol Venereol 2018; 32: 537-541.
6. Joseph RH, Haddad FA, Matthews AL, Maroufi A, Monroe B, Reynolds M. Erythema multiforme after orf virus infection: a report of two cases and literature review. Epidemiol Infect 2015; 143: 385-390.
7. White KP, Zedek DC, White WL, et al. Orf-induced immunobullous disease: a distinct autoimmune blistering disorder. J Am Acad Dermatol 2008; 58: 49-55.
8. Teng YS, Yang TT. Orf With lymphangitis. JAMA Dermatol 2025; 161: 972-973.
9. Thompson HJ, Harview CL, Swick B, Powers JG. Orf virus in humans: cases and clinical review. Cutis 2022; 110: 48-52.
10. Zaharia D, Kanitakis J, Pouteil-Noble C, Euvrard S. Rapidly growing orf in a renal transplant recipient: favourable outcome with reduction of immunosuppression and imiquimod. Transpl Int 2010; 23: e62-4.
11. Bergqvist C, Kurban M, Abbas O. Orf virus infection. Rev Med Virol 2017; 27. doi: 10.1002/rmv.1932.
Skin lesions
Rural health concerns