The older traveller

About 30% of people aged over 60 years travel overseas annually to both routine and exotic destinations. It is essential to minimise risks by encouraging the older traveller to undergo a comprehensive pretravel medical examination, which includes reviewing medications, checking vaccinations are up to date and assessing overall fitness for the intended journey. Travel can enhance physical and mental wellbeing in older adults, and may reduce mortality rates.
- Older people in Australia increasingly travel overseas each year.
- Although morbidity and mortality increase with age, healthy older travellers may face no greater risk than if they stayed home. In fact, travel itself may help maintain or improve health.
- Comorbid conditions, especially if poorly controlled, are more important to assess than chronological age when evaluating fitness to travel. Stable conditions, such as well-controlled diabetes and mild-to-moderate ischaemic heart disease, are unlikely to present issues during travel.
- A thorough pretravel medical examination should include a review of chronic diseases, medications, vaccinations and overall fitness for the intended journey.
- GPs play a key role in providing individualised preventive advice to older travellers, helping them to minimise health risks.
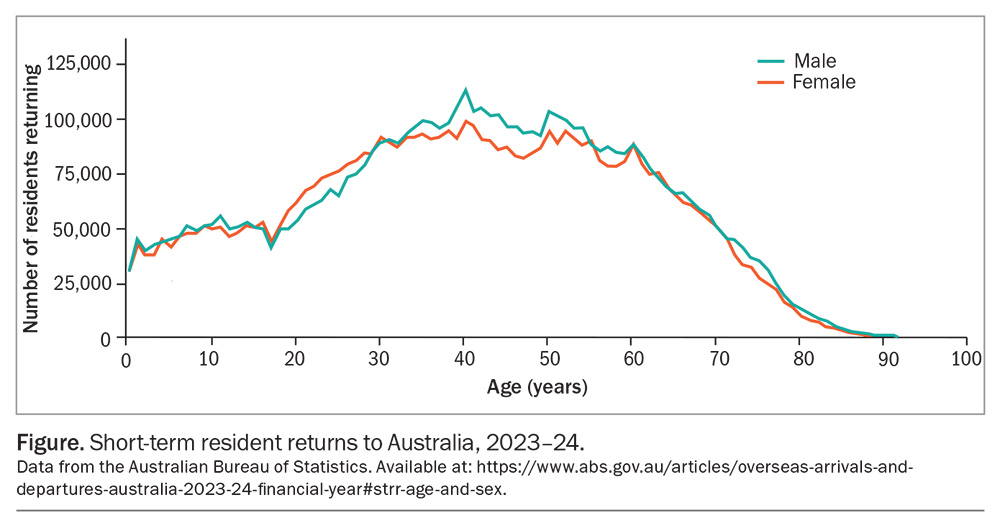
The rapid ageing of Australia’s population has resulted in 20% of people being aged 65 years or older.1,2 Although the majority of travellers are younger, it is estimated that up to 30% of people aged over 60 years (about 1.5 million individuals) travel overseas annually to both routine and exotic destinations.3 Data from the Australian Bureau of Statistics on short-term resident returns for the 2023–24 financial year is presented in the Figure. Given that most people in this age group consult with their GP annually, it is important to consider overall health and wellbeing, as well as chronological age, when providing travel advice. This article discusses key considerations for GPs to help older travellers minimise health risks.
Defining ‘old’
Various definitions of ‘old’ exist in the medical literature (Box 1). An age range over 60 to 65 years is commonly used to define ‘old’ in the medical literature and is generally accepted by the medical community.
Does travel improve health or are older travellers healthier?
It is well recognised that the risk of morbidity and mortality increases with age. Consequently, older people often face higher travel insurance premiums. However, empirical evidence specifically linking advanced age to increased travel-related risk is limited. Some studies suggest that healthy older travellers may not face significantly greater risks than if they remain at home.4-6
Older travellers may be healthier either because they are already in good health and therefore more able to travel, or because travel itself may help maintain or even improve their health. When providing travel health advice, it is important to assess individuals who are at greater risk and then provide tailored preventive advice.
