Parasomnias in children – things that go bump in the night

Parasomnias, although mostly benign, can have a dramatic effect on the child and the child’s family. Understanding this common group of sleep disorders can facilitate the GP’s role in not just improving the child’s quality of sleep but also alleviating the parents’ or carers’ anxiety.
- Parasomnias are common sleep disorders in children, often resolving spontaneously by adolescence.
- A detailed history, including sleep diaries and environmental factors, is important for diagnosing parasomnias.
- Most parasomnias are benign and can be managed with reassurance and good sleep habits.
- In more severe cases, psychological support, scheduled awakenings or medications may be considered.
- Referral to a paediatric sleep specialist is recommended for atypical cases, when another sleep disorder such as obstructive sleep apnoea is suspected or when episodes are frequent and distressing.
The term ‘parasomnia’ originates from the Greek words para and somnia meaning ‘around sleep’. The International Classification of Sleep Disorders (ICSD) defines parasomnia as undesirable physical events or experiences that occur during entry into sleep, within sleep or during arousal from sleep.1
Parasomnias are common during childhood with a tendency to resolve spontaneously at puberty. The Tucson Children’s Assessment of Sleep Apnea Study revealed prevalence rates for night terrors, sleepwalking and sleep talking of 0.6%, 6.0% and 1.1%, respectively, among children aged 6 to 11 years. When the cohort was followed up five years later, the remission rates were 100% for night terrors, 50.0% for sleepwalking and 64.8% for sleep talking.2
Although largely benign in nature, parasomnias may result in injuries during sleep and sleep disruption, which in turn may have adverse health effects and a negative impact on psychosocial functioning. Impacts on other family members can also be good. According to the ICSD-Third Edition, text-revision, parasomnias are divided into:
- events associated with nonrapid eye movement (NREM) sleep
- events associated with rapid eye movement (REM) sleep
- other parasomnias
- isolated symptoms and normal variants
(Box 1).1
This article provides an overview of parasomnias in children, with a discussion of various aspects of parasomnias, including types, causes, evaluation, diagnosis and management.
Evaluation
Sleep diaries and sleep logs of the child’s sleep behaviour and home video recordings can help to recognise various abnormalities in the child’s sleep. It is important to obtain a detailed history to determine risk of harm to self or others. A history should be obtained from the child’s parents or carers, and siblings who might have witnessed the parasomnia events. From the history, one should be able to determine possible precipitating or predisposing factors. The most common precipitants for parasomnia include:
- sleep deprivation or poor sleep quality
- medications, such as tricyclic antidepressants
- the presence of illness or fever
- certain medical and neurological disorders, such as obstructive sleep apnoea (OSA) and periodic limb movement disorder, for which screening is important.
Other aspects of the history should include a detailed sleep–wake schedule, assessment of the sleep environment and background medical information.
As parasomnias can be confused with epileptic events or neuropsychiatric disorders, a physical examination should be directed by the history findings. Routinely, an ENT examination for tonsillar enlargement, nasal patency and ear health should be conducted. A neurological history and examination are also recommended to help exclude seizures or risks of seizures. An eye examination can further help exclude other intracranial pathology but mostly reassures the parents that the symptoms are being treated seriously and thoroughly. This might be comforting and sometimes even therapeutic for the child and the child’s family.
Out-of-bed behaviours often do not occur in the sleep laboratory, as the sleeping environment is different and the child is attached to equipment. Furthermore, the probability of capturing parasomnia on polysomnography (PSG) is less likely if the events only occur infrequently. A home video is of considerable help in such cases. Investigations might include a sleep study. This is not routinely indicated except for suspected REM sleep behaviour disorder, or if there are atypical features such as stereotypy, or if the semiology is particularly distressing for the child or the child’s family. Extra EEG leads, in addition to those for sleep scoring, can be employed with infrared videography. Normal study findings do not rule out a diagnosis of a parasomnia. The evaluation recommendations, for which the acronym TERROR might be useful, are summarised in Box 2.
