Chronic migraine and other types of daily headache

Chronic daily headache is a common and disabling condition. It is usually due to primary headache, most often migraine, but other causes must be kept in mind. A simple approach to diagnosis is required.
- Chronic daily headache is a common condition.
- Establishing the presence of chronic daily headache requires documentation of 15 days or more per month of prolonged headache (lasting more than four hours).
- Most cases of chronic daily headache are due to primary headache, but other causes such as structural lesions must be considered; most cases of primary headache that are troublesome are due to chronic migraine.
- Treatments for patients with chronic migraine are now available.
- Medication overuse is a common complication of headache treatment and makes successful treatment more difficult.
Chronic daily headache is a common issue for people in Australia, with an estimated prevalence of 4% of the population.1 For most people living with daily headaches, the cause is due to a primary headache disorder, with chronic migraine being the most common cause; however, several unique conditions should be considered in this patient group.
The nomenclature here can be confusing – in every other aspect of medicine ‘chronic’ refers to the length of time that a condition has been present. Neurologists, in something of an obstinate move, use ‘chronic’ in the International Classification of Headache Disorders, 3rd edition (ICHD-3) to refer to a headache disorder where the attacks occur on more than half of the days of a month (i.e. episodic migraine is 0 to 14 migraine days per month, and chronic migraine is ≥15 days per month).2 The term ‘chronic daily headache’, therefore, is not actually a distinct diagnostic entity, and something of a tautology.
The diagnostic approach to a patient with chronic daily headache, however, is relatively simple (Flowchart). After establishing the presence of daily headaches, and consideration of secondary causes, ask the patient to identify the presence of migrainous, or cranial autonomic symptoms, which will help narrow the focus.
- The location of the pain: paying specific attention to if the headache is strictly side-locked (does not cross the midline).
- Migrainous features: presence of bilateral photophobia, phonophobia, nausea and vomiting. Apparent worsening of pain by exertion.
- Cranial autonomic symptoms: assess specifically if occurring on the same side as a side-locked headache (eye redness, tearing, nasal congestion, rhinorrhoea, eyelid oedema, ptosis and facial sweating). Note that photophobia may be present also, and curiously is often unilateral and ipsilateral.2,3
Primary headache disorders
Hemicrania continua
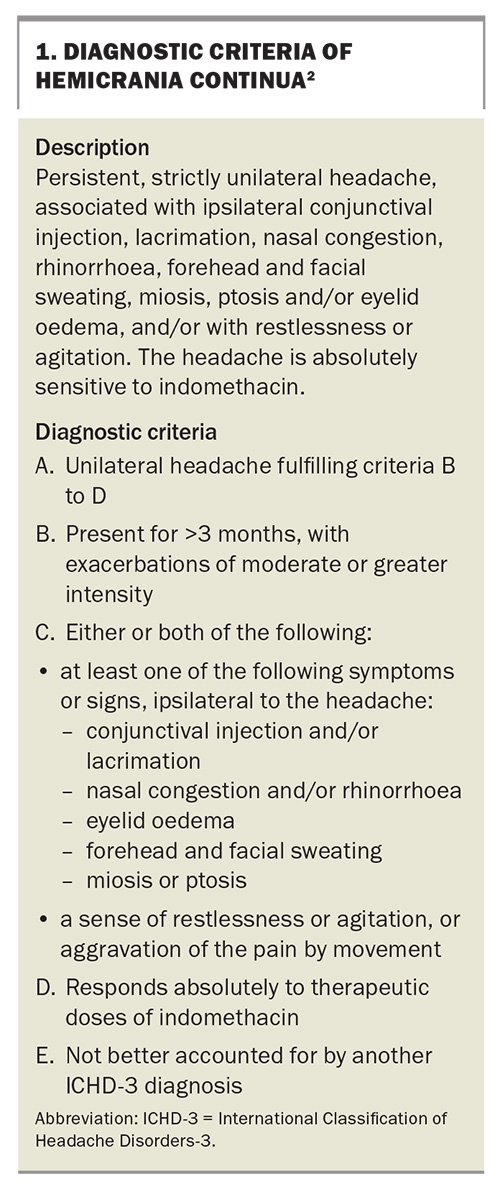
Hemicrania continua is an uncommon disorder with an estimated prevalence of 2.2 cases per 100,000 people but is very characteristic in its classic form (Box 1).4 The headache is strictly unilateral in location and present daily and continuously, without pain-free periods. The pain is usually moderate to severe in intensity, and often located in the anterior temporal or retro-orbital area. It is unique (along with paroxysmal hemicrania) as one of two headache disorders that responds dramatically to treatment with indomethacin at high dose, but not other NSAIDs. A diagnostic trial of indometacin can therefore be informative, if there is clinical suspicion.