Physiological changes associated with ageing
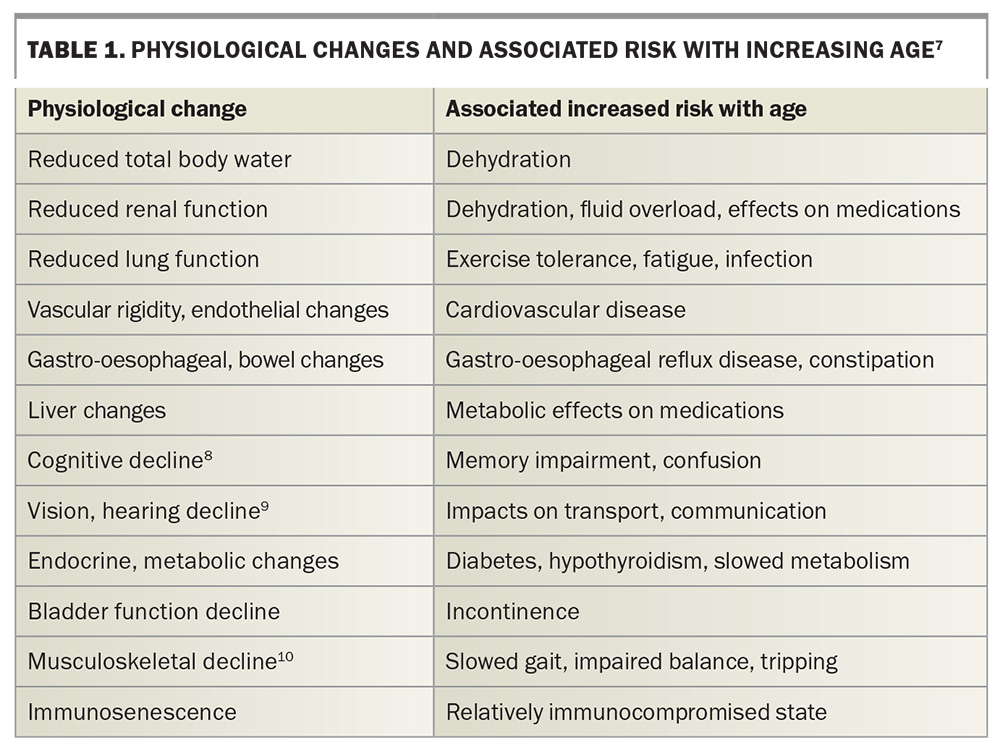
Many normal physiological changes occur with age (Table 1).7-10 For example, body tissues become less elastic and organ functions, including immune response and exercise tolerance, decrease. These changes can lead to varying degrees of acute or chronic disease, necessitating appropriate management. Immunosenescence refers to the gradual decline in immune function with age, increasing susceptibility to infections, autoimmune disease and cancer.
Travellers with chronic disease, especially if poorly controlled, are at highest risk, regardless of age.11 Conditions that are stable, such as well-controlled diabetes, mild-to-moderate ischaemic heart disease or chronic obstructive pulmonary disease, are unlikely to present issues during travel. However, risks can be mitigated with appropriate advice.
Assessing fitness for travel
Travellers should be encouraged to undergo a comprehensive medical examination with their GP prior to travel. This should include a medication review and an assessment of general fitness for the intended journey.
For strenuous activities, such as trekking, it is advisable to exclude pre-existing anaemia, cardiovascular disease and respiratory disease by tests such as a full blood examination, exercise echocardiography or thallium scan, spirometry and oxygen saturation measurement. For more leisurely travel, such as cruises or luxury safaris, a general assessment, such as the ability to climb two flights of stairs without angina or undue shortness of breath, may be sufficient.12,13
Advancements in accessibility, including wheelchair access and portable oxygen, have made travel very realistic for many travellers with severe illness. Each case should be considered individually, discussing relative risks with the traveller to enable them to make informed decisions. For more information, see: https://www.disabled-world.com/travel/.
