Palliative care in general practice: challenges, myths and opportunities

GPs play a pivotal role in palliative care, navigating complex physical, psychosocial and existential needs. Although ideally positioned to provide holistic, continuous care, they face significant challenges. This article outlines core principles, clarifies the roles of specialist services and offers practical guidance on referral.
- Palliative care can occur alongside ongoing active or disease-modifying treatment.
- Palliative care is appropriate for patients with malignant or nonmalignant life-limiting or life-threatening illness. Referral is based on unmet needs (physical, psychological, social or spiritual).
- Describing the activities of the palliative care team, including how it provides an extra layer of support, screens for and addresses unmet needs and assists with advance care planning, can reduce patient barriers to referral.
- Early integration of palliative care improves symptom control, quality of life and caregiver outcomes.
- Decision support tools (such as the Supportive and Palliative Care Indicators Tool) and local resources (such as HealthPathways) can assist GPs in identifying patients with unmet palliative care needs and navigating referral pathways.
GPs serve as the primary interface for a broad array of health concerns, delivering longitudinal care that encompasses every stage of life. However, the multifaceted nature of palliative care, encompassing physical, psychological, social and existential dimensions, presents unique and often demanding challenges. Although GPs are ideally positioned to offer holistic, continuous care throughout the lifespan, numerous well-documented barriers can impede the delivery of high-quality palliative care, particularly for patients with complex needs. This article revisits the core principles of palliative care, clarifies what specialist services can provide and offers practical guidance on when and how to refer. For many GPs, this may offer assistance in navigating this crucial area of practice.
Despite an overwhelming body of evidence that early integration of palliative care with disease management is beneficial to patients, families and health systems, there are still many people with chronic life-threatening illness who are not referred or referred only in the terminal phase of their illness.1-4 This underutilisation can result in unnecessary suffering and missed opportunities to support patients in living well despite advanced disease.5
What is palliative care?
Palliative care is an approach that improves the quality of life of patients and their families who are facing problems associated with life-threatening illness. It prevents and relieves suffering through the early identification, correct assessment and treatment of pain and other problems, whether physical, psychosocial or spiritual.1
The World Health Organization (WHO) defines palliative care as care that:
- provides relief from pain and other distressing symptoms
- affirms life and regards dying as a normal process
- intends neither to hasten nor postpone death
- integrates psychological and spiritual aspects of patient care
- offers a support system to help patients live as actively as possible until death
- offers a support system to help the family cope during the patient’s illness and in bereavement
- uses a team approach to address the needs of patients and their families
- enhances quality of life and may positively influence the course of illness
- is applicable early in the course of illness, alongside therapies intended to prolong life, such as chemotherapy or radiation therapy, and includes those investigations needed to better understand and manage distressing clinical complications.1
Benefits of early integration
There is overwhelming evidence that palliative care improves patient outcomes, including better symptom control, increased quality of life, optimisation of function (with physiotherapy, occupational therapy and dietitian involvement), and improved emotional wellbeing and caregiver outcomes, such as reduced psychological distress and complicated bereavement.2 It is also cost neutral, if not cost saving, for the health system.6 Importantly, early referral to palliative care has been shown not only to enhance quality of life but, in some cases, to prolong it.7,8
General practice and palliative care: a natural alignment
GPs are ideally placed to provide general palliative care to their patients. The WHO declaration of Astana calls for palliative care to be both ‘accessible to all’ and an ‘essential component of primary healthcare worldwide’. This aligns with the Royal Australian College of General Practitioners’ view that end-of-life care is part of comprehensive care.9
GP involvement in palliative care provides measurable benefits.10 These include improved quality of life, maintenance of functional status, increased likelihood of dying at home, reduced health service use and significant reductions in healthcare costs.10-18
Barriers to delivering palliative care in general practice
Despite this alignment, GPs face clear challenges in providing palliative care. Time constraints, poor remuneration, lack of access to informational support from specialists, and insufficient education and training, including training on difficult conversations, all contribute to waning involvement. A considerable proportion of GPs (25–37%) report minimal or no interest in providing palliative care, underscoring the importance of addressing these systemic issues.19,20
Compounding these challenges is the looming workforce shortage of GPs in Australia, set against a backdrop of an ageing population and increasing demand for palliative care services.1,2 This mismatch between capacity and need calls for thoughtful policy and service planning.
