Contraception for young people: supporting informed choice

Skilled contraceptive care for young people offers a powerful opportunity to improve health outcomes and foster lifelong engagement with healthcare. It requires clinicians to build trust while assessing psychosocial circumstances, developmental stage and decision-making capacity, ensuring safety, meeting mandatory reporting obligations, respecting individual priorities and providing evidence-based information to support informed contraceptive choice.
- Adolescents and young adults are eligible for all reversible contraceptive methods, and informed choice should be supported through confidential consultations, centred on the individual needs of the young person.
- Long-acting reversible contraceptives are highly effective and should be considered first line, while respecting individual preferences and priorities.
- Clinicians must also consider and balance young people’s rights to confidentiality, capacity to consent, safety and mandatory reporting obligations.
- Noncontraceptive benefits, bleeding patterns and potential side effects are major drivers of contraceptive choice and should be discussed openly.
- Addressing misconceptions and misinformation, such as from social media, is essential to support sustained and effective contraceptive use.
Adolescence and young adulthood are typically characterised by increasing independence from parents and other caregivers. As people in these age groups learn to negotiate intimate relationships, in a context of high baseline fertility, they have an increased risk of unintended pregnancy compared with older age groups.1 In a recent national cohort of women in Australia aged 19 to 24 years, the lifetime prevalence of unintended pregnancy was 12.6%, rising to 81.0% among ever-pregnant women.2 Furthermore, unintended pregnancy is disproportionately experienced by young people experiencing sexual coercion, where they may be pressured or manipulated into unwanted sexual activity.1,2 This highlights the need to also support young people in exercising control over decisions impacting their reproductive health.2
Supporting informed contraceptive choice for adolescents and young adults can be challenging. Importantly, while addressing a young person’s concerns, healthcare providers must also balance considerations relating to developmental capacity, safety and respect for confidentiality, as well as professional and legal obligations. This article will discuss these factors before reviewing available contraceptive options and highlighting considerations particularly relevant to young people.
Young people are potentially eligible for all reversible contraceptive methods available in Australia, and evidence suggests that they want to discuss the full range of options.3 Yet, misconceptions among healthcare providers continue to limit the contraceptive choice.4 Given their high efficacy, long-acting reversible contraceptives (LARCs) are recommended as a first-line consideration. Condoms should be encouraged to prevent sexually transmitted infections (STIs). Contraceptive choice is also often influenced by a desire for noncontraceptive benefits of hormonal contraceptives, such as for the treatment of acne, dysmenorrhoea and heavy menstrual bleeding.5 It is important to address any misconceptions and concerns regarding side effects and encourage young people to return for further review if they have any questions. These consultations can be highly rewarding, as they provide an opportunity to engage positively with young people, empowering them to make informed choices to avoid unintended pregnancy and to support their wellbeing.
An approach to contraceptive consultations with young people
Confidentiality and setting the scene
In consultations with young people, establishing a safe and collaborative environment is essential. Young people may attend a consultation alone or with a friend, partner, parent or support worker. It is best practice to spend at least part of the consultation with the young person on their own, setting this expectation early with a neutral, inclusive phrase such as, ‘I always like to see my patients on their own for some of the consultation. Is that OK?’ This approach helps build trust and can support the young person should they wish to disclose any sensitive issues or concerns. It also reinforces the notion of confidential care for the young person.
Generally, young people who have capacity to consent also have a right to confidentiality regarding their medical care.6 Parents can access their children’s Medicare claim history and My Health Record for children aged younger than 14 years.7 Young people aged 15 years and older may apply for their own Medicare card, which can be used when seeing a doctor independently and ensures that rebates (where services are not bulk billed) are paid into their own nominated account.8
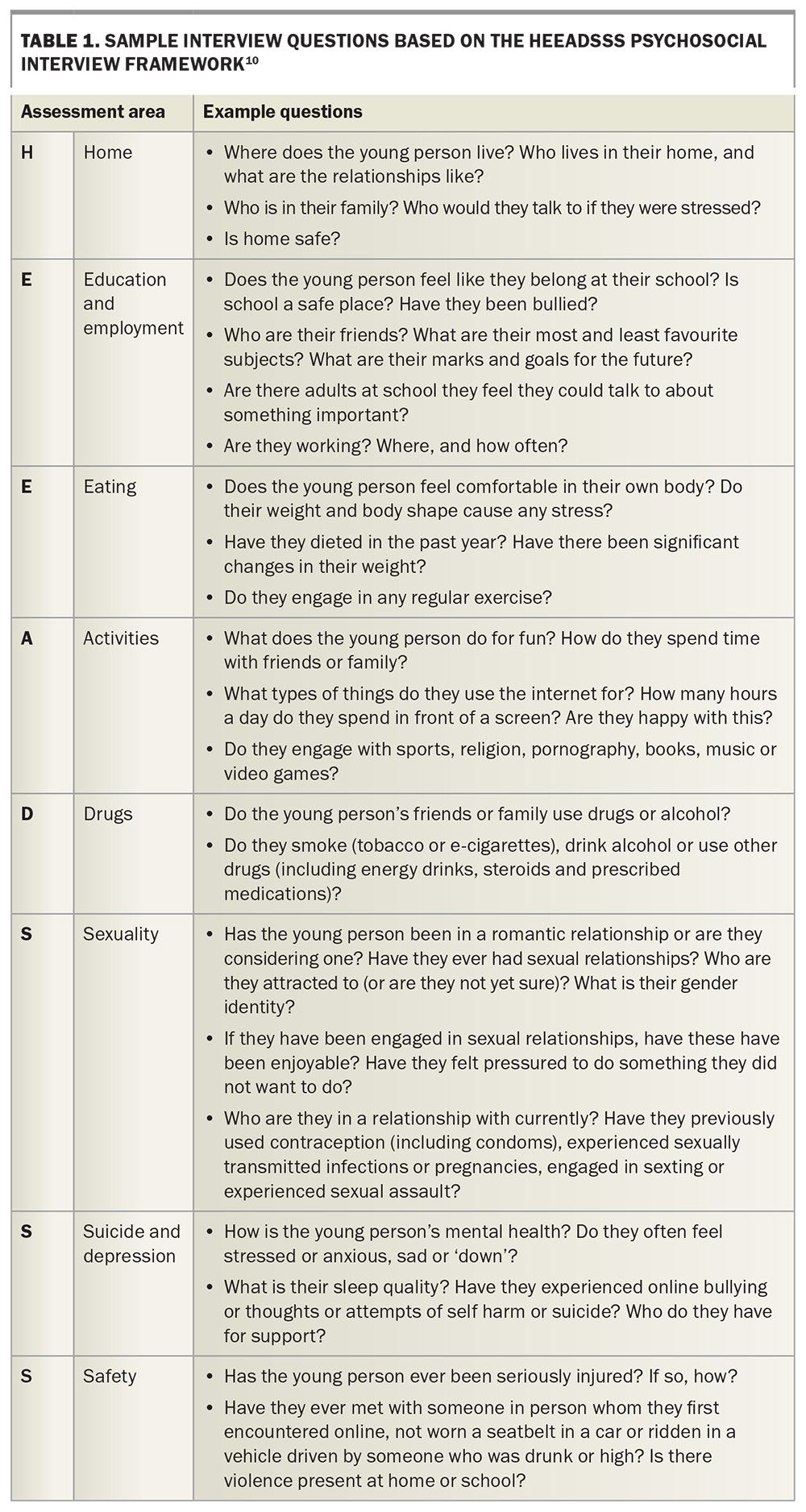
