The first psychotic episode: navigating early-stage schizophrenia and other psychoses

Psychosis is a clinical syndrome which may signal the onset of a serious mental illness, such as schizophrenia, and impact a young person over their lifetime. Early recognition, compassionate engagement and timely referral are critical in shaping long-term outcomes and supporting recovery.
- Psychosis is a critical syndrome requiring urgent attention, referral and escalation.
- Engagement of the young person presenting with psychosis may be difficult; however, a therapeutic alliance focusing on collaborative care can yield many long-term benefits.
- Early and consistent treatment with antipsychotic medication remains the cornerstone of recovery in psychotic disorders.
- The local Mental Health Act may need to be applied in enforcing treatment if there are acute concerns for safety and a likelihood or actuality of disengagement from treatment.
- The patient’s regular GP can play a vital role in monitoring adverse effects, especially in the setting of cardiometabolic risk.
- Despite the stigma associated with schizophrenia, functional recovery is possible. Actively partnering with the patient in management, monitoring treatment response and risk of relapse enhances the patient’s likelihood of a positive outcome longitudinally.
Psychosis denotes a state in which a person’s experience of reality is markedly distorted. Core features of psychosis include hallucinations (perceptions experienced without external stimuli), delusions (fixed false beliefs) and disorganised thinking or speech. Isolated or transient psychotic symptoms may occur in states of bereavement or intoxication and are experienced in up to 17% of children and around 8% of adults.1 A psychotic disorder is diagnosed when such symptoms are sustained and impairing. The Diagnostic and Statistical Manual of Mental Disorders and International Classification of Diseases classification systems for psychotic disorders include schizophrenia spectrum disorders (schizophrenia, schizophreniform, brief psychotic disorder, delusional disorder, schizotypal personality), secondary psychoses (substance- or medication-induced), psychosis due to medical conditions and mood disorders with psychotic features.
A diagnosis of a first episode of psychosis (FEP) refers to the first time a person meets the criteria for a psychotic disorder. During the initial period of follow up for FEP, efforts ought to be made to provide a more definitive diagnosis, such as schizophreniform disorder or bipolar disorder, as this is useful in treatment planning. This article focuses on the clinical presentation of psychosis in the general practice setting and holistic treatment and care in the initial stages of schizophrenia. A companion article in a future issue of Medicine Today will discuss treatments for chronic schizophrenia.
Schizophrenia – a brief overview
Psychotic disorders manifest with symptoms across several domains and can cause significant impairment to an individual’s ability to engage with loved ones and wider society. Schizophrenia is the prototypical chronic psychotic disorder. It typically presents in late adolescence or early adulthood, with females tending towards a later presentation. A case study is introduced in Box 1. Diagnosis requires at least six months of symptoms (including at least one month of active-phase symptoms, such as hallucinations or delusions) plus functional decline. Typical clinical features include positive symptoms, such as persecutory delusions, auditory hallucinations (voices commenting or commanding) and disorganised thoughts or behaviours, as well as negative symptoms (Box 2). Of note, these negative symptoms are seen as the core pathology inherent to schizophrenia and, along with cognitive symptoms, are responsible for the severe functional deficits seen in many people with schizophrenia. Many patients also have comorbid mood or anxiety disorders. Notably, insight is often poor; patients may not recognise these experiences as abnormal.
Epidemiology and course
The lifetime prevalence of schizophrenia in high-income countries is about 0.7 to 1%. Schizophrenia is a leading cause of disability among young adults; it ranks ninth in burden and healthy life years lost (disability-adjusted life years) among men aged 25 to 44 years in Australia.2 Only about 10 to 15% of patients regain full social and occupational functioning.3 The illness course is variable; up to one-third of patients achieve sustained remission of psychotic symptoms after their first episode of acute illness. However, a larger proportion (around 50%) experience recurrent relapses, which are commonly the result of medication nonadherence, concurrent substance use (especially cannabis or stimulants) or psychosocial stress. Meanwhile, the remaining roughly 20% of patients experience a chronic, function-impairing illness.