PSG may capture high-amplitude hypersynchronous delta waves and frequent arousals from slow wave sleep in disorders of arousal. However, these findings are nonspecific, as they have been reported in other disorders, such as OSA, and even in asymptomatic individuals. PSG may be useful in ruling out the differential diagnosis of nocturnal epilepsy. PSG may also demonstrate potential triggers for parasomnia such as sleep-associated breathing disorders or periodic limb movement disorder. Features such as a history of snoring, pauses in breathing and restless sleep should be elicited.
Events associated with nonrapid eye movement sleep
NREM-associated parasomnias (commonly named disorders of arousal) are an admixture of wakefulness and NREM sleep. The spectrum of these partial arousals includes confusional arousals, sleepwalking and night terrors. These conditions, which usually occur during the first third of the sleep, commence during the partial arousals from slow wave (N3) sleep. Most episodes are brief but, in some children, may last as long as 30 to 40 minutes. The eyes are usually open, often with a confused ‘glassy’ stare. The patients may be very difficult to awaken and are confused when awoken, with amnesia for the episodes the next day. Despite exhibiting complex behaviours, the high-level cognitive functions, such as attention, planning, social interaction and intent, are absent. The first reported single-photon emission computed tomography scan of sleepwalking was published in 2000, showing quiescence of the prefrontal cortex but high levels of activation in the motor cortex.3
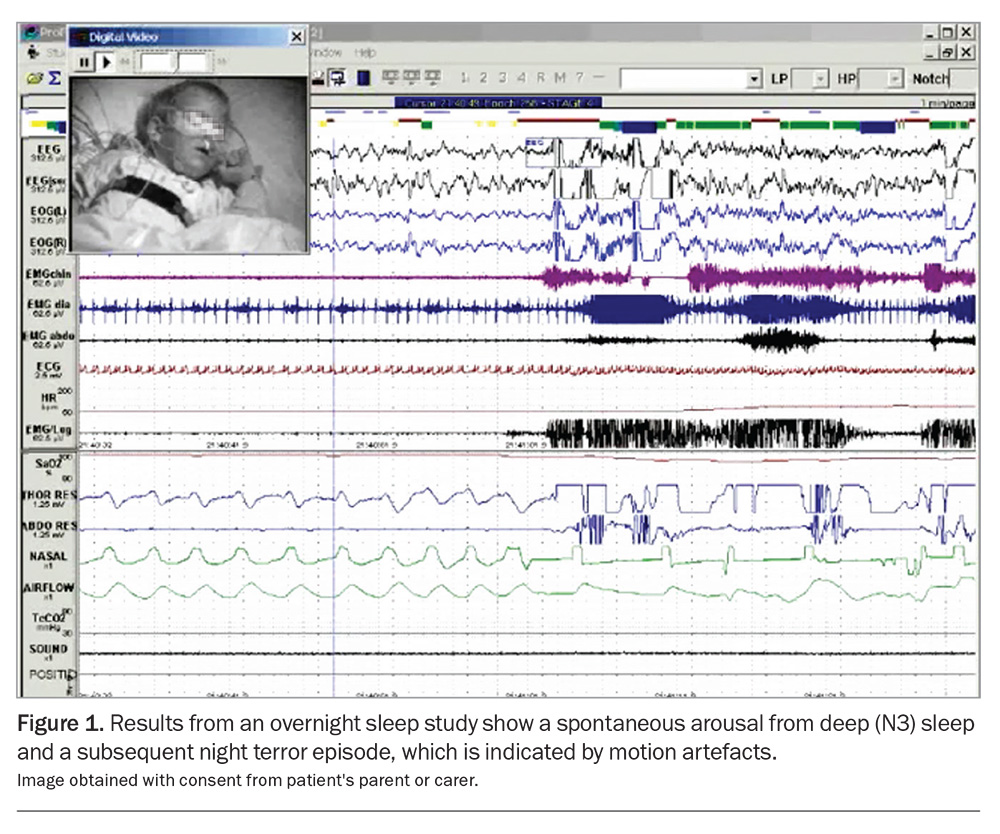
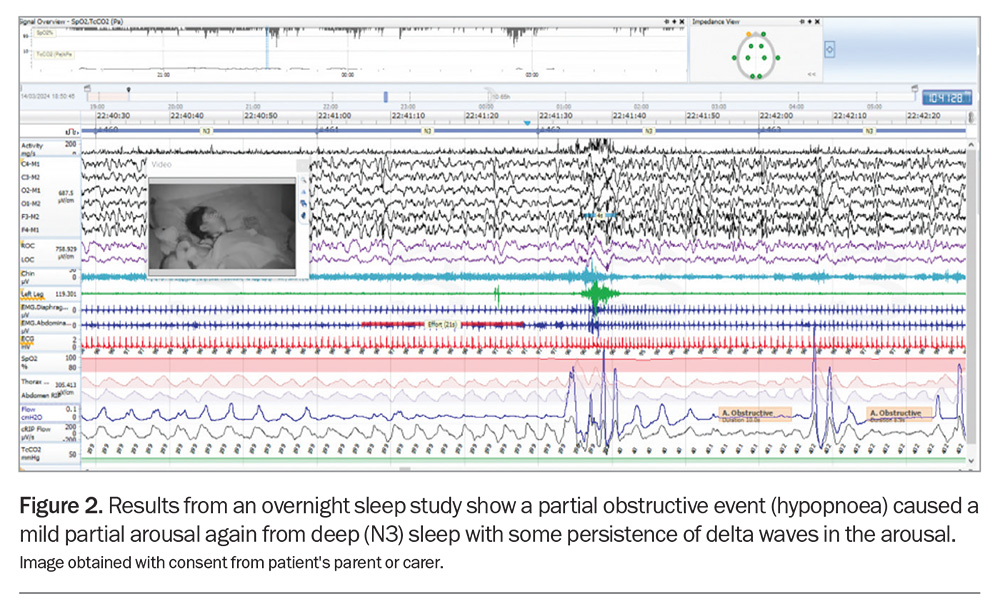
