Persistent and chronic hiccups – when trivial becomes a conundrum

Hiccups are typically benign and self-limiting; however, persistent or chronic cases, although rare, can significantly impair a patient’s quality of life. Understanding the pathophysiology and causes of chronic hiccups can improve diagnosis and management.
- The majority of hiccups are benign and self-limiting, typically resolving within 48 hours without specific intervention. However, persistent hiccups can significantly impact quality of life.
- The causes of persistent and chronic hiccups are diverse and can be categorised as central, peripheral, drug-related and iatrogenic. Gastro-oesophageal reflux disease is the most common identifiable aetiology.
- A structured diagnostic approach is essential for hiccups lasting more than 48 hours and should include a thorough history, physical examination and targeted investigations to identify treatable underlying conditions.
- Treatment should be directed at an underlying cause where identified. In idiopathic cases of persistent and chronic hiccups, empirical therapies such as proton pump inhibitors, baclofen, gabapentin and metoclopramide are frequently used.
- Refractory cases may require combination pharmacotherapy, and severe, refractory cases may require interventional treatments such as phrenic nerve blockade or vagal nerve stimulation.
Hiccups, or singultus, can be considered an almost universal human experience. For the vast majority of people, hiccups are a temporary inconvenience that resolve spontaneously and are therefore easily dismissed as trivial. However, a small number of individuals have the misfortune of experiencing chronic or intractable hiccups. For these people, prolonged hiccups interfere with their ability to eat, sleep and engage in social interactions, resulting in malnutrition, isolation and a deterioration in their quality of life.
Abrupt diaphragmatic and intercostal muscular myoclonus is responsible for the sudden entry of air into the lungs, inducing vocal cord closure and causing the characteristic ‘hic’ sound of hiccups.1 The term singultus itself is derived from singult, a Latin word aptly describing ‘the act of catching one’s breath whilst sobbing’.2 The problem of intractable hiccups has been documented in historical records. According to the Guinness World Records, the longest recorded case of hiccups spanned almost 70 years, afflicting Charles Osborne, a farmer in the USA. He reportedly sustained an intracranial injury during an attempt to lift an oversized pig. Osborne experienced up to 40 involuntary diaphragmatic spasms per minute and is estimated to have hiccupped 430 million times, although, interestingly, his hiccups spontaneously resolved one year before his death in 1991.3
Hiccups can be classified based on their duration. Although there is no clear consensus on what constitutes chronic or intractable hiccups, most definitions describe temporary hiccups as lasting less than 48 hours. Persistent hiccups last between 48 hours and one month, and chronic or intractable hiccups last longer than one month and are likely attributable to an underlying disease process. Further investigation is often required for hiccups lasting over 48 hours.
Treatment should be directed at the underlying pathology; however, management of idiopathic chronic hiccups can be challenging due to a lack of robust evidence. This has given rise to some alternative and unconventional treatments, some of which are examined in this article. Although chronic hiccups are uncommon, it is likely that a patient with this problem will be encountered at some point in primary care. Given the GP’s role as the first point of contact in the community, it is important to recognise and navigate the diagnostic and management challenges associated with chronic and persistent hiccups.
Pathophysiology
The hiccup reflex arc comprises an afferent limb arising from the vagal, sympathetic and phrenic nerves from T6 to T12, which transmits sensory information to a central processing area in the midbrain and brainstem. This central component involves the medulla oblongata, periaqueductal grey, subthalamic nuclei, reticular formation, hypothalamus and cervical cord segments C3 to C6. Signals are then conveyed to the efferent limb, consisting of the phrenic nerve and accessory nerves supplying the diaphragm and intercostal muscles, respectively.4
Several neurotransmitters appear to be involved in the mediation of the hiccup reflex arc, including serotonin, histamine, dopamine, acetylcholine and gamma-aminobutyric acid.5 A hiccup occurs following sudden contraction of the diaphragm and intercostal muscles, resulting in abrupt entry of air into the lungs and subsequent laryngeal closure.
It is commonly accepted that self-resolving hiccups are caused by rapid gastric distension and irritation. However, people with chronic hiccups are more likely to have a structural or functional disturbance of the reflex arc described above. Any lesion affecting this neurological reflex arc may be implicated in the pathogenesis of hiccups. Given the complexity and limited understanding of these neural pathways, precise lesion localisation is difficult, and attempts to terminate the pathological reflex with targeted treatments can be challenging.
