Metabolic and bariatric surgery: a vital and underutilised resource in Australia
Metabolic and bariatric surgery remains the most effective treatment for severe obesity and obesity-related disease. Surgery is low risk and cost effective. Despite this, it remains underutilised in Australia, especially in the public sector.
- Metabolic and bariatric surgery remains the gold standard for the management of obesity and obesity-related diseases, comparing favourably with lifestyle and medical interventions.
- Metabolic and bariatric surgery is low risk and durable, with long-term studies showing sustained weight loss and disease control.
- Patients with a body mass index of 35 kg/m² or higher, or those with a body mass index of 30 kg/m² or higher who have type 2 diabetes, should be recommended for metabolic and bariatric surgery.
- Compared with glucagon-like peptide-1 receptor agonists, which need to be taken indefinitely for sustained results, metabolic and bariatric surgery is more cost effective.
- Greater access to metabolic and bariatric surgery is needed in public hospitals, especially for people living in regional and remote areas and for Aboriginal and Torres Strait Islander people.
Obesity is a disease of excess adiposity that currently affects about one-eighth of the world’s population, with a prevalence that has doubled over the past three decades.1 In Australia, it is now the leading contributor to disease and death, having overtaken tobacco use since 2024.2 Obesity is linked to more than 40 diseases, including type 2 diabetes (T2DM), ischaemic heart disease, metabolic dysfunction-associated fatty liver disease, obstructive sleep apnoea, gastro-oesophageal reflux disease, degenerative and crystalline arthropathy, infertility, mental illness and a wide array of cancers. The economic effects are profound, with obesity and its direct sequelae costing Australia $11.8 billion in 2018, and this is estimated to balloon out to $87.7 billion by 2032.3
Lifestyle and dietary interventions have demonstrated limited success and sustainability, with an estimated long-term weight loss of 1 to 4%.4 Until recently, there has been an absence of efficacious pharmacologic therapies. However, with the recent rise of potent glucagon-like peptide-1 receptor agonists (GLP-1RAs), there has been a surge of interest in obesity treatment.
Indications for and barriers to metabolic and bariatric surgery