These partial arousal disorders share common genetic and familial patterns, arise from deep sleep and are similarly primed by sleep deprivation and biopsychosocial stressors. OSA and other sleep-associated respiratory events are also known precipitating factors. External or environmental stimuli, such as a telephone call, may also precipitate an episode. Some other known triggers include sleeping in new surroundings, physical or emotional stress and febrile states. A spontaneous arousal from deep (N3) sleep and a subsequent night terror episode captured on video is shown in Figure 1. A partial obstructive event (hypopnoea) that caused a mild partial arousal again from N3 with some persistence of delta waves in the arousal is shown in Figure 2.
Confusional arousals
Confusional arousals occur with the patient in bed, sitting up and looking about in a confused manner, often with vocalisation. During an episode of a confusional arousal, there is usually no autonomic arousal such as dilated pupils, tachycardia, tachypnoea or sweating.
Sleepwalking
Sleepwalking episodes usually involve the patient leaving the bed. The sleepwalker may become agitated or behave violently. At times, sleepwalking involves inappropriate behaviours such as urinating in the kitchen cabinet or climbing out a window. The sleepwalker may bump into objects, causing bruises and cuts. Sleepwalkers may even travel outside the house, raising concerns for their safety. As there is often anterograde and retrograde amnesia, the child may be disorientated to the place and time when awoken from sleep. Potentially profound forensic implications of these parasomnias are well reported in the adult literature.4-5
Sleep terrors
During a sleep terror, the child often cries or screams and episodes are typically accompanied by autonomic arousals, such as tachycardia, tachypnoea, diaphoresis, mydriasis and increased muscle tone (Table).1,6 The child can be unresponsive to external stimuli. Attempts made to calm the child via restraint may increase distress. There may be prolonged inconsolability following a night terror.
