Cranial neuroimaging: incidental findings and their significance

In recent years, advances in neuroimaging have led to an increase in the detection of incidental brain abnormalities, ranging from anatomical variants to lesions requiring specialist referral. To ensure appropriate management, it is important for GPs to have a basic understanding of these common conditions.
- The detection of incidental brain findings has increased in recent years following the expanded availability of advanced neuroimaging techniques.
- Incidental findings may cause uncertainty among GPs regarding appropriate management, in addition to significant anxiety and distress for the patient and their family.
- Although many incidental findings are benign and require no specific management, others necessitate follow up with repeat neuroimaging or specialist referral, or both.
- Indications for neuroimaging in children include progressive headaches with nausea or vomiting, seizures and the presence of abnormal neurological signs.
- Common incidental brain findings include meningiomas, arachnoid cysts, pituitary cysts, pineal cysts, developmental venous anomalies, low-grade tumours and T2 hyperintensities.
- GPs play an important role in identifying when follow up or specialist referral is necessary.
Incidental findings in this article are defined as unexpected results or asymptomatic anomalies discovered through radiological investigations completed for other purposes. In modern medical practice, the use of imaging, such as CT and MRI, has become commonplace.
Advances in technology have improved the accessibility of brain imaging, leading to an increased detection of anatomical variants, benign conditions and pathological lesions. Patients are often informed about the implications of these findings and advised on subsequent management by their primary care physician. Although not an exhaustive list, this article discusses the most common incidental findings and outlines their management approaches.
Incidental findings in children