GPs must clearly explain the limits of confidentiality upfront: without their permission, their care remains private except for very limited situations, such as if they or others are at serious risk of harm. It is important to reassure the young person that you will inform them if confidentiality needs to be breached. This framing reinforces the clinician’s supportive role rather than an authoritative one. To ease into sensitive topics such as sexual health and contraception, bridging questions can be used to develop rapport, with structured psychosocial tools such as the Home, Education and employment, Eating, Activities, Drugs, Sexuality, Suicide and depression, and Safety (HEEADSSS) assessment providing a comprehensive framework for exploring a young person’s broader wellbeing (Table 1).9,10
Safety and mandatory reporting
One of the barriers experienced by healthcare professionals in providing contraceptive advice to young people involves concerns regarding their legal and professional obligations in ensuring safety. Healthcare professionals can be reassured that discussing contraception with young people does not encourage sexual activity but is part of comprehensive care for anyone who is currently, or soon to be, sexually active.
When providing care to adolescents, clinicians have a responsibility to consider risk of harm. The legal ‘age of consent’ in Australia (when a person is deemed to have capacity to consent to sexual activity) is:
- 16 years of age in:
– the Australian Capital Territory
– New South Wales
– the Northern Territory
– Queensland
– Victoria
– Western Australia - 17 years of age in:
– South Australia
– Tasmania.11
However, we know that many young people engage in sexual activity before these ages. A survey of almost 7000 students in Australia aged 14 to 18 years reported the average age of first vaginal sex as 15 years.12 Therefore, it is important to consider not only the young person’s age, but the nature of the relationship, as well as the presence of an age difference, uneven power dynamics or coercion, and whether all parties feel able to continue or stop the activity at any time. Support at home and other risks, such as neglect, are also relevant.
Mandatory reporting requirements vary across Australian states and territories, and practitioners should be familiar with legislation relevant to their area. It should be noted that filing a mandatory report does not prohibit the provision of contraception where the young person is able to consent.13 Ideally, it is best practice to inform the young person when a mandatory report needs to be filed, although this is not a legal requirement. This decision should consider the risk of disengaging the young person from the therapeutic relationship. Individual jurisdictions set out protections for mandatory reporters, including confidentiality and immunity from civil, criminal or administrative proceedings, related to the report.14
Competence to consent to treatment
Parents or caregivers are generally involved in providing consent for medical treatment in children and young people aged younger than 18 years, but young people can provide consent independently if they are deemed to be ‘Gillick competent’ or a ‘mature minor’. This is based on the Gillick case, a 1986 United Kingdom legal judgement that determined that a doctor could legally prescribe contraception to an adolescent aged younger than 16 years without their parent’s knowledge, provided the adolescent demonstrated sufficient intellectual capacity to fully understand the nature and consequences of treatment.15 This position was approved by the High Court of Australia in a case known as Marion’s case. New South Wales and South Australia have additional legislation regarding medical treatment in children that clinicians should be aware of in these jurisdictions.15,16
When providing contraceptive care to adolescents, clinicians must consider their maturity and capacity to understand the specific treatments proposed, their purpose and nature, alternatives, risks and benefits, and their broader consequences. The adolescent must also retain the information long enough to make an informed decision.17 Importantly, a minor’s capacity to consent may vary depending on the significance of the proposed treatment; for example, a 14-year-old adolescent may be deemed to have capacity to independently consent to contraception but not for major surgery.13 It is recommended that clinicians reassess and document this competence at each visit where relevant (such as for those aged younger than 16 years).18 The Fraser guidelines (which arose from the Gillick case) provide specific criteria suggested for the provision of contraception to minors without parental consent and may be utilised as a checklist to support documentation (Box 1).17,18
Factors influencing the contraceptive choice for young people
There is no one-size-fits-all approach when it comes to contraception, including for young people. A patient-centred approach must be applied, tailoring the discussion to an individual’s current concerns and needs, with regular review. Nevertheless, there are several considerations and prevailing misconceptions, which can be particularly pertinent to this age group.
