Contraception after pregnancy
Fertility can return rapidly after pregnancy, often before menstruation resumes. Misconceptions and missed opportunities contribute to high rates of unintended pregnancy during this time. GPs play a vital role in timely, patient-centred contraceptive care following all pregnancy outcomes.
- Ovulation may occur before the return of menstruation following the end of pregnancy, creating early vulnerability to subsequent unintended conception.
- Most reversible contraceptive methods can be safely initiated immediately after pregnancy.
- Long-acting reversible contraceptives are highly effective but remain underused postpartum and post-abortion.
- GPs are well placed to provide early, nondirective contraceptive counselling tailored to individual needs.
- When recommending contraception after pregnancy, consider contextual factors such as breastfeeding, personal circumstances, medical comorbidities and the risk of reproductive coercion.
There is significant unmet need for contraception following pregnancy. Irrespective of how a pregnancy ends, fertility can return quickly, with ovulation possible before the resumption of menstruation.1,2 Misconceptions relating to the risk of repeat pregnancy, ideal pregnancy spacing and eligibility for contraceptives, as well as presumptions regarding pregnancy intention and competing demands, may contribute to women remaining vulnerable to pregnancy during this period.3
Unintended pregnancy remains common, with approximately one in four women in Australia experiencing an unintended pregnancy in their lifetime.4 It is more common in those who live in rural locations or experience social coercion or disadvantage and among Aboriginal or