MRI is a key diagnostic tool in paediatrics, often used to investigate symptoms such as persistent headaches with nausea or vomiting, seizures or abnormal neurological signs. Owing to radiation risks, CT use in children is typically limited to the evaluation of head trauma. Incidental findings have been identified with both CT and MRI.1
Furthermore, incidental findings have been reported during screenings for other syndromes, such as metabolic disorders, or in healthy volunteers during research studies.2 Increasingly, children receive scans as part of assessments for developmental delay, autism spectrum disorder, behavioural regression or learning difficulties.3 The discovery of incidental findings during these screenings may cause anxiety among patients and practitioners about the potential implications of such findings.
Studies show that incidental findings occur in about 26% of paediatric brain MRIs.4 Most are benign and include arachnoid cysts, Chiari I malformations, pineal cysts, enlarged perivascular spaces or minor white matter changes. Only a small fraction are clinically significant or require intervention. Despite their benign nature, these findings can cause distress among families and lead to further testing, referrals and, in some cases, overtreatment.5
Ultimately, the primary care physician must determine whether the findings necessitate referral for specialist review, the urgency of such referral and the need for any additional investigations. Moreover, some of these findings might require long-term follow up or procedures that may have inherent risks. This article aims to help guide some of these conversations between primary care physicians and their patients.
Meningiomas
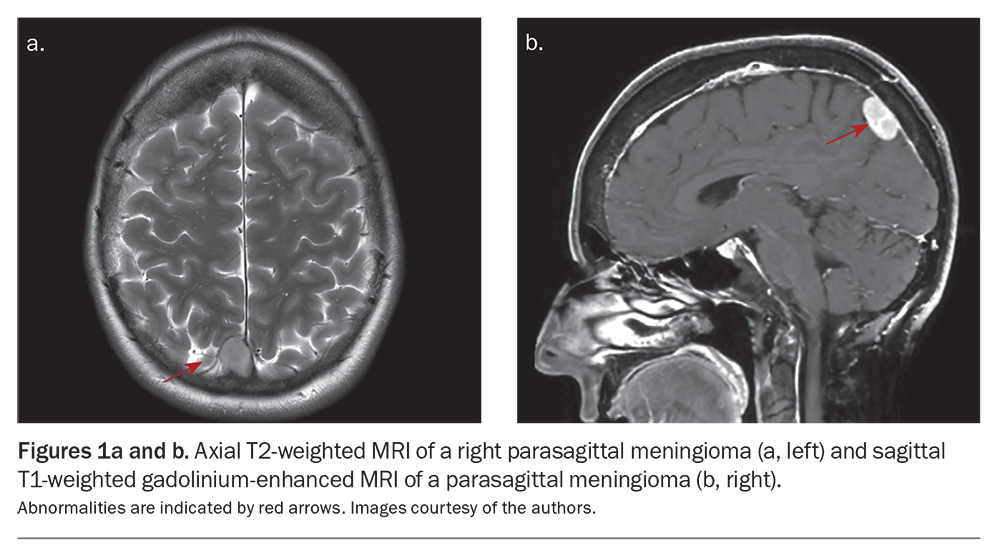
Meningiomas are one of the most common cranial imaging incidental findings in adults, occurring in about 1% of the general population.6 They are more common in women and increase in prevalence with age.7 They are often located over the convexity of the brain and may have features consistent with heavy calcification. Small lesions (<15 mm) with typical features, such as a smooth, rounded appearance with a dural tail and underlying hyperostosis of the skull, can be confidently concluded to be meningiomas (Figures 1a and b).8