Causes
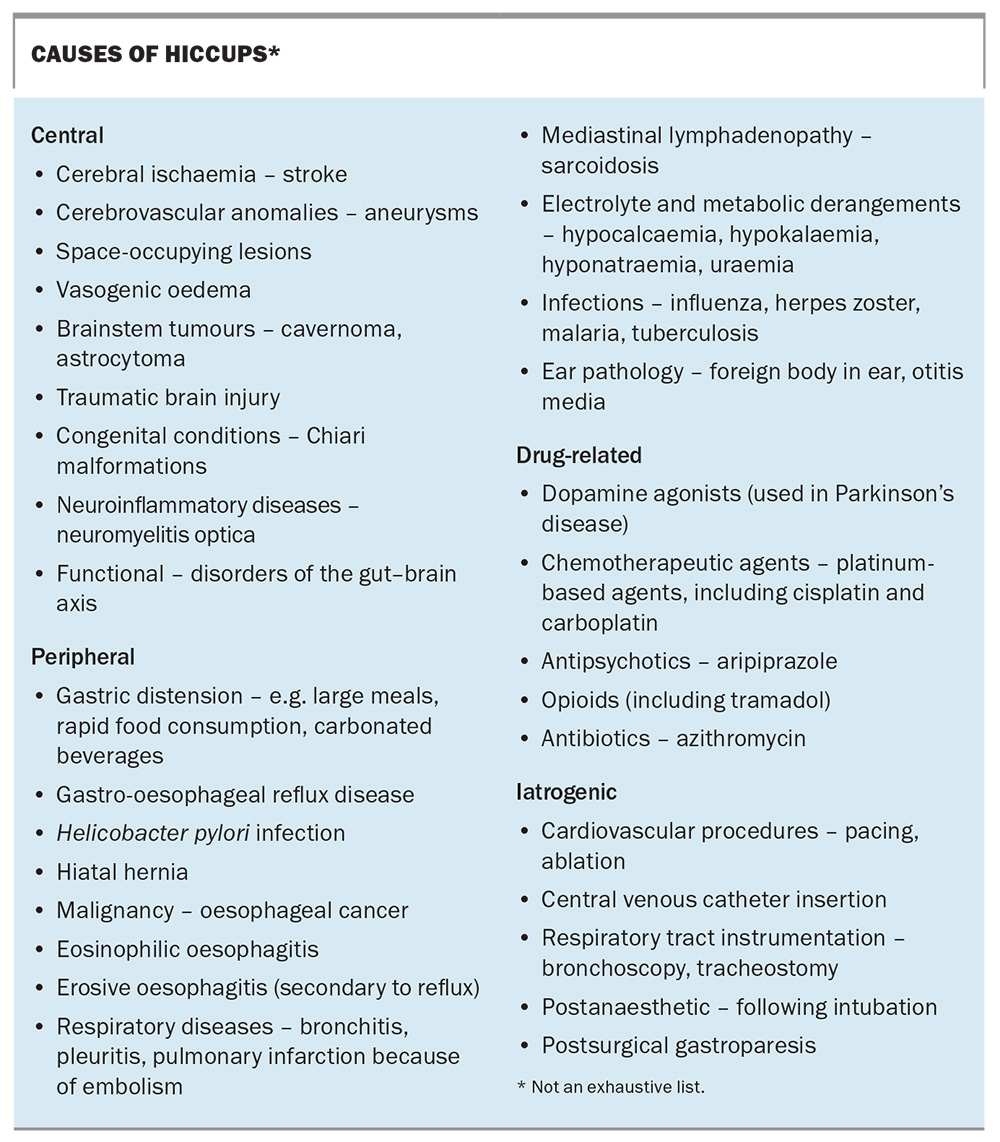
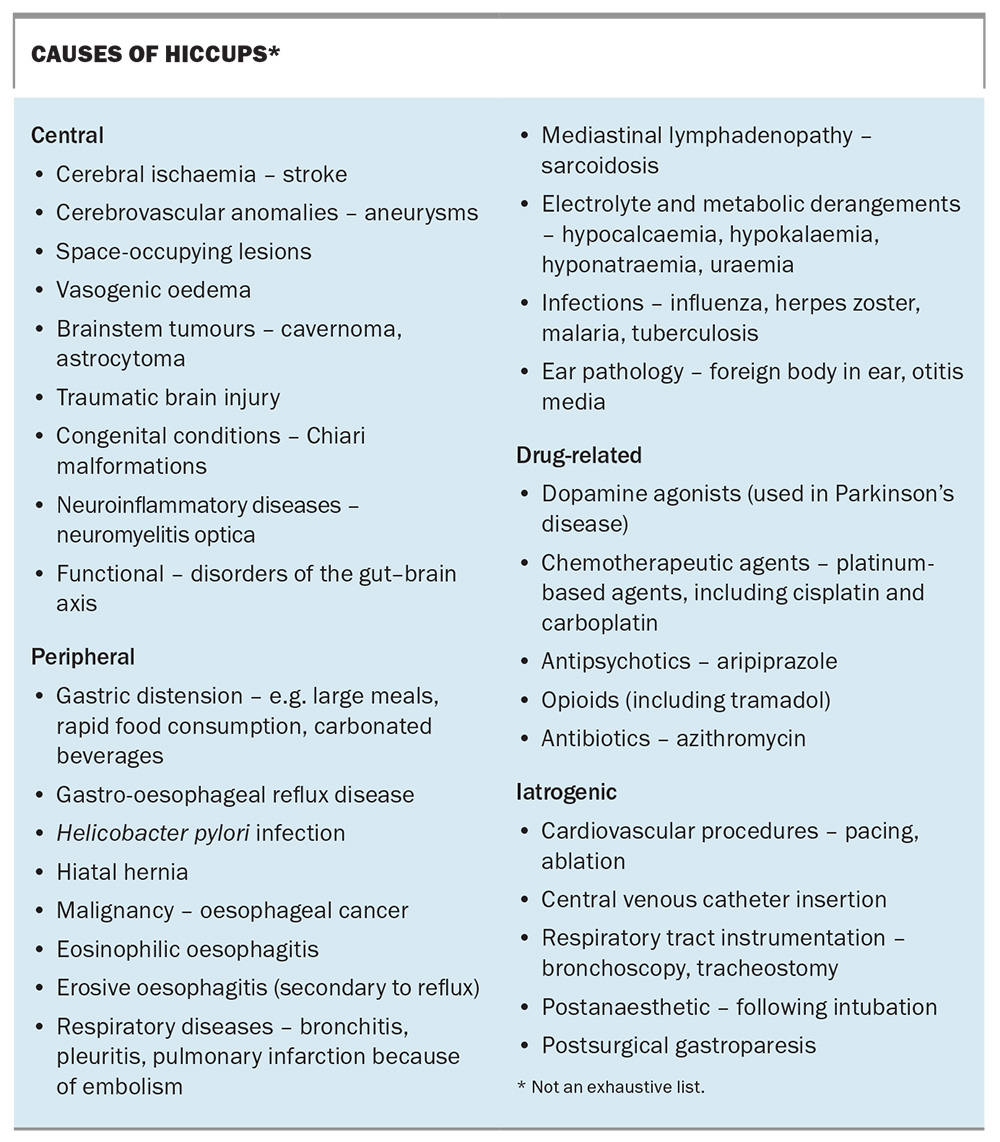
There are many known aetiologies of hiccups, and it is not helpful to simply list them all. They can be more usefully categorised into central, peripheral, drug-related and iatrogenic causes (Box).
Any structural abnormality of the central nervous system – including space-occupying lesions, traumatic brain injury, congenital malformations and neuro-inflammatory diseases – can cause chronic hiccups. Brainstem tumours, such as cavernomas and astrocytomas, have been implicated in the onset of hiccups, with symptoms not recurring following surgical resection.6
Peripheral causes of hiccups generally involve afferent pathways of the reflex arc. Hiccups are often attributed to a problem with the gastrointestinal tract. Acute hiccups can result from gastric distension following a large meal, rapid consumption of food or drinking carbonated beverages. Eating spicy foods, drinking alcohol, smoking or sudden changes in meal temperature may also precipitate hiccups.1 Older studies have demonstrated an association between underlying gastro-oesophageal reflux disease, regarded as the most common cause of chronic hiccups.7Helicobacter pylori infection has also been implicated, with eradication therapy reported to improve symptoms.1
Structural and luminal abnormalities of the gastrointestinal tract, including a large hiatal hernia, oesophageal malignancy, and erosive or eosinophilic oesophagitis, are other recognised peripheral causes of chronic hiccups, as are several respiratory conditions.8,9 Electrolyte and metabolic derangements are easily overlooked, and include hypocalcaemia, hypokalaemia, hyponatraemia and uraemia, all of which are relevant in the investigation of chronic hiccups.