Differential diagnosis
Clinicians should investigate for other medical conditions that may cause simple or complex motor patterns during sleep such as seizures, dissociative psychiatric events and even hypoglycaemia. It is important to exclude potential medical disorders as the precipitant for parasomnias. These might include diseases that are often aggravated by sleep such as gastric reflux disease and asthma. Sleep disorders, such as OSA and periodic limb movement disorder, can precipitate the disorder of arousal. In adolescents, alcohol- and drug-associated behaviours must be considered. Stereotypy should raise suspicions of a seizure disorder.7
Management
As most parasomnias are benign in nature and decline spontaneously with age, the first-line treatment in children is reassurance. However, parasomnias can disrupt parental sleep as well as causing concern and anxiety. Furthermore, parasomnias may affect a child’s behaviour and self-esteem. Some children might feel more tired during the day after an episode of parasomnia, particularly if the episode was prolonged, which may impact behaviour and functioning.
Parents or carers are taught to minimise precipitating factors such as sleep deprivation, stress and environmental disturbances, where possible. Precautions to ensure a safe home environment should be emphasised, such as securing windows, installing locks and alarms, placing barriers at staircases, securing sharp or dangerous items out of the child’s reach and removing obstacles in the bedroom.
Treatments should start with optimising sleep routines and fostering good sleep habits (sleep hygiene). Anticipatory or scheduled awakenings may be utilised, wherein parents may construct a diary to ascertain the approximate time at which the events typically occur and then awaken their child 15 to 20 minutes before the predicted time of occurrence for a period of one month.8 The success rate of this approach, anecdotally, is around 50%.
Psychological support has been suggested to overcome the manifestation from certain triggers, if certain stressors are identified. The treatment of precipitating sleep disorders such as OSA may cause a marked improvement or resolution.9 Iron therapy in children with restless legs syndrome or periodic limb movement disorder and parasomnia is associated with resolution of the parasomnia.10
Pharmacological therapy is considered if the episodes are frequent and persist despite resolution of predisposing factors, or if the behaviours are associated with a high risk of injury or cause significant daytime impairment or family disruption. Benzodiazepines, such as diazepam or clonazepam, and tricyclic medications that decrease slow-wave sleep due to their sedative effects, have been found to be effective in adults. These are rarely used in paediatrics and children should be referred to a sleep physician for further assessment. There are currently no specific medications for parasomnias approved for children. Melatonin has been found to be helpful for children with circadian rhythm disorders, potentially treats insomnia and might help in adults with REM sleep behaviour disorder (RBD). Melatonin might raise the arousal threshold and improve sleep terrors and sleepwalking.11 However the evidence level is low in terms of efficacy.
Rapid eye movement sleep parasomnias
Rapid eye movement sleep behaviour disorder
RBD was initially described as a parasomnia occurring in older men by Schenk et al. in 1986.12 This is extremely rare in children. However, Lloyd et al. reported 15 children with RBD aged 3 to 17 years from a cohort of children seen during a 10-year period.13 Comorbidities were common and multiple among children with this rare disorder, including attention deficit disorder, anxiety, developmental delays, abnormal brain scans, narcolepsy and conditions managed with the use of antidepressant medications.
The behaviours noted in RBD vary in severity from loud talking, swearing, laughing, shouting and giving speeches to grabbing and leaping out of bed. A child with RBD will awaken quickly after an episode, becoming alert with recall of the dream. The eyes are usually closed during the episode.
RBD occurs during REM sleep, and the episodes usually occur later in the sleep cycle, around 90 minutes or more after sleep onset, except if it coexists with narcolepsy, as RBD may occur during an early sleep-onset REM period. It may be challenging to distinguish REM from NREM parasomnias based on history alone. Apart from the recollection of the vivid, scary dreams, the motor activity in RBD tends to be more aggressive, causing a child with RBD to commonly experience sleep-associated injury.