People with schizophrenia live 25 fewer years than the general population (primarily because of the presence of cardiometabolic comorbidities and suicide).4 The economic burden of mental illness and, in particular, that of schizophrenia is significant and extends far beyond the direct costs of health care to the societal costs of support and the lost opportunity of employment.
Pathophysiology and hypotheses
Although the widely accepted biopsychosocial stress–vulnerability model frames psychosis as a product of genetic and environmental interactions, diagnosis and monitoring still rely solely on clinical judgement. The biology of psychosis is complex and not fully understood, but key theories highlight neurotransmitter changes, especially dopamine hyperactivity in mesolimbic pathways and hypoactivity in the prefrontal cortex, as drivers of positive and negative symptoms. The efficacy of dopaminergic antagonists in treating positive symptoms is linked to this basic hypothesis.
Inflammation and oxidative stress may be important in a subgroup of patients, but there are currently no therapies associated with their possible role. A small proportion of patients have an autoimmune psychosis, such as anti-N-methyl-D-aspartate (NMDA) encephalitis, which would require careful identification and specific multispecialty treatment, including input from immunology and neurology.5 By some estimations, up to 12% of patients with a FEP may test positive for serum immunoglobulin G antibodies against NMDA receptors; however, other studies have not consistently determined any difference in antibody frequency or titre compared with healthy controls.5,6
Assessment
Building rapport and trust is critical. A young adult experiencing psychotic symptoms may be frightened, confused or suspicious. Practical tips for GPs are listed in Box 3.
History, examination and investigations
An outpatient assessment must be thorough and systematic. The domains of assessment include history taking, a Mental State Examination and physical examination; these are further detailed in Box 4. Further investigations as recommended in the Royal Australian and New Zealand College of Psychiatrists guidelines for the management of schizophrenia and related disorders are listed in Box 5.7,8
Referral and risk management
A high index of suspicion should be maintained, and a low threshold for specialist referral is advised, given that a longer duration of undiagnosed and untreated psychosis correlates with poorer recovery. GPs should arrange urgent assessment by an early-psychosis or early-intervention service or psychiatrist. Outcomes for people treated by a specialist early psychosis team are improved compared with outcomes after treatment via standard services across all areas (e.g. treatment adherence, rate of hospitalisation, symptom severity and functional outcome).9 The national early psychosis guidelines recommend that a person with a suspected FEP be evaluated by specialist services within 48 hours of referral.10 A provisional diagnosis of FEP should be revised longitudinally, as the pattern of symptoms over time should provide clarification as to the definitive diagnosis.11 We acknowledge the difficulties present in many regional and rural areas in patients receiving tertiary care for early psychosis.
Risk
Urgent hospitalisation (emergency department or psychiatric unit) is indicated if there is any evidence of active suicidality (including severe depression with psychotic features), severe self-neglect (e.g. not eating or drinking), violent behaviour or homicidal ideation, or severe incapacity (e.g. catatonia). These features would likely necessitate involuntary care under the local Mental Health Act and collaboration between the GP, emergency services and a hospital-based facility. If risk is present but assessed to be lower (e.g. fleeting suicidality without plan, moderate disorganisation), urgent referral may still be appropriate. However, such cases can often be managed through outpatient care, supported by a comprehensive safety plan, close follow-up and a low threshold for escalation to hospital-level care if needed.
Community resources
Family and community supports must be involved early. Case management by a specialist team (from community mental health services) can help ensure safety and co-ordinate pharmacological and psychosocial interventions, functional assessment, housing options and care more broadly.
