The snotty-nosed kid – a practical approach to recurrent or chronic rhinorrhoea in children

Recurrent or chronic rhinorrhoea in children is usually due to overlapping viral upper respiratory tract infections but may reflect allergic rhinitis, adenoidal disease or chronic rhinosinusitis. A structured assessment helps distinguish these causes, identify red flags and guide stepwise management while avoiding unnecessary antibiotics and investigations.
- Symptom duration helps identify the most likely underlying cause of recurrent or chronic rhinorrhoea in children. Episodes lasting up to 10 days usually reflect viral upper respiratory tract infection, persistence beyond 14 days or deterioration after initial improvement raises suspicion for acute bacterial sinusitis and symptoms persisting for 12 weeks or longer suggest chronic rhinosinusitis.
- Persistent unilateral, malodorous discharge, epistaxis, facial swelling or orbital or neurological signs require urgent assessment.
- Intranasal saline (e.g. via sprays or irrigation) is first-line treatment for most cases and can reduce symptom burden.
- Targeted therapy is guided by the likely cause, with antibiotics reserved for suspected bacterial disease and imaging or specialist referral reserved for red-flag features or failure of optimal medical management.
A child with chronic or recurrent rhinorrhoea – often referred to as the ‘snotty-nosed kid’ – is one of the most frequent presentations in general practice. Although nasal discharge is often caused by benign, self-limiting viral infections, persistent or recurrent nasal discharge may indicate allergic rhinitis, adenoid hypertrophy, chronic rhinosinusitis, an intranasal foreign body or rarer conditions. This article equips GPs to distinguish between these possibilities, understand when to investigate or refer, and apply evidence-based management strategies to improve outcomes and minimise unnecessary interventions.
Epidemiology and pathophysiology
The epidemiology and pathophysiology of chronic or recurrent rhinorrhoea depend on the underlying cause. In children, rhinorrhoea often begins with overlapping viral upper respiratory tract infections (URTIs) and may progress to chronic rhinosinusitis in a subset of patients. Adenoid hypertrophy and adenoiditis may perpetuate nasal obstruction and impair mucociliary clearance, whereas allergic rhinitis contributes a via distinct inflammatory pathway. Other causes should be considered when the clinical features do not fit these common patterns.
Viral upper respiratory tract infections
Preschool-aged children typically experience six to eight URTIs each year, with symptoms lasting up to seven to 10 days. Overlap between sequential infections means ongoing rhinorrhoea is common and is often mistaken for chronic disease. Acute bacterial sinusitis may develop when symptoms persist beyond 14 days or worsen after initial improvement. A minority (about 5 to 13% of acute cases) progress to chronic rhinosinusitis.1
Chronic rhinosinusitis
Chronic rhinosinusitis in children is defined by 12 weeks or more of symptoms (nasal discharge or obstruction, cough, facial pain or pressure) or by mucosal findings on endoscopy or CT imaging. Prevalence estimates vary from 2 to 6% in general paediatric cohorts, with higher incidence in school-age children.2,3 Quality of life impacts include sleep disturbance, sleep-disordered breathing, cough, halitosis and association with comorbid asthma.2,3
Adenoid hypertrophy and adenoiditis
Adenoids naturally enlarge during childhood (peaking at 6 to 10 years of age) and involute by adolescence. About one-third of children have clinically significant adenoid hypertrophy.4 Chronically inflamed adenoids (chronic adenoiditis) may harbour bacterial biofilms (e.g. Haemophilus influenzae, Moraxella species, Streptococcus species), contributing to persistent rhinorrhoea, chronic rhinosinusitis, otitis media with effusion and obstructive sleep symptoms.4
Allergic rhinitis
Allergic rhinitis is the most common immunoglobulin E-mediated disease worldwide, with childhood onset in almost 50% of cases, often before 6 years of age.5 Prevalence in children ranges from 10 to 30% globally. It often coexists with asthma and eczema (the atopic triad), and can impair school performance and quality of life.6 Allergic rhinitis is a type 2 inflammatory disease; treatment aims to reduce inflammation and symptom burden.5
Other causes
Other causes of chronic or recurrent rhinorrhoea include anatomical anomalies (e.g. choanal atresia, septal deviation), an intranasal foreign body, rare neoplasms, immunodeficiency or cystic fibrosis. GPs should remain vigilant for red flags, discussed below, which may prompt further evaluation.