Why are GPs not referring more?
Given the increasing challenges GPs face in delivering palliative care, one might expect a corresponding increase in referrals to specialist services. However, referral rates remain stubbornly low. In fact, 62% of people (three in five) who would benefit from palliative care do not receive specialist palliative care services.21 This disconnect likely reflects a range of barriers, including limited awareness of services, uncertainty around referral criteria and reluctance from both clinicians and patients.
What are these challenges?
Awareness of services and navigating the referral landscape
Community palliative care teams and palliative care units are often not co-located with major hospitals, which can contribute to a lack of awareness about their existence. Limited exposure to palliative care during medical school and early clinical training further restricts understanding of what these services can offer.
As general practice becomes increasingly broad and demanding, it is difficult for GPs to maintain up-to-date knowledge of available services. Coupled with time pressures during consultations, GPs need quick, reliable access to clinical guidelines, referral criteria and service contact information.
In general, specialist palliative care services typically fall into three categories:
- inpatient consultation teams: these teams consult on hospital inpatients, usually referred by the admitting team. In some hospitals, they have admitting rights for palliative patients, and may also run outpatient clinics, which GPs may refer to
- palliative care units: stand-alone or hospital-affiliated units providing short stays for symptom management, carer stress or care in the last days of life
- community palliative care teams: multidisciplinary teams that may involve palliative care physicians, doctors in training, nurse practitioners, nurses, occupational therapists, physiotherapists and social workers. They may visit patients at home, in residential aged care facilities or conduct reviews in clinic or via telehealth. These teams are the most appropriate for GP referral.
In a study of GP perspectives, HealthPathways was frequently cited as a useful source of information.22 Developed nationally by Primary Health Networks in partnership with Local Health Districts, HealthPathways aims to consolidate fragmented clinical and referral information. In many regions, it represents the ideal starting point for locating local palliative care services.
Service structures vary significantly across the country, influenced by local resources and geography. The peak body for each state and territory can be found on the Palliative Care Australia website (https://palliativecare.org.au/about-pca/). Connecting with these organisations, such as Palliative Care NSW, can help GPs identify the most appropriate local services. If in doubt, calling the local hospital for advice remains a pragmatic and often effective option.
Knowing who and when to refer: referral criteria and decision support tools
Specialist palliative care services vary in their capacity depending on location, resources and staffing. Consequently, local referral guidelines differ. However, specialist consultation should be considered when the needs of the patient or family exceed the expertise of the primary care team, or when such referral is necessary to access specific services, such as occupational therapy, physiotherapy or social work.5
In Northern Sydney, for example, referral guidelines for community palliative care include:
- a progressive life-limiting or life-threatening illness (malignant or nonmalignant)
- the patient or substitute decision maker consents to the referral
- plus at least one of the following:
– complex symptoms requiring specialist management
– complex emotional, psychosocial or spiritual needs
– need for support in advance care planning
– where it would not be a surprise if the patient died within the next 12 months and additional support is required.
Palliative Care Australia additionally lists the following reasons for referral:
- equipment for home care
- support for sensitive family conversations
- links to financial, social or cultural support
- grief and bereavement services.
Referral documentation should ideally include:
- diagnosis and current symptom management challenges
- relevant pathology and imaging
- advance care plans, if available
- relevant specialist correspondence.
Importantly, patients do not require an oncological diagnosis. Supportive care for advanced chronic disease, such as chronic kidney disease, liver disease, heart failure or chronic obstructive pulmonary disease, falls within the palliative care umbrella. Although prognostication is more difficult, functional decline, repeated hospitalisations or escalating symptom burden are cues for referral.
Decision support tools include:
- the double surprise question: ‘Would I be surprised if this patient died within the next year?’ and ‘Would I be surprised if they didn’t?’