In older patients, in the absence of other comorbidities such as malignancy, no further follow-up imaging may be necessary. In younger patients, or when the diagnosis is uncertain, follow-up imaging should be performed. MRI with gadolinium is preferable in these circumstances, initially at six months and then annually. If the results remain stable, the interval between imaging may be further increased and eventually ceased altogether. Larger lesions, particularly in more sensitive locations such as the posterior fossa, should be referred for a neurosurgical opinion and followed up with repeat imaging.9
Most incidental meningiomas remain stable and do not require surgical intervention, given their prevalence and typically slow growth. However, larger asymptomatic tumours may warrant surgery to prevent future neurological complications. Fortunately, the vast majority can be removed safely with minimal neurological sequelae.10
Arachnoid cysts
Arachnoid cysts are a common incidental finding on brain imaging in children and adults. These cysts arise early in development, which is often evident by the way the brain forms around the cyst and by the absence of symptoms, even though these cysts may be very large. Their size often creates anxiety and an expectation that neurosurgical treatment will be required. However, the majority require no treatment or follow up.11
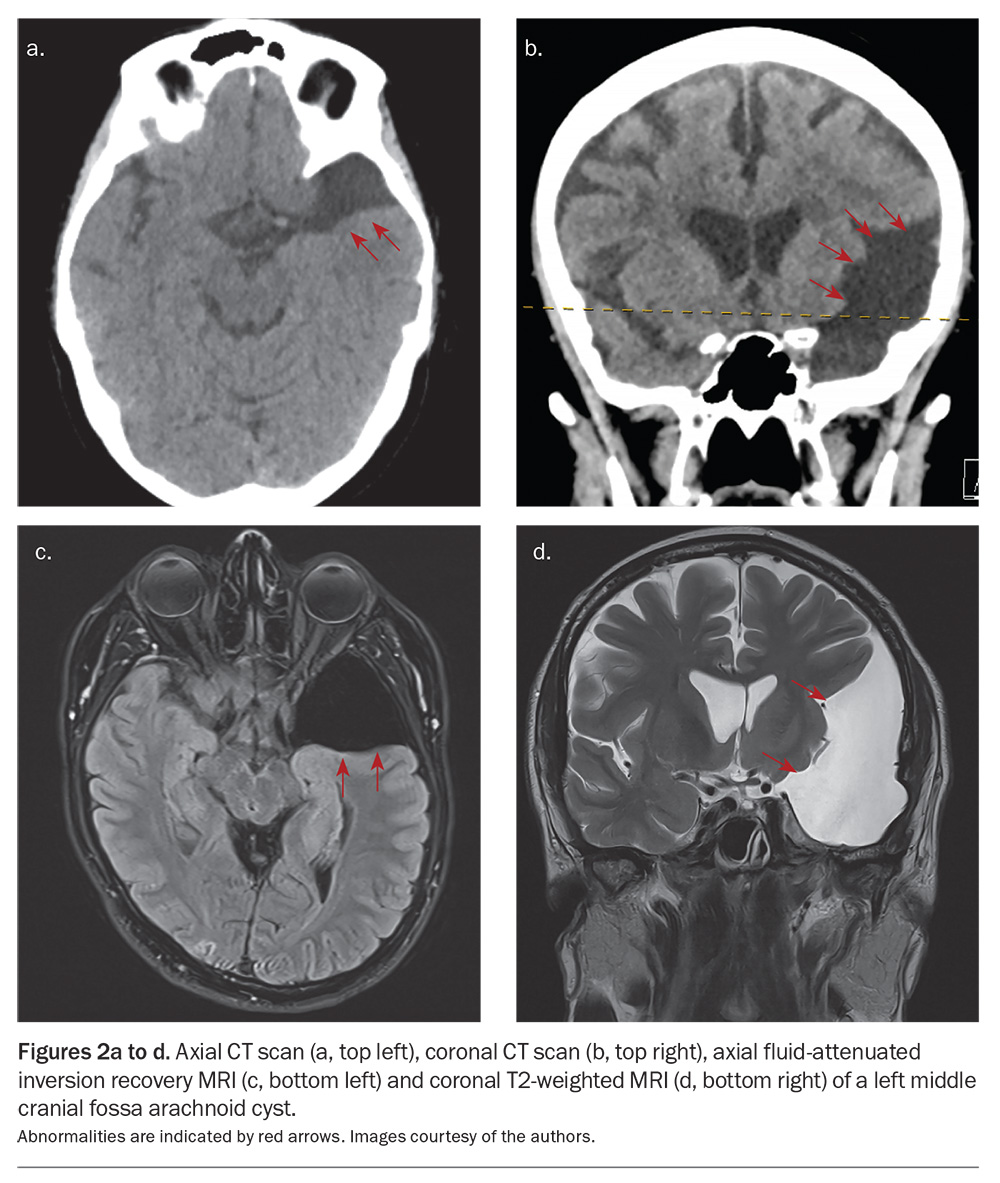
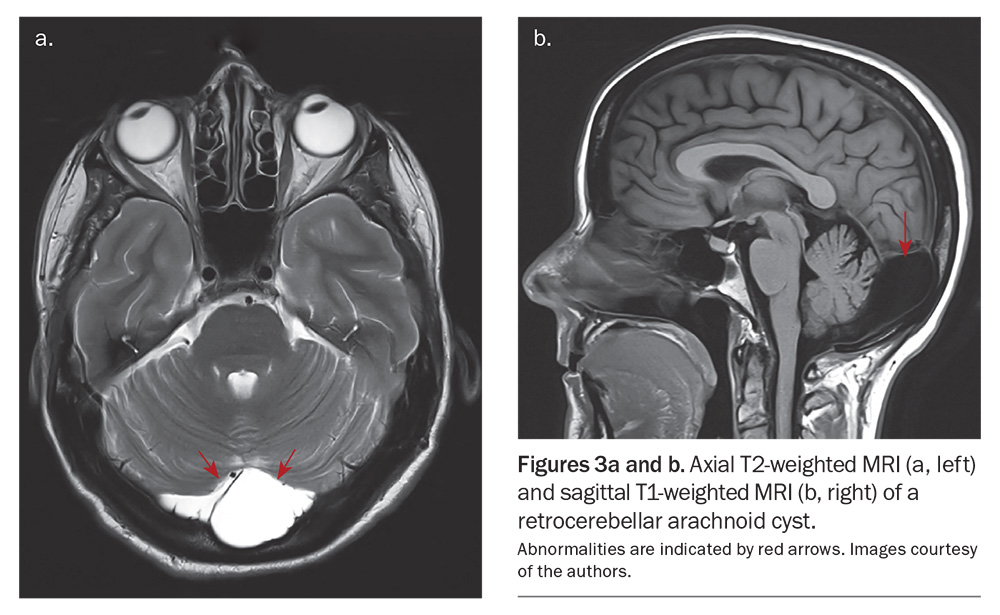
The most common location for an arachnoid cyst is the middle cranial fossa (Figures 2a to d). Cysts with significant mass effect are uncommon but may require surgical fenestration or shunting. Occasionally, patients may present with rupture of a cyst or even haemorrhage into a cyst, which is sometimes related to head trauma. Patients may be advised to avoid contact sports to reduce the risk of cyst rupture; however, the actual risk of rupture is not currently known.12 Retrocerebellar cysts are rarely symptomatic, and they seldom require treatment (Figures 3a and b).