Hiccups may also be drug-related or iatrogenic. Although hiccups may represent a nonmotor symptom of Parkinson’s disease, dopamine agonists can precipitate hiccups because of their affinity for dopamine D3 receptors involved in the hiccup reflex arc. Conversely, dopamine receptor antagonists such as metoclopramide and chlorpromazine are often used in the treatment of hiccups in people without Parkinson’s disease.10 Hiccups may occur as a side effect of chemotherapy, particularly platinum-based agents such as cisplatin and carboplatin.11 Other medications (e.g. antipsychotics, opioids [including tramadol], some antibiotics) have been reported to cause hiccups, although this is uncommon.12-15
Iatrogenic causes are mainly related to instrumentation (including bronchoscopy and tracheostomy) and cardiovascular procedures (including ablation and pacing).16-18 Postoperative hiccups may occur secondary to gastric distension and possibly as an element of postsurgical gastroparesis.4 Almost every organ system can be implicated in chronic hiccups (Box), with causes ranging from exceedingly rare case-report associations to conditions frequently encountered in everyday practice.
Hiccups versus belching
Hiccups and belching are both common upper aerodigestive phenomena, and it can be difficult to distinguish one from the other. However, they arise from distinct mechanisms and require different diagnostic and management approaches.
Belching, or eructation, refers to the audible expulsion of air from the oesophagus or stomach through the mouth and may be gastric or supragastric in origin. Gastric belching occurs when air escapes from the stomach into the oesophagus following transient lower oesophageal sphincter relaxation and is involuntary and reflexive.
