Unusual primary headaches - keys to an accurate diagnosis

A patient presents to you with recurrent headaches that do not quite fit the pattern of migraine or tension-type headaches. Which disorders should you consider?
- Primary headache disorders other than migraine and tension-type headache are less well known; however, not all are rare and they will occasionally be encountered in general practice.
- The trigeminal autonomic cephalgias (TACs) are short-lasting headaches with prominent autonomic features and should be differentiated from short-lasting headaches without autonomic features.
- Photophobia and phonophobia are usually unilateral in TACs but are bilateral in migraine, even when the pain is lateralised.
- Autonomic symptoms in TACs tend to be lateralised to the side of the pain, prominent and consistent between attacks. In contrast, those in migraine are generally mild, bilateral and do not correlate with attack severity.
- The diagnosis of other recurrent primary headache disorders is often suggested by specific triggers (e.g. sexual activity, exertion, coughing) or distinctive pain characteristics (e.g. local, brief stabbing pain, or focal coin-shaped area of pain).
Most patients with headache have a primary headache disorder, with migraine and tension-type headache being the most common. Primary headache disorders are so common that even the less well known varieties will be seen occasionally in general practice: this paper addresses a number of these. Formal diagnostic criteria are published in the International Classification of Headache Disorders (3rd edition).1 An approach to diagnosis and investigation to exclude causes of secondary headache is included as a separate paper in this collection.2
Trigeminal autonomic cephalgias
Trigeminal autonomic cephalgias (TACs) represent four conditions: cluster headache; short-lasting unilateral neuralgiform headache with conjunctival injection and tearing (SUNCT) and short-lasting unilateral neuralgiform headache with cranial autonomic symptoms (SUNA); hemicrania continua; and paroxysmal hemicrania. A patient who experiences a TAC will typically report the ‘three As’:
- anterior, side-locked pain
- autonomic features
- a sense of internal agitation or restlessness during exacerbations.
Autonomic features (which occur on the side of the headache) include:
- facial flushing, pallor or sweating