Managing hot climates and dehydration
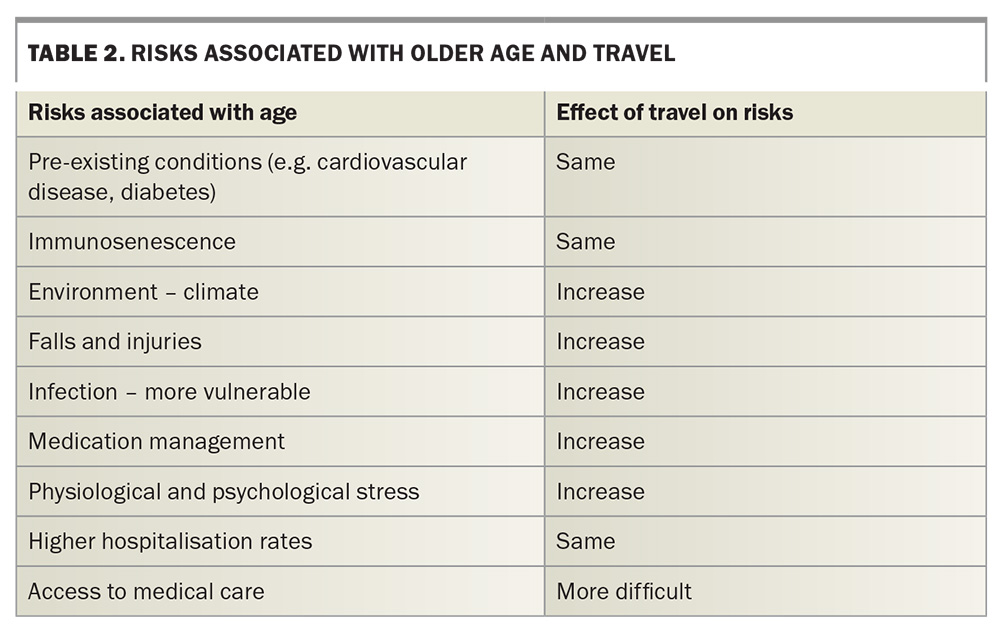
Partly due to impaired thermoregulation, older travellers are more prone to dehydration in hot climates, especially those with obesity or cardiovascular disease or taking certain medications. Reduced fluid intake to avoid having to look for a toilet can exacerbate this issue. Other considerations are included in Table 2.14
Preventive measures include avoiding excessive sun exposure and strenuous activity, planning for frequent rests, accessing air-conditioned rooms, ensuring adequate fluid intake, wearing loose clothing, and taking cool baths and showers.
Traveller’s diarrhoea poses additional risks because of the increased susceptibility to dehydration and electrolyte imbalance.15 Early attention to self-treatment with oral rehydration solutions, antidiarrhoeal agents and antibiotics, if appropriate, should be encouraged by providing the traveller with clearly written advice.
Constipation is a frequent problem at all ages, but worse with dehydration and immobility as with prolonged travel. An appropriate medication should be carried in the first-aid kit.
Considerations for cool climates
Older individuals have increased sensitivity to hypothermia in cold climates. Preventive advice includes wearing layered clothing and protecting the head and extremities.
In-flight risk factors
The jury is still out on absolute proof of air travel per se being a cause of thromboembolism. However, cabin-related risk factors include immobilisation, cramped position, insufficient fluid intake, low humidity and hypoxia. Most of these can be prevented with the appropriate advice, including regular exercise, calf exercises, support stockings and anticoagulant therapy for high-risk individuals.
Evidence from studies
A large study compared 7034 travellers aged 60 years or older with 56,042 travellers aged 18 to 45 years.3 Findings indicated a higher risk of lower respiratory tract infection, high-altitude pulmonary oedema, venous thromboembolism, arthropod bites, severe malaria, rickettsiosis, peptic ulcers, gastro-oesophageal reflux disease, trauma and injuries, urinary tract infections, heart disease and death among older travellers. Conversely, they had a lower risk of diarrhoea, upper respiratory tract infections, influenza-like illnesses, malaria, dengue, sexually transmitted infections and schistosomiasis. However, if affected, older travellers faced a higher risk of complications and hospitalisation.
A prospective analysis of 477 older Dutch travellers identified predictors for an increased risk of travel-related morbidity, including a high number of comorbid conditions, extensive travel experience, longer travel duration, multiple daily medications, destinations to northern Africa or South-East and East Asia, and use of phones and social media.16 Notably, exacerbations of pre-existing illness were rare and, importantly, age was not identified as an independent risk factor for morbidity. Similarly, another study showed mortality ratios across age groups to be similar, with deaths mainly related to injuries, notably drowning.4
Vaccinations
All travellers should be up to date with routine vaccinations as per current Australian NHMRC guidelines (Box 2).17
Other vaccines may be recommended depending on risk or legally required. Individuals born before 1966 are presumed to have natural immunity to highly contagious childhood diseases; therefore, routine measles, mumps and rubella vaccination or serological testing is generally not required for this group. For those who have had clinical varicella or positive serology, consider herpes zoster vaccination.