Social media
The contraceptive choice for young people is often influenced by experiences of family and friends, as well as information that they may have accessed online.5 Social media has increasingly become a primary source of health information for young people, although much of this content is unreliable.19 There is also a current trend that encourages ‘natural’ methods over hormonal contraceptives and an implicit distrust of healthcare professionals.20 It is important that practitioners are aware of these alternative sources of information, so that they may understand a young person’s priorities and concerns and validate their experiences, while providing evidence-based advice and countering misinformation.
Medical eligibility
Age alone is not a limiting factor for contraceptive use, with Australian and international guidelines supporting the use of any method from menarche if there are no contraindications.21-23 Similarly, nulliparity alone should not restrict contraceptive choice.17 The United Kingdom Medical Eligibility Criteria (MEC), utilised in Australia, considers patient characteristics and pre-existing conditions to guide safe contraceptive prescribing.22 These criteria are freely available as a downloadable guideline (Box 2).22
Compared with older people, young people usually have fewer comorbidities and cardiovascular risk factors that impact their medical eligibility for contraceptives. Nevertheless, it is important to consider the MEC criteria to ensure safe options are discussed. For instance, oestrogen-containing contraceptives, such as the combined oral contraceptive pill (COCP) and vaginal ring would not be recommended in the context of a personal history of venous thromboembolism, known thrombogenic mutations or migraine with aura, which are all categorised as MEC 4.22
The contraceptive injection, depot medroxyprogesterone acetate (DMPA), is associated with a small reduction in bone mineral density during use, which usually recovers upon cessation. Given that adolescence is a critical time for attaining peak bone mass, it is recommended that DMPA is considered a second-line choice in those aged younger than 18 years (MEC 2).17
Contraceptive efficacy
Contraceptive efficacy is a key consideration for young people given their high fertility.There is evidence that unintended pregnancy is twice as likely among those aged younger than 21 years using short-acting contraceptive methods compared with those who are older and using the same methods, whereas there was no difference in risk when using LARCs.24 Therefore, it is recommended that the benefits of LARC methods are discussed with young people and considered as first-line options.18 LARC methods include copper and hormonal intrauterine devices (IUDs) and the contraceptive implant, and, given they do not require any regular action on the part of the user (e.g. remembering to take a daily pill or use a condom), they are highly effective at preventing pregnancy (in more than 99% of cases).25 The How effective is my contraception? resource from Sexual and Reproductive Health Australia (formerly Family Planning Alliance Australia) can be helpful in highlighting differences in contraceptive efficacy (available at https://srha.org.au/resour/).
Although efficacy is a very important consideration, healthcare professionals must ensure that care remains patient centred. Young people may choose less effective methods for a variety of reasons, and it has been argued that it is therefore essential to communicate openly regarding the full range of options, and provide information so that young people may optimise the efficacy of their chosen method.26
Noncontraceptive benefits
Some young people may present to discuss pregnancy prevention; however, it is not uncommon for contraception to be initiated primarily noncontraceptive benefits, such as menstrual cycle control or to manage symptoms such as heavy menstrual bleeding, dysmenorrhoea or acne.5
Changes in vaginal bleeding
Impact on vaginal bleeding patterns, such as for the management of heavy menstrual bleeding or allowing for cycle control, are significant considerations impacting the contraceptive choice for young people.5