In contrast, supragastric belching is not reflexive and does not occur during sleep. Supragastric belching is defined by the Rome IV criteria as a functional disorder in which air is suctioned into the oesophagus and rapidly expelled without reaching the stomach, and is considered behavioural. Supragastric belching tends to be irregular and is frequently associated with psychosocial stressors, learned behavioural patterns or conditions such as anxiety, obsessive compulsive disorder and bulimia nervosa.19 Both 24-hour pH monitoring and oesophageal impedance studies can be used to distinguish supragastric from gastric belching.
People with supragastric belching usually have no other symptoms other than dyspepsia. Features such as dysphagia, abdominal pain, regurgitation or weight loss are not typically associated with supragastric belching and should prompt further diagnostic evaluation.
Hiccups, by contrast, are generally rhythmic and persistent, and are often resistant to voluntary control. Differentiating hiccups from belching is clinically important because management differs: hiccups may respond to pharmacological or interventional therapies, whereas supragastric belching is more likely to benefit from cognitive behavioural therapy or speech therapy aimed at behavioural retraining.20 Nevertheless, both conditions may be functional and reflect underlying dysregulation of the gut–brain axis, with hiccups involving dysfunctional neural circuits and supragastric belching involving altered cortical and behavioural responses to visceral stimuli.
Unlike belching, hiccups are not defined in the Rome IV criteria for functional gastrointestinal disorders. A functional cause of hiccups should only be diagnosed after exclusion of organic aetiologies, and management should focus on symptom control. However, there are no published data on the proportion of cases that have a functional aetiology, and it is likely that investigations identify an underlying cause. Psychogenic hiccups are an even rarer clinical entity and are not within the scope of this article.
Diagnosis and investigation
Hiccups are frequently encountered in general practice. For the vast majority of cases, they do not persist beyond 48 hours and do not require specific treatment or investigation. These episodes are usually precipitated by a simple inciting factor, such as aerophagia caused by drinking carbonated beverages or rapid eating, consumption of spicy foods or drinking alcohol. The time course and trigger are often readily identified on history taking.
If hiccups persist beyond 48 hours, there is no clear inciting event, or both, further evaluation is warranted. A comprehensive medical and psychiatric history can help narrow the range of potential underlying aetiologies. Patients should also be asked about alcohol intake, recreational drug use and smoking history, as well as about any recent surgery or procedures that may suggest an iatrogenic cause. A detailed review of current and recently ceased medications is also essential.
Physical examination is important in assessing possible gastrointestinal, cardio-respiratory or neurological causes and should include inspection of the external auditory canals for the presence of a foreign body or infection. In cases of persistent and chronic hiccups, basic investigations are appropriate, including blood tests to assess for electrolyte derangements and renal function, as well as a chest x-ray to evaluate for pulmonary pathology. As gastro-oesophageal reflux disease is a common aetiology underlying persistent and chronic hiccups, enquiry about the severity of their reflux symptoms is important. In selected patients, a urea breath test may be considered to assess for H. pylori infection.
Some patients may benefit from referral to a gastroenterologist for endoscopic assessment to exclude intraluminal aetiologies, including erosive or eosinophilic oesophagitis, large hiatal hernia or malignancy. Where an oesophageal motility disorder or belching disorder is suspected, oesophageal manometry and 24-hour pH monitoring may be appropriate. A central cause of hiccups should always be suspected if neurological symptoms are present or abnormalities are detected on neurological examination, and such cases warrant central nervous system imaging.
Management of persistent and chronic hiccups should be directed at the underlying cause, highlighting the importance of a thorough diagnostic workup. Symptomatic treatment should be considered only when no clear underlying cause is identified.
Treatment
Most hiccups are self-resolving and not concerning. Management of persistent and chronic hiccups, however, can be challenging, especially when symptoms persist despite treatment of the underlying cause or when no clear aetiology is identified. Management options can be broadly categorised into nonpharmacological, pharmacological and interventional approaches. Adjuncts and alternative treatments have also been described. It is important to recognise that the evidence base for many of these treatments is limited, consisting largely of case reports and small case series.
Nonpharmacological management
Simple nonpharmacological measures can be attempted for hiccups that persist beyond 48 hours. These manoeuvres are low risk and can be performed in the consultation room or at home. Examples include sustained breath-holding for up to 10 seconds, a Valsalva manoeuvre, gargling or sipping cold water, gentle pressure on the eyeballs and carotid massage. The underlying mechanism behind some of these ‘quick fixes’ is interruption of the hiccup reflex arc through vagal stimulation. Other, less common anecdotal methods, such as consuming sugar granules or inducing a fright, have also been described. Although evidence for their efficacy is limited, these remedies are generally safe and may be tried as an initial step.
Behavioural counselling also plays a role in hiccup management. Education regarding smaller meal sizes, slower consumption of meals and avoidance of carbonated beverages and alcohol may help prevent symptoms. Anxiety and psychological stress can often exacerbate hiccups and should be addressed, where relevant.