- redness, tearing or itchy/gritty sensation of the eye
- nasal congestion or rhinorrhoea
- drooping of the eyelid (ptosis), change in pupillary size (miosis), or Horner’s syndrome
- ear fullness
- salivation.
Photophobia and phonophobia in TACs are usually unilateral, in contrast to the bilateral sensitivity seen in migraine.3 Autonomic features in TACs are typically lateralised to the side of the pain, prominent and consistent between attacks, whereas in migraine they are generally milder, bilateral and not correlated with attack severity.
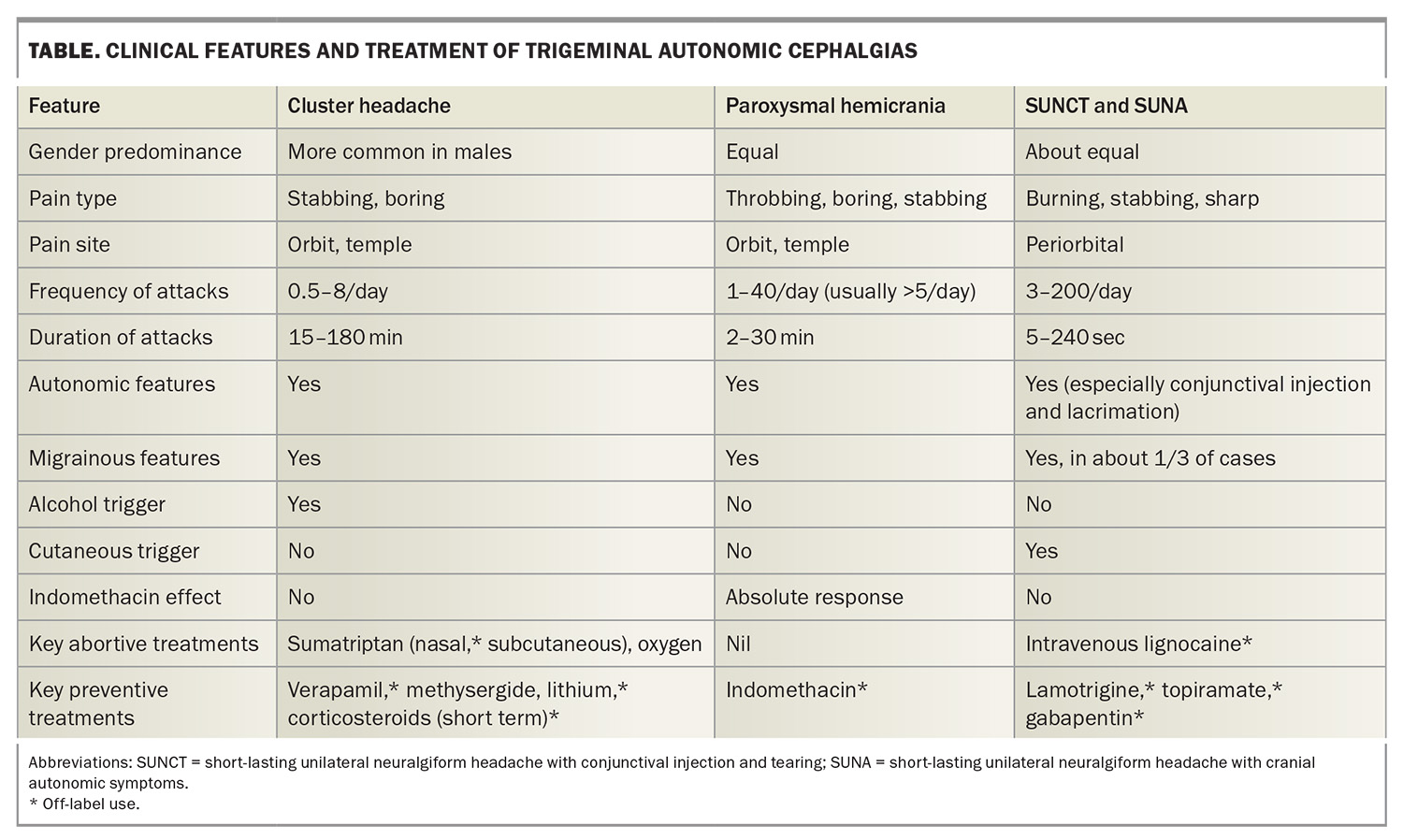
Subtypes of TACs can usually be distinguished by the cycle pattern and the length and frequency of the attacks (Table). Hemicrania continua and SUNCT/SUNA are easily distinguishable by the length of their attacks (continuous, and seconds, respectively). Cluster headache is differentiated from paroxysmal hemicrania by the timing of attacks (typically 2200–0200, more common in the springtime), the duration of attacks (average 90 minutes vs 15 minutes), average number of daily attacks (one vs five) and their differential response to acute therapies.
Other potentially catastrophic causes of sudden headache should always be considered, particularly in acute presentations. These include aneurysmal disease, subarachnoid haemorrhage, arterial dissection and acute angle closure glaucoma (which may present with headache, tearing and redness of the eye, as well as agitation).
Pituitary gland pathology may accompany TACs – up to 10% of patients with pituitary tumours and headache present with a TAC phenotype.4 MRI with pituitary views and pituitary function testing are thus appropriate in the workup of patients with an initial TAC presentation.
Cluster headache
Cluster headache affects around 0.1% of the population,5 with a male predominance, a higher frequency in cigarette smokers, and peak onset in the second and third decade of life.6 The headaches are severe and boring in quality, lasting 15 to 180 minutes, and typically occur in the orbital, supraorbital or temporal regions. Patients often describe the pain as the worst they have experienced, rivalling even childbirth. Marked agitation and restlessness are usually associated with cluster headache, in contrast with the avoidance of movement seen during attacks of migraine.6 Patients are usually asymptomatic between attacks.