Combined hormonal contraceptives (CHCs), including the COCP and vaginal ring, contain both oestrogen and progestogen. They lighten vaginal bleeding and have the additional advantage of cycle control and predictable withdrawal bleeding during the hormone-free interval. In addition, tailored regimens, which allow users to skip withdrawal bleeds, may be desirable for specific occasions (e.g. sporting events, examinations or school camp) or if the young woman experiences undesired symptoms during the hormone-free interval.27 With the COCP, this may include continuously taking the hormone pills or taking the hormone pills for an extended period (such as three months before taking the inactive pills and allowing a withdrawal bleed, known as tricycling). Available evidence regarding the safety of extended CHC regimens is reassuring, and off-label prescribing is supported by Australian guidelines.18,21
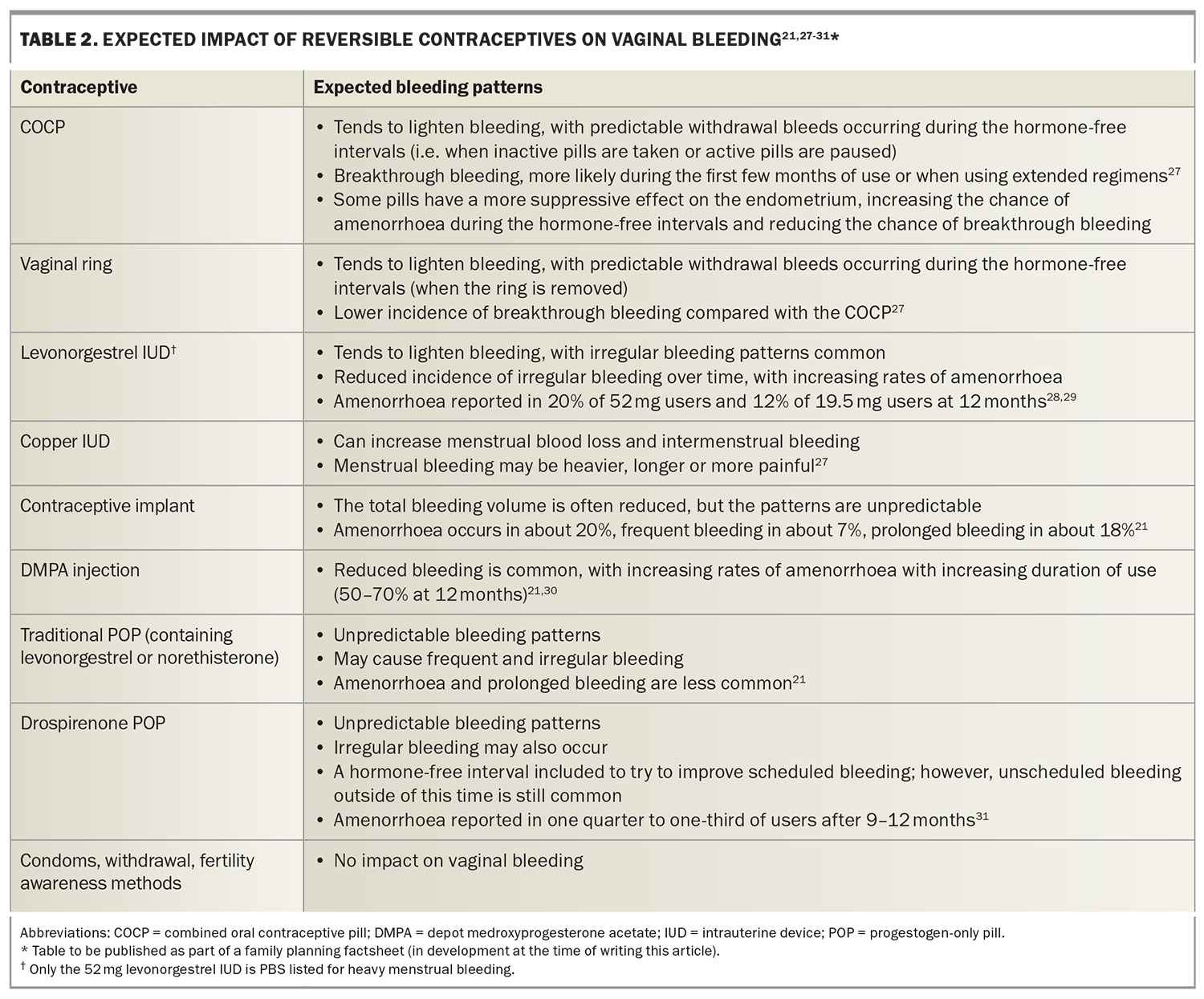
Progestogen-only contraceptives (including the contraceptive implant, hormonal IUDs, DMPA injection and drospirenone progestogen-only pill) often cause less predictable bleeding patterns, particularly during the first months of use, including unscheduled irregular bleeding or amenorrhoea. Both hormonal IUDs and DMPA tend to lighten bleeding, and, along with the drospirenone progestogen-only pill, an increasing proportion of users will experience amenorrhoea over time (Table 2).27 A clear explanation of possible bleeding patterns with hormonal contraceptives can be invaluable in improving acceptability, along with encouragement to return for review if bleeding is not tolerable.
Dysmenorrhoea treatment
Period pain that affects engagement in daily activities, such as school attendance, is common among adolescents in Australia.32 The importance of treating dysmenorrhoea has been increasingly recognised, not only to improve a young person’s wellbeing, but because of its association with an increased risk of chronic pain in adulthood.33 Along with NSAIDs, CHCs and progestogen-only contraceptives are key initial treatment options for dysmenorrhoea.21,34 Extended or continuous use of CHCs may be more effective than cyclic use, by avoiding symptoms experienced during withdrawal bleeds.34 Depending on the presentation, and certainly if there is insufficient response to initial treatments, GPs should investigate for secondary causes, such as endometriosis.34
Acne treatment
The COCP can improve acne and other symptoms of hyperandrogenism by increasing the levels of sex hormone-binding globulin, and thereby lowering levels of serum androgens.21 Although evidence is limited, the vaginal ring is also likely to improve acne.21 It is important to set expectations, as the clinical effect may not be apparent for a few months after commencement.35 Theoretically, a less androgenic or antiandrogenic progestogen (e.g. drospirenone or dienogest) may be preferable; however, all COCPs have been shown to have a beneficial effect for acne, and there is insufficient evidence for one pill over another.36 It should be noted that pills containing cyproterone acetate are TGA approved for the treatment of acne and androgenic symptoms unresponsive to other treatments; these may also provide contraception if required.37 If needed, the COCP may be safely used alongside other nonhormonal acne therapies; effective contraception is critical if using teratogenic medications, such as retinoids.38
Protection against sexually transmitted infections
External and internal condoms have a typical-use efficacy of only 79 to 88%; however, they are the only methods of contraception that also provide protection against STIs. Given sexually active young people are at an increased risk of STIs, such as chlamydia, it is important to highlight the benefits of consistent condom use and annual STI screening.39 It may also be helpful to discuss the correct use of condoms and strategies to help a young person negotiate condom use with their partner(s). Where the young person is at risk of contracting HIV infection, pre-exposure prophylaxis should be considered.40 Additionally, the ‘doxy-postexposure prophylaxis’ strategy (taking doxycycline within 72 hours of unprotected sexual activity) may benefit those at higher risk of syphilis, such as gay, bisexual or other men who have sex with men, balancing benefits against potential risks, including antibiotic resistance.41 Dual protection, where condoms are used alongside another more effective contraceptive method, is often recommended to provide both STI protection and effective contraception.
