Recurrent pregnancy loss: a GP’s guide to evidence-based care

With recurrent pregnancy loss now defined as two or more pregnancy losses, up to 5% of women are affected. Using an evidence-based approach, GPs are key in offering timely support, arranging investigations and initiating appropriate referral for ongoing management.
- Recurrent pregnancy loss (RPL) is defined as two or more pregnancy losses before 20 weeks’ gestation and affects up to 5% of women.
- The causes of RPL are diverse and include genetic, anatomical, endocrine, immunological, environmental and male factors.
- Aneuploidy is the most common cause of early miscarriage, whereas antiphospholipid syndrome is the strongest known acquired risk factor for RPL.
- Many couples with RPL will have no identifiable cause, but structured multidisciplinary care can improve outcomes and patient experience.
- Thorough evaluation of both partners, with attention to modifiable lifestyle and systemic factors, is essential in managing RPL.
Recurrent pregnancy loss (RPL) is defined as two or more pregnancy losses before 20 weeks’ gestation with the same partner, regardless of whether the losses are consecutive. Studies have shown a minimal difference in diagnostic yield when investigations are initiated after two losses versus three. This updated definition expands the eligibility for evaluation and recognises the significant psychological toll of repeated pregnancy loss. A sensitive, structured approach to management can make a meaningful difference in a couple’s experience and support their path to parenthood.
This article is based on the Australasian Recurrent Pregnancy Loss Clinical Management Guideline 2024 published by the Australasian Certificate of Reproductive Endocrinology and Infertility Consensus Expert Panel on Trial Evidence group.1,2 GPs play a crucial role, often as a trusted first point of contact for couples. This article focuses on practical steps for GPs to initiate the investigation and management of RPL, and on helping to identify clear indications for referral to a fertility specialist.
What causes recurrent pregnancy loss?
RPL affects up to 5% of women.3 There are several causes and associated factors with RPL, which can be broken down into the following groups.
Chromosomal factors