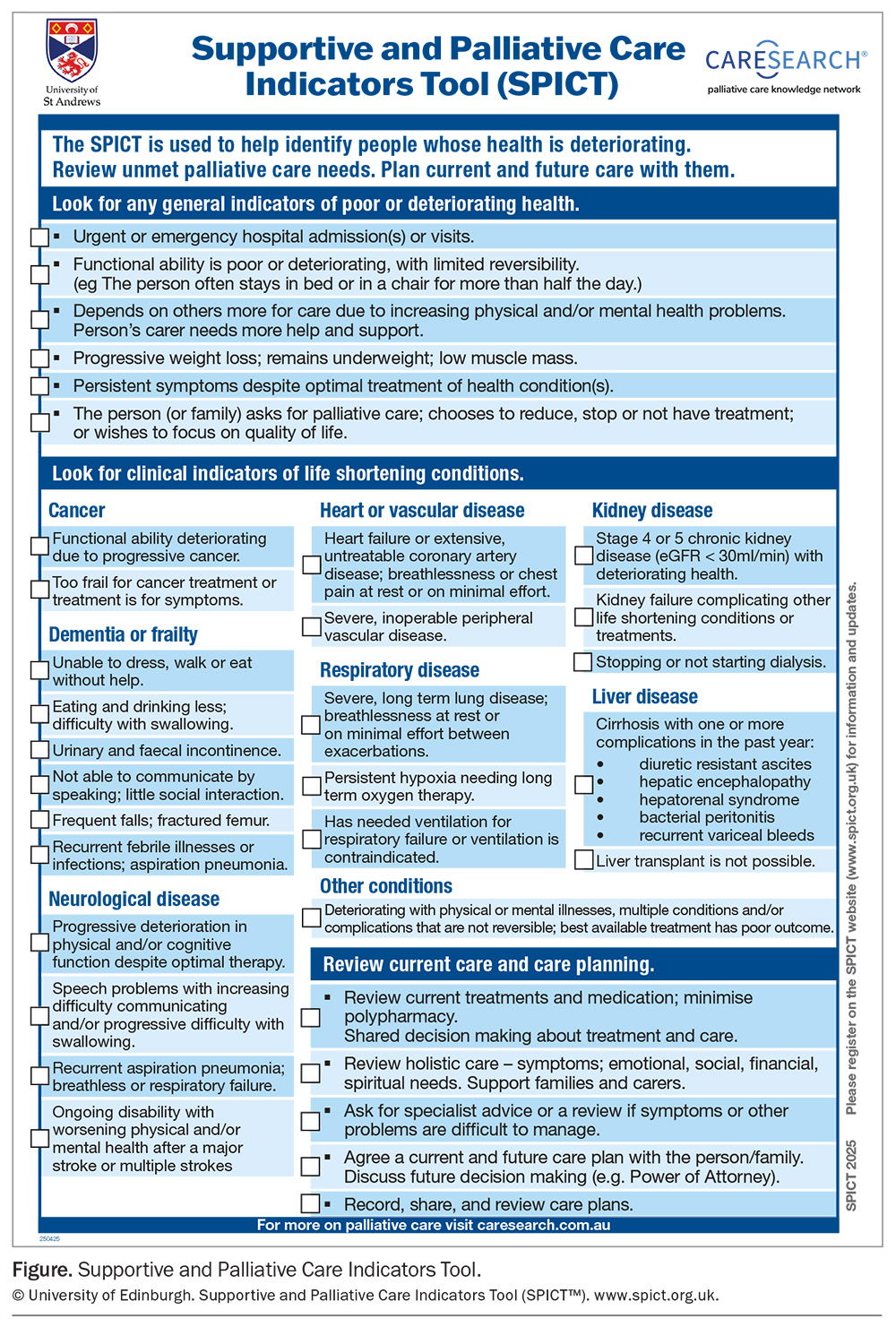
- Supportive and Palliative Care Indicators Tool (SPICT): disease-specific indicators to help identify patients with unmet needs (see Figure).
Reluctance from patients and GPs
Dispelling misconceptions
Reluctance to accept a referral to palliative care is a well-recognised issue across healthcare systems, with specific reasons for this resistance varying based on a person’s cultural, religious or ethnic background. For many, palliative care is synonymous with imminently dying and may be perceived as their GP or specialist giving up on them. Similarly, there are well-documented reasons for GPs being reluctant to refer, including patient perception of abandonment, professional territorialism, fear of the palliative care team taking over care and assumption that patients cannot have disease-modifying treatment if they are also receiving palliative care.