Common misconceptions and side effects
Appropriateness of intrauterine devices for young people
Despite current guidelines recommending IUDs as a first-line consideration for young people and evidence of higher satisfaction and continuation rates, less effective methods, such as contraceptive pills or condoms, are more often used in Australia.18,42-44 Misconceptions persist among healthcare providers, impacting the options offered to young people.4,5,45 Concerns include a risk of pelvic inflammatory disease in those exposed to STIs and insertion difficulty in nulliparous individuals. However, compared with the earlier IUDs, modern IUDs do not carry the same risk of pelvic infection. There remains a slight increase in risk, limited to the first three weeks after insertion; however, the overall risk is very low (<1%).27 To minimise this risk, STI screening should be offered before IUD insertion and may be performed on the day of insertion if the young person is asymptomatic. IUD insertion should be delayed in the presence of purulent cervicitis, gonorrhoea, symptomatic chlamydia infection or current pelvic inflammatory disease.27
In addition, there remains concern among some healthcare providers that IUD insertion may be technically more challenging and painful for young, nulliparous people. Although there is significant variability in the pain experienced during IUD insertion between individuals, higher pain scores have been reported for nulliparous women.27 Other factors associated with increased pain include dysmenorrhoea, greater anticipated pain, greater anxiety and negative perceptions of IUDs prior to insertion.46
Nevertheless, insertion pain is usually relatively short-lived, and there is evidence that insertion without sedation may be acceptable to young women.47 The rate of successful IUD placement on the first attempt in young women is very high (>98%) in community clinics, and previous vaginal delivery does not have a significant impact on success rates.48 Furthermore, new smaller IUDs, such as the 19.5 mg levonorgestrel IUD, may further facilitate easier, less uncomfortable insertion.49 There is limited evidence regarding the optimal analgesic choice for IUD insertion, but it is important to provide patients with information about IUD insertion-associated pain and pain management strategies (e.g. naproxen, 10% local anaesthetic spray, methoxyflurane) and ensure patients know that they can ask for the procedure to be ceased or paused at any time.46,50,51 IUD insertion under sedation is also an option, but this choice may be restricted by the accessibility of clinic locations, wait times and cost.
Concerns regarding side effects
Concerns associated with side effects, such as weight gain or impacts on mood, often impact contraceptive choice and discontinuation.5,17 These may be influenced by previous negative experiences or the perceptions and experiences of friends and family. Information accessed online may also play a role; social media influencers have been found to often promote the discontinuation of hormonal contraception and may provide incomplete information regarding nonhormonal options.52
Young people have highlighted their desire to discuss possible side effects as part of contraceptive consultations.3 It is important to take any concerns seriously, while providing information regarding available evidence and respecting individual experiences and choice. After initiating contraception, young people should also be encouraged to return at any time if they experience problems; a scheduled review after three months may help address concerns or side effects.18 Given that multiple factors may contribute to an altered mood or body weight, it can also be pertinent to respectfully explore these alongside the potential role of contraception.
Weight gain is frequently cited as a side effect of hormonal contraception, leading many young people and clinicians to believe a causal link exists. However, evidence for weight gain caused by most contraceptives is lacking. The exception is the DMPA injection, which has been associated with weight gain, particularly in those aged younger than 18 years who have a higher initial body mass index (≥30 kg/m2).53
Studying the association between hormonal contraceptives and mood is challenging, given the multiple potential confounding factors and difficulty in measuring subjective changes in mood. An often-cited large Danish cohort study found an increased relative risk of the diagnosis of depression or initial antidepressant prescription among those prescribed hormonal contraception, particularly adolescents.54 However, although this demonstrates an association, there remains insufficient evidence that hormonal contraceptives cause depression, and pre-existing depression is not a contraindication to their use.18 Indeed, for some people, the COCP may have a beneficial role in the treatment of premenstrual dysphoric disorder. It should be acknowledged that some users may experience mood changes while using contraceptives.18 A change in the contraceptive method may be considered, such as changing the progestogen or switching to a nonhormonal method. If mood changes occur during the hormone-free interval, a continuous or extended-use regimen of a CHC may be helpful.28
Cost
LARC options are cost-effective over the duration of use; however, upfront costs and challenges in finding providers trained in insertion and removal may limit their uptake among young people. Several measures have been introduced recently to address these barriers, including:
- significant uplifts in Medicare rebates for LARC procedures and bulk-billing incentives from November 202555
- the establishment of the online Australian Contraception and Abortion Primary Care Practitioner Support Network community of practice for primary care (AusCAPPS Network)56
- scholarships to boost clinician training in LARC (AUSLARC training scholarships).57
Additionally, several other contraceptive options have been added to the PBS in 2025, including the 4 mg drospirenone progestogen-only pill, COCPs (20 mcg ethinylestradiol and 3 mg drospirenone, 30 mcg ethinylestradiol and 3 mg drospirenone, 14.2 mg estetrol with 3 mg drospirenone) and the vaginal ring (ethinylestradiol and etonogestrel). These are welcome changes to improve access and choice for young people.