Aneuploidy (an abnormal number of chromosomes) in the embryo is the most common cause of first-trimester miscarriage and is strongly associated with increasing maternal age. Furthermore, chromosomal rearrangement in the parent, such as balanced translocations (i.e. where one segment of a chromosome breaks off and attaches to another with no overall gain or loss of genetic material), occurs in around one in 20 couples with RPL.4 These couples have a greater likelihood of creating chromosomally unbalanced embryos, leading to pregnancy loss (Box 1).
Anatomical factors
Structural uterine abnormalities, such as congenital Müllerian anomalies (e.g. unicornuate, bicornuate, septate uterus or uterus didelphys), certain types of fibroids (intramural and submucosal) and intrauterine adhesions (i.e. Asherman’s syndrome), may increase the risk of pregnancy loss. In contrast, endometrial polyps do not appear to increase the risk of RPL, although they may have a negative impact on implantation and reduce the likelihood of conception (Box 2).5
Endocrine factors
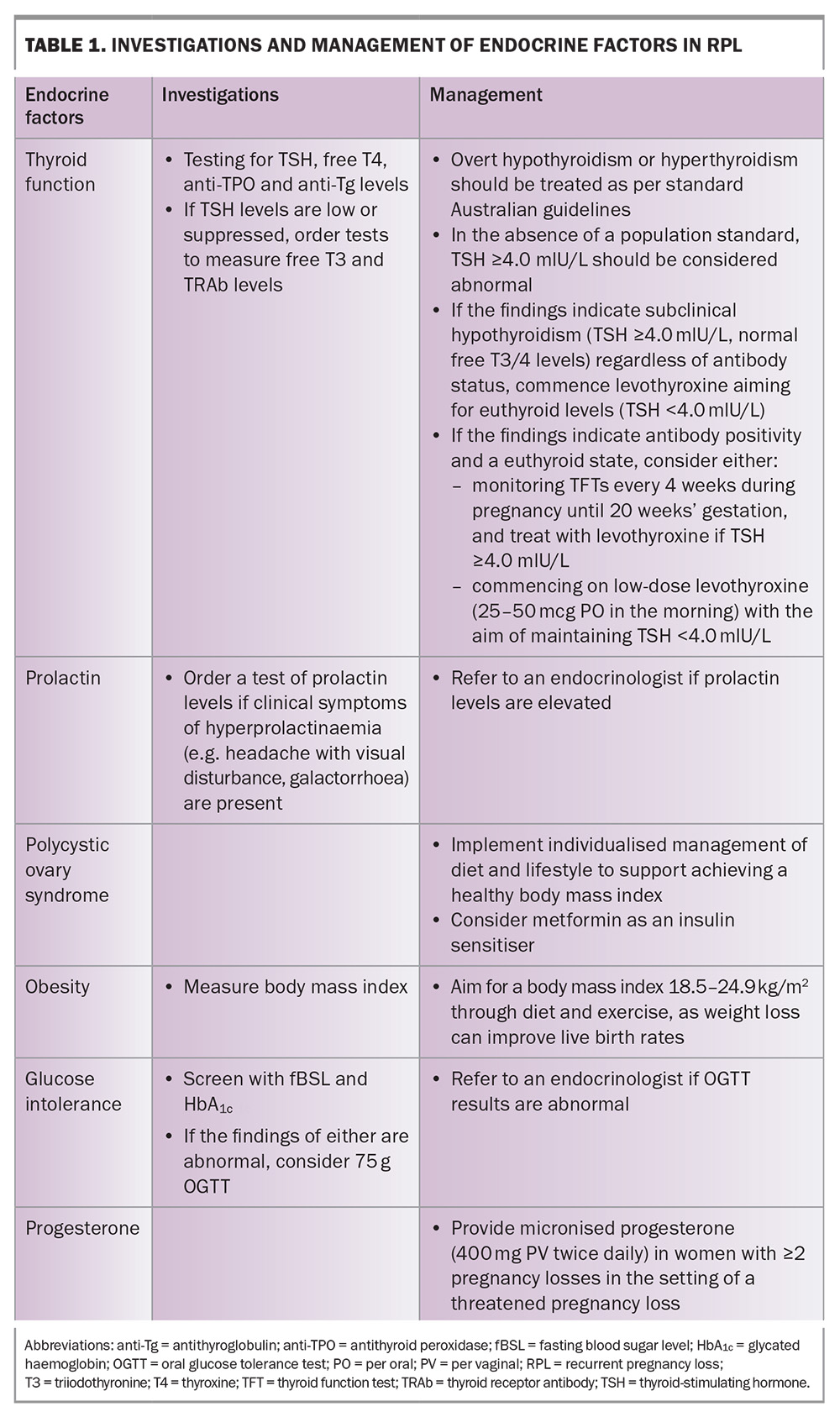
The key endocrine factors associated with RPL, along with their investigations and management approaches, are summarised in Table 1 and described below.
- Thyroid function: Overt hypothyroidism and hyperthyroidism are both associated with an increased risk of RPL and spontaneous pregnancy loss.6,7 The presence of thyroid antibodies, in the context of either normal or subclinical thyroid function, appears to be associated with RPL.8 However, management in this group remains contentious.
- Prolactin: It is unclear if high prolactin levels are associated with RPL. Nevertheless, if there is clinical suspicion of hyperprolactinaemia, levels should be checked, as treating this condition may improve the live birth rate.
- Polycystic ovary syndrome: Polycystic ovary syndrome is the most common endocrine disorder in women. It is difficult to study due to its heterogeneity and may be associated with an increased risk of spontaneous pregnancy loss.
- Obesity: Obesity is associated with an increased risk of RPL, as well as poor obstetric outcomes (e.g. increased risk of gestational diabetes, hypertensive disorders of pregnancy, preterm birth, delivery via Caesarean section, neonatal morbidity).9,10
- Glucose intolerance: Glucose intolerance is comprised of overt diabetes mellitus, impaired fasting glucose levels and impaired glucose tolerance. Evidence on its association with RPL is currently mixed and inconclusive.