Metabolic and bariatric surgery is recommended for patients with a body mass index (BMI) of 35 kg/m² and above or for those with a BMI of 30 kg/m² and above who have T2DM. It should also be considered for patients with a BMI of 30 to 34.9 kg/m² who do not achieve substantial or sustained weight loss or improvement in comorbidities using nonsurgical methods.5 Currently in Australia, over 2.5 million people have a BMI exceeding 35 kg/m2. In 2023, fewer than 16,000 primary bariatric surgeries were performed nationwide, accounting for far less than 1% of this potentially eligible patient group.6
A significant barrier to access is the lack of public facilities offering metabolic and bariatric surgery, with less than 5% of primary metabolic and bariatric surgery procedures performed in publicly funded hospitals.6 Yet, evidence suggests the cost of surgery can be offset by reductions in the incidence and severity of obesity-related diseases, emergency department visits and hospital admissions. One study examining public bariatric surgery patients in Tasmania found a $1428 reduction in diabetes care cost per episode of care in the first year after metabolic and bariatric surgery.7 Insufficiency of public bariatric services disproportionality affects underserviced groups – Aboriginal and Torres Strait Islander people have been observed to have lower rates of access to bariatric surgery despite higher rates of obesity and its complications than the broader population.8
Common bariatric procedures
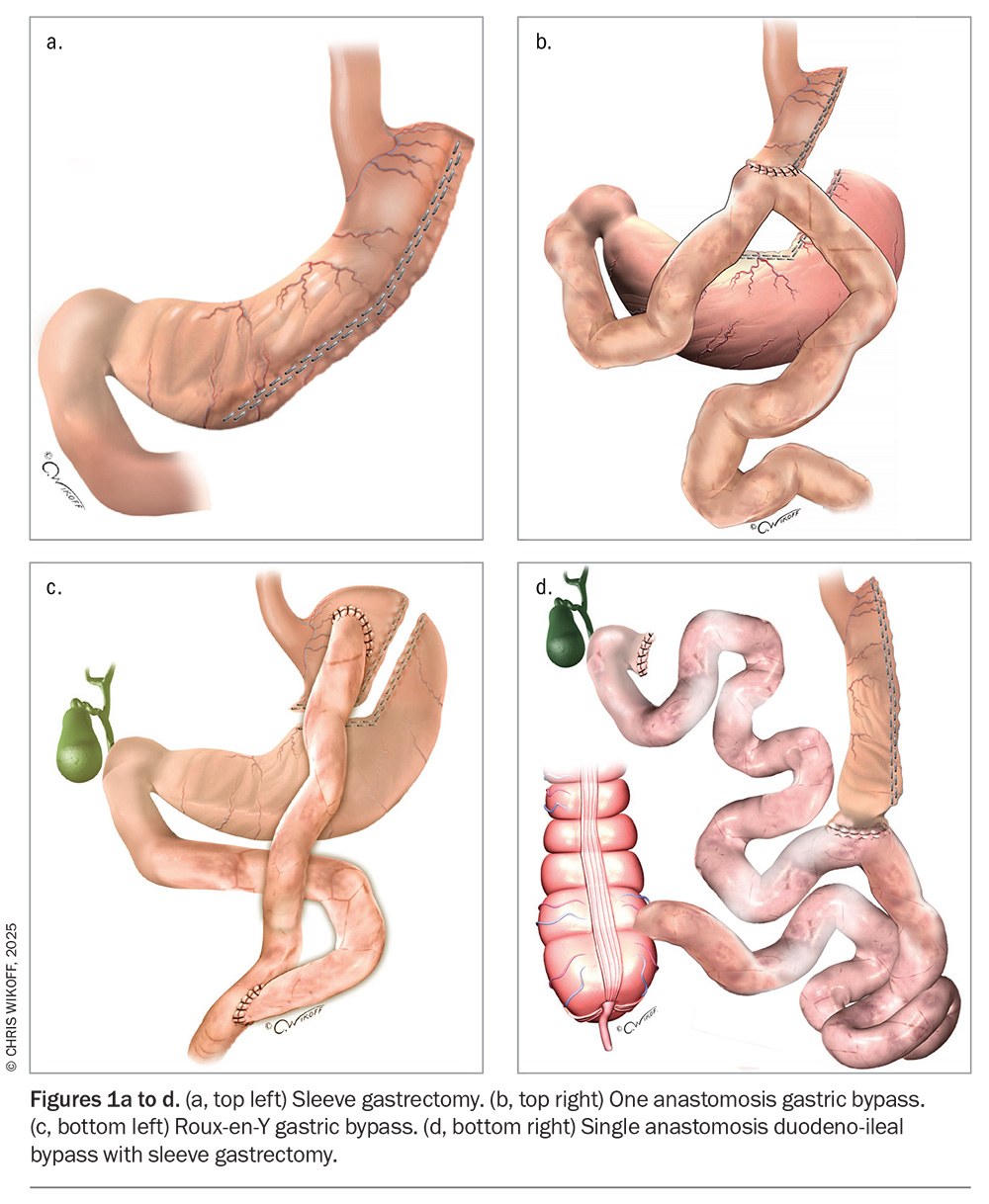
The most frequently performed metabolic and bariatric surgery procedures in Australia today are:
- sleeve gastrectomy
- one anastomosis gastric bypass
- Roux-en-Y gastric bypass
- single anastomosis duodeno-ileal bypass with sleeve gastrectomy.
These are illustrated in Figure 1a to d.
Gastric banding is rarely, if ever, performed anymore. Each procedure has a slightly different mechanism of action, with the end result being hormonally-mediated reduced hunger, increased satiation and changing food preferences.9 Selecting the most appropriate procedure for each individual patient can be complex and should take into consideration age, BMI, pre-existing gastric reflux, surgical history, medication use, comorbidities, bowel function, eating habits, smoking status, occupation, patient priorities, risk tolerance and patient preference.