Mega cisterna magna
Characterised by an enlarged cisterna magna, intact cerebellar vermis and the absence of hydrocephalus, mega cisterna magna (defined as a cisterna magna >10 mm) is an asymptomatic anatomical variant and an incidental finding on neuroimaging. It requires no specific follow up or management. The mega cisterna magna exerts no mass effect on the fourth ventricle or cerebellar vermis, distinguishing this condition from an arachnoid cyst.13
Pituitary lesions
The prevalence of pituitary lesions increases with age. Pituitary lesions are normally benign, with pituitary adenomas or pituitary cysts being the most common. Some lesions may be more complex, such as craniopharyngiomas. Pituitary function tests are required as further work-up of pituitary lesions. Small pituitary adenomas, which are nonfunctional and not hormone-producing, are common, as are small, simple cysts. Rathke’s cleft cysts also occur in the pituitary gland and may be incidentally identified on imaging. Endocrinological assessment, neurosurgical referral and radiological surveillance may be required for some of these lesions. Larger lesions that encroach on the optic chiasm may require closer surveillance or even surgical treatment if there is concern about the potential future impact on visual function.14
Pineal cysts
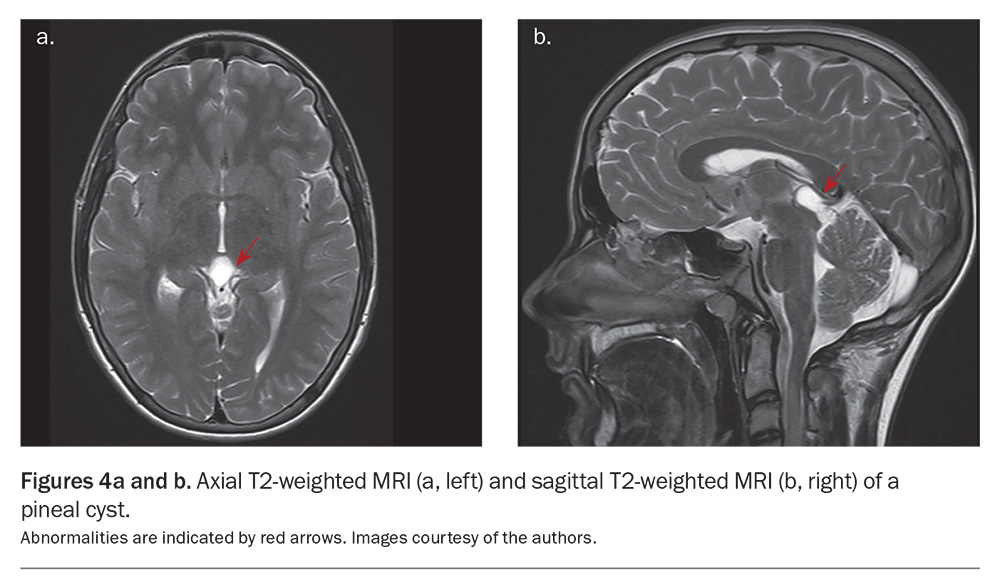
The pineal gland is largely a remnant of evolution in humans. Many different tumours can occur in the pineal region. Aggressive lesions are most often diagnosed because of symptoms, such as headaches, due to local mass effect or obstruction of the aqueduct causing hydrocephalus. Pineal cysts, however, are quite common. They are normally small simple cysts with no or minimal peripheral contrast enhancement. They do not usually require treatment. In recent years, some have argued that simple pineal cysts are a cause of headaches, but this is rarely the case. Small, simple pineal cysts seldom require ongoing radiological surveillance.15Figures 4a and b present MRI scans of a pineal cyst.
