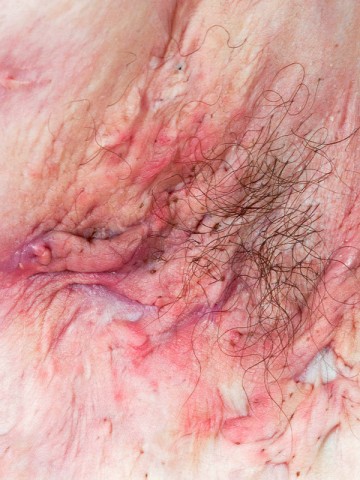
Hidradenitis suppurativa linked with anxiety and depression regardless of severity
By Melanie Hinze
A Danish study has found that people living with the chronic inflammatory skin condition hidradenitis suppurativa (HS) face a significantly higher risk of developing depression and anxiety compared with the general population, regardless of the severity of HS.
The nationwide cohort study, published in JAMA Dermatology, followed more than 10,000 patients with HS and 40,000 matched controls between 1997 and 2022. The researchers found that patients with HS were 69% more likely to develop new-onset depression and 48% more likely to experience new-onset anxiety.
The analysis also showed that these risks were consistent regardless of disease severity, as measured by type of medical treatment or number of hospitalisations for HS-related surgery. Even among patients undergoing multiple surgical procedures, the elevated risk of mental health disorders remained steady.
Associate Professor John Frew, Staff Specialist Dermatologist, at Liverpool Hospital, Sydney, and Conjoint Associate Professor at the School of Clinical Medicine, UNSW Sydney, said HS was a debilitating chronic disease and the co-occurrence of depression, anxiety and suicidality was well established and well acknowledged.
‘Given the limited treatment options and often the severe complications that come with unsuccessful surgical interventions, the results of this study suggest an increase in the risk of anxiety and depression with surgical interventions is understandable and expected,’ he said.
Although patients with HS had a greater history of depression and anxiety at baseline than controls, the study found no significant differences in risk for recurrent episodes once these conditions were established.
The study highlighted that biologic treatments did not appear to carry the same elevated risk for depression seen with other forms of therapy, although the small sample size for this group meant the results should be interpreted with caution.
‘This study highlights and concurs with previous work that HS can have a severe impact on the psychological, psychosocial and psychosexual wellbeing of our patients, and addressing these issues with patients with HS is vital for overall care,’ Associate Professor Frew said.
‘Additionally, it highlights the need for aggressive medical treatment to prevent progression to severe debilitating disease.’
The authors recommended that clinicians screen for depression and anxiety across all patients with HS, regardless of severity markers, and approach care with a multidisciplinary lens.