Pharmacological management
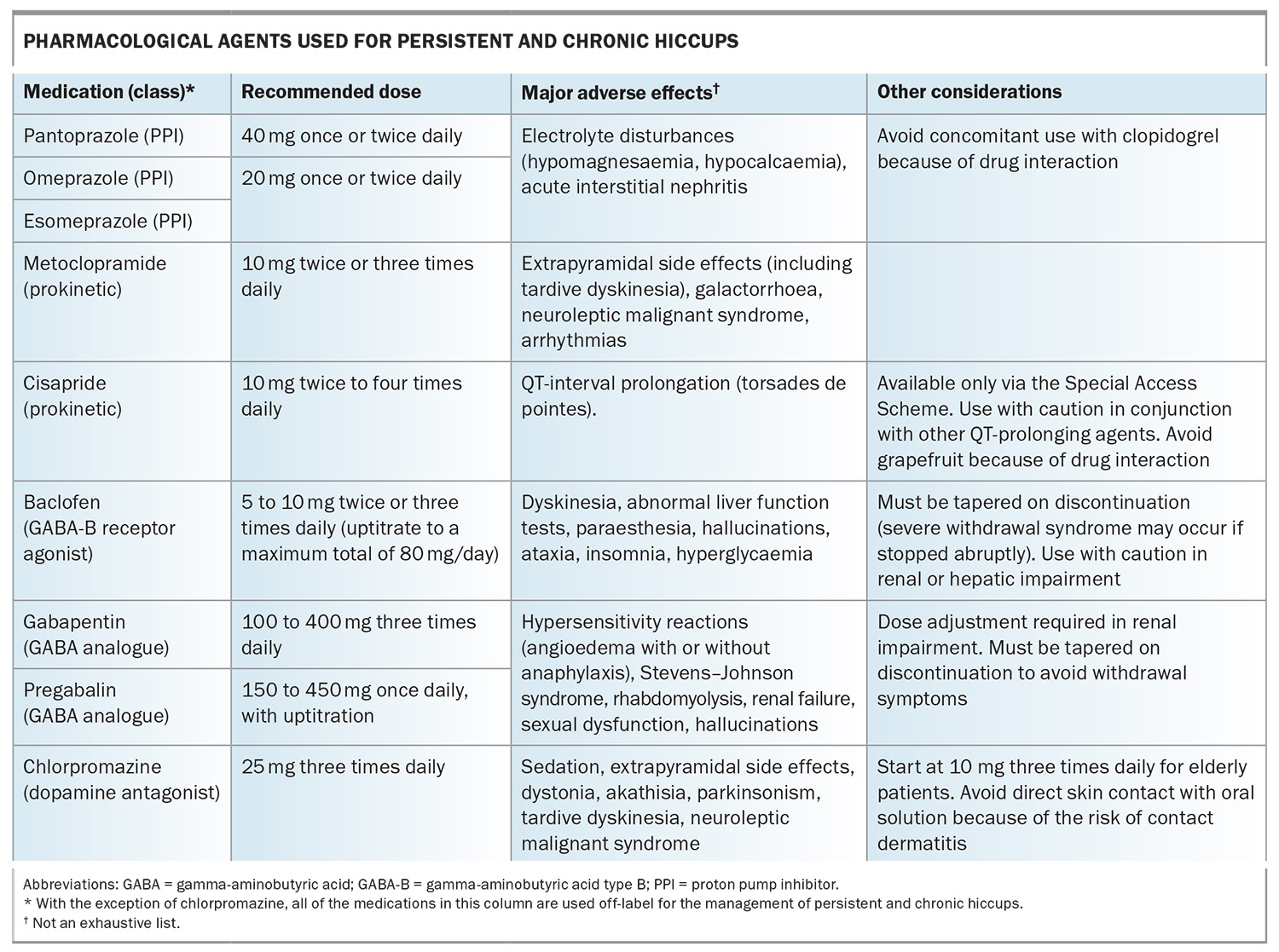
If no underlying cause is found for persistent hiccups and nonpharmacological management is unsuccessful, it is reasonable to commence empirical treatment (Table). Given the association between gastro-oesophageal reflux disease and hiccups, a trial of a proton pump inhibitor (PPI; e.g. pantoprazole, omeprazole, esomeprazole) is often considered first line. One study reported subjective improvement in hiccup severity in about two-thirds of patients treated with PPIs.21
Chlorpromazine, which has antagonistic effects on dopaminergic receptors, has historically been used in the treatment of persistent hiccups and is approved for this indication by the US Food and Drug Administration. Its approval was based on early case series published more than 70 years ago involving a total of 74 patients. The efficacy of chlorpromazine was believed to be from dopamine antagonism at the hypothalamus; however, later studies were less promising and reported limited efficacy. In Australia, chlorpromazine is indicated for the control of intractable hiccups.