Conclusion
Effective contraceptive consultations with young people can be highly rewarding for healthcare professionals and highly valued by young people. They can empower young people to make informed choices to protect their sexual health and avoid unintended pregnancy, while establishing a safe space for future healthcare engagement. In an era where misinformation about contraception is widespread, particularly through social media and peer networks, clinicians play a vital role in helping young people navigate conflicting and inaccurate information.
There is no one-size-fits-all approach to contraception; nevertheless, this article highlights some of the key considerations relevant to young people. Providing clear, evidence-based information and involving young people in shared decision-making enhances satisfaction and long-term adherence. By taking a patient-centred approach, clinicians can ensure contraceptive discussions are inclusive and support young people to make choices that align with their values, lifestyle and future reproductive goals. MT
COMPETING INTERESTS: Dr Boerma has been involved in delivering education relating to contraception for Healthed; has received travel support from Healthed; is part of the Therapeutic Guidelines Sexual and Reproductive Health expert working group; and has received support and payment from Therapeutic Guidelines to attend meetings. Dr Callister has been involved in delivering education relating to contraception for Healthed and the Royal Australian College of General Practitioners. Dr Cooper: None.
References
1. Rowe H, Holton S, Kirkman M, et al. Prevalence and distribution of unintended pregnancy: the Understanding Fertility Management in Australia National Survey. Aust N Z J Public Health 2016; 40: 104-109.
2. Shankar M, Hooker L, Edvardsson K, Norman WV, Taft AJ. The prevalence and variations in unintended pregnancy by socio-demographic and health-related factors in a population-based cohort of young Australian women. Aust N Z J Public Health 2023; 47: 100046.
3. Goldhammer DL, Fraser C, Wigginton B, et al. What do young Australian women want (when talking to doctors about contraception)? BMC Fam Pract 2017; 18: 35.
4. Botfield JR, Rathnasekara G, Mazza D, Bernard E, Watson CJ. Contraceptive counselling in regions of Victoria with high incidence of teenage pregnancy: general practitioners’ insights. Aust J Prim Health 2025; 31: PY24169.
5. Claringbold L, Sanci L, Temple-Smith M. Factors influencing young women’s contraceptive choices. Aust J Gen Pract 2019; 48: 389-394.
6. The Shopfront Youth Legal Centre. Children and healthcare. Darlinghurst: The Shopfront Youth Legal Centre; 2021. Available online at: https://www.theshopfront.org/legal-information-for-youth-workers (accessed January 2026).
7. Office of the Australian Information Commissioner. Manage your My Health Record. Canberra: Australian Government; 2026. Available online at: https://www.oaic.gov.au/privacy/your-privacy-rights/health-information/my-health-record/manage-your-my-health-record#:~:text=If%20you%20are%20under%2014,line%20on%201800%20723%20471 (accessed January 2026).
8. Youth Law Australia. Your rights at the doctor. Youth Law Australia; 2024. Available online at: https://yla.org.au/nsw/topics/health-love-and-sex/your-rights-at-the-doctor/ (accessed January 2026).
9. Doukrou M, Segal TY. Fifteen-minute consultation: communicating with young people—how to use HEEADSSS, a psychosocial interview for adolescents. Arch Dis Child Educ Pract Ed 2018; 103: 15-19.
10. Klein DA, Goldenring JM, Adelman WP. HEEADSSS 3.0: the psychosocial interview for adolescents updated for a new century fueled by media. Cranbury, NJ: Contemporary Pediatrics; 2014. Available online at: https://www.contemporary pediatrics.com/view/heeadsss-30-psychosocial-interview-adolescents-updated-new-century-fueled-media (accessed January 2026).
11. Australian Institute of Family Studies. Age of consent laws in Australia. Canberra: Australian Government; 2025. Available online at: https://aifs.gov.au/resources/resource-sheets/age-consent-laws-australia (accessed January 2026).
12. Power J, Kauer S, Fisher C, Bellamy R, Bourne A. The 7th national survey of Australian secondary students and sexual health 2021 (ARCSHS Monograph Series No. 133). Melbourne: The Australian Research Centre in Sex, Health and Society, La Trobe University; 2022. Available online at: https://www.latrobe.edu.au/arcshs/work/sexual-health/national-survey-of-secondary-students (accessed January 2026).
13. NSW Health. Consent to Medical and Healthcare Treatment Manual. St Leonards: NSW Ministry of Health; 2025. Available online at: https://www.health.nsw.gov.au/policies/manuals/Pages/consent-manual.aspx (accessed January 2026).
14. Australian Institute of Family Studies. Mandatory reporting of child abuse and neglect (resource sheet). Canberra: Australian Government; 2023. Available online at: https://aifs.gov.au/resources/resource-sheets/mandatory-reporting-child-abuse-and-neglect (accessed January 2026).