Treatment of early schizophrenia symptoms
Pharmacological treatments
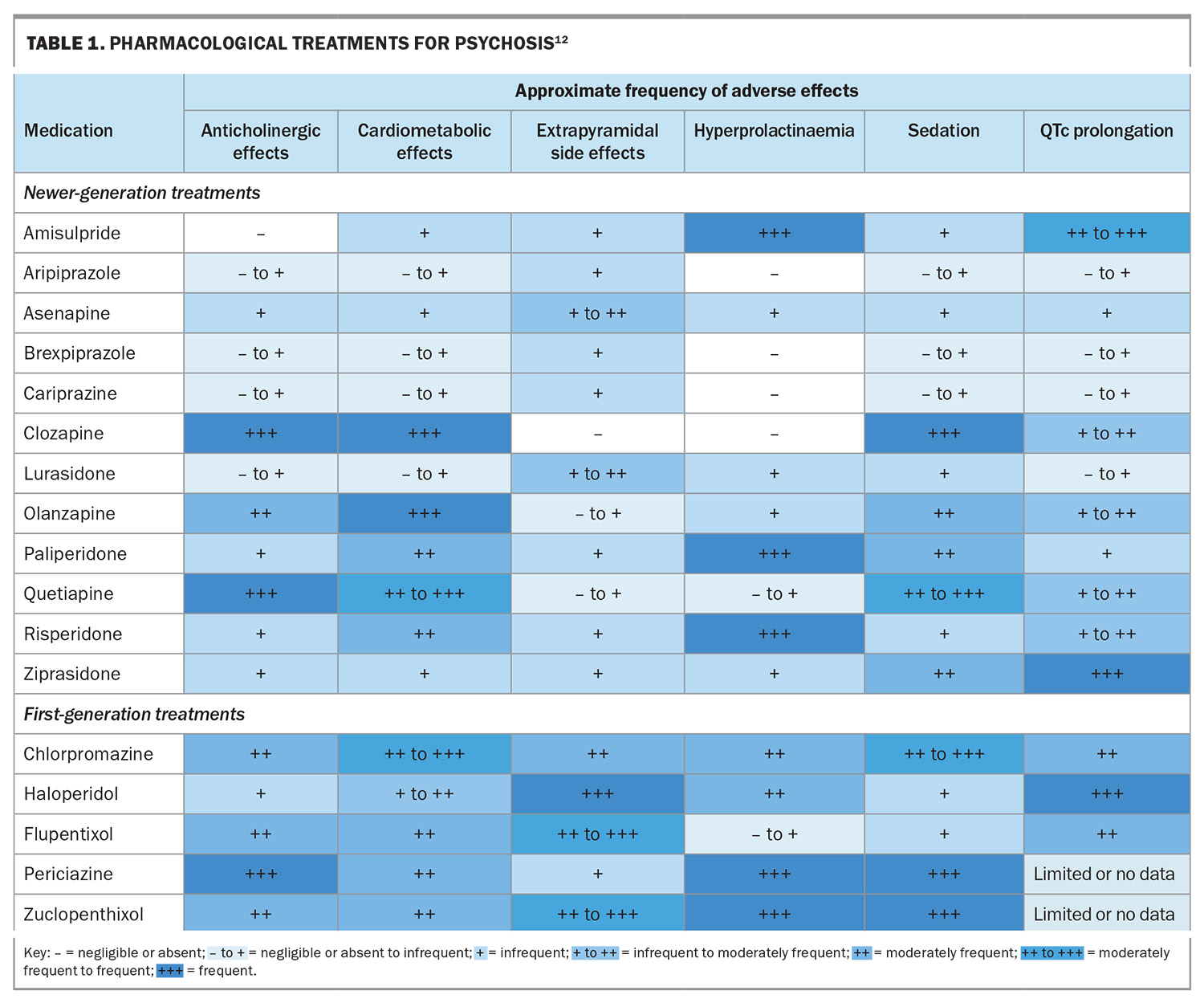
Antipsychotic medications remain the mainstay of treatment for psychosis. The newer second- or third-generation antipsychotics are first-line treatments for schizophrenia. Common oral choices in Australia include amisulpride, aripiprazole, quetiapine, risperidone and ziprasidone (Table 1).12 These are recommended by existing guidelines; however, all available antipsychotics are effective for the FEP.7 Olanzapine is not initially recommended because of the high risk of metabolic side effects. Although it is commonly prescribed in acute hospital settings for its sedating properties, long-term use is problematic for patients because of its side-effect burden, and so, stabilisation and maintenance of remission on alternative agents is preferred. Haloperidol and other first-generation drugs are seldom used as they have a higher risk of extrapyramidal side effects. Long-acting injectable formulations (e.g. aripiprazole, paliperidone and risperidone) are available and can be considered early, including in the setting of the first episode of illness (when the primary differential diagnosis is that of a schizophreniform illness or schizophrenia). Clozapine is reserved for third-line treatment because of the risk of agranulocytosis, requiring consistent monitoring of the white cell and neutrophil counts.