Torres Strait Islander people.4,5 Fertility can return rapidly following a pregnancy, creating a vulnerable period for unintended (including unwanted or mistimed) conception (Table 1).6,7 Many women in Australia report not using contraception at the time of unintended pregnancy, and when it is being taken, contraceptive pills and condoms are more often used than highly effective long-acting reversible contraceptives (LARCs), which include intrauterine devices (IUDs) and the progestogen-only implant.8 Contact with healthcare providers, including GPs, during and after pregnancy presents an important opportunity to dispel misconceptions and support contraceptive choice for those not imminently desiring another pregnancy.
As with contraceptive counselling at other times during the reproductive lifespan, clinicians should provide information about, and access to, all effective contraceptive methods, including LARCs, within the context of informed choice.7,9 The Family Planning Alliance Australia contraceptive efficacy chart is a useful counselling tool outlining the efficacy of the various contraceptive methods, freely available online (https://familyplanningalliance australia.org.au/wp-content/uploads/2024/07/EFFICACY-OF-CONTRACEPTIVE-METHODS-July-2024.pdf).
This article reviews the current evidence and best practice in the provision of reversible contraception following various pregnancy outcomes, including birth, abortion, miscarriage, ectopic pregnancy and gestational trophoblastic disease. In addition to this, GPs should consider the increased risk of intimate partner violence during pregnancy and the postnatal period.10 This may include reproductive coercion and influence on contraceptive choice, pregnancy outcomes, or both.11