Colloid cysts of the third ventricle
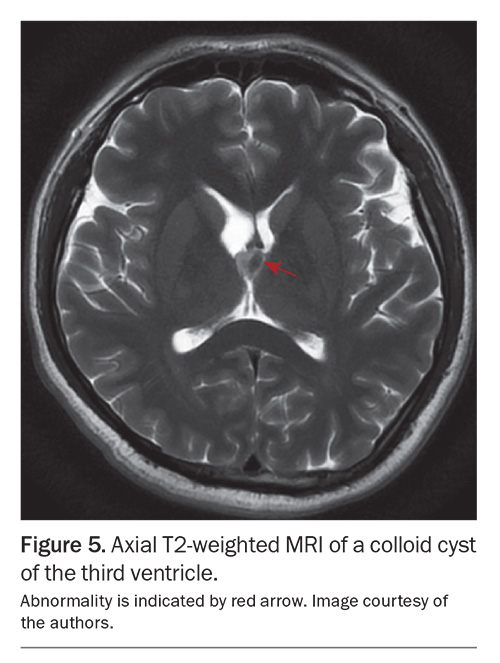
Colloid cysts of the third ventricle warrant specific consideration. These lesions are histologically benign but can cause acute obstructive hydrocephalus, leading to rapid deterioration and unexpected death. In some cases, they are identified incidentally; however, even asymptomatic lesions require neurosurgical assessment and, at a minimum, close radiological surveillance.16 A colloid cyst of the third ventricle is shown in Figure 5.
Chiari malformations
Chiari type I malformations are typically symptomatic between the ages of 25 and 45 years.17 A Chiari malformation is a condition in which the cerebellar tonsils project through the foramen magnum. This descent can obstruct the normal circulation of CSF from the cranial to the spinal subarachnoid space.18
Symptomatic Chiari malformations are most commonly associated with headaches precipitated by coughing, stooping, sneezing or straining. There are also many other symptoms attributed to Chiari malformation.
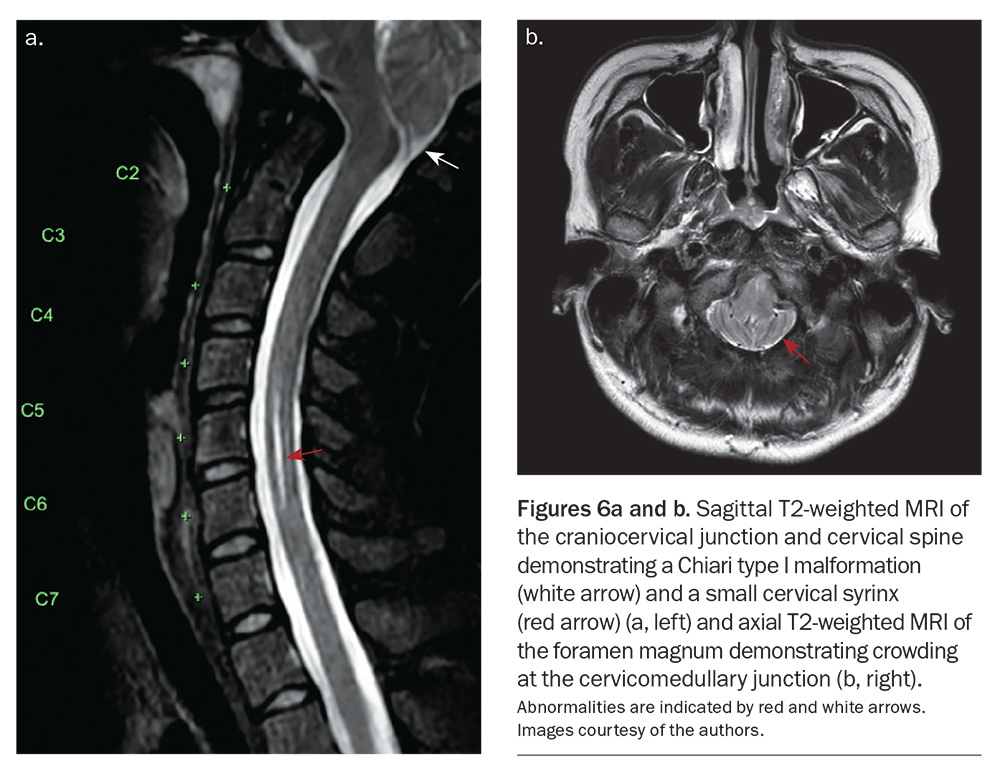
In some cases, a Chiari malformation is present, but it may be uncertain whether the symptoms prompting the scan are related to the malformation itself.19 Nonetheless, a neurosurgical opinion in these circumstances is often necessary. In the absence of other imaging findings, such as a syrinx, no treatment is usually required. Figure 6a shows a Chiari type I malformation and a small cervical syrinx, and Figure 6b shows crowding at the cervicomedullary junction of the foramen magnum.