A common misconception is that palliative care is only appropriate once all disease-modifying therapies are exhausted. However, evidence shows that the earlier the introduction of palliative care, the better the outcomes in terms of quality of life and length of life.7,8 Hence palliative care can be delivered alongside treatments targeting the underlying disease, and patients can still choose to have treatment of reversible causes in an acute hospital if they wish, and if it is clinically appropriate.
Uncertainty about roles
Instead of a handover model, shared care should be promoted, with the right person providing the right care at the right time. This may mean the palliative care team steps in and out throughout a patient’s illness trajectory.
Communication is key. Some GPs appreciate phone calls or inclusion in case conferences, whereas others prefer written updates. Early conversations between teams to set expectations can improve satisfaction and continuity of care. Patients also benefit, with studies showing they report better experiences when their healthcare providers are aligned.23,24
An area for early role clarification is prescription writing. Most community palliative care teams operate as consult teams. Although occasionally they may write prescriptions for medication initiation or urgent medication changes, services typically do not have capacity to provide ongoing prescriptions for all the patients they consult on, and patients are referred back to primary care for this, as happens with other specialist consultations. Depending on resourcing and geography, there will be some community palliative care teams that are nurse led and without capacity to prescribe at all, so early discussions around expectations are valuable.
Separating palliative care from voluntary assisted dying
Palliative care is distinct from voluntary assisted dying (VAD). Although palliative care patients may consider VAD, the process is managed by a separate team. Referral to palliative care is not a gateway to VAD, nor is it incompatible with its consideration. In fact, palliative care should be offered to all patients exploring VAD, to support the relief from distressing symptoms (experienced or anticipated) and ensure comprehensive psychosocial care.
Practical recommendations for GPs
To support increased and effective GP engagement in palliative care, we recommend:
- early identification of patients with palliative care needs: use SPICT, the double surprise question and clinical red flags (as outlined in the referral criteria section above and the specific clinical signs described in SPICT)
- use of HealthPathways: access local referral criteria, services and clinical guidelines
- starting the conversation early: introduce palliative care by describing its activities, including screening for physical, psychological, spiritual and social needs; conversations to determine the patient’s goals for care; support of the patient and family; and a focus on living well, not dying soon25
- early partnership with specialist teams: refer when the patient’s needs exceed the GP’s scope of practice; do not wait for a crisis
- clarifying roles and communication: establish responsibilities and preferred communication processes with palliative care teams
- educating patients and families: reframe palliative care as added support, not an end-of-line service.
Some useful online resources for GPs on palliative care are included in the Box.
Conclusion
GPs are already equipped with the core competencies required to provide meaningful palliative care – compassion, continuity and a deep understanding of their patients. With greater clarity around referral pathways, access to multidisciplinary support and the debunking of common misconceptions, GPs can feel empowered to initiate and integrate palliative care earlier and more confidently.
Importantly, referral to specialist palliative care services is usually straightforward and well supported. Community teams are experienced in working closely with general practice and are very willing to be contacted directly. GPs are encouraged to phone their local palliative care service to discuss whether a patient may be appropriate for referral or to seek guidance on symptom management and care planning.
Palliative care does not signal the end. It signals the opportunity to live better, longer and with more support. GPs do not need to carry the whole weight alone. With a few good tools, a trusted referral network and a shift in perspective, palliative care becomes not a burden, but a natural extension of the care GPs already provide so well. MT
COMPETING INTERESTS: Dr Fletcher: None. Professor Lovell has received support for attending Asia Pacific Hospice Conference from the organisers.
References
1. World Health Organization. Palliative care. Geneva: WHO; 2020. Available online at: https://www.who.int/news-room/fact-sheets/detail/palliative-care (accessed February 2026).
2. NSW Government. NSW Health. End of life and palliative care framework 2019–2024. Sydney: NSW Government; 2019.
3. Creangă-Murariu I, Froicu EM, Scripcariu DV, et al. Timing matters: a systematic review of early versus delayed palliative care in advanced cancer. Cancers (Basel) 2025; 17: 2598.
4. Haroen H, Maulana S, Harun H, et al. The benefits of early palliative care on psychological well-being, functional status, and health-related quality of life among cancer patients and their caregivers: a systematic review and meta-analysis. BMC Palliat Care 2025; 24(1): 120.
5. Hawley P. Barriers to access to palliative care. Palliat Care: 2017; 10: 1178224216688887.
6. Temel JS, Greer JA, Muzikansky A, et al. Early palliative care for patients with metastatic non-small-cell lung cancer. N Engl J Med 2010; 363: 733-742.