Permanent contraception, including vasectomy and tubal libation, are beyond the scope of this article; however, these may be valuable options for those not wanting any future pregnancies. In addition, fertility awareness methods are not discussed. These are highly user-dependent and include various approaches aimed at predicting the timing of ovulation, so that intercourse may be avoided during fertile periods. However, reliable identification of these signs and symptoms may be particularly difficult after pregnancy.
Although ‘women’ are referred to throughout this article, as those most commonly requiring contraception after pregnancy, it is acknowledged that transgender and gender-diverse people may also require contraception following pregnancy. Inclusivity in the delivery of healthcare services is encouraged.
Contraception after childbirth
An Australian survey found approximately 20% of pregnancies occurred within 12 months of childbirth, with most being unintended.12 A UK study found that more than one in eight parous women seeking abortion had conceived within 12 months postpartum.13 For those who chose to continue the pregnancy, the opportunity to provide interconception care, optimising maternal health prior to subsequent pregnancies, is missed.3 Furthermore, short interpregnancy intervals, defined as less than 12 months from childbirth to subsequent conception, are associated with an increased risk of perinatal complications, including stillbirth, small size for gestational age, preterm delivery and infant death.14
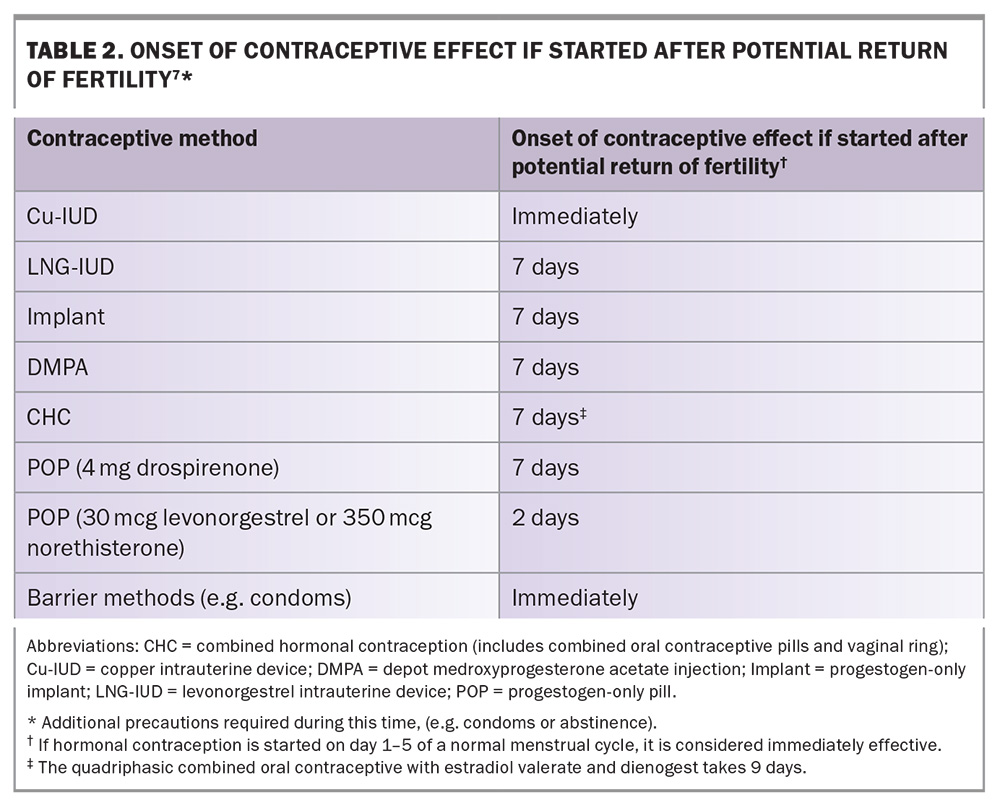
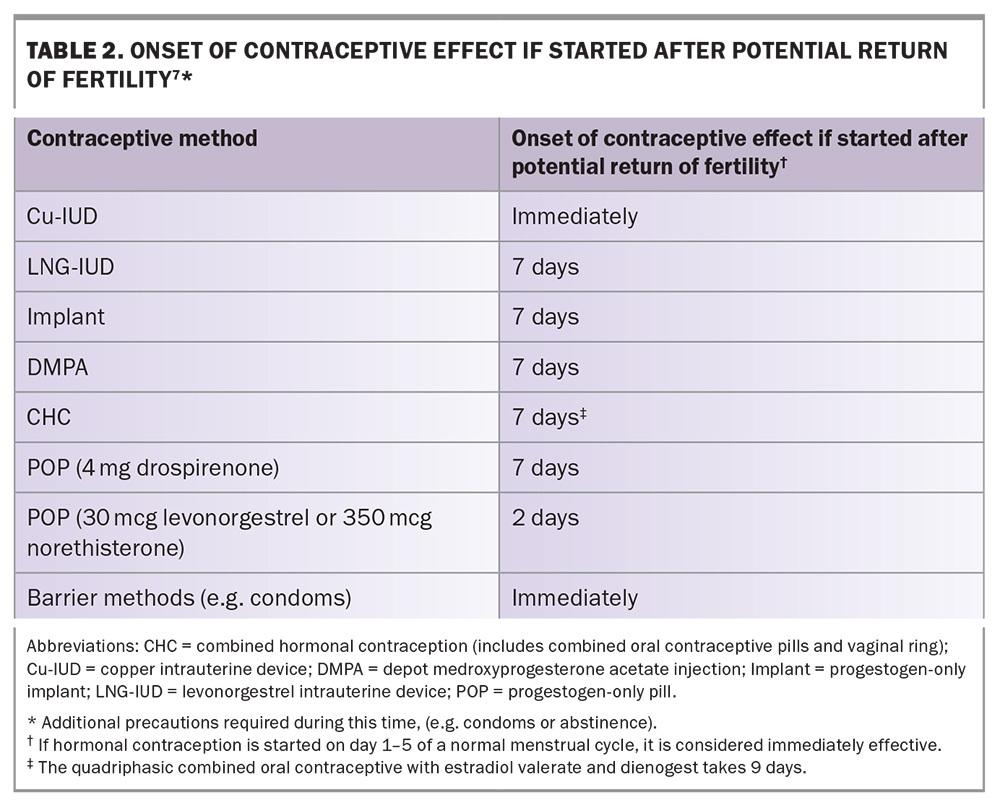