Developmental venous anomalies
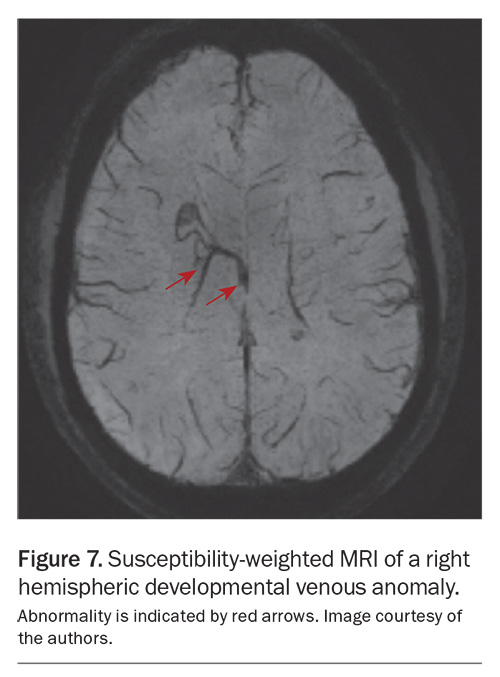
Developmental venous anomalies (DVAs), or cerebral venous angiomas, are one of the most common incidental findings on neuroimaging, with a prevalence of about 6%. DVAs are the most common cerebral vascular malformation, are usually asymptomatic and require no specific treatment. They are characterised by a number of smaller veins converging centrally into a single collecting vein, the so-called caput medusae. The majority of DVAs are supratentorial, with about 20% located in the cerebellum. These veins represent the only venous drainage pathway for the involved areas of the brain. Although the natural history is generally benign, DVAs may be associated with cerebral cavernous malformations (CCMs), increasing the risk of haemorrhage.20 These may require further neurovascular assessment and radiological surveillance. A developmental venous anomaly is shown in Figure 7.
Cerebral cavernous malformations
With a prevalence of 0.16 to 0.5%, CCMs, or cavernomas, are composed of a cluster of abnormally dilated and hyalinised capillaries, with an appearance similar to a small mulberry. About 20 to 50% of CCMs are asymptomatic and are discovered incidentally on MRI. Such lesions are generally managed conservatively with follow-up MRIs.
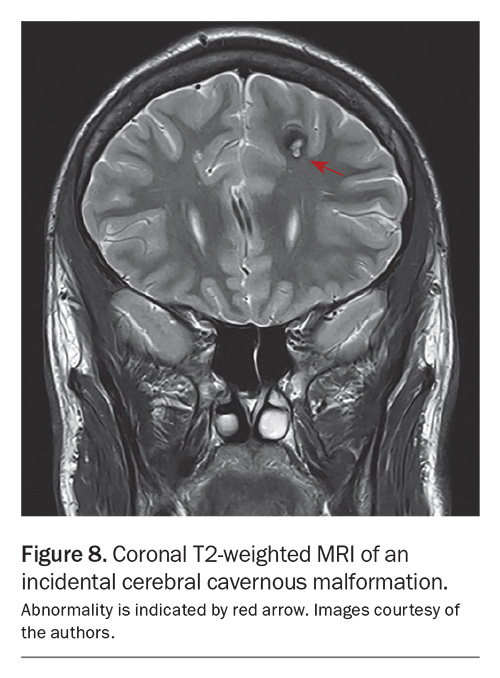
Management of symptomatic lesions (i.e. seizures, haemorrhage, focal neurological deficits) is determined by a range of factors, including surgical accessibility, eloquence of surrounding brain tissue and the presence or absence of an associated DVA.21 These will require neurosurgical review and follow up. An incidental CCM is shown in Figure 8.
Aneurysms
Aneurysms are potentially dangerous vascular lesions that are sometimes found incidentally on CT or MRI. Treatment may include craniotomy and clipping or, more commonly, endovascular treatment such as coiling. Not all aneurysms require treatment.