Cranial autonomic symptoms such as conjunctival injection or lacrimation, nasal congestion and ptosis or miosis are common when the pain is more severe and intermittent jabs or jolts of pain may be superimposed over the persistent headache. It can occur at any age; however, the mean age of diagnosis is 47.1 years and it is more common in women (2.8:1, female to male ratio).4 In most patients the condition is unremitting.
The first-line treatment of patients with hemicrania continua is with indomethacin, but the doses required are often high (often 150 mg/day; sometimes 225 mg/day in divided doses). This means that gastric, renal and other side effects can limit its use.
New daily persistent headache
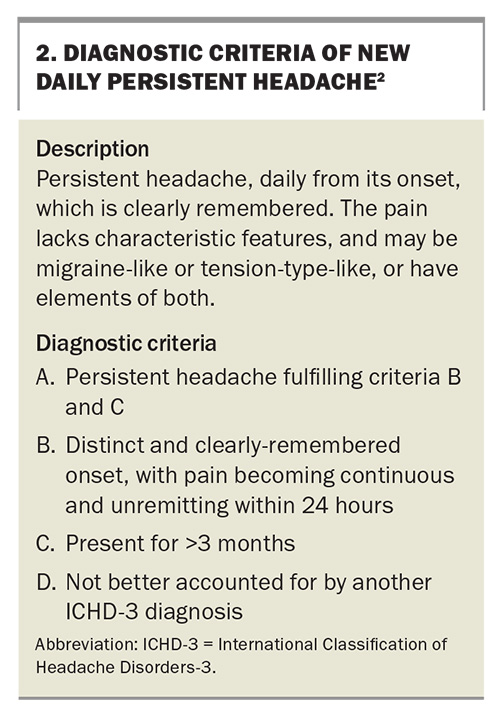
New daily persistent headache (NDPH) has an estimated prevalence of 0.03 to 0.1% in the general population, with an increased prevalence in adolescents than in adults.5 Correct diagnosis has both therapeutic and prognostic implications because patients with this condition generally respond less well to many preventive strategies, and can be refractory to treatment. The major diagnostic pointer is that the patient can give the date of onset of the headache with considerable precision. The overall phenotype of a patient’s headache may have migrainous or tension-type features (Box 2), which helps guide initial choices of therapy to medications that are more efficacious for either condition.
Most patients (53%) report no trigger for NDPH; however, in those with an identifiable trigger, the most common causes are a flu-like illness (22%), stressful life event (9%) and surgical procedures (9%).5
There appears to be two subtypes of NDPH: a self-limiting form, with 66% of patients achieving headache freedom by 24 months; and a refractory form, which is often resistant to aggressive preventive strategies, and can be challenging to treat.5
Chronic migraine
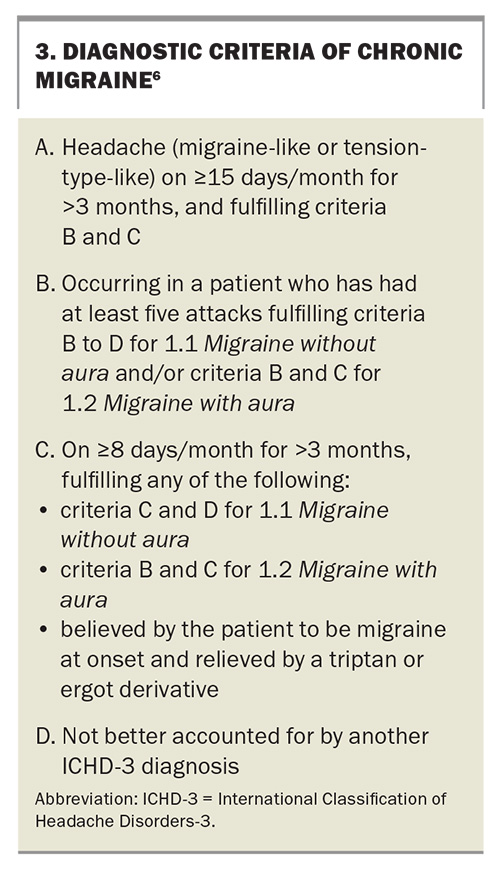
As the second leading cause of years lived with disability, chronic migraine may be the most important cause of chronic daily headache. Chronic migraine is defined as a patient who experiences headaches on 15 days or more per month for more than three months, which, on at least eight days per month, has the features of migraine (Box 3).2,6 It has a global prevalence of 1 to 5%.7
The definition of chronic migraine has evolved amid some controversy. The problem is that as migraine becomes more frequent, the characteristic features (i.e. nausea, vomiting, light and sound sensitivity and throbbing) may become less prominent. The definitions of chronic migraine do not require that all headache episodes be migrainous, but various attempts have been made to set out the minimum requirement. Practically, if a patient with chronic daily headache has evolved gradually from a previous diagnosis of migraine, it is likely to be evolution of the disease, even if the patient does not quite meet the eight migraine days per month outlined in the diagnostic criteria.