Metoclopramide, a dopamine D2-receptor antagonist with weak serotonin 5-HT4-receptor agonist activity, has prokinetic effects on gastrointestinal motility. Randomised controlled trial data demonstrate symptomatic improvement in patients with intractable hiccups treated with metoclopramide. Severe adverse effects are rare, but the possibility of tardive dyskinesia should always be considered. Smaller case series have also reported symptomatic improvements, supporting the use of metoclopramide as a practical first-line treatment option for chronic hiccups.22 Other prokinetic agents, such as cisapride, have been used in combination with acid-suppressive therapy.23
Baclofen and gabapentin are increasingly used as first- or second-line pharmacological options in the management of persistent and chronic hiccups, and contemporary treatment approaches have largely centred on these agents. Baclofen is a gamma-aminobutyric acid type B receptor agonist and is thought to exert its effects through reduced dopaminergic release within the central nervous system and inhibition of the hiccup reflex arc. It is often used in the management of spasticity and, in some cases, refractory gastro-oesophageal reflux disease to reduce episodes of transient lower oesophageal sphincter relaxation. Early randomised controlled trial data, limited to stroke populations, demonstrated efficacy of baclofen in persistent hiccup treatment, with a mean time to symptom resolution of five days.24 Subsequent studies reported a similar benefit with baclofen monotherapy, with an average of six days to symptom resolution.25
Gabapentin, a gamma-aminobutyric acid analogue, acts on presynaptic voltage-gated calcium channels and modulates the excitability of diaphragmatic and inspiratory muscles. Although randomised controlled trial data assessing its effectiveness as monotherapy are lacking, case series have reported symptomatic improvement or complete resolution of hiccups in 81 of 83 patients.26 Treatment duration extended up to six months in some cases, with gradual dose reduction required to prevent withdrawal symptoms.27 Pregabalin, another gamma-aminobutyric acid analogue, has also been described as an alternative to gabapentin.28 Overall, gabapentin appears to have a slightly more favourable side-effect profile than baclofen and may be preferable in patients with multiple comorbidities.
In one case series, combined PPI (omeprazole) and prokinetic (cisapride) therapy resulted in improvement or resolution of hiccup symptoms in nine of 15 patients, with three patients responding after the addition of gabapentin or baclofen.29 Another study showed symptomatic improvement following stepwise addition of baclofen in eight of 20 patients who did not respond to PPI therapy alone.23,30 Other successful combinations described in the literature include baclofen with olanzapine or chlorpromazine.29 Despite this, evidence supporting combination therapy remains limited.
Previous exposure to medications for existing comorbidities may contribute to treatment failure, possibly because of drug tolerance, and should be considered when selecting pharmacological therapy.25
Interventional management
Interventional treatments to treat chronic hiccups should be reserved for cases refractory to medical management. Given the role of the phrenic nerve in hiccup pathophysiology, interventional approaches such as ultrasound-guided blockade or radiofrequency ablation of the phrenic nerve, as well as epidural blockade at C3 to C5, have been described.4,31 Reported adverse effects following nerve blockade include respiratory compromise and acute dyspnoea. Vagal nerve stimulation has also been used for protracted hiccups, particularly following stroke, in patients who have not responded to phrenic nerve blockade.4 This approach is likely only effective in patients with hiccups secondary to a central aetiology. Invasive interventions should be undertaken only in severe, medically refractory cases and require specialist input.
Adjuncts and alternative treatments
Acupuncture has been described as both an alternative treatment and as an adjunct in the management of hiccups. Evidence for its efficacy remains limited, and a systematic review identified a high risk of bias among the included studies, although some benefit when compared with other medications was reported.4,28 Robust randomised controlled trial evidence and further safety data are required to define acupuncture’s role in treatment algorithms.
