The pregnant traveller

Travel during pregnancy carries additional risks for both the mother and fetus. Pretravel counselling on recommended vaccinations, mosquito avoidance, venous thromboembolism prevention and food safety is essential. With careful planning, most pregnant women can travel safely, although high-risk travel may require expert advice.
- Pregnancy is associated with some risks for both the mother and fetus, which can be compounded by travel.
- Risk assessment and counselling should be discussed with the pregnant woman, ideally before booking the trip.
- Risk-reduction strategies include destination-specific advice on required immunisations, mosquito-borne disease prevention and venous thromboembolism prophylaxis.
- Airline restrictions and travel insurance cover should be checked in advance, as both may have limitations associated with pregnancy.
- Travellers should consider the availability of medical support at the proposed destination, ideally before booking the trip, in case medical assistance is required.
- For higher-risk travel, consultation with both an obstetrician and a dedicated travel medicine clinic is recommended.
Pregnancy may not be the ideal time to travel because of practical considerations such as physical comfort and variable access to healthcare. Both the mother and fetus are exposed to increased risks during travel, in addition to risks associated with the specific destination. However, for clinicians providing advice to pregnant women who plan to travel, this article provides an overview of preventive strategies to reduce these risks. The safest period to travel is generally considered to be in the second trimester (14 to 28 weeks’ gestation) when complications are least likely and before the growing fetus restricts mobility.
General pretravel advice
In Australia, many women travel during pregnancy but may not always seek pretravel advice.1 This is despite the presence of both obstetric and travel-related issues that may put their trip at risk.1-3 It is therefore important that clinicians discuss risks and benefits with their pregnant patients and provide tailored preventive advice (Box 1).
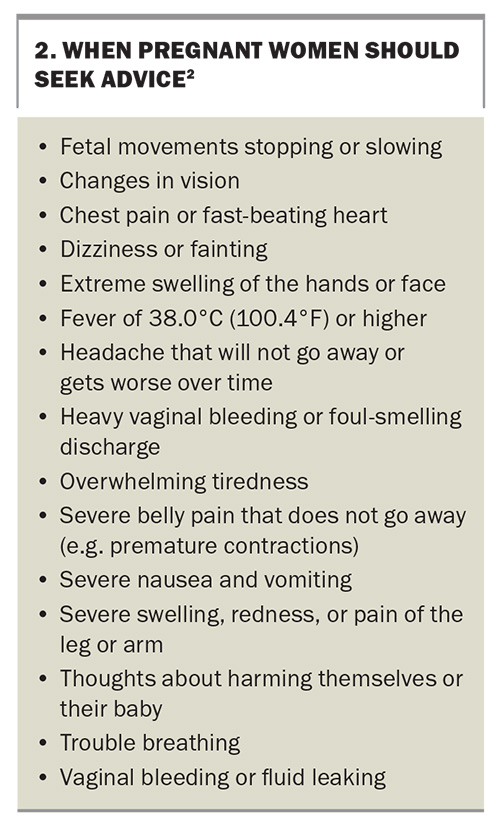
Even routine pregnancies have associated risks, so it is important to consider the availability of medical support at the proposed destination, ideally prior to booking the trip. Pregnant women should also be advised on when to seek medical advice while travelling (Box 2).2 Clinicians can also provide guidance on managing common travel-related problems such as nausea, back pain and leg swelling.
Contraindications to travel during pregnancy are listed in Box 3.2 Airline restrictions generally apply from 36 weeks for singleton pregnancies for flights of less than four hours, earlier for longer flights and from 32 weeks for multiple pregnancies. A doctor’s letter may also be required, and individual airline policies should be consulted. Travel insurance should specifically cover pregnancy, with the policy wording checked to ensure adequate cover for complications, childbirth and neonatal care.
Vaccinations
Vaccinations recommended in pregnancy include:
- influenza (any time during pregnancy)
- pertussis (optimal between 20 and 32 weeks’ gestation)
- respiratory syncytial virus (Abrysvo is the only currently approved brand for use in pregnant women) between 28 and 36 weeks’ gestation.4
COVID-19 vaccination is recommended as a primary dose for unvaccinated pregnant women at any stage of pregnancy.4 N95 masks and hygiene measures can reduce exposure to aerosol-borne disease.