Cluster headaches tend to occur in bouts, with the attacks within a bout linked to the circadian rhythm, occurring at the same time each day. Also, bouts exhibit a circannual periodicity; they are often more frequent in spring or autumn, around the time that the clocks change for daylight saving, and typically last about eight to 10 weeks.
Alcohol, nitrates, exercise and warmth may trigger attacks, but only in ‘at-risk’ periods. The attacks may be associated with ‘migrainous’ features, such as photophobia, phonophobia, nausea and vomiting. However, the other clinical features and temporal pattern are so distinctive that diagnostic confusion between cluster headache and migraine should be rare.
Cluster headaches are classified according to the duration of the bout. Episodic forms occur in bouts lasting seven days to one year, with bouts separated by at least a one-month pain-free period, while a chronic cluster lasts for one year or longer, without remissions or with less than one month of remission.7
As headache resembling cluster headache may occur secondary to a number of structural pathologies, good quality imaging with MRI focused especially on the pituitary and cavernous sinus region is prudent in all cases.
Management of cluster headaches involves both preventive and acute treatment measures. Agents to abort the acute attack include:
- 100% oxygen administered at 12 to 15 L/min via a non-rebreather mask for 15 to 20 minutes
- subcutaneous sumatriptan 6 mg
- intranasal sumatriptan 20 mg (off-label use, currently limited access in Australia).
Oral triptans are not usually helpful because by the time they become effective, the relatively short duration cluster headache is already spontaneously subsiding.
Preventive treatments are useful in patients with chronic cluster headache and may shorten the duration of the active period in those with the episodic form. Options for prevention depend on the length of the bout. Longer bouts require safe and effective agents that can be administered long term, such as verapamil, lithium and topiramate (all off-label uses), whereas shorter bouts may be managed by prednisolone (off-label use), which acts quickly but should not be used for long periods.
Verapamil often needs to be used at higher than usual doses, reached by gradually increasing the dose: up to 960 mg/day in split doses of the immediate release form has been used. There is a risk of conduction block occurring with higher doses, so two weekly monitoring with ECG after each dose increase to detect any emerging conduction block (lengthening of the PR interval) should be performed before the next increase. Six-monthly ECG can be performed when a stable dose is reached.8
A useful strategy for patients with episodic cluster headache is to use prednisolone (starting at 75 mg/day and weaning rapidly to zero over two to three weeks) as a means of gaining rapid control of the bout, and starting verapamil at low dose (for example, up to 80 mg thrice daily, increasing by up to 80 mg every two weeks) at the same time. The verapamil thus starts to have an impact as the prednisolone is weaned.
Other treatments include greater occipital nerve block (with corticosteroids and local anaesthetic) and surgical options for refractory cases (e.g. occipital nerve stimulators, posterior hypothalamic neurostimulation).9,10
SUNCT and SUNA
SUNCT and SUNA are rare TACs characterised by short-duration attacks of unilateral head pain with associated autonomic features, often triggered by cutaneous stimuli. SUNCT is defined by the presence of significant tearing and conjunctival injection, and SUNA by their absence; however, these conditions are clearly part of the same spectrum.
These headaches are an important differential diagnosis for trigeminal neuralgia. Key distinguishing features of SUNCT/SUNA include pain typically localised to the ophthalmic division of the trigeminal nerve (rare for trigeminal neuralgia) and the presence of autonomic features. Cutaneous triggers of pain paroxysms are often a feature of both trigeminal neuralgia and SUNCT/SUNA. However, trigeminal neuralgia is characteristically associated with a ‘refractory period’ during which the same cutaneous trigger is unable to reproduce the pain for a brief period after an attack.11 The pain of SUNCT/SUNA may present as short-lived single stabs (lasting five to 240 seconds), groups of stabs, or a saw-tooth pattern where the pain does not return to baseline between stabs and the attack lasts several minutes.