Although their headaches are not always migrainous, patients with chronic migraine are much more disabled than those with episodic migraine. The inability to commit reliably to routine work or domestic and social activities because of headache present most days is often the most disturbing issue for patients. Attempts to continue to function by taking escalating doses of acute medication may help in the short term but tend to produce intractable chronic migraine complicated by medication overuse.
Most cases of chronic migraine evolve from a pattern of episodic migraine. It is therefore sensible to look at the risk factors that contribute to this conversion (Box 4).
The single most important issue when presented with a patient with increasing frequency of migraine (especially if they are approaching the chronic migraine range with a frequency of almost 15 days per month) is to avoid overusing acute treatments that are known to produce medication overuse headache. These include, either individually or in combination:
- triptans: should use less than 10 days per month
- simple analgesia (paracetamol or NSAIDs): should use less than 15 days per month
- opiates or combination analgesics: generally not recommended, or use less than 10 days per month.
Starting effective preventive therapy is a key modifiable factor that impacts progression. Preventive treatments for migraine, including chronic migraine, are discussed in the article on ‘Migraine in 2025: an update on management’ elsewhere in this Focus on headache supplement. If there is a component of medication overuse headache, withdrawing the offending medication in combination with preventive therapy can be effective (see article on ‘Medication overuse headache: less is MOH’, included in this Focus on headache supplement).
Concomitant medical and psychiatric disorders, including depression, sleep disorders and obesity, should be managed at the same time as the chronic migraine. Patients with a susceptibility to migraine may have migrainous headaches triggered by other painful conditions around the head and neck and, if present, these should also be treated; however, some patients invest substantial effort in pursuing unrewarding treatments of the neck, temporomandibular joint, sinuses and so forth.
Although challenging, the treatment of patients with chronic migraine can be enormously rewarding. Patients who can once more engage reliably in work and family and social activities are among the most grateful patients seen in neurological practice.
Chronic tension-type headache
Chronic tension-type headache is defined as chronic daily headache that fails to meet the criteria for the other three disorders discussed, namely hemicrania continua, NDPH and chronic migraine. It is often described as a featureless band of pain. Chronic tension-type headache is somewhat controversial as an entity as many US headache specialists believe that it is over diagnosed and is in fact rare: they point to the fact that when diary data are collected, many diagnoses of tension-type headache should in fact be migraine.8 In Europe, there is a different view, and tension-type headache is considered common. It does seem clear, however, that chronic tension-type headache is much less disabling than chronic migraine.
Despite its apparent frequency (up to 2% of the population in many surveys), the treatment of patients with chronic tension-type headache is not well defined.1 There have been few trials addressing this. There is some evidence to support the use of amitriptyline in doses of 10 to 75 mg/day (off-label use).9
Secondary headaches that can produce a pattern of chronic daily headache
Although most patients with chronic daily headache have a primary headache with no obvious structural or other cause, some specific conditions that may cause headache should be considered. Pain arising from the neck, sinuses or eyes is usually diagnosed easily. The following conditions also deserve attention.