Inactivated bacterial or viral vaccines are not routinely recommended but are considered relatively safe if the pregnant traveller is at high risk. Hepatitis A vaccination is generally considered to be safe for nonimmune pregnant women, as is typhoid Vi vaccination for higher risk trips.
Live viral vaccines are generally contraindicated, although there is little evidence of harm if inadvertently given. The exception to this is the yellow fever vaccine, which is a precaution rather than an absolute contraindication and may be given if the traveller will be at significant risk of exposure and following a discussion of risks and benefits as well as patient consent.2,4
Ideally, women considering pregnancy should have their serology checked and be offered relevant live vaccines before becoming pregnant. Cases of vaccine-preventable childhood diseases, such as measles, are significantly increasing worldwide, including in Australia. The Australian Immunisation Handbook provides an excellent summary of recommended vaccinations for women who are pregnant or breastfeeding (see: https://immunisationhandbook.health.gov.au/contents/vaccination-for-special-risk-groups/vaccination-for-women-who-are-planning-pregnancy-pregnant-or-breastfeeding).
Mosquito-borne diseases
Malaria
Travel during pregnancy to areas where malaria is prevalent is generally discouraged because of the significantly higher risks of complications for both mother and fetus. Malaria infection and antimalarial treatments can result in both fetal harm and pregnancy loss.
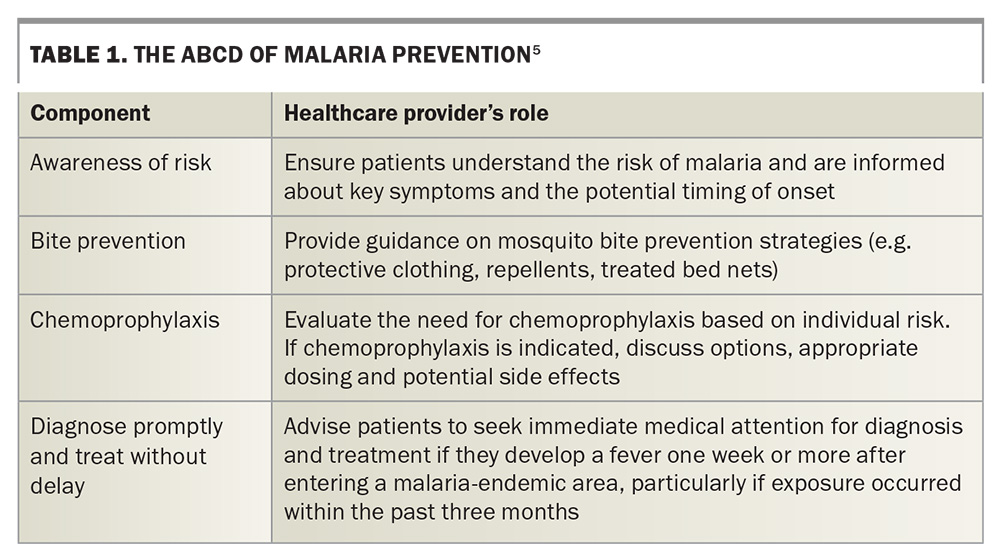
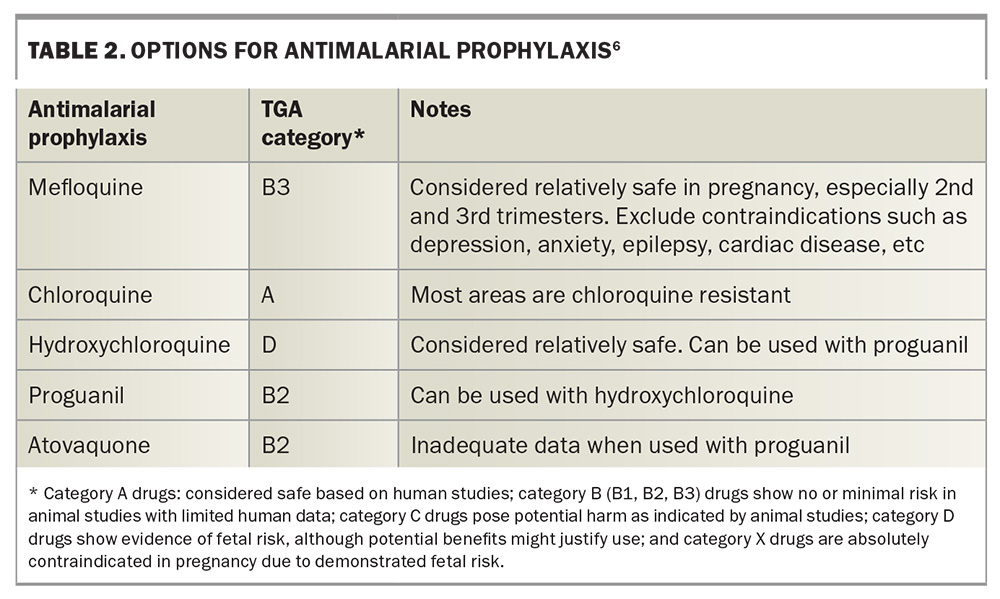
It is important to discuss with the traveller strategies to minimise mosquito bites, including the ‘ABCD’ approach (Table 1) and the Australasian College of Tropic Medicine guidelines on malaria prevention.5 Antimalarial prophylaxis, as described below, may be indicated where benefits outweigh the risks, noting that no regimen provides complete protection (Table 2).6
- Mefloquine, preferably taken after the first trimester, is generally considered the prophylactic medication of choice, with counselling on the contraindications and risk of neuropsychiatric side effects such as mood disorders, hyperarousal, psychosis and seizures.
- Hydroxychloroquine plus proguanil – this is considered safe in pregnancy but there are few chloroquine-sensitive areas.
- Atovaquone plus proguanil – there are inadequate data on this combination for use in pregnancy.