Management will be determined by a range of factors that balance the risk of rupture, causing subarachnoid haemorrhage, against the risks of potential treatment. Patient factors, such as age, family history and general health, and the features of the aneurysm, such as size, shape and location, are all relevant in decision-making.
Referral to a neurosurgeon with subspecialisation in vascular neurosurgery should be made to determine the appropriate management. An urgent referral should be made if there is any concern that the aneurysm is symptomatic, an example being a third nerve palsy from a posterior communicating artery aneurysm. Sentinel headaches in which there is no evidence of haemorrhage sometimes occur when aneurysms are rapidly enlarging and may herald subsequent subarachnoid haemorrhage.22
Low-grade tumours and other intra-axial lesions
Most of the lesions described above have a typical appearance, and the diagnosis can be made confidently on CT or MRI. However, a common incidental finding is a lesion within the brain that may represent low-grade tumours, such as a lower-grade glioma. MRI typically shows a lesion that is hyperintense on T2-weighted images, hypointense on T1-weighted images and without gadolinium enhancement. The imaging report may describe a list of differential diagnoses, including low-grade glioma.
Diagnosis of these lesions is important because surgery may be the best option to prevent progression in the long term. However, the lesions must be differentiated from other lesions, such as demyelinating lesions, developmental anomalies or even other tumours. As such, they can represent a diagnostic dilemma and may require further assessment with other modalities such as positron emission tomography scanning or even biopsy. An assessment and follow up with a neurosurgeon is necessitated.
In many cases, neurosurgical review will be useful for patients with incidental findings on imaging. A neurosurgical opinion can establish the importance of the finding and whether follow up is required. Most neurosurgeons have well-established follow-up protocols for these pathologies. Providing education and reassurance for the patient and their family is an important part of neurosurgical practice; however, when GPs can offer guidance on some of the more common findings, it helps mitigate unnecessary anxiety before the neurosurgical review.23
T2 hyperintensities
T2 hyperintensities are another common finding on neuroimaging with a wide differential diagnosis. They have a prevalence ranging from 11 to 21% among those who are 64 years of age, and increasing to 94% among those who are 82 years of age. White matter T2 hyperintensities are thought to result from chronic hypoperfusion secondary to small vessel disease and are more common in patients with high cardiovascular risk.24 White matter hyperintensities can be divided into deep white matter and periventricular hyperintensities; subcortical grey matter hyperintensities occur in the basal ganglia. Although often an incidental finding associated with ageing (leukoaraiosis), T2 hyperintensities, depending on the location, morphology and clinical correlation, may also be a sign of ischaemia or infarction, inflammation or demyelination (e.g. multiple sclerosis), vascular abnormalities (e.g. microangiopathies, venous infarctions) or infection (e.g. encephalitis).25
Conclusion
Advances in neuroimaging techniques and their widespread uptake in clinical practice have led to a substantial increase in the detection of incidental brain findings. Patients and their families may experience significant anxiety and distress in relation to such findings. These abnormalities may represent anatomical variants, benign lesions or true pathology that requires follow up or specific management, or both. Therefore, it is important that GPs have a basic understanding of the more common incidental findings from cranial imaging and are equipped to guide their appropriate management. MT
COMPETING INTERESTS: None.
References
1. Rogers AJ, Maher CO, Schunk JE, et al. Incidental findings in children with blunt head trauma evaluated with cranial CT scans. Pediatrics 2013; 132: e356-e363.
2. Byrne D, Fisher A, Baker L, Twomey E, Gorman KM. Yield of brain MRI in children with autism spectrum disorder. Eur J Pediatr 2023; 182: 3603-3609.
3. Biebl A, Frechinger B, Fellner CM, et al. Prospective analysis on brain magnetic resonance imaging in children. Eur J Paediatr Neurol 2015; 19: 349-353.
4. Jansen PR, Dremmen M, van den Berg A, et al. Incidental findings on brain imaging in the general pediatric population. N Engl J Med 2017; 377: 1593-1595.