Postpartum contraception is most commonly accessed at or after the six-week postnatal check, leaving some women vulnerable to another pregnancy.15 Contraception is recommended by day 21 postpartum (Table 1), and hormonal contraception may not be immediately effective if started after this time (Table 1 and Table 2).7,9 Furthermore, over 40% of women may resume vaginal sex before six weeks.16 At the postnatal check, competing priorities (including review of the birth experience, pregnancy and birth complications, perinatal mental health, cervical screening [if due] and breastfeeding concerns) may delay contraceptive discussion.17 Given these barriers, early antenatal or immediate postpartum discussions and prompt initiation of contraception are recommended.9,15 Although maternity services have a role, GPs are well positioned to support these contraceptive discussions due to their continuity of care and understanding of patients’ circumstances and medical history.
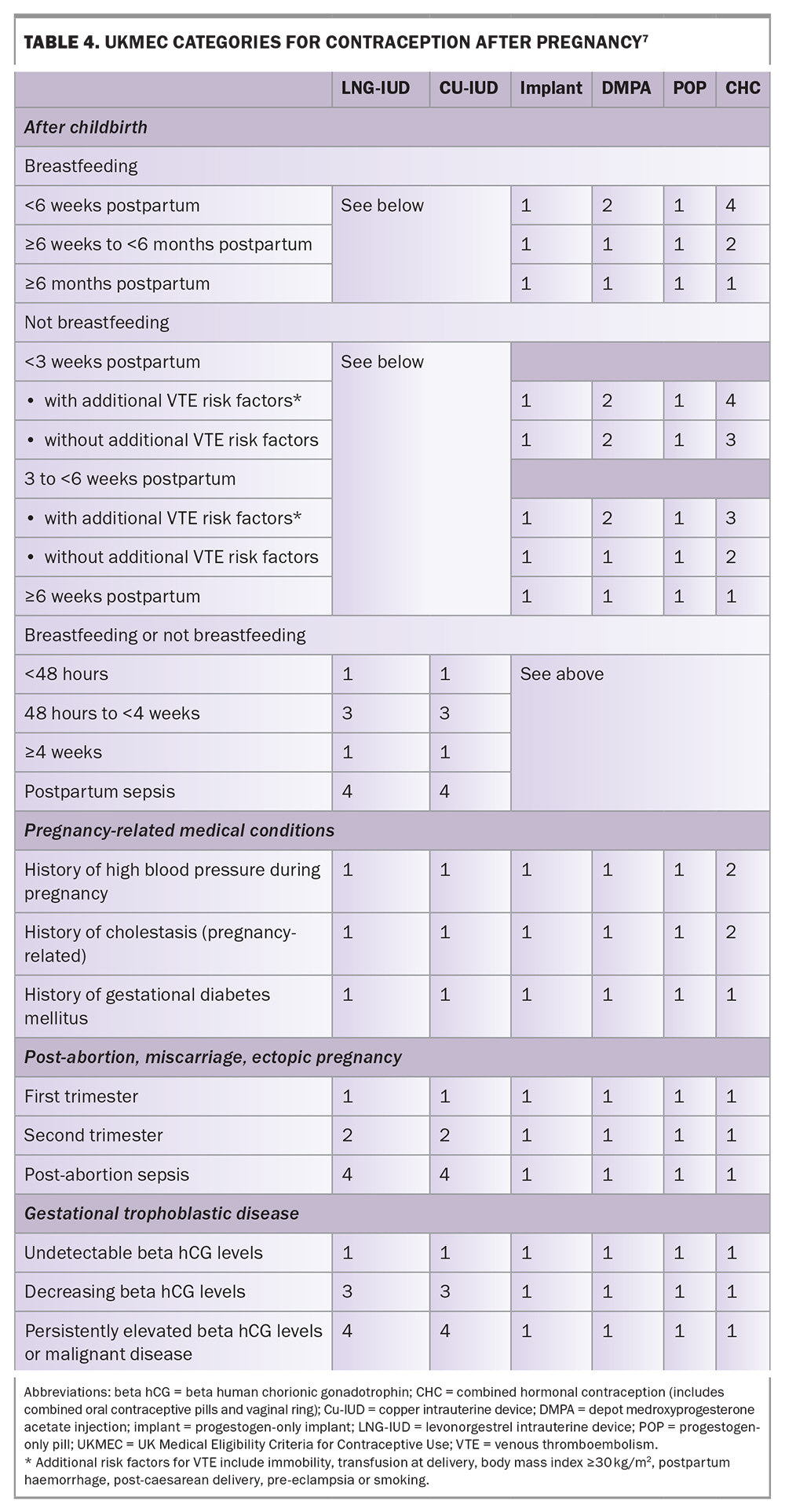
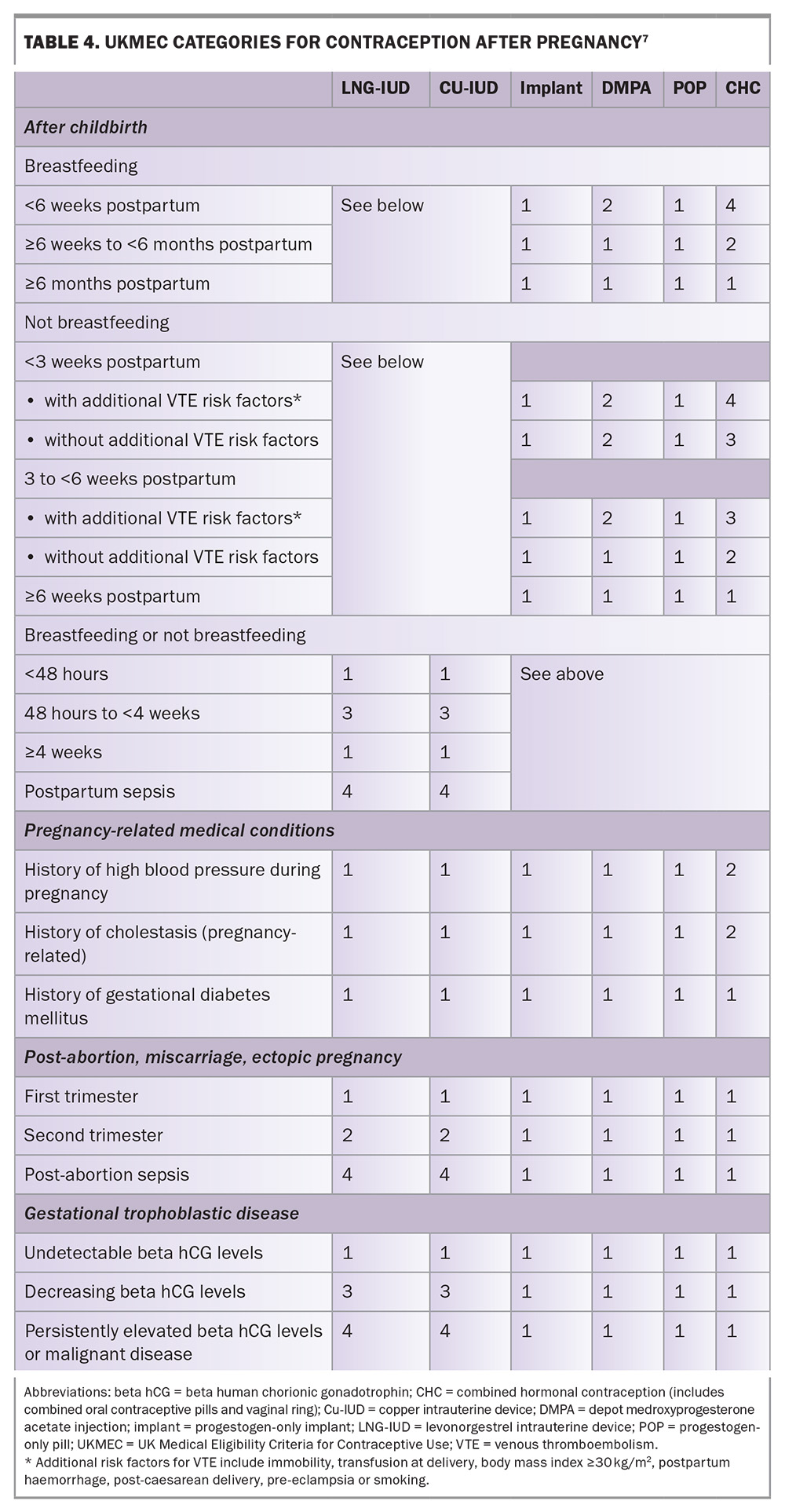
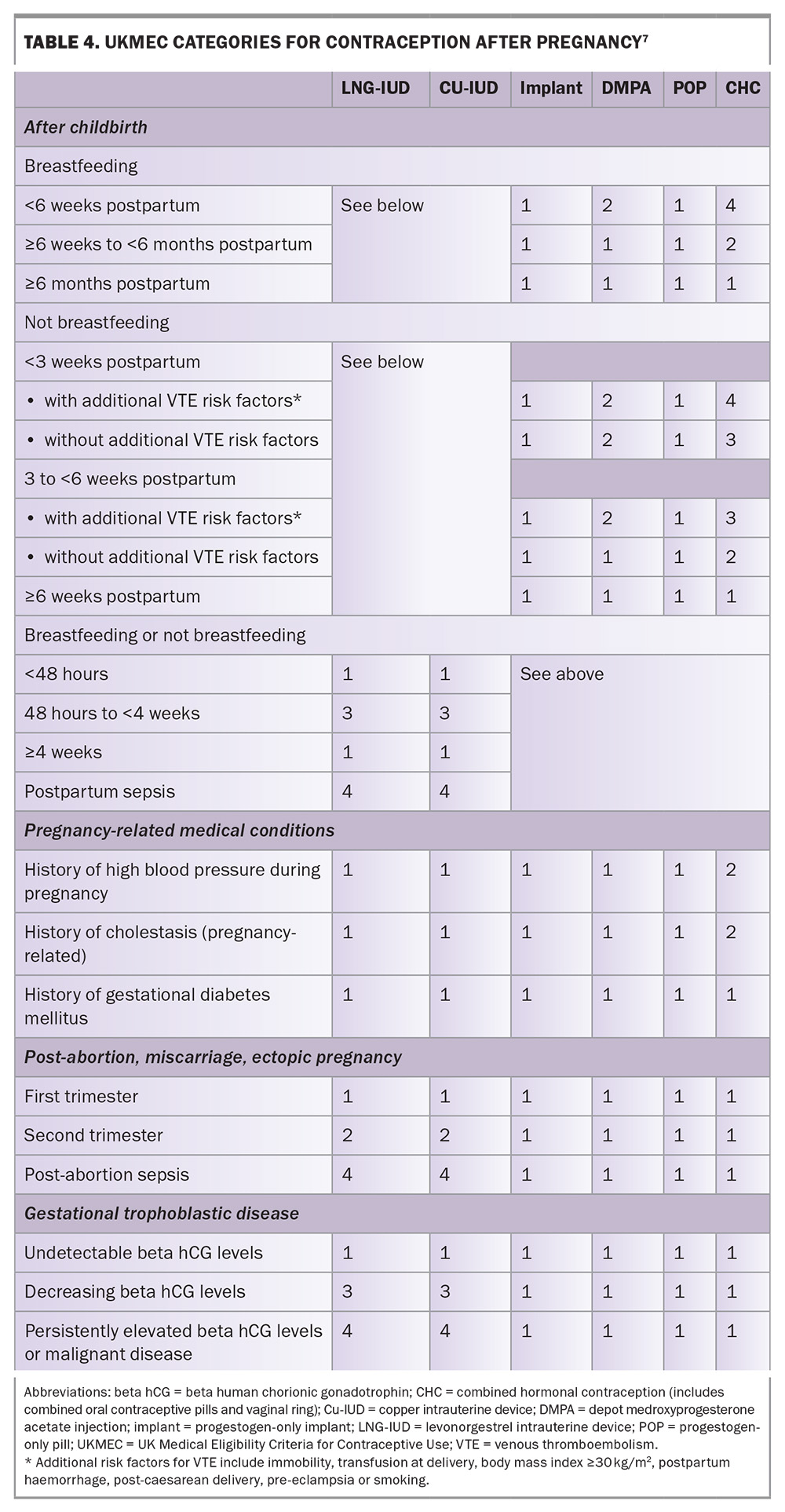
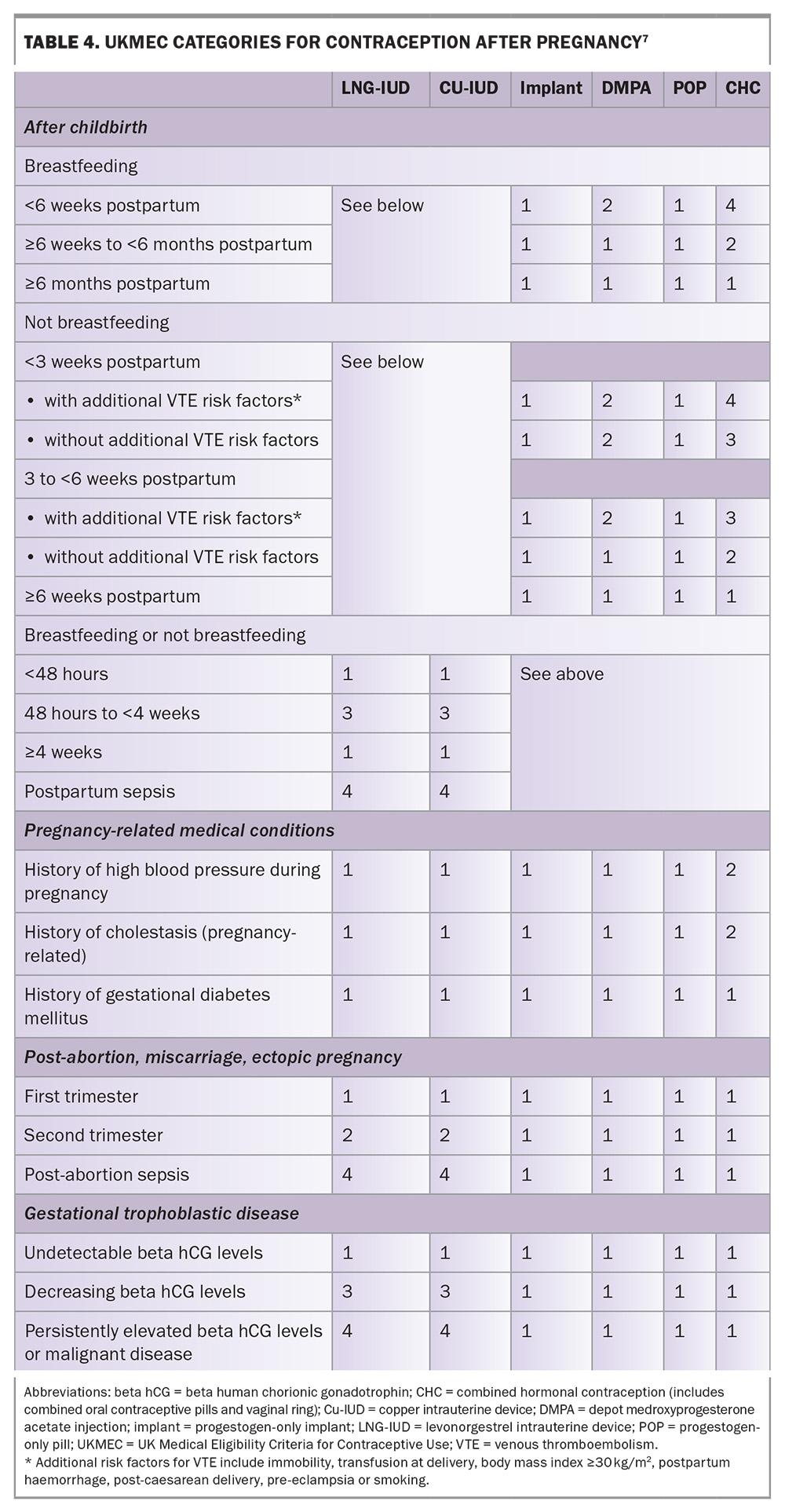
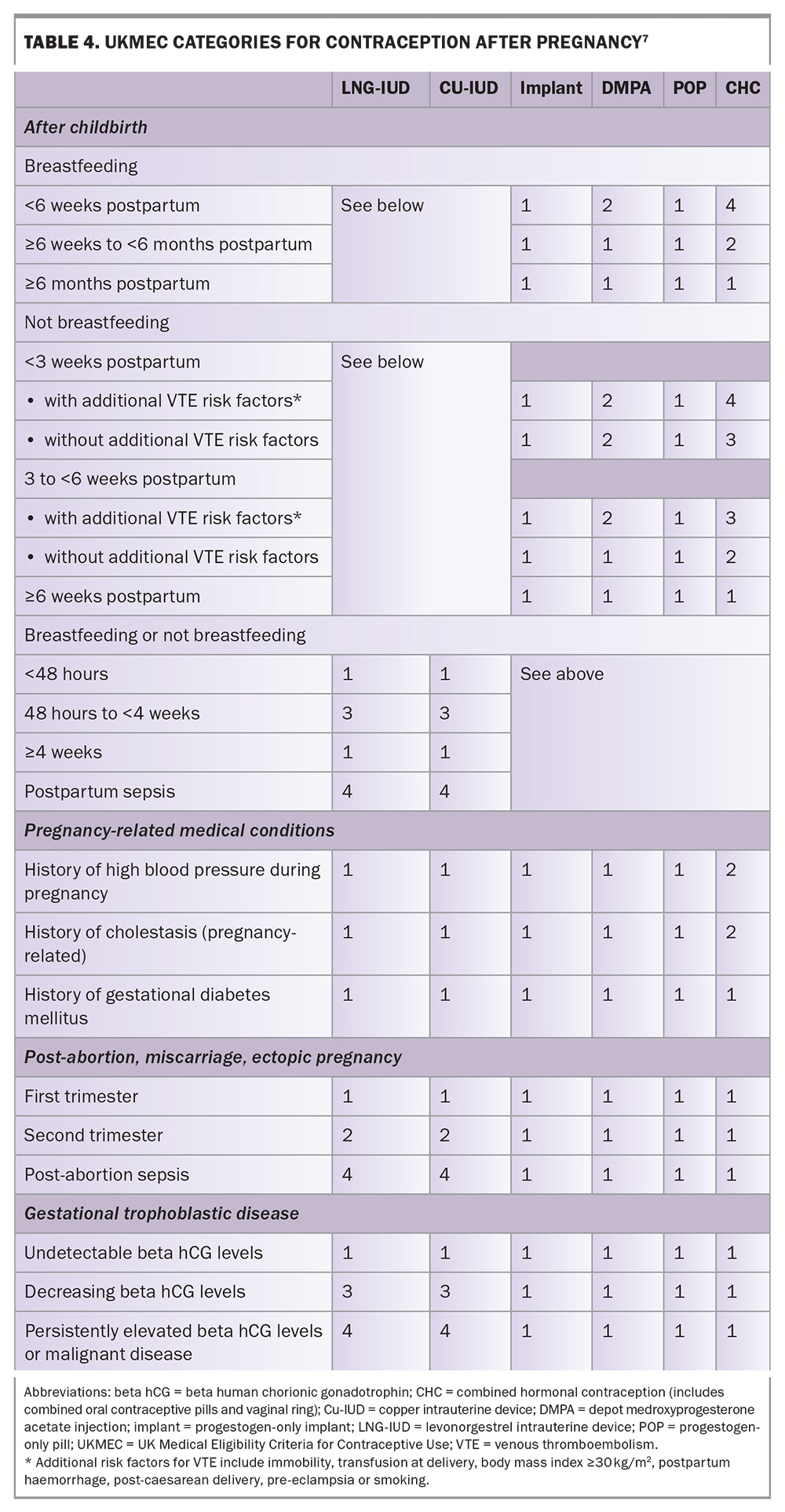
The UK Medical Eligibility Criteria for Contraceptive Use (UKMEC) offers evidence-based guidance for safe contraceptive prescribing, including following pregnancy. Excluding combined hormonal contraception and the diaphragm, most contraceptive options, including LARCs, may be initiated safely from childbirth in both breastfeeding and nonbreastfeeding women. The four UKMEC categories are defined in Table 3 and the UKMEC guidance following pregnancy is summarised in Table 4.7