- Chloroquine is generally considered safe; however, its use is limited as there are few chloroquine-sensitive areas and a lack of availability in Australia. Hydroxychloroquine is an acceptable substitute.
- Doxycycline is contraindicated because of the significant adverse risk to fetal bone formation.
- Primaquine and tafenoquine are contraindicated because of the unknown risk of fetal G6PD deficiency.5
Zika and other arbovirus infections
Zika virus infection can cause microcephaly and other significant birth defects. Travel to outbreak and high-risk areas is therefore best avoided from two months before conception, and to delay conception for two to three months after leaving the area.
Other arbovirus infections of concern include yellow fever (in tropical South America and sub-Saharan Africa), Japanese encephalitis (in Asia and recently in Australia), dengue fever, which is increasing worldwide and is especially common across Asia, with an incidence of about one in 200 travellers per month. There is currently insufficient information to make any recommendation on the use of the dengue vaccine in pregnant travellers. A similar lack of evidence exists for chikungunya and any associated vaccines.
Travellers to areas at risk should be given appropriate information on insect-avoidance strategies, including physical barriers and repellents.7
Food- and water-borne diseases
Travellers’ diarrhoea is common and more likely in areas where food and water supplies may be contaminated. Hepatitis E is a particular risk in pregnancy and is more common in areas with poor sanitation. Routine preventive strategies include ‘boil it, cook it, bottle it or peel it’ and good hand hygiene before eating.6 Foods to avoid during pregnancy include liver, which is high in vitamin A; undercooked meat, which may transmit toxoplasmosis; and unpasteurised dairy food, which may be contaminated with listeriosis.8 Although symptoms are generally self-limiting, treatment includes intake of an oral rehydration solution and avoidance of irritant foods. If symptoms significantly compromise a person’s function, azithromycin is generally considered safe to use in pregnancy. It covers many of the more common bacterial infection strains seen in travellers, including Escherichia coli, Salmonella, Shigella and Campylobacter.
For women needing frequent access to toilets while travelling, apps such as the Toilet Finder may be helpful.9 Pregnant women should also avoid iodine-based water treatment because of the risk of fetal goitre and avoid category D medications, including oral thrush treatments such as fluconazole.