Hepatitis B vaccination was not routinely administered until the 1980s; therefore, most older individuals will lack immunity. Vaccination is recommended because of inadvertent exposure to body fluids, such as during emergency dental work, injury or sexual contact. Hepatitis A immunity is common in those born before the introduction of universal water treatment in 1945; however, serology or vaccination should still be considered.
A three-dose rabies vaccination course over four weeks has been shown to be effective in older travellers, with positive serology sustained for many years.18
Assessing for significant immunosuppression is crucial, as it contraindicates the use of live viral vaccines. This is particularly relevant for yellow fever vaccination, where the risks of vaccination need to be weighed against the risk of disease. According to current WHO guidelines, age over 60 years is considered a precaution, rather than a contraindication, because of the potential risk of yellow fever vaccine-associated neurotropic or viscerotropic disease. Notably, one study found that adverse events following immunisation were less common in older adults and extremely rare in those who had tolerated a previous dose without adverse events.19 If the yellow fever vaccine has been administered in the past to an individual with normal immunity, a subsequent dose is generally not required.20 A detailed discussion of risks versus benefits is essential if there is a medical risk at the destination or if certification may be needed for future travel. Otherwise, a correctly completed waiver certificate can be provided to the traveller.
Medications
Older travellers often have high medication adherence, but are more susceptible to side effects, particularly from anticholinergics (e.g. most antimotion sickness medications) and psychotropics (e.g. sleeping tablets and opioids). Potential side effects should be discussed with travellers in advance, with advice to trial the medication at home before travel and to use the lowest effective dose for the shortest possible duration.
Malaria prophylaxis has shown no difference in efficacy or adverse reactions in older travellers compared with younger travellers.21 However, emphasis should be placed on strategies for insect avoidance, including the use of insect repellents (DEET 30 to 40% or picaridin 20%), permethrin-impregnated clothing and physical barriers (such as bed nets and protective clothing).
A comprehensive review of all medications intended for use during travel is prudent. This includes assessing the necessity of each drug and considering dose reduction, timing adjustments or possible discontinuation. Travellers should also be advised to carry spare medication in a separate bag. They should be made aware of the risk associated with different formulations or dosages abroad, the potential unavailability of equivalent medications overseas and the risk of counterfeit medications in some countries. Information on the use of restricted medications in specific destinations is available on the International Narcotics Control Board website (see: https://www.incb.org/incb/en/travellers/country-regulations.html).
Benefits of travel
Several benefits of travel for older adults have been described, including improvement in physical and mental health, as well as enhanced overall wellbeing.22 Travellers often report enjoyment from cultural and historical experiences, as well as strengthened social and family connections. Emerging studies are now documenting these positive outcomes. For example, the experience of travel and the number of trips taken have been associated with a significantly reduced risk of mortality in older adults.5 Additionally, tourism has been linked to a lower all-cause mortality rate (13.7 vs 5.24 per 100 person-years), with a relative risk of 0.38 (95% confidence interval: 0.33–0.44; n = 9520).6 Similarly, a Dutch study found that despite common travel-related illnesses and injuries, older travellers reported improved self-perceived health following travel.16
Conclusion
As GPs, our role is to provide medical information that is tailored to each traveller (Box 3). By addressing the considerations outlined above and helping patients avoid common risks, we can greatly increase the likelihood that older travellers enjoy safe and memorable experiences. To quote L Visser, ‘The older traveller can still climb mountains, it’s just their definition of mountains may change considerably’.23. MT
COMPETING INTERESTS: Dr Cohen has received financial support for provision of and attendance at educational events from Sanofi and CSL Seqirus.
References
1. Australian Institute of Health and Welfare. Older Australians: demographic profile [Internet]. Canberra: AIHW; 2023 [cited 2025 Jun 30]. Available online at: https://www.aihw.gov.au/reports/older-people/older-australians/contents/demographic-profile (accessed July 2025).