Medical conditions arising during pregnancy that may impact the eligibility criteria for use of contraception, particularly if they have not resolved postpartum (e.g. hypertensive disorders, diabetes or obesity), should be considered. UKMEC categorisations for contraception in women with these conditions are given in Table 4.
Lactational amenorrhoea method
Breastfeeding suppresses ovarian activity and the return of menstrual periods. It can be an effective contraceptive (with a failure rate of less than 2%), provided that the patient is less than six months postpartum, amenorrhoeic and exclusively breastfeeding (with no more than four hours between breastfeeds during the day and six hours at night).7
However, as breastfeeding may gradually reduce, or be disrupted by illness or supplementary feeding, the use of additional contraceptives is often required. Clinicians should advise women using lactational amenorrhoea methods to start using another reliable form of contraception by six months.
Progestogen-only methods
Progestogen-only pills (POPs), as well as the progestogen-only implant and depot medroxyprogesterone acetate (DMPA) injections, can be safely initiated at any time postpartum. Progestogen-only methods (including the methods listed and hormonal IUDs) do not adversely affect lactation or infant outcomes and may be started before sexual activity has resumed if that is most convenient. The 4 mg drospirenone pill was added to the PBS in March 2025. Compared with the traditional POPs or ‘minipills’ (i.e. 30 mcg levonorgestrel or 350 mcg norethisterone), which have a narrow three-hour administration window, the drospirenone POP can be taken within a more forgiving 24-hour window. This may be particularly valuable in maintaining contraceptive efficacy postpartum, during a time of disrupted sleep and altered routine.