Venous thromboembolism
Pregnancy is a well-recognised risk factor for venous thromboembolism with up to a 10-fold increase in risk compared to that in nonpregnant women,8 which may continue for weeks postpartum. Travel for four to eight hours or more doubles the risk regardless of mode (air, train, bus or car). Additional risk factors, such as obesity, thrombophilia from Factor V Leiden and other genetic causes, past or family history, recent surgery and varicose veins increase the risk even further.10 Preventive strategies include aisle seating for easier access for mobilisation, regular leg exercises and maintenance of good hydration. There is evidence for the use of below-knee graduated compression stockings and, with relevant specialist advice, low-molecular-weight heparin during and for a few days after a flight or long trips on land transport.3 There are several excellent risk assessment tools to assess risk and stratify management.11,12
Flight factors
Pregnant women should wear seat belts low around the pelvis and throughout the flight. Radiation exposure from occasional flights is less than annual background exposure.7 There is no evidence linking occasional flights to pregnancy complications or fetal malformations.8 Most healthy pregnant women and their fetuses are able to compensate for the reduced cabin oxygen partial pressure.8 However, the low humidity can contribute to dehydration, highlighting the need to ensure adequate fluid intake.
Environmental health risks
Several environmental factors may affect a pregnant woman and their fetus. Air pollution is associated with exacerbation of maternal respiratory disease and may restrict fetal growth.2 Exposure to wildfire smoke or local burn offs can also have adverse effects and so the use of a N95 mask is recommended.2 Pregnant women are more prone to extreme heat and should ensure access to air-conditioned accommodation and adequate hydration. There are inadequate data on high altitude travel in pregnancy. Short-term travel to elevations of 2500 metres appears to pose minimal risk in uncomplicated pregnancies, but longer stays at elevations above 3500 metres are not recommended, especially if this precludes access to urgent medical care.13 Pregnant travellers are generally advised to avoid high-risk activities such as skiing (increased risk of physical injury) or scuba diving (increased risk of decompression effects on the fetus).
Medications
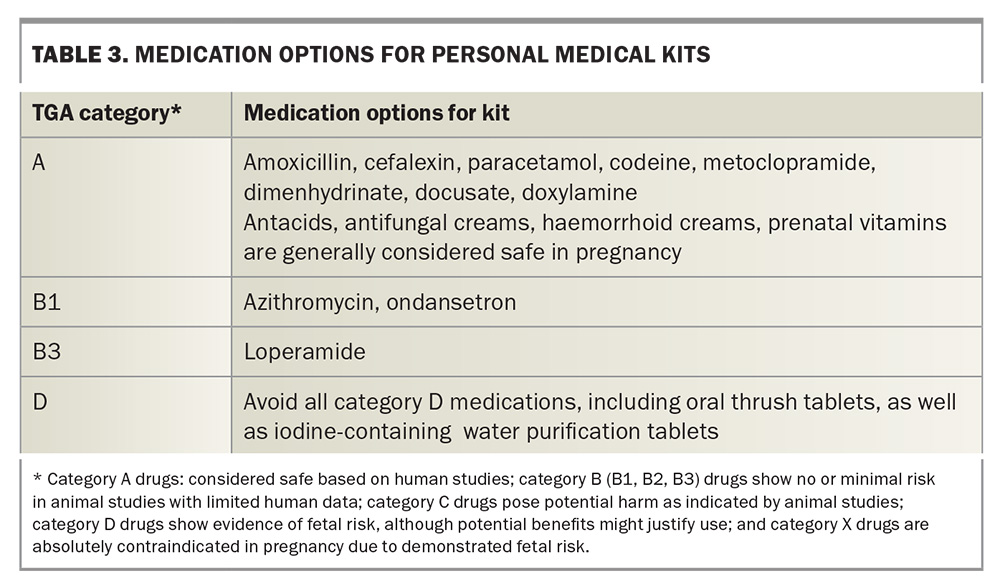
Travellers should carry their own medications, rather than purchasing them overseas to avoid counterfeit medications. A personal medical kit is recommended containing basic dressings and medications that may be required if medical care or pharmacies are hard to access. Antacids, antifungal creams, haemorrhoid creams and prenatal vitamins are generally considered safe in pregnancy (Table 3). Emergency antibiotics may be appropriate for urinary tract infections or moderate to severe travellers’ diarrhoea. Antinausea and analgesic medications are often needed. Their appropriate use should be discussed and written information provided for the traveller to take with them.7,14 Information about the use of medications in pregnancy can be accessed from the TGA website.6
Post-travel time to conception
For women planning a pregnancy, conception should be delayed for two to three months after returning from high-risk areas. Infections and their treatments, such as those for malaria, may result in fetal harm or pregnancy loss. The risk of congenital Zika virus syndrome is higher if infection occurs in the first trimester; this risk can be reduced by delaying conception for two to three months in women, and for six months in men.