- Progesterone: Progesterone supplementation may help reduce the rate of pregnancy loss in RPL. Evidence favours progesterone supplementation in women who have had three or more previous losses, and a threatened pregnancy loss (i.e. bleeding in early pregnancy).11
Thrombophilia
It is unclear whether inherited thrombophilias (such as Factor V Leiden, prothrombin gene mutation, protein C and S deficiency and antithrombin deficiency) are associated with RPL. As such, routine testing for these conditions is not recommended (Box 3).12
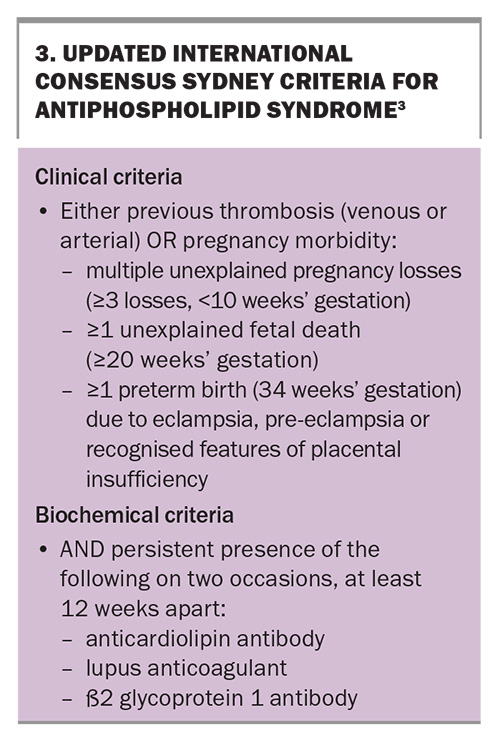
Conversely, acquired thrombophilia, namely antiphospholipid syndrome, and its associated antibodies are strongly associated with RPL and should be considered in the workup (Box 4).13 Although the methylenetetrahydrofolate reductase mutation is often grouped with thrombophilias, it is not classified as one and has no established link with RPL.
Autoimmune conditions
It is acknowledged that immune factors are associated with RPL. Currently, strong evidence is lacking, although research in this area continues to evolve. Therefore, it is recommended that autoimmune-related investigations occur only within a research setting (Box 5). Poorly controlled coeliac disease has been associated with RPL.14
Endometrial factors
Infective
Chronic endometritis may be more prevalent in women with RPL. If diagnosed, it can be easily treated with antibiotics, and some evidence suggests this may improve live birth rates.15 However, as diagnosis requires an endometrial biopsy, patients should be referred to a fertility specialist for further evaluation in suspected cases (Box 6).
Endometriosis
Endometriosis is an inflammatory condition that can affect egg quality and early pregnancy outcomes. Nationwide historical cohort study data from Danish national health registers have revealed a link to RPL, strengthened by the number of pregnancy losses.16 Currently, there are no identified treatments that have proven to be effective in reducing RPL within this population.
Lifestyle and environmental factors
Exposure to endocrine-disrupting chemicals (e.g. bisphenol A and phthalates) and heavy metals, high caffeine intake, cigarette smoking and alcohol consumption may be associated with an increased risk of spontaneous pregnancy loss (Box 7). There is no evidence to support routine serum or urine testing for heavy metal exposure.