The progestogen-only implant requires no regular user action and, when inserted soon after birth, has been found to be both convenient and acceptable, with high continuation rates.7 DMPA may be considered as a second-line option in the first six weeks postpartum due to a theoretical concern of increased risk of venous thromboembolism (VTE) compared with other progestogen-only methods. Nevertheless, when preferred, its use is supported by the UKMEC; it is categorised as UKMEC 2 from birth to six weeks postpartum, and UKMEC 1 thereafter (Table 4).7 Although irregular bleeding is possible with all progestogen-only contraceptives, available evidence does not suggest it is more problematic with use in the postpartum period.7
Intrauterine methods
IUDs, including copper IUDs (Cu-IUDs) and progestogen-only hormonal IUDs containing levonorgestrel (LNG-IUDs), can be safely inserted within 48 hours of uncomplicated childbirth (caesarean section or vaginal delivery).18 The timing is highly convenient, avoiding the need for additional medical visits, and many women will have existing analgesia in place. Contraindications to IUD insertion at the time of delivery include prolonged rupture of membranes, postpartum haemorrhage and sepsis.7
Given uterine involution following birth, more women may require investigations for missing threads, and long IUD threads may require trimming at follow-up. Compared with delayed insertion (i.e. four to eight weeks postpartum), IUD placement at the time of delivery is associated with a higher rate of expulsion, particularly after vaginal birth.9,19 However, continuation of IUD use at six months is higher following insertion at birth compared with delayed insertion, given not all women will attend for insertion at subsequent follow-up appointments.18 Thus, for some, the benefits of early insertion of an IUD and immediate contraceptive cover may outweigh the increased risk of expulsion.18 GPs can support women in discussing postpartum IUD options with the obstetric team prior to delivery.
From 48 hours to 28 days postpartum, the UKMEC advises delaying IUD insertion due to concerns regarding the risk of uterine perforation during this time.9 If delayed insertion is being considered, alternative bridging contraception should be offered to provide cover. Although the absolute rate of perforation remains low (about 1%), the risk is increased up to six-fold in breastfeeding women and during the first nine months postpartum.20,21 Although the clinical course after perforation is usually benign, women should be counselled regarding this small but elevated risk.
Combined hormonal methods
Combined hormonal contraceptives (CHCs) contain oestrogen with progestogen and include the combined oral contraceptive pill (COCP) and the vaginal ring. Medical eligibility for CHC use after pregnancy depends on VTE risk factors and breastfeeding status. The risk of VTE is significantly elevated in the weeks after childbirth, and oestrogen-containing contraceptives further increase this risk; their use is therefore restricted during this period.
Evidence on the impact of CHCs on lactation is limited and conflicting; however, there appears to be no adverse impact on infant weight gain or development when used after six weeks postpartum.22 For individuals without additional VTE risk factors (e.g. immobility, obesity, postpartum haemorrhage or blood transfusion at delivery, caesarean section, pre-eclampsia or smoking) and who are not breastfeeding, CHCs may be started from three weeks postpartum. For those with additional VTE risk factors or who are breastfeeding, CHCs should not be used before six weeks postpartum. In breastfeeding individuals, CHCs are generally considered acceptable from six weeks (UKMEC 2), with no restriction from six months onward (UKMEC 1).7
Barrier methods
Use of the diaphragm should be delayed until at least six weeks postpartum (allowing for uterine involution). Condoms (male/external or female/internal) may be used at any time postpartum.
Emergency contraception
Emergency contraception is not required before 21 days postpartum. Both levonorgestrel and ulipristal acetate emergency contraceptive pills are considered safe for use up to four or five days, respectively, after unprotected intercourse, including during breastfeeding (off-label use). Interruption of breastfeeding (i.e. ‘pump and dump’) following ulipristal acetate is no longer recommended, as there is no published evidence of harm.23,24 Cu-IUDs are the most effective form of emergency contraception when inserted within five days of unprotected intercourse and may be used from 28 days postpartum, as discussed above.
Contraception after abortion
All GPs in Australia are now authorised to prescribe medical abortion medications, which include mifepristone and misoprostol, sold together and licensed for use up to nine weeks’ (63 days’) gestation. The approved regimen is mifepristone 200 mg, followed 36 to 48 hours later by misoprostol 800 mcg. Medical abortion may also be provided in hospital settings at later gestations. Surgical abortion can be performed in either the first or second trimester.
Contraception is a key part of comprehensive abortion care, and guidelines recommend it be offered to women at the time of abortion.25 Return to fertility can be rapid, with ovulation possible from day eight following abortion, and contraception is advised from day five (Table 1).2 Furthermore, over half of patients are likely to resume sexual activity within two weeks.26 Early provision of hormonal contraception, LARCs in particular, following medical abortion is associated with a reduced risk of subsequent unintended pregnancy and repeat abortion.27 This can be a time when many women are motivated to initiate contraception and are actively engaged with healthcare services.
However, abortion consultations can be complex and time-intensive, and some patients may need more time to consider their contraceptive options. It is essential that contraception counselling remains patient-centred and free from pressure or coercion, even in the context of abortion care. Healthcare providers should support informed contraceptive decision making after abortion, in line with each woman’s preferences and needs.
All contraceptive methods may be commenced at the time of uncomplicated abortion, with the exemption of IUDs during medical abortion, where insertion must be delayed until the products of conception have passed (Table 4). If contraception is started within five days of abortion, it is effective immediately (Table 1 and Table 2). Method-specific considerations are detailed below.
Intrauterine contraception
The Cu-IUD or LNG-IUD can be inserted at the time of an uncomplicated first- or second-trimester surgical abortion and provides immediate contraception protection. Insertion at this time is safe and convenient.7 IUD insertions are UKMEC 1 following first-trimester abortion and UKMEC 2 following second-trimester abortion, due to the slightly higher expulsion rate at later gestations.7
Cu- and LNG-IUDs can be inserted following medical abortion once the pregnancy tissue has passed. In practice, this is often more than five days after the abortion, so bridging contraception should be provided to women in the interim.
An additional potential benefit of LNG-IUD insertion is that it may be associated with reduced uterine bleeding after surgical or medical abortion.7
In the case of septic abortion, IUD insertion should be delayed until the infection has fully resolved.
Progestogen-only methods
All progestogen-only contraceptive methods (POP, progestogen-only implant and DMPA injection) may be safely initiated from the time of medical or surgical abortion.
There has been theoretical concern that progestogen-only contraception may reduce the efficacy of medical abortion due to competition at progesterone receptors, as mifepristone is a progesterone-receptor modulator. However, insertion of the progestogen-only implant at the time of medical abortion has not been shown to influence the efficacy of medical abortion.7 Furthermore, implant placement at this time is convenient, highly acceptable and results in higher continuation rates.28
In contrast, there is limited evidence that DMPA administration at the time of mifepristone may be associated with a slightly increased risk of medical abortion failure.7 This does not preclude its use at the time of mifepristone when preferred, but this small potential risk should be discussed with the patient.