Conclusion
With appropriate pretravel advice and planning, most trips in pregnancy can be made safely. It is important for GPs to identify and discuss pregnancy- and travel-related issues with the patient and to refer them to an obstetrician or a dedicated travel medicine clinic for higher-risk trips. A balanced, individualised approach offers pregnant travellers the best chance of a safe and enjoyable journey. MT
COMPETING INTERESTS: Dr Cohen has received financial support for provision of and attendance at educational events from Sanofi Pasteur, CSL Seqirus and Biocelect.
References
1. Chu SHS, Krishnaswamy S, Cole S, et al. Travel patterns and advice-seeking behaviour of pregnant women in the Australian context: a multicentre cross-sectional analysis. Aust N Z J Obstet Gynaecol 2022; 62: 688-694.
2. Centers for Disease Control and Prevention (CDC).Pregnant travelers. In: CDC Yellow Book [Internet].Atlanta: CDC. Available online at: https://www.cdc.gov/yellow-book/hcp/family-travel/pregnant-travelers.html (accessed September 2025).
3. Fernando M, Giles ML, Krishnaswamy S, et al. The pregnant traveller: an overview of general travel advice. Aust N Z J Obstet Gynaecol 2023; 63: 638-642.
4. Australian Government Department of Health and Aged Care. Vaccination for women who are planning pregnancy, pregnant or breastfeeding. In: Australian Immunisation Handbook: Canberra: Australian Government. Available online at: https://immunisationhandbook.health.gov.au/contents/vaccination-for-special-risk-groups/vaccination-for-women-who-are-planning-pregnancy-pregnant-or-breastfeeding (accessed September 2025).
5. McGuiness S, Lau C. ACTM malaria prevention guidelines [Internet]. Brisbane: Australasian College of Tropical Medicine. Available online at: https://www.tropmed.org/malaria-prevention-guidelines/ (accessed September 2025).
6. Australian Government Department of Health, Disability and Ageing. The Therapeutics Goods Administration. Prescribing medicines in pregnancy database. Available online at: https://www.tga.gov.au/products/medicines/find-information-about-medicine/prescribing-medicines-pregnancy-database (accessed September 2025).
7. Cohen J. The Traveller’s Pocket Medical Guide. 13th ed. Melbourne: Travel Clinics Australia; 2024. Available as ‘The Travel Clinic App’ on Google Play and the App Store.
8. Jasper B, Aiken C. International travel during pregnancy: a review of current literature and guidelines. Obstet Gynaecol Reprod Med 2024; 34: 338-343.
9. Toilet Finder. Toilet Finder app [Internet]. Google Play. Available online at: https://play.google.com/store/apps/details?id=com.bto.toilet&hl=en_AU (accessed September 2025).
10. Cannegieter SC, Doggen CJM, van Houwelingen HC, et al. Travel-related venous thrombosis: Results from a large population-based case control study (MEGA Study). PLoS Med 2006; 3: e307.
11. Choy KR, Emmett S, Wong A. Venous thromboembolism prophylaxis in pregnancy: are we adequately identifying and managing risks? Aust N Z J Obstet Gynaecol 2022; 62: 915-920.
12. Clinical Excellence Commission (CEC). VTE prevention: Risk Assessment and Prophylaxis. Sydney: CEC. Available online at: https://www.cec.health.nsw.gov.au/keep-patients-safe/medication-safety/vte-prevention/risk-assessment-and-prophylaxis (accessed September 2025).
13. Shoreland Travax Library. Pregnant Travelers [Internet]. Madison (WI): Shoreland; 2021 Nov.
14. Mills D. Travelling Well. 21st ed. Brisbane: Dr Deborah Mills; 2025.
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.