Dosing
Patients with a FEP are likely to be more sensitive to medication. The approach should be to start low and titrate slowly; typical effective doses for the FEP are about half of those used in chronic illness. For example, risperidone may be started at 0.5 to 1 mg/day and aripiprazole at 5 mg/day. The patient must be reassessed weekly for the treatment response and side effects. Improvement often begins after one to two weeks of treatment. If there is no clear response, the dose can be raised cautiously every one to two weeks until efficacy is evidenced on clinical assessment. Rapid escalations in dose are to be avoided, as this increases the risk of adverse effects and neuroleptic malignant syndrome. Most patients who will respond to a single agent do so within three to four weeks.13 It is important to monitor and assess for adherence, as one of the most common reasons for treatment failure is, sometimes insidiously, poor adherence to prescribed treatment.14
Duration and monitoring
After symptom remission is achieved, maintenance treatment with antipsychotic medication is recommended. Many experts advise continuing the chosen agent for at least two to five years after the FEP before tapering, given the high early relapse rates. If there is good recovery with no loss of function (i.e. the person is diagnosed with a schizophreniform disorder), then a slow reduction in antipsychotic medication over six to 12 months, while proactively monitoring for early warning signs of relapse, is almost always requested by the patient and may be considered.15 Continued symptomatology or functional decline would not support this course of action and, therefore, consistent vigilance is required of the therapeutic partnership formed between the patient, carer and clinician. The monitoring response includes regular psychiatric review (weekly initially, then monthly). Rating scales should be used if available (e.g. Clinical Global Impression) for more clarity on progression and avenues for further symptom improvement, as well as for communication around deterioration.16
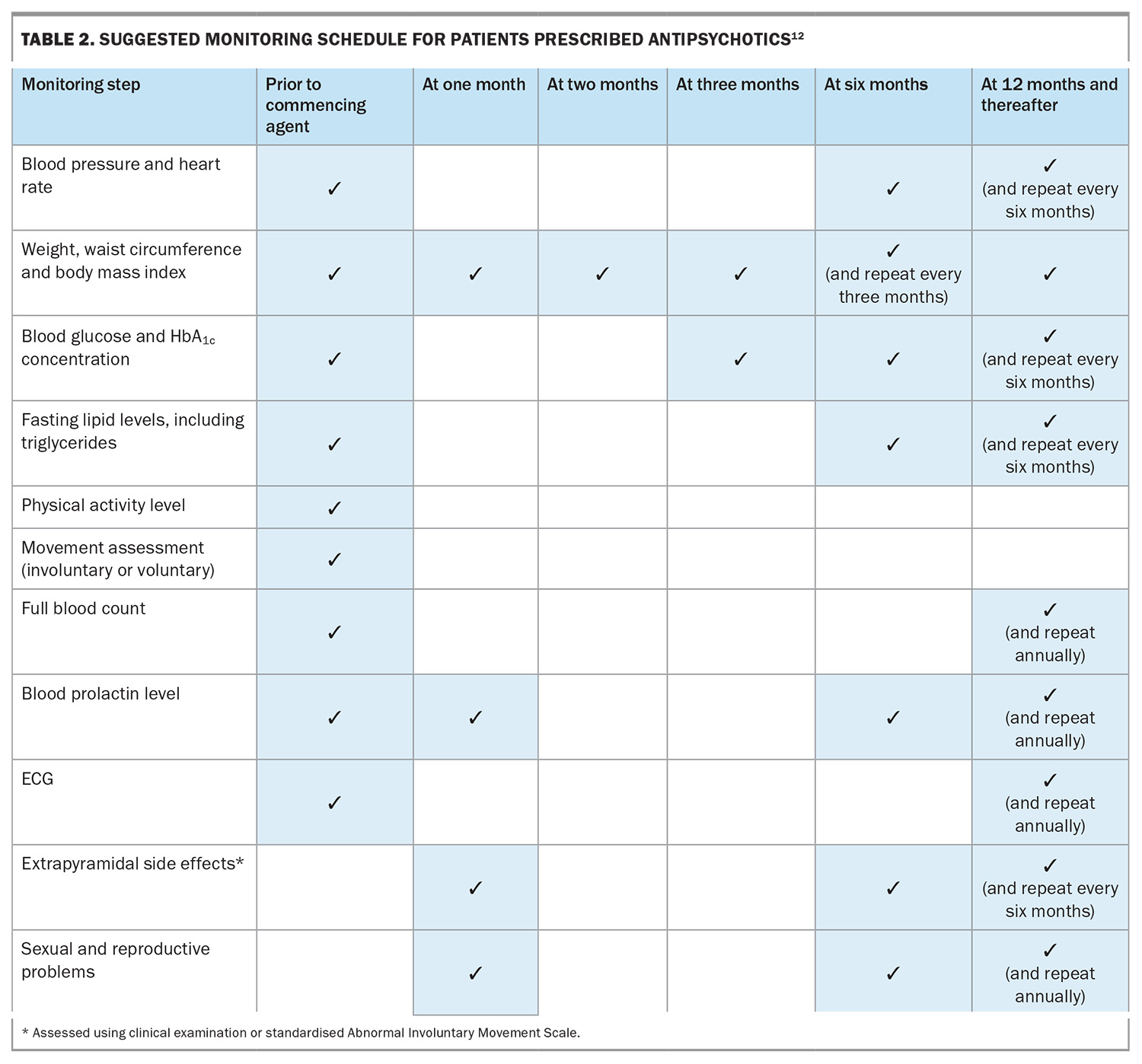
The patient must be screened frequently for side effects, including metabolic parameters (weight, body mass index, waist circumference, fasting blood glucose levels and lipid levels every three to six months) and movement disorders (Parkinsonism, dystonia or tardive dyskinesia). Serum prolactin levels need monitoring, as many antipsychotics (e.g. first-generation antipsychotics, amisulpride, paliperidone and risperidone) cause hyperprolactinaemia (inducing galactorrhoea