Patients with these headaches show no response to indomethacin (see paroxysmal hemicrania) or to the typical relievers for cluster headache. The most effective treatment is lamotrigine, with some efficacy also seen for topiramate and gabapentin (all off-label uses). Ten days of intravenous lignocaine treatment may also induce a remission.12
Paroxysmal hemicrania
Paroxysmal hemicrania comprises short attacks of severe unilateral pain (lasting two to 30 minutes), typically in the ophthalmic division, occurring several times daily and accompanied by autonomic features. There is often associated unilateral photophobia and phonophobia, as well as restlessness and agitation. The attacks usually occur during the day, and a small percentage are triggered by alcohol or a manual trigger, such as head movement and pressure on C4 or C5, the C2 root or the greater occipital nerve. There are no cutaneous triggers, such as seen in SUNCT/SUNA. Paroxysmal hemicrania may be episodic (with remissions lasting more than one month) or chronic (with no remission in one year).
Paroxysmal hemicrania exhibits a lasting response to indomethacin; however, in patients intolerant to the gastric effects of this medication, the alternatives are less clearly defined. Cyclooxygenase-2 inhibitors, topiramate and greater occipital nerve block with lidocaine and methylprednisolone acetate may be beneficial (all off-label uses).13
Hemicrania continua
Hemicrania continua is a continuous side-locked headache of varying intensity. Exacerbations may be accompanied by ipsilateral autonomic symptoms as well as migrainous features (nausea, photophobia, phonophobia). The background pain in hemicrania continua is greater than the interparoxysmal pain seen in other TACs, and the exacerbations longer in duration – features that help distinguish it from paroxysmal hemicrania.
There is a complete resolution of the headache with therapeutic doses of indomethacin, which is one of the diagnostic criteria. Similarly to paroxysmal hemicrania, topiramate, greater occipital nerve block and occipital nerve stimulators have all been reported to be beneficial.14,15
An oral indomethacin test may be performed using a regimen of 25 mg thrice daily for one week, increasing to 50 mg thrice daily in the second week and 75 mg thrice daily in the third. The patient should keep a headache diary before and during the test so changes in pain scores can be evaluated. Prophylactic use of a proton pump inhibitor is advisable to reduce the risk of gastrointestinal complications. If the test is positive, the dose can be gradually decreased by 25 mg thrice daily every few weeks until the minimal effective dose is established.
Miscellaneous primary headaches
There are a number of other headache syndromes with characteristic patterns, some of which occur after specific triggers. These conditions are not rare.
Primary stabbing headache
Primary stabbing headache, also known as ‘jabs and jolts’ or the more evocative ‘ice-pick pains’, is a term patients readily identify with, as the pain is often described as being like a very brief and localised stab into the head.
The pain occurs spontaneously (unprovoked), with 80% of stabs lasting three seconds or less. The attack frequency is generally low and will occur outside of the distribution of the trigeminal nerve in 70% of cases. Although the pain is often confined to one area, in some patients it may shift locations, including to the opposite side of the head. There are usually no accompanying symptoms such as nausea, photophobia or autonomic changes. Physical examination and imaging, if performed, are typically normal.
This condition is not rare, though many patients do not bother to report it. Others, however, may be concerned that it represents serious pathology and are reassured by a definite diagnosis. Rarely is the condition disabling, and most patients do not require treatment. Many patients with primary stabbing headache also experience migraine,16 in which case the stabbing pains are felt predominantly on the side most affected during migraine attacks.
The differential diagnoses would include brief forms of TACs such as SUNCT and paroxysmal hemicrania, but these would typically have associated autonomic symptoms. A positive response to indomethacin in affected patients has been reported in some uncontrolled studies, whereas others have found partial or no response.
Cough headache
Cough headache is a headache of sudden onset, lasting from one second to 30 minutes, brought on by, and occurring only in association with, coughing, straining or the Valsalva manoeuvre.17 It is typically bilateral, very abrupt in onset and reaches peak severity immediately. The pain then subsides gradually over 15 to 30 seconds, often with a pulsatile quality during this time.