Medication overuse headache
Medication overuse headache is a significant health issue, affecting one-quarter of patients with migraine, and up to 70% of patients in specialist clinics and with chronic daily headache.10 The mechanism seems to be that regular use of the offending agent results in a degree of physiological habituation. Absence of the agent can produce a withdrawal effect, the most prominent feature of which (in a headache-prone individual) is recurrent headache. This is sometimes described as rebound headache and some patients find this term helpful in understanding the condition; however, it is important to recognise that this habituation or sensitisation of pain circuits in the brain also occurs in patients who do not experience rebound headaches.
Making a diagnosis of medication overuse headache is not difficult: it simply requires an accurate history of medication use. This is often best approached by asking how many days in a month there is no medication taken by the patient for headache.
The traditional approach to the treatment of patients with medication overuse headache has involved abrupt withdrawal of the agent in question. However, it is certainly reasonable to counsel patients on the importance of eliminating such medications and to offer migraine prophylaxis to allow them to wean off the offending drug gradually, although, in practice, few patients achieve this.
Abrupt withdrawal is also difficult as it requires fortitude and commitment from the patient who must obviously see the point and want treatment. Even when the overused agent is an opioid, most patients are keen to stop taking it because their dependence on the drug has no recreational element. Naturally, such abrupt withdrawal inevitably causes a severe headache that must be managed in some other way. Outpatient protocols include the use of NSAIDs (e.g. naproxen sustained release 750 mg daily for a week) or corticosteroids (e.g. prednisolone 60 mg/day for a week and then taper). Inpatient treatment excludes the patient from day-to-day responsibilities and allows for a wider range of options to control headache, including dihydroergotamine or lignocaine by infusion. Severe withdrawal headaches often settle within two to four days for triptan overuse, four to seven days for ergotamine overuse and seven to 10 days for substantial codeine overuse. The withdrawal phase must be followed by a plan to manage breakthrough headaches without reverting to the offending drugs. Medication overuse headache is discussed in more detail in the article on ‘Medication overuse headache: less is MOH’, included in this Focus on headache supplement.
Intracranial structural lesions
Space-occupying lesions such as tumours may present with headache as the primary complaint. For a lesion to become so large as to cause raised intracranial pressure without obvious focal signs, it must reside in a ‘silent area’ of the brain (an area not likely to produce obvious physical signs), such as the frontal lobes and anterior temporal lobes. Lesions near the third ventricle, aqueduct or fourth ventricle may be smaller but cause hydrocephalus through ventricular obstruction. Typically, headache caused by raised intracranial pressure is said to be worse in bed or on waking, but this feature is not reliable. Most mass lesions produce a gradually progressive increase in symptoms over weeks or months. Often a careful neurological examination will show abnormalities such as papilloedema or focal signs. Modern imaging, especially MRI, is excellent at revealing such problems and should be performed if there is any suspicion of a space-occupying lesion.
Idiopathic intracranial hypertension
Formerly called benign intracranial hypertension or pseudotumour cerebri, idiopathic intracranial hypertension typically occurs in overweight young women. Diagnostic clues include symptoms of transient visual obscuration (darkening of vision in one eye) on rising from a stooped position, pulsatile tinnitus, diplopia (from partial sixth nerve palsy) and the finding of papilloedema. Imaging is typically normal, but cerebrospinal fluid pressure measured by lumbar puncture is high.
Idiopathic intracranial hypertension is an important diagnosis to make because neglecting the condition may result in severe visual loss from prolonged papilloedema. Treatment includes weight loss and acetazolamide, which is typically commenced at 500 mg twice per day, and advanced as required or tolerated to 2 to 4 g per day. Surgery (such as optic nerve sheath fenestration or shunting) may be required in refractory cases to save the patient’s vision. The pathogenesis is complex but an important mechanism contributing to persistent raised pressure is dynamic narrowing of venous sinuses: the elevated intracranial pressure compresses the sinuses, causing obstruction to venous outflow and thus even higher pressures. This vicious cycle can be addressed by stenting the offending sinus (identified by venography) but the long-term pros and cons of this technique are debated.11
Low-pressure headache
Leakage of cerebrospinal fluid from the dural sac can cause headache. This is a well-known condition after lumbar puncture (or when the dura is accidentally punctured in an epidural injection or infusion), when postural headache (present soon after rising and relieved by lying down) is the obvious clue. It is less well known that a similar headache may occur spontaneously. This is usually caused by leakage of cerebrospinal fluid from a nerve root sleeve in the spine. The headache often appears over a day or two (similar to NDPH) and has the expected postural features.