or amenorrhea), and prolonged periods of hyperprolactinaemia increase the risk of osteoporosis and breast cancer.17,18 ECG is advised at baseline as antipsychotic drugs may prolong the QTc (especially ziprasidone, amisulpride and haloperidol), and then repeated annually or more frequently depending on the agent prescribed. Clozapine requires additional monitoring secondary to the uncommon risks of agranulocytosis, myocarditis and cardiomyopathy. An overview of the monitoring schedule is provided in Table 2.12 The case study is revisited in Box 6.
Ongoing management and developments
Considerations in pregnancy and breastfeeding
Proactive discussions with patients should be had around contraception and family planning, as well as preconception and antenatal psychotropic use. Mothers with psychotic disorders are best placed to parent their children if their illness is well managed in sustained remission and they have strong support from family and a multidisciplinary team throughout the perinatal period and beyond. For information and support, the MotherSafe (https://www.seslhd.health.nsw.gov.au/royal-hospital-for-women/services-clinics/directory/mothersafe) and MotherToBaby (https://mothertobaby.org/) resources and other equivalent resources provide information about medications in the setting of pregnancy and breastfeeding. Different antipsychotics have varying safety profiles in these settings, and use of these resources and psychiatrist involvement are recommended in such cases.
Challenges with ongoing treatment
Many patients, especially young people, struggle with medication adherence, and this is not limited to those with very poor insight. Stigma, side effects, an itinerant or chaotic lifestyle and a lack of social support are all factors that can reduce adherence. By simplifying treatment plans and timing, engaging in ongoing attempts to build and maintain rapport, offering ongoing education, utilising available family supports and using long-acting injectables proactively, the patient may improve their resilience to relapse. Other strategies to improve adherence include carefully listening to and responding to patient concerns about side effects, communicating empathetically about the management of any side effects, implementing cognitive behavioural approaches and applying motivational interviewing techniques. It is often helpful to establish a good therapeutic alliance as a basis for open and frank medication discussions. The GP Psychiatry Support Line (1800 16 17 18) may aid GPs in supporting their patients while optimising their treatment.
