A patient with pruritic, blistering patches of acute onset

Test your diagnostic skills in our regular dermatology quiz. What is the cause of these erythematous-to-violaceous skin patches, which are pruritic and blistering?
Case presentation
A 39-year-old man is admitted to hospital for a planned coronary artery bypass graft. During his admission, he develops an acute flare of gout of his left big toe and commences treatment with allopurinol. Within 24 hours, he has several pruritic patches on his skin (Figures 1a to c) and two of these patches develop blisters.
The patient has an elevated body mass index and a history of inadequately controlled type 2 diabetes and hypertension. His regular medications include metformin and perindopril. In addition, he takes indomethacin occasionally for flares of gout. He is a lifelong nonsmoker and consumes about two standard drinks per week.
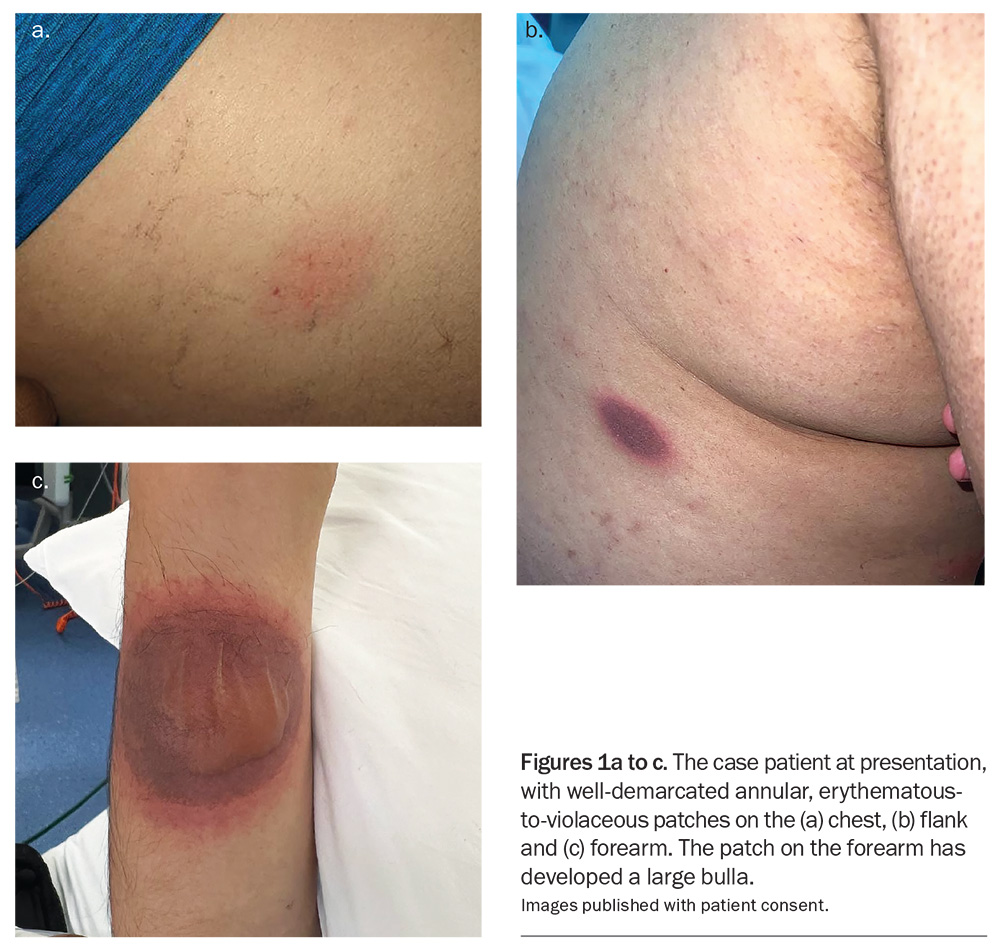
On examination, well-demarcated annular, erythematous-to-violaceous patches are observed on the patient’s forearm, chest, shoulder, flank, buttocks and the urethral meatus of the glans penis. The lesion on his arm has a large central bulla and the lesion on his penis is centrally erosive. There are no conjunctival or oral lesions. He is systemically well and afebrile.