Clinical assessment
The duration and pattern of rhinorrhoea help guide diagnosis. An illness lasting seven to 10 days usually indicates a viral URTI, whereas acute bacterial sinusitis should be suspected if symptoms persist beyond 14 days or worsen after initial improvement. Chronic rhinosinusitis is defined by symptoms lasting 12 weeks or more, which may be continuous or intermittent, and either seasonal or perennial in pattern.
The characteristics of the nasal discharge also provide clues. Clear, watery discharge suggests allergy or viral infection, whereas purulent discharge is nonspecific and may occur with viral URTI or chronic rhinosinusitis; however, persistent unilateral purulence raises concern for an intranasal foreign body. Associated symptoms further refine the differential: nasal itching, sneezing and red or watery eyes point toward allergic rhinitis; mouth breathing, snoring, sleep disturbance and otitis media suggest adenoid hypertrophy; and nocturnal cough, facial pain or pressure, halitosis and fatigue may be present in both acute and chronic bacterial sinusitis.
The assessment of a child presenting with recurrent or chronic rhinorrhoea is summarised in Box 1.
Red flags
Red flag features warranting urgent assessment of a child with rhinorrhoea by an ENT surgeon, to exclude serious complications (such as orbital cellulitis, abscess, meningitis or intracranial collections) include the following:
- unilateral symptoms
- malodorous discharge
- epistaxis
- facial swelling or pain
- orbital signs or symptoms
- severe or prolonged fever
- acute severe headache
- lethargy
- neurological changes, including cranial nerve abnormalities.
Atopy and comorbidities
Asthma, eczema and a family history of allergy should be specifically asked about when taking a medical history for a child with chronic or recurrent rhinorrhoea, as these factors can identify children at higher risk of allergic rhinitis. Poor response to appropriate initial therapy, growth concerns and speech or hearing issues should also be noted, as they may prompt referral to an ENT specialist.
Examination
On anterior rhinoscopy, the appearance of the mucosa and turbinates provides important diagnostic clues. Pale, boggy mucosa with a purplish hue (reflecting venous sinusoid engorgement) is characteristic of allergic rhinitis, whereas erythematous, swollen mucosa is more suggestive of infection or vasomotor rhinitis.
Clinical examination should include observation of nasal airflow, evaluation of adenoidal facies and the presence of any mouth breathing. Otoscopy is important to assess for middle ear effusion. Inspection and palpation should also assess for the presence of lymphadenopathy or facial swelling.
Further investigations
Further investigations, undertaken by an ENT surgeon, may include nasal endoscopy to directly visualise the adenoids and middle meatus. Imaging studies such as CT or MRI should be reserved for cases where medical therapy has failed or when red-flag features are present.
Management principles
The management of chronic or recurrent rhinorrhoea is best approached stepwise, starting with low-risk measures that improve comfort and mucociliary clearance, followed by targeted therapy based on the most likely diagnosis. Antibiotics and imaging should be reserved for children with features suggesting bacterial infection or complications, with clear safety-net advice and follow up if symptoms persist or worsen.
Case vignettes illustrating the assessment and management of recurrent or chronic rhinorrhoea due to a range of underlying causes are presented in Box 2.
Symptomatic relief
Intranasal saline is a cornerstone therapy for rhinorrhoea of most aetiologies, and may be in the form of nasal drops, sprays or irrigation several times daily. For younger children, bulb suction after saline drops can assist. Saline is effective in reducing discharge and improving comfort, and may also reduce the need for additional pharmacotherapy.7
Analgesia or antipyretics (paracetamol or ibuprofen) should be offered as needed. Unless specifically prescribed by an ENT surgeon, over-the-counter topical nasal decongestants should be avoided in children younger than 6 years of age.