Current clinical guidelines recommend follow-up after all medical abortions.29 Patients should receive clear guidance on what to expect following medical abortion, including bleeding patterns. Minimal bleeding may indicate failed medical abortion and should not automatically be attributed to use of hormonal contraception.
Combined hormonal methods
CHCs, including the COCP and the vaginal ring, can be commenced at the time of medical or surgical abortion. In practice, oral CHCs are often started the day after a surgical procedure or the day after misoprostol (which may cause nausea and vomiting) is taken for a medical abortion.
Following abortion, it is advised that nothing be inserted into the vagina for at least seven days to reduce the risk of infection. Although there is limited evidence supporting this recommendation, if the vaginal ring is the chosen contraceptive method, insertion on day one to five (with hygiene precautions) is considered reasonable. In such cases, the benefits of timely initiation, particularly the prevention of unintended pregnancy, are likely to outweigh the theoretical risks.28
Barrier methods
Condoms may be used any time following an abortion. Diaphragms may be used immediately following a first-trimester abortion but should be delayed for six weeks following a second-trimester abortion, as uterine involution may affect the fit. It should be noted that barrier methods have higher typical-use failure rates compared with the other contraceptives discussed, although condoms remain the only method that also provides protection against sexually transmitted infections.
Emergency contraception
There are no restrictions on the use of emergency contraception after abortion. It should be considered when a woman has had unprotected intercourse five or more days after an abortion.
Contraception after miscarriage or ectopic pregnancy
Pregnancies ending in miscarriage or ectopic pregnancy may have been intended or unintended.1 For instance, in one national telephone survey, over 15% of unintended pregnancies ended in miscarriages.8 It is therefore important to avoid assumptions and to sensitively ask about future pregnancy intentions, offering contraception where appropriate.
Following uncomplicated miscarriage, there is no need to delay conception if pregnancy is desired. Conversely, it may be recommended to delay pregnancy after medical management of ectopic pregnancy, due to the teratogenic potential of methotrexate.1 Specific advice will usually be provided by the treating specialist team, based on the method of treatment.
The UKMEC recommendations for contraception following miscarriage or ectopic pregnancy are the same as those for after abortion (Table 4). As for induced abortion, contraception is recommended by five days after treatment of miscarriage or ectopic pregnancy. If unprotected intercourse occurs after this time, emergency contraception may be used without restriction.
Miscarriage (spontaneous abortion) can occur in the first or second trimester. Management may be expectant (the pregnancy tissue is allowed to pass unaided), medical or surgical. Ovulation may occur as soon as eight days after miscarriage, and contraception is required from day five (Table 1). All contraceptive methods can be safely commenced once the miscarriage is complete and will be effective immediately if commenced within days one to five following treatment.
For ectopic pregnancy, any contraceptive method can be commenced on the day of treatment, whether surgical or medical. Contraceptive protection will be immediate if commenced within days one to five following management of ectopic pregnancy (Table 1). All contraceptive choices are suitable, but the most effective methods (i.e. LARCs) may be preferred, given the increased risk of recurrence in those with a history of ectopic pregnancy.8
Although ectopic pregnancy is more likely in the very rare occurrence of IUD contraceptive failure, IUDs remain among the most effective methods of contraception overall. By reducing the chance of all pregnancies, including ectopic pregnancies, IUDs are an appropriate option for most women.7
Contraception after gestational trophoblastic disease
Gestational trophoblastic disease (GTD) refers to a group of placental related disorders derived from a pregnancy, commonly known as molar pregnancies. These range from local pathology (partial molar and full molar pregnancies) to malignant gestational trophoblastic neoplasia.
Treatment involves surgical evacuation followed by serial serum beta human chorionic gonadotrophin (beta hCG) surveillance to monitor for recurrence of GTD and reduce the risk of missing malignant transformation. The duration of the surveillance period is determined by the rate of decline in serum beta hCG levels and the specific subtype of GTD diagnosed on histopathology. As pregnancy interferes with interpretation of beta hCG and may impact prognosis, conception should be avoided until serial beta hCG readings have returned to normal (undetectable) and the relevant surveillance period after treatment is complete.1,30 People diagnosed with gestational trophoblastic neoplasia are generally advised not to conceive for 12 months after completion of treatment with chemotherapy.30
As fertility can return rapidly following treatment, early initiation of effective contraception is a key component of management.7 Most types of contraception are suitable to commence immediately after surgical evacuation of GTD, with the exception of IUDs. Hormonal fluctuations caused by GTD result in softening of the uterine wall, increasing the risk of uterine perforation. Accordingly, it is recommended that IUD use should generally be avoided for at least six weeks following surgical evacuation, and until beta hCG levels are undetectable.31
The UKMEC supports the use of progestogen-only methods (such as the POP, progestogen-only implant and DMPA injection) and CHCs (such as the POP, progestogen-only implant and DMPA injection) from the day of surgical evacuation, provided the individual is otherwise medically eligible (Table 4). Emergency contraceptive pills are also considered safe to use as required.
Conclusion
Fertility can return rapidly after pregnancy due to early ovulation and the resumption of sexual activity. GPs are well placed to initiate timely discussions and provide information on suitable contraceptive options. Most contraceptive options can be commenced without delay following the end of a pregnancy. Evidence-based guidelines such as the UKMEC should be consulted to guide safe prescribing. A patient-centred approach, supporting informed choice through clear, nondirective counselling, ensures women are empowered to select a method that aligns with their unique needs and circumstances. MT
COMPETING INTERESTS: Dr Boerma and Dr Callister have been involved in delivering education relating to contraception for Healthed, an education provider for GPs. Dr Ong: None.
References
1. Cooper M, Cameron S. Contraception after abortion, miscarriage, ectopic and molar pregnancy. Best Pract Res Clin Obstet Gynaecol 2024; 92: 102428.
2. Schreiber CA, Sober S, Ratcliffe S, Creinin MD. Ovulation resumption after medical abortion with mifepristone and misoprostol. Contraception 2011; 84: 230-233.
3. Dorney E, Mazza D, Black KI. Interconception care. Aust J Gen Pract 2020; 49: 317-322.
4. Rowe H, Holton S, Kirkman M, et al. Prevalence and distribution of unintended pregnancy: the Understanding Fertility Management in Australia National Survey. Aust N Z J Public Health 2016; 40: 104-109.