15. Bird S. Consent to medical treatment: the mature minor. Aust Fam Physician 2011; 40: 159-160.
16. Ross S, Polyakov A. Contraception options during pubertal transition: risks, benefits and considerations. Aust J Gen Pract 2024; 53: 740-745.
17. Faculty of Sexual & Reproductive Healthcare (FSRH). FSRH Clinical Guideline: contraceptive choices for young people (March 2010, amended May 2019). London: FSRH; 2010. Available online at: https://www.cosrh.org/Public/Standards-and-Guidance/Young-People.aspx (accessed January 2026).
18. Royal Australian and New Zealand College of Obstetricians and Gynaecologists (RANZCOG). C-Gyn 3 Contraception Guideline Development Group. C-Gyn 3 contraception. Melbourne: RANZCOG; 2024. Available online at: https://ranzcog.edu.au/wp-content/uploads/Contraception-Clinical-Guideline.pdf (accessed January 2026).
19. The Royal Children’s Hospital National Child Health Poll. A teen perspective: health messages and social media. Melbourne: Royal Children’s Hospital Melbourne; 2025. Available online at: https://rchpoll.org.au/polls/a-teen-perspective-health-messages-and-social-media/ (accessed January 2026).
20. de Moel‐Mandel C, Donnelly A, Bugden M. "Do you know what birth control actually does to your body?": assessing contraceptive information on TikTok. Perspect Sex Reprod Health 2025; 57: 358-367.
21. Contraception (updated 2025). In: eTG complete. Melbourne: Therapeutic Guidelines; 2020. Available online at: https://www.tg.org.au (accessed January 2026).
22. College of Sexual and Reproductive Healthcare. UK Medical Eligibility Criteria for Contraceptive Use (UKMEC). London: College of Sexual and Reproductive Healthcare; 2025. Available online at: https://www.cosrh.org/Public/Standards-and-Guidance/uk-medical-eligibility-criteria-for-contraceptive-use-ukmec.aspx (accessed January 2026).
23. Nguyen A, Curtis K, Naomi K, et al. US medical eligibility criteria for contraceptive use, 2024. MMWR Recomm Rep 2024; 73: 1-126.
24. McNicholas C, Madden T, Secura G, Peipert JF. The contraceptive CHOICE project round up: what we did and what we learned. Clin Obstet Gynecol 2014; 57: 635-643.
25. Bradley SE, Polis CB, Micks EA, Steiner MJ. Effectiveness, safety, and comparative side effects. In: Cason P, Cwiak C, Edelman A, et al., eds. Contraceptive technology, 22nd ed. Jones & Bartlett Learning; 2023. p. 130-131.
26. Coombe J, Wigginton B, Loxton D, Lucke J, Harris ML. How young Australian women explain their use of condoms, withdrawal and fertility awareness: a qualitative analysis of free-text comments from the CUPID study. Cult Health Sex 2022; 24: 1563-1574.
27. Faculty of Sexual & Reproductive Healthcare (FSRH). Clinical guideline: combined hormonal contraception (updated 2023). London: FSRH; 2019. Available online at: https://www.cosrh.org/Public/Public/Standards-and-Guidance/Combined-Hormonal-Contraception.aspx (accessed January 2026).
28. Faculty of Sexual & Reproductive Healthcare (FSRH). Clinical guideline: intrauterine contraception (updated 2025). London: FSRH; 2015. Available online at: https://www.cosrh.org/Public/Public/Standards-and-Guidance/Intrauterine-Contraception.aspx (accessed January 2026).
29. Sergison JE, Maldonado LY, Gao X, Hubacher D. Levonorgestrel intrauterine system associated amenorrhea: a systematic review and metaanalysis. Am J Obstet Gynecol 2019; 220: 440-448.
30. Faculty of Sexual & Reproductive Healthcare (FSRH). Clinical guideline: progestogen-only injectable contraception (updated 2023). London: FSRH; 2014. Available online at: https://www.cosrh.org/Public/Public/Standards-and-Guidance/Progestogen-only-Injectables.aspx (accessed January 2026).
31. Faculty of Sexual & Reproductive Healthcare (FSRH). Clinical guideline: progestogen-only pills (updated 2023). London: FSRH; 2022. Available online at: https://www.cosrh.org/Public/Public/Standards-and-Guidance/Progestogen-only-Pills.aspx (accessed January 2026).
32. Cameron L, Mikocka‐Walus A, Sciberras E, Druitt M, Stanley K, Evans S. Menstrual pain in Australian adolescent girls and its impact on regular activities: a population‐based cohort analysis based on Longitudinal Study of Australian Children survey data. Med J Aust 2024; 220: 466-471.
33. Reid-McCann R, Poli-Neto OB, Stein K, et al. Longitudinal association between dysmenorrhoea in adolescence and chronic pain in adulthood: a UK population- based study. Lancet Child Adolesc Health 2025; 9: 766-775.
34. Ferries-Rowe E, Corey E, Archer JS. Primary dysmenorrhea: diagnosis and therapy. Obstet Gynecol 2020; 136: 1047-1058.
35. Acne (updated 2025). In: eTG Complete. Melbourne: Therapeutic Guidelines; 2022. Available from: http://www.tg.org.au (accessed January 2026).