Pharmacotherapy
Allergic rhinitis
Nonsedating, second-generation oral antihistamines can be used for immediate symptom relief in cases of chronic or recurrent rhinorrhoea caused by allergic rhinitis. Intranasal corticosteroids, such as fluticasone or mometasone, are first-line therapy for moderate to severe allergic rhinitis in children aged 2 years or older, with evidence of reduced inflammation and improved nasal patency. The best technique for administering an intranasal spray is detailed in Box 3, and involves tilting the head forward and aiming the nozzle slightly away from the midline.8 In moderate to severe disease, particularly in adolescents, combination therapy with an intranasal antihistamine plus an intranasal corticosteroid may be considered. All pharmacotherapy should be used in conjunction with allergen avoidance of common allergens (e.g. pet dander, pollen, house dust mite, mould), if the child has been identified as being sensitised to these allergens on skin or serum immunoglobulin E testing.
Referral for immunotherapy should be considered if symptoms persist despite three to six months of optimal medical therapy.5,7
Acute bacterial sinusitis
Most presentations of acute rhinosinusitis are viral in nature, and about 80% resolve spontaneously or improve within two weeks. Antibiotics may be considered when there is purulent nasal discharge persisting for more than 14 days, sinus tenderness, fever or clinical deterioration after initial improvement.
The first-line antibiotic of choice is amoxicillin (15 mg/kg per dose [to a maximum of 500 mg] three times daily for 10 days [reassess at five days]). In cases of recent amoxicillin exposure or treatment failure, amoxicillin/clavulanic acid (22.5 mg/kg per dose [to a maximum of 875 mg amoxicillin component] twice daily for five days) should be used instead.9 Culture-directed therapy is recommended if infection persists despite medical treatment.10
Chronic rhinosinusitis
Initial medical management of chronic rhinosinusitis involves intranasal saline and intranasal corticosteroids, both administered for a minimum of six weeks, together with allergen minimisation.9 Additionally, an extended antibiotic course (typically 20 days or longer) may be considered, targeting common pathogens.2,3,10
Surgical options
Adenoidectomy is recommended when adenoidal hypertrophy contributes to chronic rhinosinusitis or nasal obstruction, and symptoms are severe or persist despite appropriate conservative and medical management. Studies estimate that about 70% of children with chronic rhinosinusitis have symptom resolution following the procedure.11 For children older than 6 to 7 years of age who have persistent disease after adenoidectomy or who demonstrate significant sinus pathology, functional endoscopic sinus surgery may be considered, with success rates for the former procedure between 82 and 100% in appropriately selected patients.3,4,11
Safety netting and parental advice
Parents should be reassured that most viral URTIs resolve within seven to 10 days, with longer duration often resulting from overlapping infections, and that purulent nasal discharge alone does not necessarily indicate bacterial infection. Routine antibiotics are not required for viral or allergic cases of rhinorrhoea and may cause adverse effects; they should be reserved for suspected bacterial disease.
Families should be educated about the red flags associated with rhinorrhoea (as listed above), which require prompt re-evaluation. Daily nasal care should be encouraged, including intranasal saline (e.g. sprays or irrigation), as should adequate hydration and rest, environmental and allergen control and maintaining a smoke-free home.
Expectations should be set that if symptoms improve within two to three weeks after a trial of saline and (where appropriate) intranasal corticosteroids, these measures should be continued under observation of the child’s GP; if there is no improvement or symptoms worsen, follow up with their GP is necessary.
When to refer
For children with chronic or recurrent rhinorrhoea, referral to an ENT specialist is recommended when red-flag features are present. Referral is also indicated for persistent chronic rhinosinusitis (symptoms for longer than 12 weeks) despite optimal medical therapy; suspected anatomical abnormalities; nasal polyps or masses; sleep-disordered breathing or growth concerns related to adenoid hypertrophy; and cases with associated recurrent otitis media, hearing loss or language delay.
Additionally, children with refractory allergic rhinitis despite at least three to six months of optimal intranasal corticosteroid therapy and allergen avoidance should be considered for immunotherapy or review by an allergist. Further information for GPs on referral for allergic rhinitis can be found in the Australasian Society of Clinical Immunology and Allergy’s Allergic Rhinitis Clinical Update and The Royal Children’s Hospital Melbourne’s guidance on primary care liaison for allergic rhinitis and hay fever.