During REM, the typical electromyographic findings are atonia in the normal population. The use of video PSG is recommended as per the ICSD-3 to help diagnose RBD, as PSG helps detect an excess of muscle tone and an excess of phasic twitching activity during REM sleep, which are the hallmarks of RBD.
Most children with RBD respond to treatment with low-dose clonazepam and melatonin, but the evidence base for these is thin. For those on antidepressant medications, withholding these medications may result in resolution of RBD.
Recurrent isolated sleep paralysis
Sleep paralysis (SP) can be frightening for children. The episodes of paralysis or inability to move the legs, arms and often the entire body, frequently with a feeling of a great weight on the chest, are accompanied by vivid hypnagogic (sleep onset) and hypnopompic (sleep offset) hallucinations; these may be either auditory, visual or tactile in 25 to 75% of patients. For centuries and across different cultures, SP is thought to be a spiritual or supernatural phenomenon attributed to witchcraft, malevolent spirits or alien abductions.14
SP is common, with data from 35 studies including 36,533 patients showing that 7.6% of the general population has experienced at least one episode of SP in their lifetime.15 There is usually a positive history of SP in the family, suggesting a genetic predisposition. Other risk factors linked to SP are an increased body mass index, smoking, alcohol consumption, poor sleep quality, anxiety disorders and exposure to traumatic events. Idiopathic hypersomnia, OSA, narcolepsy and Wilson’s disease also increase the risk for SP.
Management for SP initially focuses on improving sleep hygiene, minimising sleep loss and reducing insomnia symptoms. Cognitive behavioural therapy focusing on relaxation techniques for use during SP episodes has been practised with positive results reported. This method involves helping the child reframe the experience of the SP episode by reassuring themselves that these episodes are common, harmless and temporary, and that there is no need to be afraid. The child should then focus their attention on a positive object, such as a pleasant memory, song or prayer, while relaxing the muscles until the episode ceases.16 The extraocular muscles and diaphragm are relatively spared in REM atonia; thus, anecdotally, blinking, panting or coughing can sometimes shorten the SP episode.
Nightmare disorder
Between 60 and 75% of children have occasional nightmares, which typically start between the ages of 3 and 6 years. More children between 6 and 10 years of age report nightmares, but the occurrence decreases in older children. Frequent nightmares, however, are uncommon, occurring in 3 to 6% of children. The prevalence of nightmare disorder is higher in children with severe psychosocial stressors.
Nightmare disorder typically occurs in the last third of the night, at the time when REM pressure is the most prominent. The content of nightmare disorder often causes grief to the child, as it involves distressing themes and is associated with negative emotions, such as fear, anxiety, anger, embarrassment and disgust. Upon awakening, the child can usually provide a detailed description of the events. This may cause anxiety and hinder the resumption of sleep. Reassurance, avoidance of the use of electronic devices for at least an hour before bedtime, rescripting techniques or ‘dream imagery rehearsal’ may be helpful, in which the child and the child’s parents or carers, possibly with a therapist, discuss the dream and invent less frightening endings.17 The child might be encouraged to write or draw out their dreams. The use of medications that can cause nightmares, such as antidepressants and antihypertensives, should be re-evaluated. Prazosin has been used with some positive results in severe cases, especially in the context of post-traumatic stress disorder.18
Conclusion
In summary, parasomnias are common in children. Compared with adults, in whom parasomnias may be associated with psychiatric or neurodegenerative disorders, parasomnias in children are usually benign in nature and do not tend to persist into adolescence or adulthood. A thorough and targeted history is the mainstay of diagnosing parasomnia. Management generally focuses on improving sleep habits, optimising environmental safety, avoiding trigger factors, treating underlying causes and reassuring the child and child’s family. A referral to a paediatric sleep physician should be considered where there are atypical features, suspicion of an underlying disorder (such as OSA) or if the episodes are very distressing and frequent. MT
COMPETING INTERESTS: Dr Razak: None. Dr Teng has received honoraria for lectures from Aspen Pharmaceuticals.