Evidence for long-term efficacy
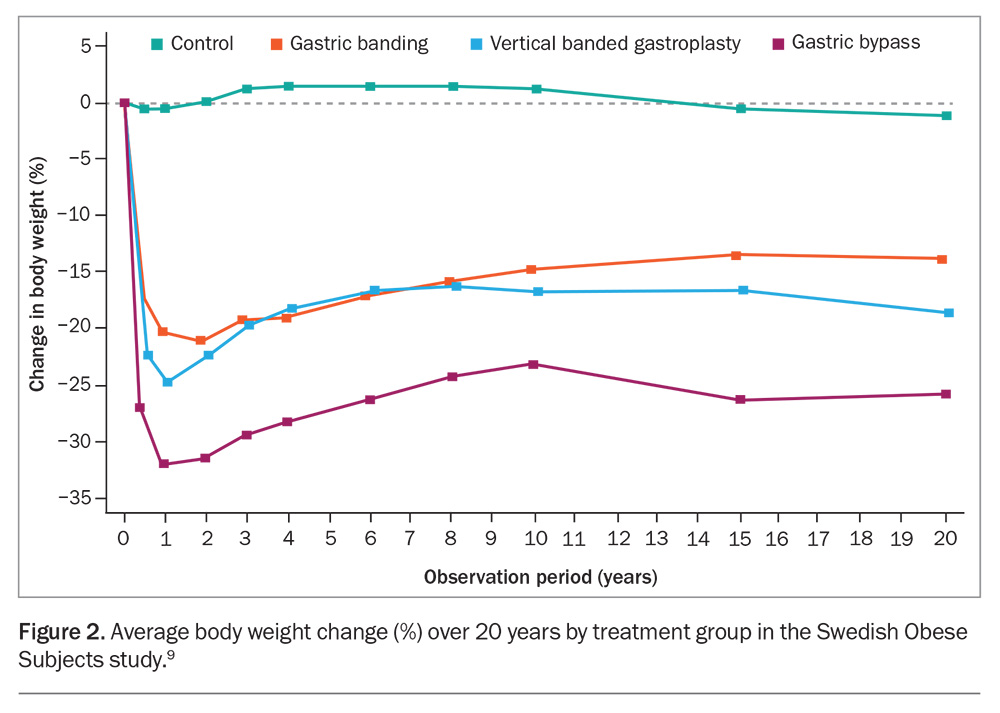
Metabolic and bariatric surgery is the most efficacious intervention in the management of obesity and its associated comorbidities. The Swedish Obese Subjects study is the most comprehensive body of evidence in this regard.10 It is an ongoing prospective controlled cohort study comparing metabolic and bariatric surgery with usual obesity care, with patients recruited from 1987 through to 2001 (Figure 2). Conventional lifestyle and behavioural interventions were not associated with a meaningful change in body habitus, whereas gastric bypass was associated with a 32% total body weight loss at one year, stabilising at a 25% body weight loss at 10 years. Secondary metabolic effects included significant reductions in the incidence of T2DM and dyslipidaemia. After over 20 years of follow-up, patients in the surgery cohort demonstrated a three-year gain in life expectancy and a 37% reduction in cancer incidence. Among patients with sustained diabetes remission, cancer incidence reduction was even greater at 60%.11
The Alliance of Randomized Trials of Medicine vs Metabolic Surgery in Type 2 Diabetes study was a multicentre pooled trial comparing surgical with medical and lifestyle interventions in patients with coexisting T2DM, with long-term follow-up, published in 2024. It found that metabolic and bariatric surgery (primarily Roux-en-Y gastric bypass and sleeve gastrectomy) resulted in significant reductions in glycated haemoglobin levels, with some patients achieving complete diabetes remission at 12-year follow-up.12 In comparison, no patients in the medical and lifestyle cohort had complete diabetes remission at 12 years.
Safety profile
Metabolic and bariatric surgery has been optimised to have one of the lowest risk profiles among major gastrointestinal surgeries, with a similar risk profile to laparoscopic cholecystectomy or appendicectomy.13 The Australian Bariatric Surgical Registry reports a 90-day adverse outcome rate (including hospital readmission or return to theatre) of 2% and a 90-day all-cause mortality rate of 0.03%.6
Nutritional monitoring and follow up
Nutritional deficiencies are the principle adverse consequence of metabolic and bariatric surgery, particularly following bypass procedures. Lifelong supplementation with bariatric-specific multivitamins is imperative, alongside annual blood test monitoring with a primary care physician (Box 1).
Vitamin B1 (thiamine) deficiency, if untreated, may cause irreversible neurological effects. This should be considered in patients who are nonadherent with multivitamins, and those with food intolerances, vomiting or excess alcohol intake. Vitamin B6 levels can be paradoxically elevated in patients taking regular multivitamins, and this can cause peripheral neuropathy. Regular bone density assessment is also an important consideration in certain patient populations, particularly postmenopausal women undergoing gastric bypass procedures.