Barriers to care
Patients with psychosis face multiple care barriers. Stigma and lack of insight often delay help-seeking. Rural and remote regions have fewer specialist services, a lack of dedicated local early psychosis teams and long travel distances. Even in urban regions, wait times for psychiatric assessment can be lengthy.19 In relation to service structure, youth services often cease at 25 years of age, and adult services may not be youth-friendly or may be overwhelmed by case numbers, causing young adults to fall through service cracks. Cultural and linguistic barriers affect migrants and Aboriginal and Torres Strait Islander communities disproportionately. Socioeconomic disadvantage, homelessness, trauma and comorbid substance abuse further impede engagement with care along with the gap between Medicare payments and doctor’s fees. GPs can help overcome barriers by continuing to play a vigilant role and offering supportive counselling, co-ordinating with local support agencies (headspace outreach, homelessness services, drug and alcohol clinics) and continuing to advocate for the patient’s care needs if barriers are present.
Substance use
Co-occurring substance use disorders are very common (up to 40 to 60% over a lifetime). Smoking cessation must be addressed, as smoking rates are higher than 60% among people with schizophrenia, contributing to physical health decline and worsening of the cardiovascular risk profile. Cannabis and methamphetamine use can worsen psychosis or trigger relapses. Alcohol misuse may mask symptoms. GPs should screen and address substance use assertively via brief interventions, the use of nicotine replacement or other pharmacotherapy (such as varenicline or bupropion), referral of the patient to counselling or rehabilitation services and consideration of integrated dual-diagnosis programs.20 Reducing substance use can improve outcomes substantially.
Other psychiatric comorbidities
Depressive and anxiety disorders frequently co-occur. Depression is not merely a reaction to having a psychotic illness diagnosed and must be managed independently. Comorbid depression and anxiety may be treated with selective serotonin reuptake inhibitors or psychotherapy, as appropriate.
Suicide
Worryingly, patients with schizophrenia have a rate of suicide 10 times that of the general population.21 The risk is especially high in the first five years of illness. Risk factors include male gender, previous suicidal behaviour, depressive symptoms, hopelessness, recent loss, sudden cessation of medication and the FEP itself. Every young person with psychosis should be assessed for suicidal ideation and provided with a safety plan. This includes identifying warning signs (e.g. insomnia, withdrawal), coping strategies and emergency contacts. GPs should ask openly about suicidal thoughts at each visit, maintain a low threshold for urgency and involve crisis teams or hospital admission if suicidal intent is present.
Safety planning example
Patients must be encouraged and assisted to complete a safety plan that covers who to call if thoughts of suicide recur, removal of means (e.g. storing sharp objects securely), places they feel safe and scheduling of regular follow-up appointments. A web-based application (such as the Lifeline Beyond Now safety plan tool, available online at: https://www.lifeline.org.au/get-help/beyond-now/) may assist in this important endeavour. GPs should provide clear crisis contact details (e.g. Lifeline, local mental health crisis teams) and consider involving carers or family members if there is evidence of acute risk. The case study is concluded in Box 7.
Relapse prevention and nonpharmacological interventions
At this early stage in care, psychosocial interventions are primary interventions that support relapse prevention and rehospitalisation. However, all nonpharmacological interventions are important yet adjunctive in nature; effective and safe pharmacotherapy remains the primary treatment modality for schizophrenia and associated illnesses, and they are deemed essential in preventing relapse. Nonmedical interventions are listed below and will be summarised in an article by Professor Anthony Harris et al. in a future issue of Medicine Today.
- Psychoeducation: providing information about the illness, its causes, treatment and the mental health system that they are trying to navigate.