MRI scanning of the brain, with contrast, shows a number of characteristic features (including prominent enhancement of the dura) but they may be subtle and not recognised if the clinical suspicion of low cerebrospinal fluid pressure has not been conveyed to the radiologist. Locating the leak in the spine may be difficult and again it is vital to liaise with the radiologist to obtain the best results. Post-lumbar puncture headache that does not resolve promptly usually responds well to epidural autologous blood patch. Similar techniques can be used in patients with spontaneous low-pressure headache if the site of the leak can be identified.
Giant cell arteritis
Giant cell arteritis typically occurs after 55 years of age. It presents with nonspecific headache (and often diffuse malaise and muscular pain from associated polymyalgia rheumatica). Erythrocyte sedimentation rate and C-reactive protein levels are usually markedly elevated and are useful screening tests. The diagnosis should be confirmed by temporal artery biopsy; however, treatment should not be delayed until the biopsy in cases of strong clinical suspicion. The diagnosis is important because of the risk of blindness from retinal artery occlusion if untreated. In selected patients, glucocorticoid-sparing agents such as tocilizumab are considered.
Conclusion
Chronic daily headache is a common and debilitating disorder. Accurate diagnosis is not difficult in most cases. Modern approaches to treatment, with recognition of medication overuse and active management of chronic migraine, may provide substantial relief to many patients. Helping patients with such a disabling condition to improve their quality of life is very rewarding. MT
COMPETING INTERESTS: Professor Stark has served on advisory boards for Teva, Eli Lilly, AbbVie, Viatris and Lundbeck; and received payment for educational presentations from AbbVie, Teva, Eli Lilly and Viatris. Dr Ray has received honoraria for educational presentations for AbbVie, Novartis and Viatris; has served on medical advisory boards for Pfizer, Viatris and Lilly; and his institution has received funding for research grants, clinical trials and projects supported by the International Headache Society, Brain Foundation, Lundbeck, AbbVie, Pfizer and Aeon. Dr Hutton has served on advisory boards for Sanofi-Genzyme, Novartis, Teva, Eli Lilly, Allergan, Lundbeck, been involved in clinical trials sponsored by Novartis, Teva, Xalud and Cerecin, and has received payment for educational presentations from Allergan, Teva, Eli Lilly and Novartis.
References
1. Pascual J, Colas R, Castillo J. Epidemiology of chronic daily headache. Curr Pain Headache Rep 2001; 5: 529-536.
2. Headache Classification Committee of the International Headache Society. The International Classification of Headache Disorders. 3rd ed. Cephalalgia 2018; 38: 1-211.
3. Irimia P, Cittadini E, Paemeleire K, Cohen AS, Goadsby PJ. Unilateral photophobia or phonophobia in migraine compared with trigeminal autonomic cephalalgias. Cephalalgia 2008; 28: 626-630.
4. Hagan K. One-year prevalence of cluster headache, hemicrania continua, paroxysmal hemicrania and SUNCT in Norway: a population-based nationwide registry study. J Headache Pain 2024; 25: 30.
5. Yamani N, Olesen J. New daily persistent headache: a systematic review on an enigmatic disorder. J Headache Pain 2019; 20: 80.
6. Headache Classification Committee; Olesen J, Bousser MG, Diener HC, et al. New appendix criteria open for a broader concept of chronic migraine. Cephalalgia 2006; 26: 742-746.
7. Natoli JL, Manack A, Dean B, et al. Global prevalence of chronic migraine: a systematic review. Cephalalgia 2010; 30: 599-609.
8. Lipton RB, Cady RK, Stewart WF, Wilks K, Hall C. Diagnostic lessons from the spectrum study. Neurology 2002; 58(9 Suppl 6): S27-S31.
9. Lance JW, Curran DA. Treatment of chronic tension headache. Lancet 1964; 1: 1236-1239.
10. Fischer A, Jan A. Medication-overuse headache. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2025.
11. Ahmed RM, Wilkinson M, Parker GD, et al. Transverse sinus stenting for idiopathic intracranial hypertension: a review of 52 patients and of model predictions. AJNR 2011; 32: 1408-1414.