In about 40% of cases, an underlying pathology is found. The most common such cause is Chiari malformation. This makes sense as the headache can be explained by failure of intracranial and intraspinal pressures to equilibrate immediately (as they normally do) after coughing or straining. The raised intrathoracic pressure is transmitted through the venous system to the intracranial cavity. If there is then a pressure gradient across the foramen magnum, pain will arise from traction on meninges, vessels and other pain-sensitive structures in the region. The pain wanes as pressures gradually equalise. Other reported causes include spontaneous intracranial hypotension, carotid or vertebrobasilar disease, and tumours in the middle or posterior fossa.
Cough headache obviously mandates careful imaging of the brain, and the region of the foramen magnum in particular. MRI provides excellent views of this area, but the radiologist must be alerted that this is the area of interest.
Patients with no abnormalities on imaging are classified as having ‘primary cough headache’, formerly called ‘benign cough headache’. It is plausible that some cases may involve structural abnormalities too subtle to detect radiologically. The authors report one case in which the symptoms were relieved after surgical exploration of the region showed fine bands of arachnoid tissue that were then cleared away.
Cough headache often responds, at least partially, to indomethacin. However, this response occurs both in primary cases and in those with demonstrable obstruction, and is therefore not diagnostically specific.
Primary headache associated with sexual activity
Two subtypes of primary headache are associated with sexual activity (‘benign sex headache’). The less common pre-orgasmic subtype starts as a dull bilateral ache in the head and neck that intensifies with sexual arousal and is often associated with awareness of neck or jaw muscle contraction. The more common and more severe form occurs at orgasm and is explosive and instantaneous in onset. It is thus a form of thunderclap headache and subarachnoid haemorrhage must be the provisional diagnosis until definitely excluded.
Orgasmic headache is severe and patients are typically appropriately anxious about a serious cause; once this is excluded, they remain anxious about the effect recurrent headaches might have on their quality of life. The natural history of orgasmic headache is for recurrences to occur (with sexual activity or with lifting or straining) over a period of a few weeks and then for the condition to subside. During the period of susceptibility, indomethacin may provide some symptomatic relief and there is some anecdotal evidence that beta blockers (such as propranolol) or calcium channel blockers (such as verapamil) may also be of value (all off-label uses).
There are many similarities between orgasmic headache and the thunderclap headache seen in reversible cerebral vasoconstriction syndrome (RCVS). RCVS may cause single or recurrent episodes (over a few weeks) of instantaneous headache and is diagnosed when computed tomography angiography, magnetic resonance angiography or other vascular imaging shows vasospasm. It may be triggered by various stimuli, often of an adrenergic nature (such as cocaine or amphetamine use), but also by sexual activity.
It is tempting, therefore, to conclude that many cases of orgasmic headache may be a version of RCVS. In a recent study in which detailed vascular imaging was carried out in 30 patients with orgasmic headache, 60% had evidence of RCVS.18 Importantly, clinical features were similar in those with and without vasospasm on imaging, suggesting considerable overlap between the two conditions.
Primary exercise headache
Primary exercise headache, previously called primary or benign exertional headache, likely represents a heterogenous group of conditions. Its pathophysiology is unknown, but it is believed to have a vascular origin, with researchers hypothesising that venous or arterial distension secondary to exercise is the pain-inducing mechanism. It typically occurs after intense physical activity, particularly in hot weather or at high altitude, with ‘weightlifter’s headache’ being a recognised subtype.
Exercise headache is not uncommon. One survey found 30% of adolescents experienced headaches during or after physical activity. These headaches were often bilateral, pulsating and brief (lasting less than an hour).19 Migraine was a predisposing factor: 47% of individuals with migraine reported exercise headache, compared with 21% of those without.
Hypnic headache
Hypnic headache is a rare primary headache disorder, predominantly affecting older adults (average age of onset is about 60 years). It is characterised by headaches that occur exclusively during sleep, typically once or twice nightly, and are disruptive enough to wake the patient.20 The pain may be unilateral or bilateral and is usually severe or at least moderately severe.
Patients often find some relief by getting up and moving about, and many report that drinking caffeine helps. Prophylactic treatments that are sometimes effective include caffeine before bed, lithium, topiramate, indomethacin, melatonin and amitriptyline (all off-label uses).