References
1. American Academy of Sleep Medicine (AASM). The AASM International Classification of Sleep Disorders – Third Edition, Text Revision (ICSD-3-TR). Darien, IL, USA: AASM; 2023.
2. Furet O, Goodwin JL, Quan SF. Incidence and remission of parasomnias among adolescent children in the Tucson Children's Assessment of Sleep Apnea (TuCASA) Study. Southwest J Pulm Crit Care 2011; 2: 93-101.
3. Bassetti C, Vella S, Donati F, et al. SPECT during sleepwalking. Lancet 2000; 356: 484-485.
4. Pressman R, Mahowald M, Schenck CH, et al. Alcohol-induced sleepwalking or confusional arousal as a defense to criminal behavior: a review of scientific evidence, methods and forensic considerations. J Sleep Res 2007; 16: 198-212.
5. Castelnovo A, Schraemli M, Schenck CH, et al. The parasomnia defence in sleep-related homicide: a systematic review and a critical analysis of the medical literature. Sleep Med Rev 2024; 74: 101898.
6. Lam JS. NREM Parasomnias: Disorder of arousal. In: Li AM, Chan KC, editors. Paediatric sleep disorders: Case-based practical guide. Singapore; Springer: 2022. p. 139-144.
7. Derry CP, Davey M, Johns M, et al. Distinguishing sleep disorders from seizures: diagnosing bumps in the night. Arch Neurol 2006; 63: 705-709.
8. Tobin JD Jr. Treatment of somnambulism with anticipatory awakening. J Pediatr 1993; 122: 426-427.
9. Guilleminault C, Palombini M, Pelayo R, Chervin RD. Sleepwalking and sleep terrors in prepubertal children: what triggers them? Pediatrics 2003; 111: e17-e25
10. Gurbani N, Dye TJ, Dougherty K, Jain S, Horn PS, Simakajornboon N. Improvement of parasomnias after treatment of restless leg syndrome/ periodic limb movement disorder in children. J Clin Sleep Med 2019; 15: 743-748.
11. Proserpio P, Terzaghi M, Manni R, Nobili L. Drugs used in parasomnia. Sleep Med Clin 2018; 13: 191-202.
12. Schenck CH, Bundlie SR, Ettinger MG, Mahowald MW. Chronic behavioral disorders of human REM sleep: a new category of parasomnia. Sleep 1986;9: 293-308.
13. Lloyd R, Tippmann-Peikert M, Slocumb N, Kotagal S. Characteristics of REM sleep behavior disorder in childhood. J Clin Sleep Med 2012; 8: 127-131.
14. Sharpless B, Doghramji K. Chapter 3, The history of sleep paralysis in folklore and myth. In: Sleep paralysis: historical, psychological, and medical perspectives. New York, NY, USA: Oxford Academic; 2015. p.17-44.
15. Sharpless BA, Barber JP. Lifetime prevalence rates of sleep paralysis: a systematic review. Sleep Med Rev 2011; 15: 311-315.
16. Jalal B. How to make the ghosts in my bedroom disappear? Focused-attention meditation combined with muscle relaxation (MR Therapy)-a direct treatment intervention for sleep paralysis. Front Psychol 2016; 7: 28.
17. Gill P, Fraser E, Tran TTD, et al. Psychosocial treatments for nightmares in adults and children: a systematic review. BMC Psychiatr 2023; 23: 283.
18. Paiva HS, Filho IJZ, Cais CFDS. Using prazosin to treat posttraumatic stress disorder and associations: a systematic review. Psychiatry Investig 2021; 18: 365-372.
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.