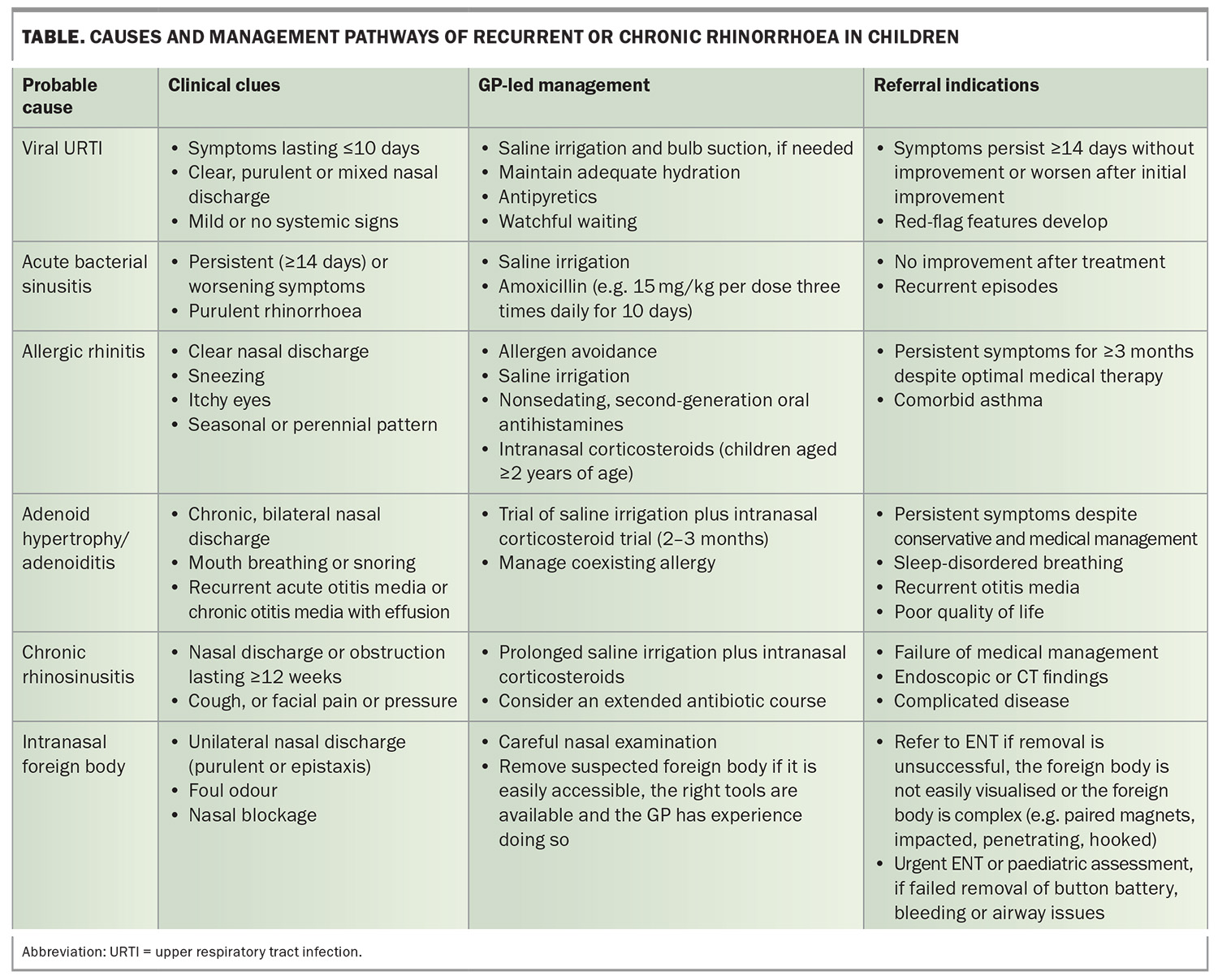
The causes, initial management and referral indications for recurrent or chronic rhinorrhoea in children are summarised in the Table.