It is acknowledged that a high level of psychological stress is associated with RPL. Positive outcomes (i.e. higher live birth rates) have been observed when couples have received formal clinical support for the first 12 weeks of pregnancy within multidisciplinary care settings.17,18
Male factors
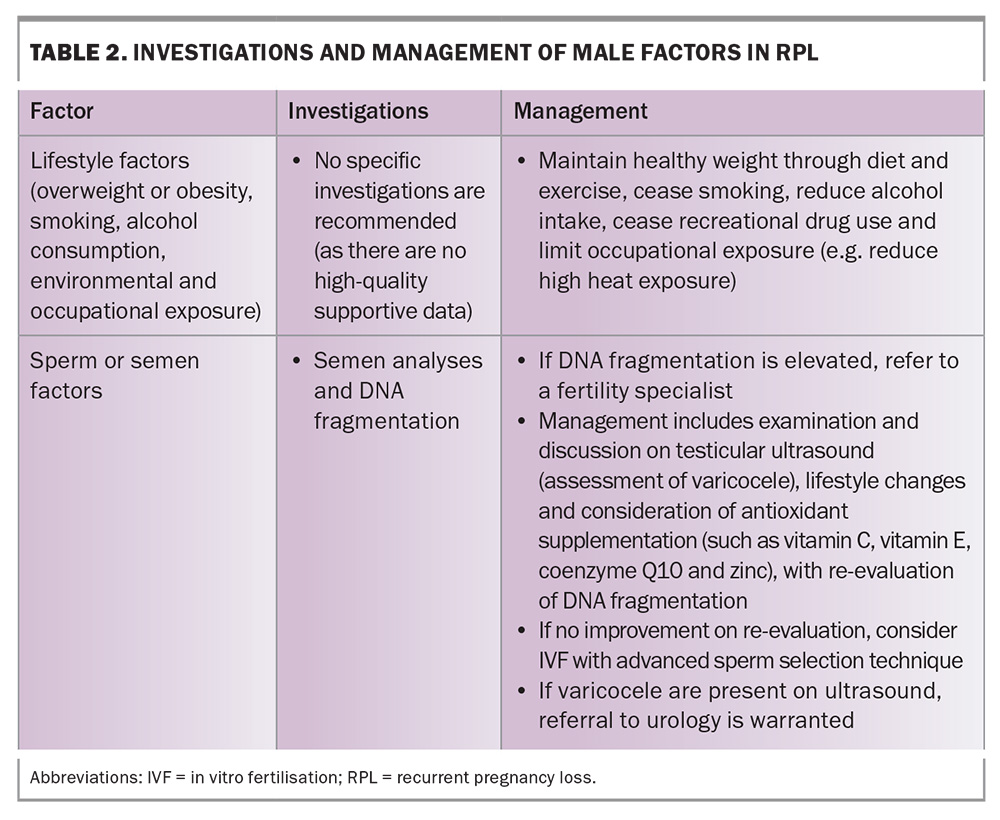
Excessive weight (overweight and obesity), smoking, alcohol consumption, and environmental and occupational exposures in men have all been associated with RPL (Table 2). It is important to take a thorough history of the male partner to identify and address these modifiable risk factors.
Damage to sperm DNA, which can occur during spermatogenesis or during transit through the reproductive tract, has been implicated in RPL. Elevated levels of sperm DNA fragmentation have been observed in affected couples, suggesting a potential contributing role.
Unexplained recurrent pregnancy loss
In up to 50 to 70% of couples with RPL, no specific underlying cause is identified.19 These couples may benefit from specialist referral for further evaluation, support and management.