5. HTANALYSTS. Impact of Unintended Pregnancy. Sydney: Organon; 2022. Available online at: https://www.organon.com/australia/wp-content/uploads/sites/16/2022/09/ORG01_Report_FINAL_28June2022.pdf (accessed July 2025).
6. Cooper M, Black K, Cameron S. Expanding access to postpartum contraception. Curr Opin Obstet Gynecol 2024; 36: 331-337.
7. Faculty of Sexual & Reproductive Healthcare (FSRH). FSRH Guideline: Contraception After Pregnancy. London: FSRH; 2017 (amended 2020). Available online at: https://www.fsrh.org/Common/Uploaded-20files/documents/contraception-after-pregnancy-guideline-oct2020.pdf (accessed July 2025).
8. Taft AJ, Shankar M, Black KI, Mazza D, Hussainy S, Lucke JC. Unintended and unwanted pregnancy in Australia: a cross-sectional, national random telephone survey of prevalence and outcomes. Med J Aust 2018; 209: 407-408.
9. Royal Australian and New Zealand College of Obstetricians and Gynaecologists (RANZCOG). C-Gyn 3 Contraception (Signposting): Clinical Guideline. Melbourne: RANZCOG; 2024.
10. Campo M. Domestic and family violence in pregnancy and early parenthood; policy & practice paper. Melbourne: Australian Institute of Family Studies, Commonwealth of Australia; 2015.
11. MacDonald JB, Gartoulla P, Truong M, Tarzia L, Willoughby M. Reproductive Coercion and Abuse; Practice Guide. Melbourne: Australian Institute of Family Studies, Commonwealth of Australia; 2023.
12. Yang JM, Cheney K, Taylor R, Black K. Interpregnancy intervals and women’s knowledge of the ideal timing between birth and conception. BMJ Sex Reprod Health 2019; 45: 249-254.
13. Heller R, Cameron S, Briggs R, Forson N, Glasier A. Postpartum contraception: a missed opportunity to prevent unintended pregnancy and short inter-pregnancy intervals. J Fam Plann Reprod Health Care 2016; 42: 93-98.
14. Taylor RAM, Yang JM, Cheney K, Black K. Short interpregnancy interval: circumstance or choice? BMJ Sex Reprod Health 2022; 48: 110-116.
15. Singh R, Botfield JR. Postpartum contraception in Australia: opportunities for increasing access in the primary care setting. Aust J Prim Health 2024; 30.
16. McDonald E, Brown S. Does method of birth make a difference to when women resume sex after childbirth? BJOG 2013; 120: 823-830.
17. Milroy T, Frayne J. Postnatal care: the general practitioner visit. Aust J Gen Pract 2022; 51: 105-110.
18. Lopez LM, Bernholc A, Hubacher D, Stuart G, Van Vliet HA. Immediate postpartum insertion of intrauterine device for contraception. Cochrane Database Syst Rev 2015; 6: CD003036.
19. Goldthwaite LM, Shaw KA. Immediate postpartum provision of long-acting reversible contraception. Curr Opin Obstet Gynecol 2015; 27: 460-464.
20. Therapeutic Guidelines. Choice of Contraceptive Method. Melbourne: Therapeutic Guidelines; 2020. Available online at: https://app.tg.org.au/viewTopic?etgAccess=true&guidelinePage=Sexual-20and-20-Reproductiv-20Health&topicfile=contraceptive-choice (accessed July 2025).
21. Heinemann K, Reed S, Moehner S, Do Minh T. Risk of uterine perforation with levonorgestrel-releasing and copper intrauterine devices in the European Active Surveillance Study on Intrauterine Devices. Contraception 2015; 91: 274-279.
22. Tepper NK, Phillips SJ, Kapp N, Gaffield ME, Curtis KM. Combined hormonal contraceptive use among breastfeeding women: an updated systematic review. Contraception 2016; 94: 262-274.
23. Faculty of Sexual & Reproductive Healthcare (FSRH). FSRH Statement: Ulipristal Acetate and Breastfeeding. London: FSRH; 2025. Available online at: https://www.fsrh.org/Public/Documents/FSRH-statement-Ulipristal-Acetate-and-Breastfeeding.aspx (accessed July 2025).
24. Therapeutic Guidelines. Emergency Contraception. Melbourne: Therapeutic Guidelines; 2020. Available online at: https://app.tg.org.au/viewTopic?etgAccess=true&guidelinePage=Sexual-20and-20Reproductive-20Health&topicfile=emergency-contraception (accessed July 2025).
25. Royal Australian and New Zealand College of Obstetricians and Gynaecologists (RANZCOG). Clinical Guideline for Abortion Care: An Evidence-Based Guideline on Abortion Care in Australia and Aotearoa New Zealand. Melbourne: RANZCOG; 2023.
26. Boesen HC, Rorbye C, Norgaard M, Nilas L. Sexual behavior during the first eight weeks after legal termination of pregnancy. Acta Obstet Gynecol Scand 2004; 83: 1189-1192.
27. Grzeskowiak LE, Rumbold AR, Subasinghe A, et al. Long‐acting reversible contraception use after medical abortion is associated with reduced likelihood of a second medical abortion. Med J Aust 2022; 216: 476-477.
28. Fine PM, Tryggestad J, Meyers NJ, Sangi-Haghpeykar H. Safety and acceptability with the use of a contraceptive vaginal ring after surgical or medical abortion. Contraception 2007; 75: 367-371.
29. Therapeutic Guidelines. Medical Abortion. Melbourne: Therapeutic Guidelines; 2020. Available online at: https://app.tg.org.au/viewTopic?etgAccess=true&guideline Page=Sexual-20and-20Reproductive-20Health&topicfile=medical-abortion (accessed July 2025).
30. Tidy J, Seckl M, Hancock B, on behalf of the Royal College of Obstetricians and Gynaecologists. Management of gestational trophoblastic disease. BJOG 2021; 128: e1-e27.
31. Duggan P, Leung L, Neesham D, et al. RANZCOG Statement for the Management of Gestational Trophoblastic Disease. C-Gyn Melbourne: Royal Australian and New Zealand College of Obstetricians and Gynaecologists; 2017.
Single article purchases are temporarily unavailable due to site maintenance.
If you would like to purchase an article during this time, please email us at [email protected] with the article details and we'll assist you directly. We'll also let you know when online purchasing is available again.
Thank you for your patience and understanding.