Differential diagnoses
Conditions to consider among the differential diagnoses for a patient with an acute onset of erythematous patches and bullae include the following.
Erythema multiforme
Erythema multiforme most frequently occurs following a herpes simplex virus infection but may be caused by a drug (e.g. antibiotics, antiepileptics and NSAIDs). Lesions develop at the peripheries before spreading centrally. The distribution is usually symmetrical with a preference for extensor surfaces. Systemic symptoms such as malaise, arthralgia, myalgia and fever are common.1
For the case patient, the absence of typical target-like lesions or systemic symptoms made this diagnosis less likely.
Bullous pemphigoid
Bullous pemphigoid is an autoimmune subepidermal blistering disease that generally presents with erythematous, urticarial and/or eczematous plaques that are pruritic and develop into widespread tense bullae.2 It tends to occur in older patients and frequently affects the skinfolds. The condition is diagnosed by skin biopsy, which typically shows dermal oedema, subepidermal blistering and dermal infiltration of neutrophils and eosinophils. Direct immunofluorescence staining shows linear deposition of IgG and C3 along the basement membrane.2
Clinically, bullous pemphigoid is not the most likely diagnosis for the case patient, who is younger than the usual age group and whose lesions are not located in skinfolds. The condition has not been associated with allopurinol.3
Bullous insect bite reaction
Most patients with insect bite reactions present with groups of pruritic erythematous papules with blisters in exposed areas, such as on the arms and lower legs.4 The location can raise suspicion of the diagnosis, even if a patient may not remember being bitten. After sensitisation, consequent bites from the same insect result in progressively more severe and diffuse reactions as previous bites are reactivated.4 A history of recent travel, time spent outdoors and exposure to insects will help with the diagnosis.
For the case patient, this diagnosis was less likely because his lesions were not papules and not grouped in exposed areas.
Bullous impetigo
Bullous impetigo presents as intensely pruritic lesions that may begin as small vesicles before developing into large flaccid bullae. It is seen most frequently on the face or at a site of trauma. Systemic symptoms of malaise, fever and lymph-adenopathy are not uncommon.5
For the case patient, bullous impetigo was an important consideration because inadequately controlled type 2 diabetes is a risk factor for the condition.5 However, it is not the most likely diagnosis.
Fixed drug eruption
This is the correct diagnosis. A fixed drug eruption (FDE) is a delayed cutaneous hypersensitivity reaction that recurs at the same site each time an individual is re-exposed to an offending drug.6 The known causes include NSAIDs and antibiotics (such as penicillins, tetracyclines and sulfamethoxazole–trimethoprim) and, less frequently, allopurinol.
FDEs occur in all age groups without sex predilection and are far less common than exanthematous eruptions. One or more erythematous or violaceous patches or plaques, which are well-defined and typically round, develop within minutes or hours of exposure. These are usually asymptomatic but pain or itch may occur. Subsequent flares can be more severe, and the number or severity of patches or plaques may increase with each exposure. Any cutaneous surface may be affected but involvement of mucosa, such as the oral or anogenital mucosa, is generally minimal, and it is mostly restricted to mucocutaneous junctions.6 Patients often remain systemically well. Healing with postinflammatory hyperpigmentation is common.6
An FDE that covers a significant percentage of body surface area is referred to as a generalised bullous FDE, which may present like Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) with widespread epidermal loss. Generalised bullous FDEs can be life-threatening, and a 20% mortality rate has been reported.7
Diagnosis
FDEs are generally diagnosed clinically and rarely cause any abnormalities on laboratory tests. A biopsy may be undertaken, and it is important to include a clear history or suspicion of FDE in the pathology request to assist with the diagnosis because of similarities in histological features with SJS/TEN. A mixed inflammatory infiltrate (including eosinophils and neutrophils) is suggestive for FDE, compared with a predominant lymphohistiocytic inflammatory infiltrate for SJS/TEN. Dermatology consultation is recommended if there is diagnostic uncertainty, including any suspicion of SJS/TEN, or mucosal or systemic involvement.