5. Dangouloff-Ros V, Roux CJ, Boulouis G, et al. Incidental brain MRI findings in children: a systematic review and meta-analysis. AJNR Am J Neuroradiol 2019; 40: 1818-1823.
6. Sunny DE, Amoo M, Al Breiki M, et al. Prevalence of incidental intracranial findings on magnetic resonance imaging: a systematic review and meta-analysis. Acta Neurochir 2022; 164: 2751-2765.
7. Wiemels J, Wrensch M, Claus EB. Epidemiology and etiology of meningioma. J Neurooncol 2010; 99: 307-314.
8. Lyndon D, Lansley JA, Evanson J, Krishnan AS. Dural masses: meningiomas and their mimics. Insights Imaging 2019; 10: 11.
9. Goldbrunner R, Stavrinou P, Jenkinson MD, et al. EANO guideline on the diagnosis and management of meningiomas. Neuro Oncol 2021; 23: 1821-1834.
10. Islim AI, Millward CP, Mills SJ, et al. The management of incidental meningioma: an unresolved clinical conundrum. Neurooncol Adv 2023; 5 (Suppl 1): i26-i34.
11. Al-Holou WN, Terman S, Kilburg C, Garton HJ, Muraszko KM, Maher CO. Prevalence and natural history of arachnoid cysts in adults. J Neurosurg 2013; 118: 222-231.
12. Rogers AJ, Kuppermann N, Thelen AE, Stanley RM, Maher CO. Children with arachnoid cysts who sustain blunt head trauma: injury mechanisms and outcomes. Acad Emerg Med 2016; 23: 358-361.
13. Shekdar K. Posterior fossa malformations. Semin Ultrasound CT MR 2011; 32: 228-241.
14. Tritos NA, Miller KK. Diagnosis and management of pituitary adenomas: a review. JAMA 2023; 329: 1386-1398.
15. Jussila MP, Olsén P, Salokorpi N, Suo-Palosaari M. Follow-up of pineal cysts in children: is it necessary? Neuroradiology 2017; 59: 1265-1273.
16. Jenkinson MD, Mills S, Mallucci CL, Santarius T. Management of pineal and colloid cysts. Pract Neurol 2021; 21: 292-299.
17. Fernández AA, Guerrero AI, Martínez MI. Malformations of the craniocervical junction (Chiari type I and syringomyelia: classification, diagnosis and treatment). BMC Musculoskelet Disord 2009; 10 (Suppl 1): S1.
18. Raybaud C, Jallo GI. Chiari 1 deformity in children: etiopathogenesis and radiologic diagnosis. Handb Clin Neurol 2018; 155: 25-48.
19. Khalsa SSS, Geh N, Martin BA, et al. Morphometric and volumetric comparison of 102 children with symptomatic and asymptomatic Chiari malformation type I. J Neurosurg Pediatr 2018; 21: 65-71.
20. Linscott LL, Leach JL, Jones BV, Abruzzo TA. Developmental venous anomalies of the brain in children - imaging spectrum and update. Pediatr Radiol 2016; 46: 394-406.
21. Akers A, Al-Shahi Salman R, A Awad I, et al. Synopsis of guidelines for the clinical management of cerebral cavernous malformations: consensus recommendations based on systematic literature review by the Angioma Alliance Scientific Advisory Board Clinical Experts Panel. Neurosurgery 2017; 80: 665-680.
22. Thompson BG, Brown RD Jr, Amin-Hanjani S, et al. Guidelines for the management of patients with unruptured intracranial aneurysms: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2015; 46: 2368-2400.
23. Shah AH, Madhavan K, Heros D, et al. The management of incidental low-grade gliomas using magnetic resonance imaging: systematic review and optimal treatment paradigm. Neurosurg Focus 2011; 31: E12.
24. Debette S, Markus HS. The clinical importance of white matter hyperintensities on brain magnetic resonance imaging: systematic review and meta-analysis. BMJ 2010; 341: c3666.
25. Dhabalia R, Kashikar SV, Parihar PS, Mishra GV. Unveiling the intricacies: a comprehensive review of magnetic resonance imaging (MRI) assessment of T2-weighted hyperintensities in the neuroimaging landscape. Cureus 2024; 16: e54808.
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.