2. Low LF. Confronting ageing: the talk Australia has to have [Internet]. Sydney: University of Sydney; 2023 Oct 9 [cited 2025 Jun 30]. Available online at: https://www.sydney.edu.au/news-opinion/news/2023/10/09/confronting-ageing-the-talk-australia-has-to-have.html (accessed July 2025).
3. Gautret P, Gaudart J, Leder K, et al. Travel-associated illness in older adults (>60 y). J Travel Med 2012; 19: 169-177.
4. Wyler BA, Young HM, Hargarten SW, et al. Risk of deaths due to injuries in travellers: a systematic review. J Travel Med 2022; 29: taac074.
5. Qiao G, Ding L, Xiang K, et al. Understanding the value of tourism to seniors’ health and positive aging. Int J Environ Res Public Health 2022; 19: 1476.
6. Du M, Tao L, Liu M, et al. Tourism experiences and the lower risk of mortality in the Chinese elderly: a national cohort study. BMC Public Health 2021; 21: 996.
7. Lee TK, Hutter JN, Masel J, et al. Guidelines for the prevention of travel-associated illness in older adults. Trop Dis Travel Med Vaccines 2017; 3: 10.
8. Jafari Z, Kolb BE, Mohajerani MH, et al. Age-related hearing loss and tinnitus, dementia risk, and auditory amplification outcomes. Ageing Res Rev 2019; 56: 100963.
9. Torresi J, McGuinness SL, Leder K, et al. Travellers with special needs. In: Manual of travel medicine. 4th ed. Cham: Springer; 2019. pp. 297-376.
10. King M, Lipsky MS. Clinical implications of aging. Dis Mon 2015; 61: 467-474.
11. Barnett K, Mercer SW, Norbury M, et al. Epidemiology of multimorbidity and implications for health care, research, and medical education: a cross-sectional study. Lancet 2012; 380: 37-43.
12. Hammadah M, Kindya BR, Allard-Ratick MP, et al. Navigating air travel and cardiovascular concerns: is the sky the limit? Clin Cardiol 2017; 40: 660-666.
13. Smith D, Toff W, Joy M, et al. Fitness to fly for passengers with cardiovascular disease. Heart 2010; 96(Suppl 2): 1-16.
14. Cohen J. The Traveller’s Pocket Medical Guide and International Certificate of Vaccination or Prophylaxis. 13th ed. Melbourne: Cohen Publications; 2023.
15. Yamakawa M, Sasai M, Kasai Y, et al. Diarrhea and related factors among passengers on world cruises departing from Japan. Travel Med Infect Dis 2018; 23: 56-63.
16. Vlot JA, Vive MGD, Brockhoff HJ, et al. Predicting morbidity in older travellers during a short-term stay in the tropics: the ELDEST study. J Travel Med 2021; 28: taaa216.
17. Australian Government Department of Health and Aged Care. Australian Immunisation Handbook. Canberra, 2022. Available online at: https://immunisationhandbook. health.gov.au (accessed July 2025).
18. Furuya-Kanamori L, Ramsey L, Lau CL, et al. Intradermal rabies pre-exposure vaccination schedules in older travellers: comparison of immunogenicity post-primary course and post-booster. J Travel Med 2020; 27: taaa006.
19. Tanizaki R, Ujiie M, Hori N, et al. Comparative study of adverse events after yellow fever vaccination between elderly and non-elderly travellers: questionnaire survey in Japan over a 1-year period. J Travel Med 2016; 23: taw012.
20. Rosenstein MD, de Visser AW, Visser LG, et al. Long-term immunity after a single yellow fever vaccination in travelers vaccinated at 60 years or older: a 10-year follow-up study. J Travel Med 2021; 28: taab126.
21. Lewis J, Gregorian T, Portillo I, et al. Drug interactions with antimalarial medications in older travelers: a clinical guide. J Travel Med 2020; 27: taz089.
22. Flaherty GF, Steffen R, Leder K, et al. Towards travel therapy: addressing the health benefits of international travel. J Travel Med 2024; taae091.
23. Visser L. The older traveller. In: SASTM Conference Proceedings. South African Society of Travel Medicine; 2016.
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.