Potential complications
Despite the excellent operative safety profile and long-term efficacy of metabolic and bariatric surgery, medium- to long-term complications can still arise, even when weight loss is successful (Box 2). GPs should be cognisant of these possibilities and refer patients back to their bariatric surgeon or another appropriate specialist should any concerns arise.
Metabolic and bariatric surgery versus incretin therapy
Comparisons with GLP-1RAs and dual glucose-dependent insulinotropic polypeptide/GLP-1RAs, collectively known as incretins, are limited because of the recent emergence of the latter in obesity treatment. A recent retrospective matched cohort study demonstrated that metabolic and bariatric surgery was associated with a significant reduction in mortality, as compared with first-generation GLP-1RAs, in patients with a diabetes duration of less than 10 years.14
High-quality randomised controlled trials have shown that semaglutide is associated with a 15 to 16% mean total weight loss15 and tirzepatide with a 21% mean total weight loss.16 In comparison, metabolic and bariatric surgery results in a greater degree of total weight loss, ranging from 20 to 40%.17,18 Although incretin therapy is sustainable over the medium-term, with most studies being limited to two years of follow-up data, long-term data on the durability of weight loss are still pending. The Semaglutide Treatment Effect in People With Obesity 4 trial, a randomised controlled trial, demonstrated an immediate reversal of weight loss effects on cessation of GLP-1RA therapy.19 At current cost levels, incretins do not yet compare favourably with metabolic and bariatric surgery.
There is a role for both the medical and surgical treatment of obesity. Incretins are increasingly used to support weight loss before surgery in patients with very high starting BMIs, helping to reduce operative risk and improve surgical eligibility. For those with weight regain after metabolic and bariatric surgery, medical therapy can support further weight loss and help maintain it. A complementary approach is likely to become more common, with both modalities balanced by a multidisciplinary team – similar to current standards for cancer care. When initially considering metabolic and bariatric surgery, it is therefore also important to choose a surgeon who is well supported and works within a multidisciplinary team. Access to regular pre- and postoperative input from bariatric nurses, dietitians, physicians and psychologists is crucial for positive outcomes and the ongoing support these patients require.
Stigma and the need for education
Stigma surrounding obesity as a disease state remains significant, both in the general public and within the healthcare system, including stigma against metabolic and bariatric surgery as a valid treatment option. People with obesity are more likely to be overlooked for employment and promotion because of perceptions of laziness or lack of self-discipline.20 Surveys of physicians have found that two-thirds consider patients with obesity to lack self-control, and that obesity is often ranked alongside alcoholism and drug addiction as conditions that elicit feelings of discomfort or dislike by clinicians.21
This is despite the evidence that obesity has a strong genetic component, with heritability estimated at 40 to 70% when there is a background obesogenic environment.22 Stigma continues to prevent many patients from accessing metabolic and bariatric surgery and deters policymakers from increasing public funding and access. It is important that doctors empower their patients by educating them on the nature of obesity and modern paradigms for its treatment.
Conclusion
Metabolic and bariatric surgery is an efficacious, low risk and cost-efficient treatment for obesity that has demonstrated sustainable reductions in body weight, the incidence of obesity-related diseases and premature mortality. Although currently underutilised, there is hope that with greater awareness and acceptance, we will be one step closer to reducing the impact of the obesity epidemic and improving the overall health of people in Australia. MT
COMPETING INTERESTS: Associate Professor Williams is a faculty member at Medtronic and Ethicon; and is the president of the Australian & New Zealand Metabolic and Obesity Surgery Society. Dr Smith and Dr Honore: None.
References
1. World Health Organization (WHO). Obesity and overweight fact sheet. Geneva: WHO; 2025. Available online at: https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight (accessed September 2025).
2. Australian Institute of Health and Welfare (AIHW). Australian Burden of Disease Study. Canberra: AIHW; 2024. Available online at: https://www.aihw.gov.au/reports/burden-of-disease/australian-burden-of-disease-study-2024/contents/about (accessed September 2025).
3. Health Ministers’ Meeting. National Obesity Strategy 2022 – 2032. Canberra: Australian Government; 2022. Available online at: https://www.health.gov.au/sites/default/files/documents/2022/03/national-obesity-strategy-2022-2032_0.pdf (accessed September 2025).