Nummular headache
Nummular headache is a rare primary headache disorder in which there is a focal ‘coin-shaped’ circumscribed area of pain, two to six cm in diameter (from the Latin nummulus, a small coin).21 Nummular headache is typically persistent in type with some superimposed exacerbations of more severe pain (which is still usually described as a dull ache). Sharp pain or local tenderness is rare.
No treatment is reliably effective, although there is an anecdotal report of benefit from botulinum toxin injection in a small number of patients.22 The natural history is very variable: some cases resolve spontaneously, whereas others may persist for years.
Exploding head syndrome
Exploding head syndrome involves alarming but painless episodes described as a loud ‘explosion’ in the head. Attacks tend to occur at the onset of sleep, even at the start of daytime naps.
This condition is probably not rare. When Pearce first described 10 cases with this evocative name, it received substantial press coverage, and he was then inundated with correspondence describing similar cases. Within a year, he was able to publish a review of 50 well-documented cases.23 The cause remains uncertain but the timing suggests a similarity to the other physiological phenomena, such as nocturnal myoclonus, that mark the transition from wakefulness to stage one sleep.
No established treatment exists, but clomipramine has been used anecdotally.
Ice cream headache
Ice cream headache is so common that it is almost a normal phenomenon. It is termed officially (but more prosaically) as ‘headache attributed to ingestion or inhalation of a cold stimulus’. The short-lasting pain, which may be severe, is induced in susceptible individuals by the passage of cold material over the palate or posterior pharyngeal wall.
Ice cream headache affects about 40% of adolescents.24 Like exercise headache, it occurs more often in individuals with migraine: one study reported it in 55% of people with migraine, compared with 29% of those with no background history of headache.24 Another study found that cold-induced headache was triggered experimentally in 74% of people with migraine (who often reported unilateral throbbing pain) and in only 32% of patients with tension-type headache (whose pain was usually bilateral and not throbbing).25