Treatment algorithm
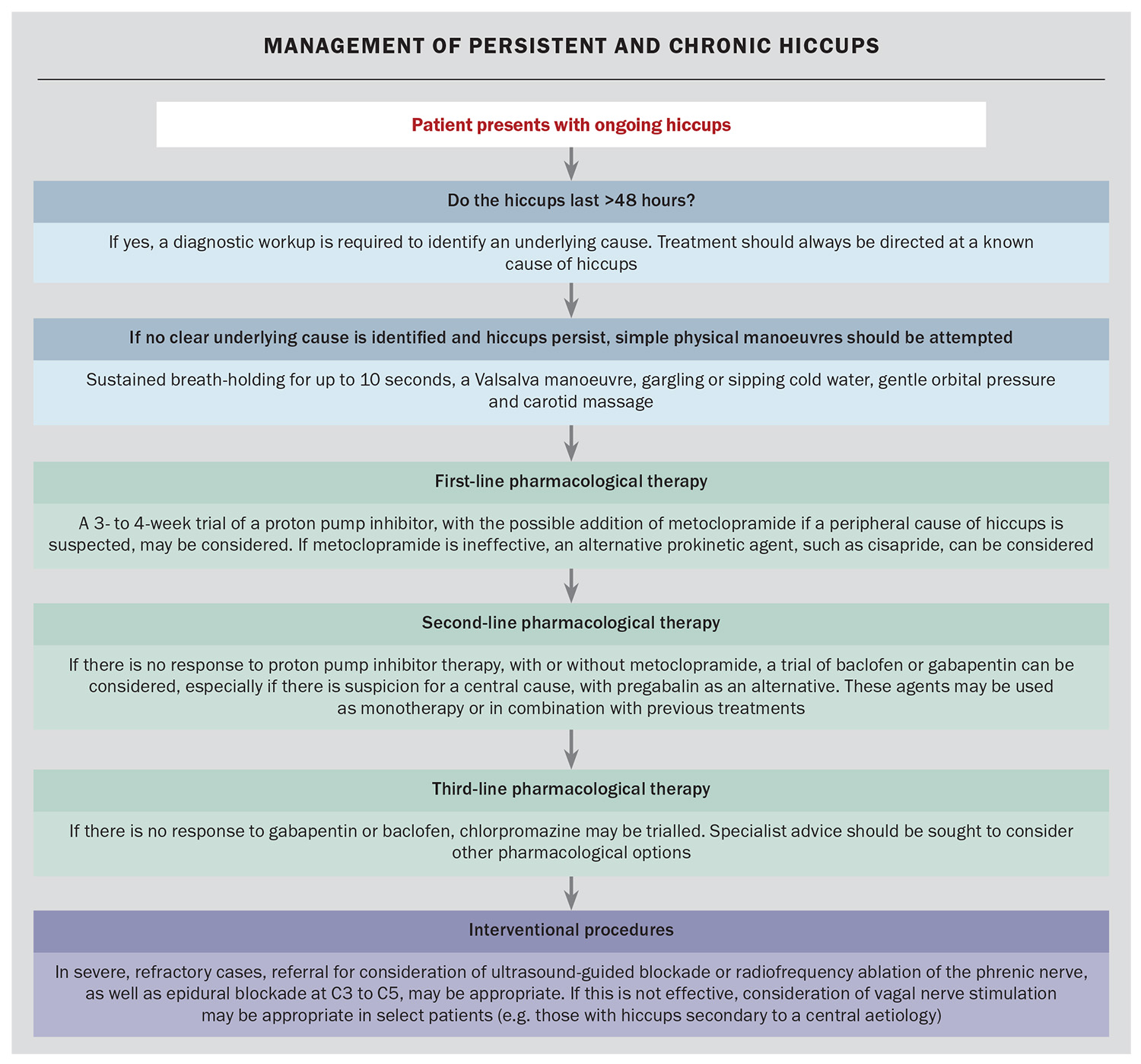
Based on current evidence, PPI therapy should be considered first-line treatment for persistent hiccups without an identified cause. Prokinetic agents, such as metoclopramide or cisapride, can also be cautiously trialled as first-line options when a peripheral cause is suspected. Baclofen or gabapentin should be considered second-line agents, especially if a central cause is suspected. Chlorpromazine may be considered if earlier treatments are unsuccessful.
Monotherapy is preferred where possible, given the limited evidence supporting combination therapy. However, combined PPI therapy with baclofen or gabapentin has demonstrated some efficacy and may be appropriate in selected patients. If hiccups remain refractory to medical management, interventional options may be considered with appropriate specialist consultation (Flowchart).
Conclusion
Although hiccups are often dismissed as a benign and transient phenomenon, persistent or chronic cases warrant careful clinical attention because of their potential to significantly impair a patient’s quality of life. Understanding the complex neurophysiology of the hiccup reflex arc, alongside a broad differential diagnosis, is essential for effective evaluation and management. For GPs and gastroenterologists alike, a structured approach – beginning with thorough history taking and targeted investigations – can help identify reversible causes.
Empirical treatment, particularly for idiopathic cases, should be evidence informed, with PPIs, baclofen and gabapentin emerging as key therapeutic agents. In refractory cases, multidisciplinary collaboration and specialist referral for interventional options may be appropriate. Ultimately, recognising that persistent and chronic hiccups are more than a trivial complaint can lead to meaningful improvements in patient outcomes. MT
COMPETING INTERESTS: None.
References
1. Chang FY, Lu CL. Hiccup: mystery, nature and treatment. J Neurogastroenterol Motil 2012; 18: 123-130.
2. Patel N, O’Brien K. Persistent singultus: addressing complexity with simplicity. ACG Case Rep J 2015; 2: 150-151.
3. Gormly KB. The curious case of Charles Osborne, who hiccupped for 68 years straight. Washington: Smithsonian Magazine 2022. Available online at: https://www.smithsonianmag.com/history/the-curious-case-of-charles-osborne-who-hiccuped-for-68-years-straight-180980232/ (accessed December 2025).