Conclusion
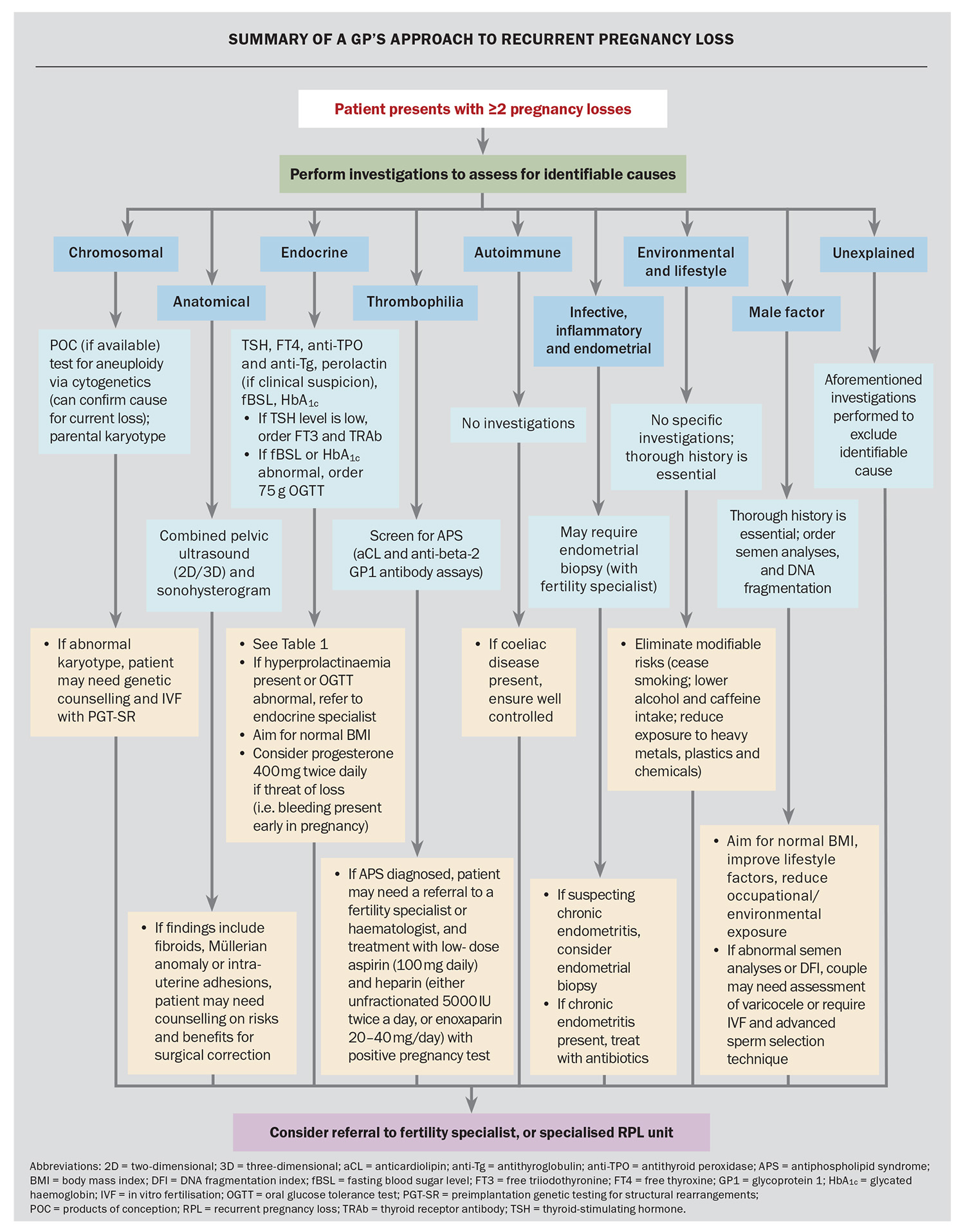
RPL can be multifactorial, complex and emotionally distressing for couples. As the first point of contact, GPs are uniquely positioned to offer early clinical assessment and emotional support. With a structured history and appropriate investigations, a potential cause can be identified in up to half of all cases, many of which are treatable. Referral to a fertility specialist is appropriate when no clear causes are found, or if specialist management is needed. Patient-friendly resources are now also available to help guide and support couples through this challenging time. 20 A summary of a GP’s approach to RPL is presented in the Flowchart. MT
COMPETING INTERESTS: None.
References
1. Suker A, Li Y, Robson D, Marren A; Australasian CREI (Certificate of Reproductive Endocrinology and Infertility) Consensus Expert Panel on Trial Evidence (ACCEPT) group. Australasian recurrent pregnancy loss clinical management guideline 2024 Part I. Aust N Z J Obstet Gynaecol 2024; 64: 432-444.