Summary
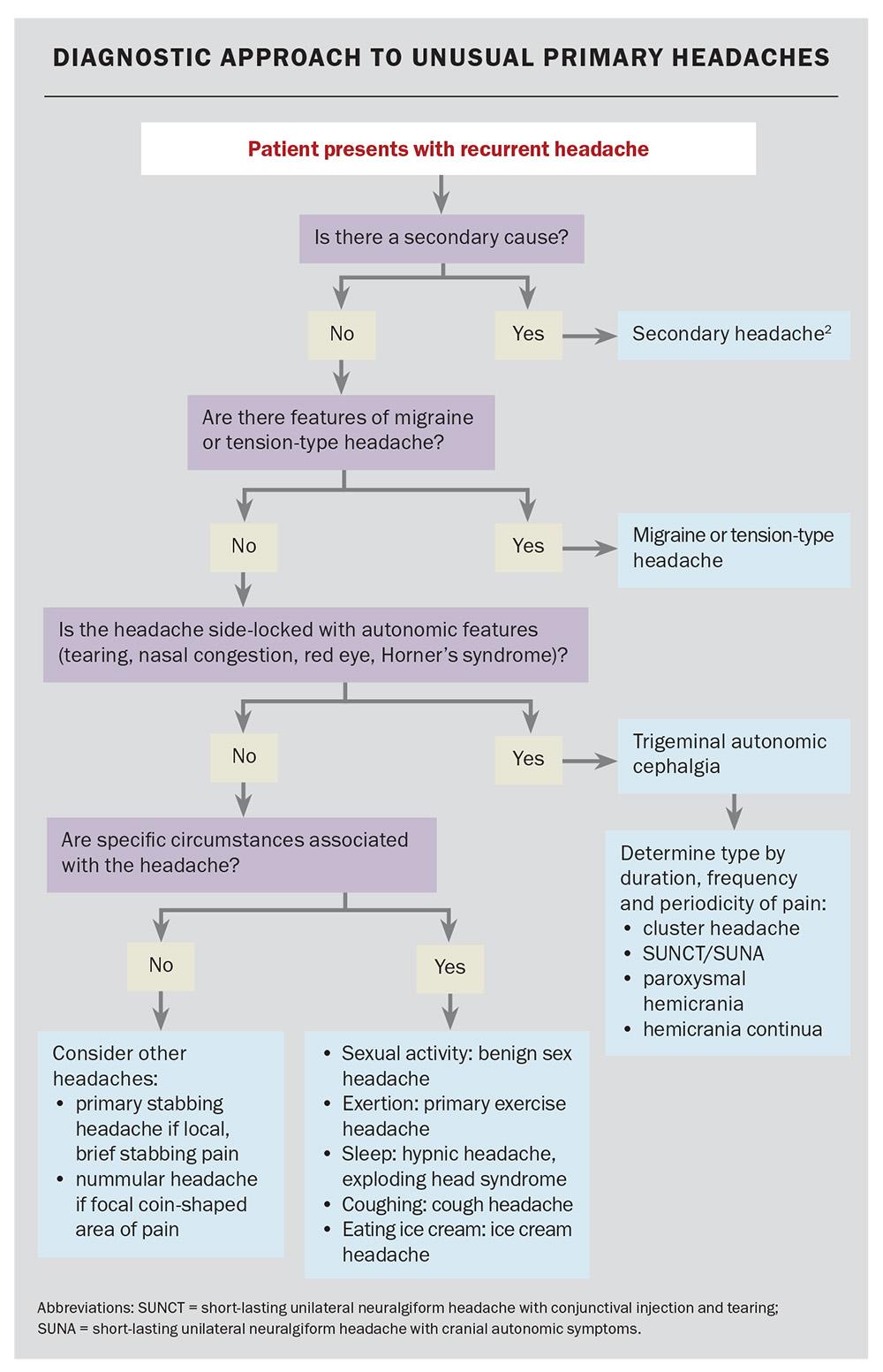
Although some of the primary headache disorders are relatively uncommon, GPs will occasionally encounter them in practice. The strictly unilateral nature and associated autonomic features of the TACs are strong diagnostic clues. For many of the other headache types, specific trigger factors (sexual activity, exertion, sleep or coughing) can offer diagnostic clues. The flowchart provides a diagnostic approach to patients presenting with recurrent headaches. MT
COMPETING INTERESTS: Dr Hutton has served on advisory boards for Sanofi-genzyme, Novartis, Teva, Eli Lilly, Allergan and Lundbeck; been involved in clinical trials sponsored by Novartis, Teva, Xalud and Cerecin; and received payment for educational presentations from Allergan, Teva, Eli Lilly and Novartis. Dr Ray has received honoraria for educational presentations for AbbVie, Novartis and Viatris. He has served on medical advisory boards for Pfizer, Viatris and Eli Lilly. His institution has received funding for research grants, clinical trials and projects supported by the International Headache Society, Brain Foundation, Lundbeck, AbbVie, Pfizer and Aeon. Professor Stark has served on advisory boards for Teva, Eli Lilly, AbbVie, Viatris and Lundbeck; and received payment for educational presentations from AbbVie, Teva, Eli Lilly and Viatris.
References
1. Headache Classification Committee of the International Headache Society. The International Classification of Headache Disorders, 3rd ed. Cephalalgia 2018; 38(Suppl 1): 1-211.
2. Stark RJ. Headache: Investigating the cause. Med Today 2025; 26(7 Suppl): 2-7.
3. Irimia P, Cittadini E, Paemeleire K, Cohen AS, Goadsby PJ. Unilateral photophobia or phonophobia in migraine compared with trigeminal autonomic cephalalgias. Cephalalgia 2008; 28: 626-630.
4. Levy MJ, Matharu MS, Meeran K, Powell M, Goadsby PJ. The clinical characteristics of headache in patients with pituitary tumours. Brain 2005; 128: 1921-1930.