4. Reichenbach ZW, Piech GM, Malik Z. Chronic hiccups. Curr Treat Options Gastroenterol 2020; 18: 43-59.
5. Nausheen F, Mohsin H, Lakhan SE. Neurotransmitters in hiccups. Springerplus 2016; 5: 1357.
6. Eisenächer A, Spiske J. Persistent hiccups (singultus) as the presenting symptom of medullary cavernoma. Dtsch Arztebl Int 2011; 108: 822-826.
7. Pooran N, Lee D, Sideridis K. Protracted hiccups due to severe erosive esophagitis: a case series. J Clin Gastroenterol 2006; 40: 183-185.
8. Levy AN, Rahaman SM, Bonis PA, Javid G, Leung J. Hiccups as a presenting symptom of eosinophilic esophagitis. Case Rep Gastroenterol 2012; 6: 340-343.
9. Khorakiwala T, Arain R, Mulsow J, Walsh TN. Hiccups: an unrecognized symptom of esophageal cancer? Am J Gastroenterol 2008; 103: 801.
10. Miwa H, Kondo T. Hiccups in Parkinson’s disease: an overlooked non-motor symptom? Parkinsonism Relat Disord 2010; 16: 249-251.
11. Takahashi T, Hoshi E, Takagi M, Katsumata N, Kawahara M, Eguchi K. Multicenter, phase II, placebo-controlled, double-blind, randomized study of aprepitant in Japanese patients receiving high-dose cisplatin. Cancer Sci 2010; 101: 2455-2461.
12. Ray P, Zia Ul Haq M, Nizamie SH. Aripiprazole-induced hiccups: a case report. Gen Hosp Psychiatry 2009; 31: 382-384.
13. Jover F, Cuadrado JM, Merino J. Possible azithromycin-associated hiccups. J Clin Pharm Ther 2005; 30: 413-416.
14. McGrane IR, Shuman MD, McDonald RW. Donepezil-related intractable hiccups: a case report. Pharmacotherapy 2015; 35: e1-5.
15. Panchal R, Bhutt V, Anovadiya A, Purohut B, Dekhaiya F, Goswami N. Tramadol-induced hiccups: a report of two cases. Drug Saf Case Rep 2018; 5: 3.
16. Doshi H, Vaidyalingam R, Buchan K. Atrial pacing wires: an uncommon cause of postoperative hiccups. Br J Hosp Med (Lond) 2008; 69: 534.
17. Sacher F, Monahan KH, Thomas SP, et al. Phrenic nerve injury after atrial fibrillation catheter ablation: characterization and outcome in a multicenter study. J Am Coll Cardiol 2006; 47: 2498-2503.
18. Sav T. Hiccups, a rare complication arising from use of a central venous catheter. Hemodial Int 2010; 14: 337-338.
19. Bredenoord AJ. Management of belching, hiccups, and aerophagia. Clin Gastroenterol Hepatol 2013; 11: 6-12.
20. Sawada A, Fujiwara Y, Sifrim D. Belching in gastroesophageal reflux disease: literature review. J Clin Med 2020; 9: 3360.
21. Cabane J, Bizec JL, Derenne JP. A diseased esophagus is frequently the cause of chronic hiccup. A prospective study of 184 cases. Presse Med 2010; 39: e141-6.
22. Wang T, Wang D. Metoclopramide for patients with intractable hiccups: a multicentre, randomised, controlled pilot study. Intern Med J 2014; 44: 1205-1209.
23. Polito NB, Fellows SE. Pharmacologic interventions for intractable and persistent hiccups: a systematic review. J Emerg Med 2017; 53: 540-549.
24. Zhang C, Zhang R, Zhang S, Xu M. Baclofen for stroke patients with persistent hiccups: a randomized, double-blind, placebo-controlled trial. Trials 2014; 15: 295.
25. Kohse EK, Hollmann MW, Bardenheuer HJ, Kessler J. Chronic hiccups: an underestimated problem. Anesth Analg 2017; 125: 1169-1183.
26. Jatzko A, Stegmeier-Petroianu A, Petroianu GA. Alpha-2-delta ligands for singultus (hiccup) treatment: three case reports. J Pain Symptom Manage 2007; 33: 756-760.
27. Thompson DF, Brooks KG. Gabapentin therapy of hiccups. Ann Pharmacother 2013; 47: 897-903.
28. Choi TY, Lee MS, Ernst E. Acupuncture for cancer patients suffering from hiccups: a systematic review and meta-analysis. Complement Ther Med 2012; 20: 447-455.
29. Petroianu G, Hein G, Petroianu A, Bergler W, Rüfer R. Idiopathic chronic hiccup: combination therapy with cisapride, omeprazole, and baclofen. Clin Ther 1997; 19: 1031-1038.
30. Guelaud C, Similowski T, Bizec JL, Cabane J, Whitelaw WA, Derenne JP. Baclofen therapy for chronic hiccup. Eur Respir J 1995; 8: 235-237.
31. Zhang Y, Duan F, Ma W. Ultrasound-guided phrenic nerve block for intraoperative persistent hiccups: a case report. BMC Anesthesiol 2018; 18: 123.
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.