2. Suker A, Li Y, Robson D, Marren, A; Australasian CREI (Certificate of Reproductive Endocrinology and Infertility) Consensus Expert Panel on Trial Evidence (ACCEPT) group. Australasian recurrent pregnancy loss clinical management guideline 2024 Part II. Aust N Z J Obstet Gynaecol 2024; 64: 445-458.
3. Stirrat GM. Recurrent miscarriage I: definition and epidemiology. Lancet 1990; 336: 673-675.
4. De Braekeleer M, Dao TN. Cytogenetic studies in couples experiencing repeated pregnancy losses. Hum Reprod 1990; 5: 519-528.
5. Pérez-Medina T, Bajo-Arenas J, Salazar F, et al. Endometrial polyps and their implication in the pregnancy rates of patients undergoing intrauterine insemination: a prospective, randomized study. Hum Reprod 2005; 20: 1632-1635.
6. Stagnaro-Green A. Thyroid antibodies and miscarriage: where are we at a generation later? J Thyroid Res 2011; 2011: 841949.
7. Negro R, Stagnaro-Green A. Clinical aspects of hyperthyroidism, hypothyroidism, and thyroid screening in pregnancy. Endocr Pract 2014; 20: 597-607.
8. Thangaratinam S, Tan A, Knox E, et al. Association between thyroid autoantibodies and miscarriage and preterm birth: meta-analysis of evidence. BMJ 2011; 342: d2616.
9. Boots CE, Bernardi LA, Stephenson MD. Frequency of euploid miscarriage is increased in obese women with recurrent early pregnancy loss. Fertil Steril 2014; 102: 455-459.
10. Mukhtar F. A systematic review of the management of maternal obesity in pregnancy: antenatal management, outcomes, and long-term implications on maternal health. Cureus 2025; 17: e87258.
11. Coomarasamy A, Devall AJ, Cheed V, et al. A randomized trial of progesterone in women with bleeding in early pregnancy. N Engl J Med 2019; 380: 1815-1824.
12. Miyakis S, Lockshin MD, Atsumi T, et al. International consensus statement on an update of the classification criteria for definite antiphospholipid syndrome (APS). J Thromb Haemost 2006; 4: 295-306.
13. Sauer R, Roussev R, Jeyendran RS, Coulam CB. Prevalence of antiphospholipid antibodies among women experiencing unexplained infertility and recurrent implantation failure. Fertil Steril 2010; 93: 2441-2443.
14. Tersigni C, Castellani R, de Waure C, et al. Celiac disease and reproductive disorders: meta-analysis of epidemiologic associations and potential pathogenic mechanisms. Hum Reprod Update 2014; 20: 582-593.
15. McQueen DB, Bernardi LA, Stephenson MD. Chronic endometritis in women with recurrent early pregnancy loss and/or fetal demise. Fertil Steril 2014; 101: 1026-1030.
16. Boje AD, Egerup P, Westergaard D et al. Endometriosis is associated with pregnancy loss: a nationwide historical cohort study. Fertil Steril 2023; 119: 826-835.
17. Clifford K, Rai R, Regan L. Future pregnancy outcome in unexplained recurrent first trimester miscarriage. Hum Reprod 1997; 12: 387-389.
18. Liddell HS, Pattison NS, Zanderigo A. Recurrent miscarriage—outcome after supportive care in early pregnancy. Aust N Z J Obstet Gynaecol 1991; 31: 320-322.
19. Practice Committee of the American Society for Reproductive Medicine. Evaluation and treatment of recurrent pregnancy loss: a committee opinion. Fertil Steril 2012; 98: 1103-1111.
20. Suker A, Li Y, Marren A, Robson D; Australasian CREI (Certificate of Reproductive Endocrinology and Infertility) Consensus Expert Panel on Trial evidence (ACCEPT) group. Plain language summary of the ACCEPT guideline for the management of recurrent pregnancy loss, Aust N Z J Obstet Gynaecol 2025 Feb 12; e-pub (https://doi.org/10.1111/ajo.70000).
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.