4. Sjostrom L, Larsson B, Backman L, et al. Swedish Obese Subjects (SOS): recruitment for an intervention study and a selected description of the obese state. Int J Obes Relat Metab Disord 1992; 16: 465-479.
5. Eisenberg D, Shikora SA, Aarts E, et al. 2022 American Society for Metabolic and Bariatric Surgery (ASMBS) and International Federation for the Surgery of Obesity and Metabolic Disorders (IFSO): indications for metabolic and bariatric surgery. Surg Obes Relat Dis 2022; 18: 1345-1356.
6. Australia and New Zealand Bariatric Surgery Registry. Annual Report 2023. Melbourne: Monash University; 2023. Available online at: https://www.monash.edu/__data/assets/pdf_file/0007/3757876/Bariatric_Surgery_Registry_-Annual_Report_2023.pdf (accessed September 2025).
7. Campbell JA, Hensher M, Davies D, et al. Long-term inpatient hospital utilisation and costs (2007-2008 to 2015-2016) for publicly waitlisted bariatric surgery patients in an Australian public hospital system based on Australia’s activity-based funding model. Pharmacoecon 2019; 4: 599-618.
8. Rahiri JL, Tuhoe J, MacCormick A, et al. A narrative review of bariatric surgery in Indigenous peoples. Obes Res Clin Pract 2019; 13: 1-5.
9. Miras A, le Roux CW. Mechanisms underlying weight loss after bariatric surgery. Nat Rev Gastroenterol Hepatol 2013; 10: 575-584.
10. Sjöström L. Review of the key results from the Swedish Obese Subjects (SOS) trial – a prospective controlled intervention study of bariatric surgery. J Intern Med 2013; 273: 219-234.
11. Sjöholm K, Carlsson LMS, Svensson PA, et al. Association of bariatric surgery with cancer incidence in patients with obesity and diabetes: long-term results from the Swedish Obese Subjects Study. Diabetes Care 2021; 45: 444-450.
12. Kirwan JP, Courcoulas AP, Cummings DE, et al. Diabetes remission in the Alliance of Randomized Trials of Medicine Versus Metabolic Surgery in Type 2 Diabetes (ARMMS-T2D). Diabetes Care 2022; 45: 1574-1583.
13. Clapp B, Abi Mosleh K, Glasgow AE, et al. Bariatric surgery is as safe as other common operations: an analysis of the ACS-NSQIP. Surg Obes Relat Dis 2024; 20: 515-525.
14. Dicker D, Sagy YW, Ramot Nl. Bariatric metabolic surgery vs glucagon-like peptide-1 receptor agonists and mortality. JAMA Netw Open 2024; 7: e2415392.
15. Bergmann NC, Davies MJ, Lingvay I, et al. Semaglutide for the treatment of overweight and obesity: a review. Diabetes Obes Metab 2023; 25: 18-35.
16. Jastreboff AM, Aronne LJ, Ahmad NN, et al. Tirzepatide once weekly for the treatment of obesity. N Engl J Med 2022; 387: 205-216.
17. Adams TD, Davidson LE, Litwin SE, et al. Weight and metabolic outcomes 12 years after gastric bypass. N Engl J Med 2017; 377: 1143-1155.
18. Boyle M, Mahawar K. One anastomosis gastric bypass performed with a 150-cm biliopancreatic limb delivers weight loss outcomes similar to those with a 200-cm biliopancreatic limb at 18-24 months. Obes Surg 2020; 30: 1258-1264.
19. Rubino D, Abrahamsson N, Davies M, et al. STEP 4 Investigators. Effect of continued weekly subcutaneous semaglutide vs placebo on weight loss maintenance in adults with overweight or obesity: the STEP 4 randomized clinical trial. JAMA 2021; 325: 1414-1425.
20. Westbury S, Oyebode O, van Rens T, et al. Obesity stigma: causes, consequences, and potential solutions. Curr Obes Rep 2023; 12: 10-23.
21. Puhl R, Brownell KD. Bias, discrimination, and obesity. Obes Res 2001; 9: 788-805.
22. Barsh GS, Farooqi IS, O’Rahilly S. Genetics of body-weight regulation. Nature 2000; 404: 644-651.
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.