- Assertive community care: involvement of a community team to provide assertive support for the person with schizophrenia and their family improves satisfaction with services and decreases rates of relapse and rehospitalisation.
- Cognitive behavioural therapy: evidence supports its use as an adjunct to antipsychotic medication.22
- Family interventions: family-based therapy and education has strong evidence in the treatment of FEP and schizophrenia. Structured family interventions (psychoeducation, communication skills) significantly reduce relapse rates and rehospitalisation.23 GPs can play a role in encouraging family participation in treatment and can refer families to educational and carer support programs or nongovernmental organisation programs.
- Social and vocational support: early engagement in education, employment or training is crucial. Social skills training and occupational therapy can be valuable.
- Substance use disorder treatment: any substance use disorder treatment or intervention is relapse prevention. Ensure alcohol and other drugs specialists are involved if this comorbidity is detected.
- Personal relapse prevention plan: GPs can work with the patient (and family) to draft a safety and relapse prevention plan. This might include:
– identifying personal triggers (e.g. stress, sleep loss)
– early warning symptoms (e.g. mood changes, thinking speed)
– coping strategies (e.g. maintaining routine, contacting supportive friends)
– a list of emergency resources (e.g. 24-hour crisis line, nearest emergency department, trusted clinician). - Medication plan: documentation of the medication plan (name, dose and where to obtain scripts) and arranging a backup prescriber (if the regular GP is unavailable) is helpful, especially in the setting of social isolation or the cognitive impacts of severe mental illness.
Conclusion
GPs in Australia play a crucial role in the early recognition, initial assessment and ongoing management of individuals experiencing a FEP. Timely identification, accurate assessment and appropriate referral to specialist mental health services are essential for improving long-term outcomes. GPs are also vital in providing continuous care, including monitoring medication adherence and side effects, managing physical and mental health comorbidities and developing relapse prevention plans in collaboration with non-GP specialists and allied health professionals. By understanding the complexities of psychosis and the schizophrenia spectrum, addressing stigma and utilising effective engagement and assessment techniques, GPs can significantly empower their patients on their journey towards recovery. Collaboration with specialist services and a multidisciplinary approach are key to providing comprehensive and effective care for individuals experiencing this critical stage of illness. MT
COMPETING INTERESTS: Dr Shivakumar has received grant funding from the Greek Young Matrons’ Associations. Dr Cannon has received ongoing grant funding for insomnia research from the Medical Research Futures Fund; has received payment for involvement in educational events from United Clinical Australia and Pfizer; participates on the Migraine advisory board for Pfizer; and is Co-Chair of the Primary Care Council at the Australasian Sleep Association. Professor Harris has received a trial payment to the Westmead Institute of Medical Research from Alto Neuroscience; has received an investigator-initiated grant from the Balnaves Foundation; has received grants as an Investigator from the Australian Research Council, the Medical Research Futures Fund and the National Health and Medical Research Council; has received consultancy fees and participates on an advisory board for Boehringer Ingelheim; is Director of Mind Australia; and is Chair of the Research trust Fund of the Schizophrenia of New South Wales. Dr Holdenson Kimura: None.
References
1. Staines L, Healy C, Coughlan H, et al. Psychotic experiences in the general population, a review; definition, risk factors, outcomes and interventions. Psychol Med 2022; 52: 1-12.
2. Australian Institute of Health and Welfare (AIHW). Australian Burden of Disease Study: Impact and causes of illness and death in Australia 2018. Canberra: AIHW; 2021. Available online at: https://www.aihw.gov.au/reports/burden-of-disease/abds-impact-and-causes-of-illness-and-death-in-aus/summary (accessed June 2025).
3. Mayer SF, Corcoran C, Kennedy L, Leucht S, Bighelli I. Cognitive behavioural therapy added to standard care for first-episode and recent-onset psychosis. Cochrane Database Syst Rev 2024; 3(3): CD015331.
4. Kritharides L, Chow V, Lambert TJ. Cardiovascular disease in patients with schizophrenia. Med J Aust 2017; 206: 91-95.