For the case patient, a biopsy of the chest lesion was performed, which showed confluent apoptotic keratinocytes and lymphocytosis, with large numbers of eosinophils. The histological findings did not distinguish between SJS/TEN, bullous FDE and erythema multiforme, but a drug cause was favoured because of the number of eosinophils. The results of immunofluorescence staining were nonspecific, with scattered IgA, IgG, IgM, C3 and fibrinogen within apoptotic keratinocytes. A diagnosis of bullous FDE caused by allopurinol was made on the basis of the clinical and histological features. Questioning revealed that the patient had experienced a skin eruption after allopurinol treatment six years earlier, with a very similar lesion on the same site on the forearm that was the same size, slightly paler in colour, with no bulla or erosion.
Management
The mainstay of treatment of any FDE is identification and discontinuation of the culprit medication. Subsequent flares can be more severe and it is important to avoid the implicated medication indefinitely.8
For patients with localised FDE, treatment includes topical corticosteroids: medium-potency for the face or flexures and high-potency for the body. An antihistamine, such as loratadine, fexofenadine or cetirizine, can be used to alleviate itch. General skin care measures include showering in lukewarm water with a soap-free cleanser and applying a moisturiser daily.
Patients with generalised bullous FDE may be managed with topical or systemic corticosteroids.8 In severe cases, the clinical presentation may resemble SJS/TEN, with extensive epidermal detachment, necessitating management in a burns intensive care unit for specialised wound care and supportive therapy.
There is recent interest in the use of ciclosporin for generalised bullous FDE, with case reports describing improvement of erythema and cessation of blistering within 24 hours of commencing therapy.8 Despite the favourable results, further high-quality studies with large sample sizes are needed before ciclosporin is implemented in clinical practice.
Outcome
The patient’s allopurinol was ceased immediately. He was treated with loratadine 10 mg tablets and twice daily topical betamethasone dipropionate 0.05% until his symptoms resolved. Appropriate skin care was encouraged. His lesions resolved within a few days, with residual hyperpigmentation for several weeks but no long-term scarring. The patient’s allergy to allopurinol was documented in his electronic medical record and all of his healthcare providers were notified of the allergy. He was advised not to take allopurinol in the future.
Febuxostat, a newer xanthine oxidase inhibitor, has been described to have about 10% cross-reactivity with allopurinol. However, this risk may be nonspecific, as patients who are allergic to a given drug are generally more likely to show allergic reactions to other drugs.9 MT
COMPETING INTERESTS: None.
References
1. Sokumbi O, Wetter DA. Clinical features, diagnosis, and treatment of erythema multiforme: a review for the practicing dermatologist. Int J Derm 2012; 51: 889-902.
2. Carr DR, Houshmand E, Heffernan MP. Approach to the acute, generalized, blistering patient. Semin Cutan Med Surg 2007; 26: 139-146.
3. Yang C, Chen C, Deng S, et al. Allopurinol use and risk of fatal hypersensitivity reactions: a nationwide population-based study in Taiwan. JAMA Intern Med 2015; 175: 1550-1557.
4. Collins P, Sepede J. Bullous arthropod bite reaction. BMJ Case Rep 2018; 11: e228079.
5. Hartman-Adams H, Banvard C, Juckett G. Impetigo: diagnosis and treatment. Am Fam Physician 2014; 90: 229-235.
6. Flowers H, Brodell R, Brents M, Wyatt JP. Fixed drug eruptions: presentation, diagnosis, and management. South Med J 2014; 107: 724-727.
7. Lipowicz S, Sekula P, Ingen-Housz-Oro S, et al. Prognosis of generalized bullous fixed drug eruption: comparison with Stevens-Johnson syndrome and toxic epidermal necrolysis. Br J Dermatol 2013; 168: 726-732.
8. Anderson HJ, Lee JB. A review of fixed drug eruption with a special focus on generalized bullous fixed drug eruption. Medicina (Kaunas) 2021; 57: 925.
9. Bardin T, Chalès G, Pascart T, et al. Risk of cutaneous adverse events with febuxostat treatment in patients with skin reaction to allopurinol. A retrospective, hospital-based study of 101 patients with consecutive allopurinol and febuxostat treatment. Joint Bone Spine 2016; 83: 314-317.
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.