5. Tonon C, Guttmann S, Volpini M, Naccarato S, Cortelli P, D’Alessandro R. Prevalence and incidence of cluster headache in the Republic of San Marino. Neurology 2002 14; 58: 1407-1409.
6. Lambru G, Matharu MS. Trigeminal autonomic cephalalgias: a review of recent diagnostic, therapeutic and pathophysiological developments. Ann Indian Acad Neurol 2012; 15(Suppl 1): S51-S61.
7. Matharu MS, Goadsby PJ. Trigeminal autonomic cephalgias. J Neurol Neurosurg Psychiatry 2002; 72(Suppl 2): ii19-ii26.
8. Cohen AS, Matharu MS, Goadsby PJ. Electrocardiographic abnormalities in patients with cluster headache on verapamil therapy. Neurology 2007; 69: 668-675.
9. Burns B, Watkins L, Goadsby PJ. Treatment of intractable chronic cluster headache by occipital nerve stimulation in 14 patients. Neurology 2009; 72: 341-345.
10. Leone M, Proietti Cecchini A, Franzini A, et al. Lessons from 8 years’ experience of hypothalamic stimulation in cluster headache. Cephalalgia 2008; 28: 787-797; discussion 798.
11. Cohen AS, Matharu MS, Goadsby PJ. Short-lasting unilateral neuralgiform headache attacks with conjunctival injection and tearing (SUNCT) or cranial autonomic features (SUNA) – a prospective clinical study of SUNCT and SUNA. Brain 2006; 129: 2746-2760.
12. Matharu MS, Cohen AS, Boes CJ, Goadsby PJ. Short-lasting unilateral neuralgiform headache with conjunctival injection and tearing syndrome: a review. Curr Pain Headache Rep 2003; 7: 308-318.
13. Cohen AS, Goadsby PJ. Paroxysmal hemicrania responding to topiramate. J Neurol Neurosurg Psychiatry 2007; 78: 96-97.
14. Brighina F, Palermo A, Cosentino G, Fierro B. Prophylaxis of hemicrania continua: two new cases effectively treated with topiramate. Headache 2007; 47: 441-443.
15. Burns B, Watkins L, Goadsby PJ. Treatment of hemicrania continua by occipital nerve stimulation with a bion device: long-term follow-up of a crossover study. Lancet Neurol 2008; 7: 1001-1012.
16. Guerrero AL, Herrero S, Peñas ML, et al. Incidence and influence on referral of primary stabbing headache in an outpatient headache clinic. J Headache Pain 2011; 12: 311-313.
17. Calandre L, Hernandez-Lain A, Lopez-Valdes E. Benign Valsalva’s maneuver-related headache: an MRI study of six cases. Headache 1996; 36: 251-253.
18. Yeh YC, Fuh JL, Chen SP, Wang SJ. Clinical features, imaging findings and outcomes of headache associated with sexual activity. Cephalalgia 2010; 30: 1329-1335.
19. Chen SP, Fuh JL, Lu SR, Wang SJ. Exertional headache – a survey of 1963 adolescents. Cephalalgia 2009; 29: 401-407.
20. Holle D, Naegel S, Krebs S, et al. Clinical characteristics and therapeutic options in hypnic headache. Cephalalgia 2010; 30: 1435-1442.
21. Moon J, Ahmed K, Garza I. Case series of sixteen patients with nummular headache. Cephalalgia 2010; 30: 1527-1530.
22. Mathew NT, Kailasam J, Meadors L. Botulinum toxin type A for the treatment of nummular headache: four case studies. Headache 2008; 48: 442-447.
23. Pearce JM. Clinical features of the exploding head syndrome. J Neurol Neurosurg Psychiatry 1989; 52: 907-910.
24. Fuh JL, Wang SJ, Lu SR, Juang KD. Ice-cream headache – a large survey of 8359 adolescents. Cephalalgia 2003; 23: 977-981.
25. Selekler HM, Erdogan MS, Budak F. Prevalence and clinical characteristics of an experimental model of ‘ice-cream headache’ in migraine and episodic tension-type headache patients. Cephalalgia 2004; 24: 293-297.