7. Bakitas MA, Tosteson TD, Li Z, et al. Early versus delayed initiation of concurrent palliative oncology care: patient outcomes in the enable III randomized controlled trial. J Clin Oncol 2015; 33: 1438-1445.
8. Temel JS, Greer JA, El-Jawahri A, et al. Effects of early integrated palliative care in patients with lung and GI cancer: a randomized clinical trial. J Clin Oncol 2017; 35: 834-841.
9. Royal Australian College of General Practitioners (RACGP). Standards for general practice. 5th Ed. Melbourne: RACGP; 2023.
10. Damarell RA, Morgan DD, Tieman JJ, Healey D. Bolstering general practitioner palliative care: a critical review of support provided by Australian Guidelines for Life–Limiting Chronic Conditions. Healthcare (Basel) 2020; 8(4): 553.
11. Han PK, Rayson D. The coordination of primary and oncology specialty care at the end of life. J Natl Cancer Inst Monogr 2010; 2010: 31-37.
12. Mitchell G, Zhang J, Burridge L, et al. Case conferences between general practitioners and specialist teams to plan end of life care of people with end stage heart failure and lung disease: an exploratory pilot study. BMC Palliat Care 2014; 13: 24.
13. Tapsfield J, Hall C, Lunan C, et al. Many people in Scotland now benefit from anticipatory care before they die: an after death analysis and interviews with general practitioners. BMJ Support Palliat Care 2019; 9(4): e28.
14. Carmont SA, Mitchell G, Senior H, Foster M. Systematic review of the effectiveness, barriers and facilitators to general practitioner engagement with specialist secondary services in integrated palliative care. BMJ Support Palliat Care 2018; 8: 385-399.
15. Mitchell GK, Del Mar CB, O’Rourke PK, Clavarino AM. Do case conferences between general practitioners and specialist palliative care services improve quality of life? A randomised controlled trial. Palliat Med 2008; 22: 904-912.
16. Kim SL, Tarn DM. Effect of primary care involvement on end-of-life care outcomes: a systematic review. J Am Geriatr Soc 2016; 64: 1968-1974.
17. Thoonsen B, Vissers K, Verhagen S, et al. Training general practitioners in early identification and anticipatory palliative care planning: a randomized controlled trial. BMC Fam Pract 2015; 16: 126.
18. Tran B, Falster MO, Girosi F, Jorm L. Relationship between use of general practice and healthcare costs at the end of life: a data linkage study in New South Wales, Australia. BMJ Open 2016; 6:e009410.
19. Rhee JJ, Zwar N, Vagholkar S, Dennis S, Broadbent AM, Mitchell G. Attitudes and barriers to involvement in palliative care by Australian urban general practitioners. J Palliat Med 2008; 11: 980-985.
20. Coulton C, Boekel C. Research into awareness, attitudes and provision of best practice advance care planning, palliative care and end of life care within general practice. Canberra: Australian Government, Department of Health, Disability and Ageing; 2017. Available online at: https://www.health.gov.au/sites/default/files/gp-best-practice-research-project_0.pdf (accessed February 2026).
21. Palliative Care Australia. Recent developments in national palliative care data. Canberra: Palliative Care Australia; 2025. Available online at: https://palliativecare.org.au/statement/recent-developments-in-national-palliative-care-data/ (accessed February 2026).
22. Fletcher A. Understanding the functional relationship between general practice and specialist palliative care. RACP project 2024 [not published].
23. Nielsen JD, Palshof T, Mainz J, Jensen AB, Olesen F. Randomised controlled trial of a shared care programme for newly referred cancer patients: bridging the gap between general practice and hospital. Qual Saf Health Care 2003; 12: 263-272.
24. Couchman E, Ejegi-Memeh S, Mitchell S, Gardiner C. Facilitators of and barriers to continuity with GPs in primary palliative cancer care: a mixed-methods systematic review. Prog Palliat Care 2022; 31: 18-36.
25. Selvam D, Crawford GB, Rizvi F, Bellingham K, Philip J. CarePlus: a model to address barriers to early palliative care in cancer. J Pain Symptom Manage 2024; 67: e495-e497.
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.