Conclusion
Most cases of paediatric chronic or recurrent rhinorrhoea are due to overlapping viral URTIs and resolve within 14 days, whereas persistent nasal discharge beyond 12 weeks suggests possible chronic rhinosinusitis. In young children, adenoid hypertrophy is a common driver (often associated with bacterial biofilms), and allergic rhinitis is prevalent and may coexist.
Management should begin with intranasal saline sprays or irrigation, nasal hygiene, allergen avoidance where needed and appropriate pharmacotherapy, including antihistamines and intranasal corticosteroids, with antibiotics used only when clearly indicated. Adenoidectomy remains the key surgical treatment for adenoid-driven chronic rhinosinusitis in younger children, whereas functional endoscopic sinus surgery is an effective option for older children who fail medical therapy.
Clinicians should recognise and act on red-flag features, and follow an evidence-based, stepwise approach to reduce unnecessary antibiotic use and reinforce referral thresholds. MT
COMPETING INTERESTS: Professor Vijayasekaran has received payment or honoraria for his participation on a Smith & Nephew coblation course, and has previously been the president of the Australian and New Zealand Society of Paediatric Otorhinolaryngology.
References
1. Leung AK, Hon KL, Chu WC. Acute bacterial sinusitis in children: an updated review. Drugs Context 2020; 9: 2020-9-3.
2. Bulfamante AM, Saibene AM, Felisati G, Rosso C, Pipolo C. Adenoidal disease and chronic rhinosinusitis in children—is there a link? J Clin Med 2019; 8: 1528.
3. Brietzke SE, Shin JJ, Choi S, et al. Clinical consensus statement: pediatric chronic rhinosinusitis. Otolaryngol Head Neck Surg 2014; 151: 542-553.
4. Ahmad Z, Krüger K, Lautermann J, et al. Adenoid hypertrophy - diagnosis and treatment: the new S2k guideline. HNO 2023; 71: 67-72.
5. Miraglia del Giudice M, Marseglia GL, Peroni DG, et al. Allergic rhinitis management: a Delphi Consensus promoted by the Italian Society of Pediatric Allergy and Immunology (SIAIP). Ital J Pediatr 2024; 50: 254.
6. Cohen B. Allergic rhinitis. Pediatr Rev 2023; 44: 537-550.
7. Sapsford T, Dawson B, Anderson D. Approach to paediatric nasal obstruction. Aust J Gen Pract 2022; 51: 787-791.
8. National Asthma Council Australia. Intranasal spray technique. Melbourne: National Asthma Council Australia; 2014. Available online at: https://www.nationalasthma.org.au/living-with-asthma/resources/health-professionals/information-paper/intranasal-spray-technique (accessed January 2026).
9. The Royal Children’s Hospital Melbourne (RCH). Clinical practice guideline: rhinitis and rhinosinusitis. Melbourne: RCH; 2025. Available online at: https://www.rch.org.au/Persistent_nasal_discharge_rhinosinusitis/.aspx (accessed January 2026).
10. Chandy Z, Ference E, Lee JT. Clinical guidelines on chronic rhinosinusitis in children. Curr Allergy Asthma Rep 2019; 19: 14.
11. Tuncer U, Aydogan B, Soylu L, Simsek M, Akcali C, Kucukcan A. Chronic rhinosinusitis and adenoid hypertrophy in children. Am J Otolaryngol 2004; 25: 5-10.
Further reading
Australasian Society of Clinical Immunology and Allergy (ASCIA). Allergic rhinitis clinical update. Sydney: ASCIA; 2024. Available online at: https://www.allergy.org.au/hp/papers/allergic-rhinitis-clinical-update (accessed January 2026).
The Royal Children’s Hospital Melbourne (RCH). Primary care liaison: allergic rhinitis hay fever. Melbourne: RCH; 2014. Available online at: https://www.rch.org.au/primary-care-liaison/prereferral_guidelines/Allergic_rhinitis_hay_fever/ (accessed January 2026).
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.