36. Arowojolu A, Gallo M, Lopez L, Grimes D. Combined oral contraceptive pills for treatment of acne. Cochrane Database Syst Rev 2012; 2012(7): CD004425.
37. Therapeutic Goods Administration. Cyproterone: products containing cyproterone with ethinyloestradiol, such as Diane-35. Canberra: Australian Government, Department of Health, Disability and Ageing; 2013. Available online at: https://www.tga.gov.au/safety/safety-monitoring-and-information/safety-alerts/cyproterone-products-containing-cyproterone-ethinyloestradiol-such-diane-35 (accessed January 2026).
38. Reynolds RV, Yeung H, Cheng CE, et al. Guidelines of care for the management of acne vulgaris. J Am Acad Dermatol 2024; 90: 1006.e1-1006.e30.
39. Australasian Society for HIV, Viral Hepatitis and Sexual Health Medicine (ASHM). Australian STI management guidelines for use in primary care. Young people. Sydney: ASHM; 2024. Available online at: https://sti.guidelines.org.au/populations-and-situations/young-people/ (accessed January 2026).
40. Australasian Society for HIV, Viral Hepatitis and Sexual Health Medicine (ASHM). Prevent HIV by prescribing PrEP. Sydney: ASHM; 2025. Available online at: https://ashm.org.au/resources/australian-prep-guidelines/ (accessed January 2026).
41. Cornelisse VJ, Riley B, Medland NA. Australian consensus statement on doxycycline post‐exposure prophylaxis (doxy‐PEP) for the prevention of syphilis, chlamydia and gonorrhoea among gay, bisexual and other men who have sex with men. Med J Aust 2024; 220: 381-386.
42. Diedrich JT, Klein DA, Peipert JF. Long-acting reversible contraception in adolescents: a systematic review and meta-analysis. Am J Obstet Gynecol 2017; 216: 364.e1-364.e12.
43. Rosenstock JR, Peipert JF, Madden T, Zhao Q, Secura GM. Continuation of reversible contraception in teenagers and young women. Obstet Gynecol 2012; 120: 1298-1305.
44. Harris ML, Coombe J, Forder PM, Lucke JC, Bateson D, Loxton D. Young women’s complex patterns of contraceptive use: findings from an Australian cohort study. Perspect Sex Reprod Health 2020; 52: 181-190.
45. Garrett CC, Keogh LA, Kavanagh A, Tomnay J, Hocking JS. Understanding the low uptake of long-acting reversible contraception by young women in Australia: a qualitative study. BMC Womens Health 2015; 15: 72.
46. Faculty of Sexual & Reproductive Healthcare (FSRH). Clinical guideline: pain associated with insertion of intrauterine contraception. London: FSRH; 2021. Available online at: Available online at: https://www.cosrh.org/Public/Documents/fsrh-statement-pain-associated-with-insertion-of-intrauterine.aspx (accessed January 2026).
47. Wright S, Kidman P, Boerma C, Botfield JR. Acceptability of intrauterine device insertion without sedation for young nulliparous people: a mixed-methods study. Sex Health 2025; 22: SH25100.
48. Wise MK, Okuyemi O, Flint M, et al. Intrauterine device placement success for adolescents and young adults at community-based reproductive health clinics. J Pediatr Adolesc Gynecol 2024; 37: 160-164.
49. Gemzell-Danielsson K, Schellschmidt I, Apter D. A randomized, phase II study describing the efficacy, bleeding profile, and safety of two low-dose levonorgestrel-releasing intrauterine contraceptive systems and Mirena. Fertil Steril 2012; 97: 616-622.e1-3.
50. Ovsepyan V, Kelsey P, Evensen AE. Practical recommendations for minimizing pain and anxiety with IUD insertion. J Am Board Fam Med 2024; 37: 1150-1155.
51. Sairally BZF, Smith PP, De Silva PM, O’Connor S, Yates C, Clark TJ. Inhaled methoxyflurane (Penthrox®) as a novel pain relief for outpatient hysteroscopy and other gynaecological procedures. Eur J Obstet Gynecol Reprod Biol 2024; 302: 206-210.
52. Pfender EJ, Devlin MM. What do social media influencers say about birth control? A content analysis of YouTube vlogs about birth control. Health Commun 2023: 38: 3336-3345.
53. Faculty of Sexual & Reproductive Healthcare (FSRH). Clinical guideline: overweight, obesity and contraception. London: FSRH; 2019. Available online at: https://www.cosrh.org/Public/Standards-and-Guidance/Overweight-and-Obesity.aspx (accessed January 2026).
54. Skovlund CW, Morch LS, Kessing LV, Lidegaard O. Association of hormonal contraception with depression. JAMA Psychiatr 2016; 73: 1154-1162.
55. Medicare Benefits Schedule. November 2025 news. Canberra: Australian Government, Department of Health, Disability and Ageing; 2025. Available online at: https://www.mbsonline.gov.au/internet/mbsonline/publishing.nsf/Content/news-251101 (accessed January 2026).
56. SPHERE. The AusCAPPS Network. Melbourne: SPHERE; 2025. Available online at: https://www.spherecre.org/research/current-trials/auscapps-network (accessed January 2026).
57. Sexual and Reproductive Health Australia (SRHA). AUSLARC training scholarship guidelines. Canberra: SRHA; 2025. Available online at: https://familyplanningalliance australia.org.au/auslarc-scholarship/ (accessed January 2026).