5. Pollak TA, Lennox BR, Müller S, et al. Autoimmune psychosis: an international consensus on an approach to the diagnosis and management of psychosis of suspected autoimmune origin. Lancet Psychiatry 2020; 7: 93-108.
6. Pearlman DM, Najjar S. Meta-analysis of the association between N-methyl-d-aspartate receptor antibodies and schizophrenia, schizoaffective disorder, bipolar disorder, and major depressive disorder. Schizophr Res 2014; 157: 249-258.
7. Galletly C, Castle D, Dark F, et al. Royal Australian and New Zealand College of Psychiatrists clinical practice guidelines for the management of schizophrenia and related disorders. Aust N Z J Psychiatry 2016; 50: 410-472.
8. Forbes M, Stefler D, Velakoulis D, et al. The clinical utility of structural neuroimaging in first-episode psychosis: a systematic review. Aust N Z J Psychiatry 2019; 53: 1093-1104.
9. Correll CU, Galling B, Pawar A, et al. Comparison of early intervention services vs treatment as usual for early-phase psychosis: a systematic review, meta-analysis, and meta-regression. JAMA Psychiatry 2018; 75: 555-565.
10. Early Psychosis Guidelines Writing Group and EPPIC National Support Program. Australian clinical guidelines for early psychosis, 2nd ed. Melbourne: Orygen, The National Centre of Excellence in Youth Mental Health; 2016.
11. Pelizza L, Plazzi E, Leuci E, et al. Diagnostic shift in adolescents with first episode psychosis: findings from the 2-year follow-up of the "Parma Early Psychosis" program. Soc Psychiatry Psychiatr Epidemiol 2025; 60: 375-385.
12. Therapeutic Guidelines. Psychoses. Melbourne: Therapeutic Guidelines; 2025.
13. Leucht S, Busch R, Hamann J, Kissling W, Kane JM. Early-onset hypothesis of antipsychotic drug action: a hypothesis tested, confirmed and extended. Biol Psychiatr 2005; 57: 1543-1549.
14. Pandey A, Kalita KN. Treatment-resistant schizophrenia: how far have we traveled? Front Psychiatr 2022; 13: 994425.
15. Keks N, Schwartz D, Hope J. Stopping and switching antipsychotic drugs. Aust Prescr 2019; 42: 152.
16. Busner J, Targum SD. The clinical global impressions scale: applying a research tool in clinical practice. Psychiatry (Edgmont) 2007; 4: 28-37.
17. Taipale H, Solmi M, Lähteenvuo M, Tanskanen A, Correll CU, Tiihonen J. Antipsychotic use and risk of breast cancer in women with schizophrenia: a nationwide nested case-control study in Finland. Lancet Psychiatry 2021; 8: 883-891.
18. Lally J, Sahl AB, Murphy KC, Gaughran F, Stubbs B. Serum prolactin and bone mineral density in schizophrenia: a systematic review. Clin Psychopharmacol Neurosci 2019; 17: 333-342.
19. Yang O, Zhang Y. Wait times for psychiatric specialist services in Australia. JAMA Netw Open 2025; 8: e2461947.
20. Siskind DJ, Wu BT, Wong TT, Firth J, Kisely S. Pharmacological interventions for smoking cessation among people with schizophrenia spectrum disorders: a systematic review, meta-analysis, and network meta-analysis. Lancet Psychiatry 2020; 7: 762-774.
21. Correll CU, Solmi M, Croatto G, et al. Mortality in people with schizophrenia: a systematic review and meta-analysis of relative risk and aggravating or attenuating factors. World Psychiatry 2022; 21: 248-271.
22. Bighelli I, Rodolico A, García-Mieres H, et al. Psychosocial and psychological interventions for relapse prevention in schizophrenia: a systematic review and network meta-analysis. Lancet Psychiatry 2021; 8: 969-980.
23. Camacho-Gomez M, Castellvi P. Effectiveness of family intervention for preventing relapse in first-episode psychosis until 24 months of follow-up: a systematic review with meta-analysis of randomized controlled trials. Schizophr Bull 2020; 46: 98-109.
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.